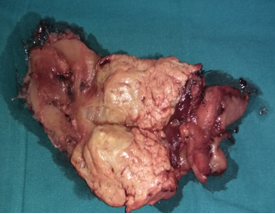
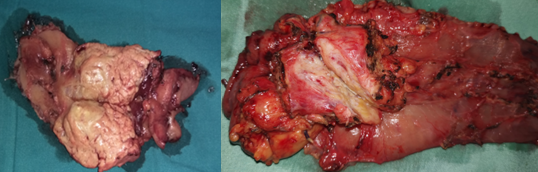
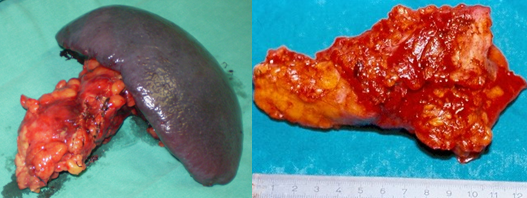
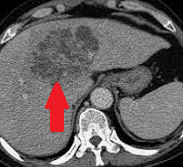
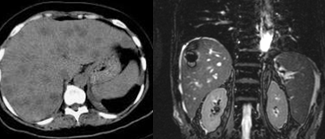
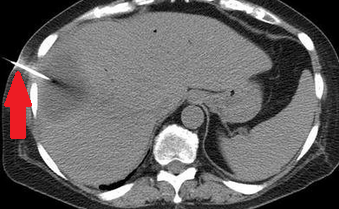
Liver Abscesses following Pancreaticoduodenectomy.
Αποστήματα ήπατος μετά παγκρεατικο12δακτυλεκτομή.
The postoperative development of biliary fistulas and the need for reoperations are considered the most significant risk factors for the development of pyogenic liver abscesses. Antibiotic administration and, when necessary, percutaneous drainage of the abscesses, yield excellent/beneficial results in the majority of patients without any negative impact on hepatic function or survival.
Introduction
Pyogenic hepatic abscesses constitute a significant clinical problem. Unfortunately, little is known about the current microbial sensitivity profile and the frequency of multidrug-resistant micro-organisms capable of causing pyogenic liver abscesses in the Western world.Nevertheless, this critical information is decisive for guiding empirical antibiotic therapy.
Pancreaticoduodenectomy is a demanding surgical procedure, with postoperative complication rates reaching 40%. The development of pyogenic liver abscesses following pancreaticoduodenectomy constitutes an uncommon complication, and there is a lack of information regarding their incidence and therapeutic management.
In this study, we examined the incidence, risk factors, treatment, and long-term outcomes of pyogenic liver abscesses following pancreaticoduodenectomy.
Material - Methods
We retrospectively studied 250 patients who underwent pancreaticoduodenectomy (n=200) or distal pancreatectomy (n=50) during the period 1995-2010 at our Department, and focused our study on the postoperative complications encountered by both patient groups.We identified 6 patients in the first group (3 developed pyogenic liver abscesses) and no patients in the second group. These patients were matched regarding age, sex, year of operation, indications for surgical intervention, postoperative complications, and need for reoperation.
Pyogenic abscesses developed in 6/200 (3%) patients who underwent pancreaticoduodenectomy and in none of the patients who underwent distal pancreatectomy. Of these, 3 had solitary abscesses (50%) and the remaining 3 had multiple abscesses (50%). 3/6 developed biliary fistulae postoperatively, while 3/6 required reoperation for reconstruction of the pancreaticojejunal anastomosis. All patients received broad-spectrum antibiotic therapy, while 3 of them additionally required percutaneous drainage of the abscesses. The mean hospitalization duration was 21 days. There were no deaths.
Conclusions
The postoperative development of biliary fistulae and the need for reoperation are considered the most significant risk factors for the development of pyogenic hepatic abscesses. Administration of antibiotics and occasionally the need for percutaneous abscess drainage yield excellent beneficial results in the majority of patients, without adverse effects on hepatic function and survival.
- Pyogenic liver abscesses following pancreaticoduodenectomy occur in approximately 3% of cases and are associated with biliary fistulae and need for reoperation
- Solitary and multiple abscesses occur with equal frequency (50% each)
- Management with broad-spectrum antibiotics and percutaneous drainage when indicated achieves excellent outcomes with no mortality
- Distal pancreatectomy does not carry the same risk of hepatic abscess formation
- Early recognition of biliary fistulae is crucial as they represent the primary risk factor for hepatic abscess development
Sign in to join the discussion
Loading...