Large Intestine
Παχύ Έντερο
390 images · 2 sub-chapters
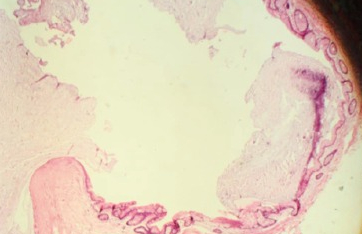
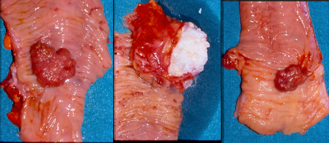
Cyst containing condensed mucus, lined with benign colonic epithelium, surrounded by fibrosis (Courtesy Dr. V. Penopoulos)
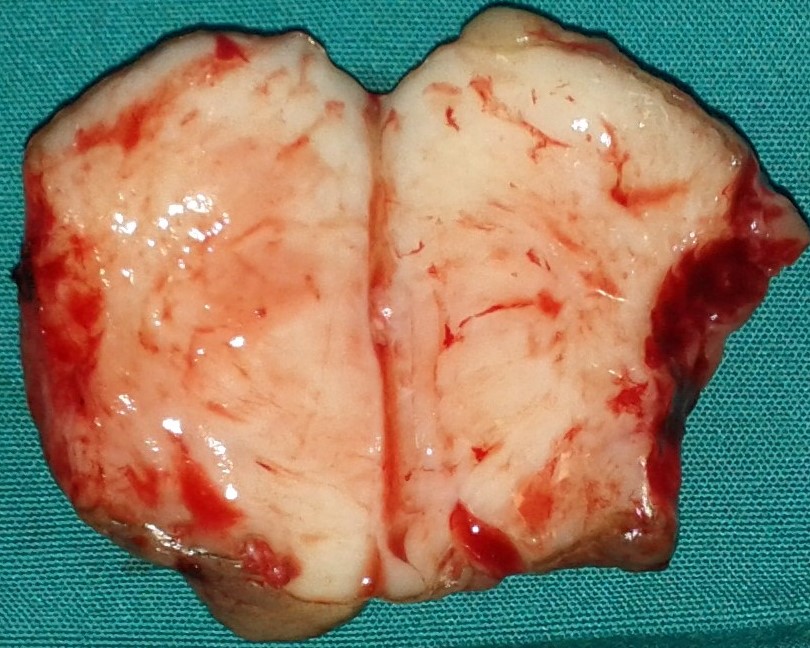
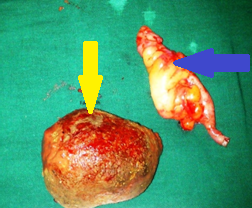
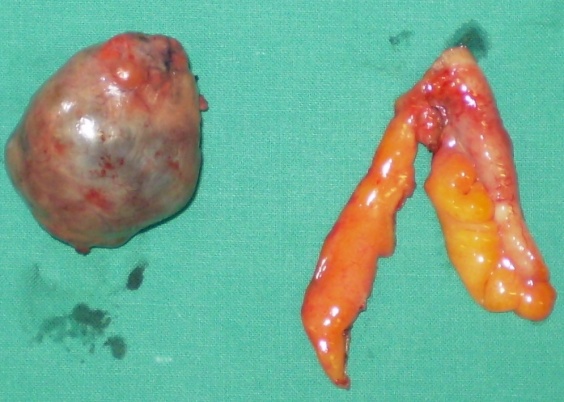
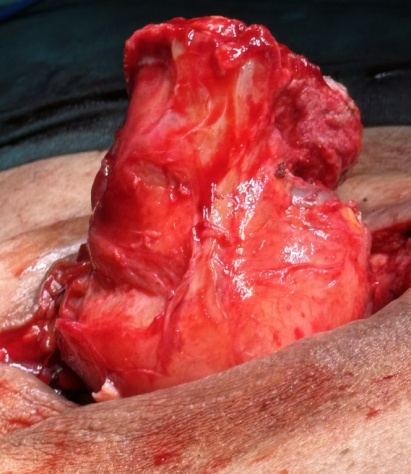
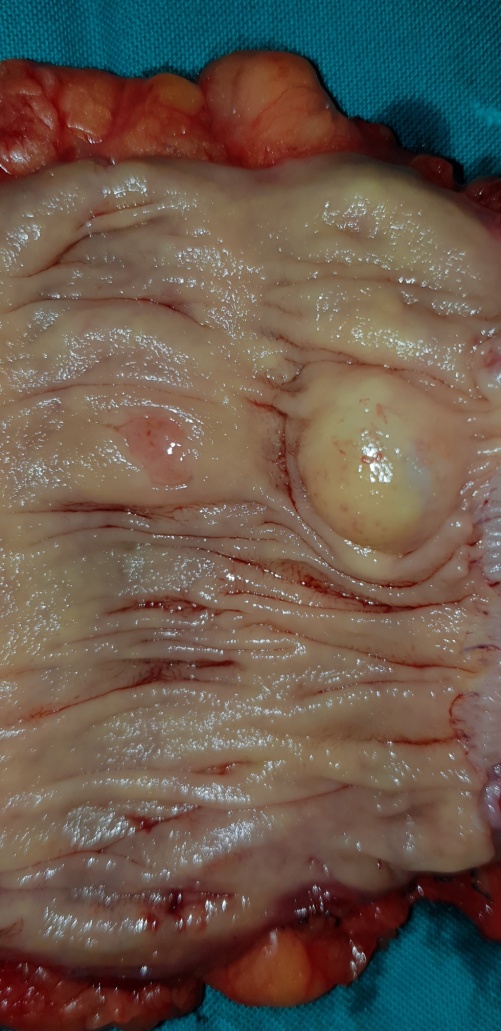
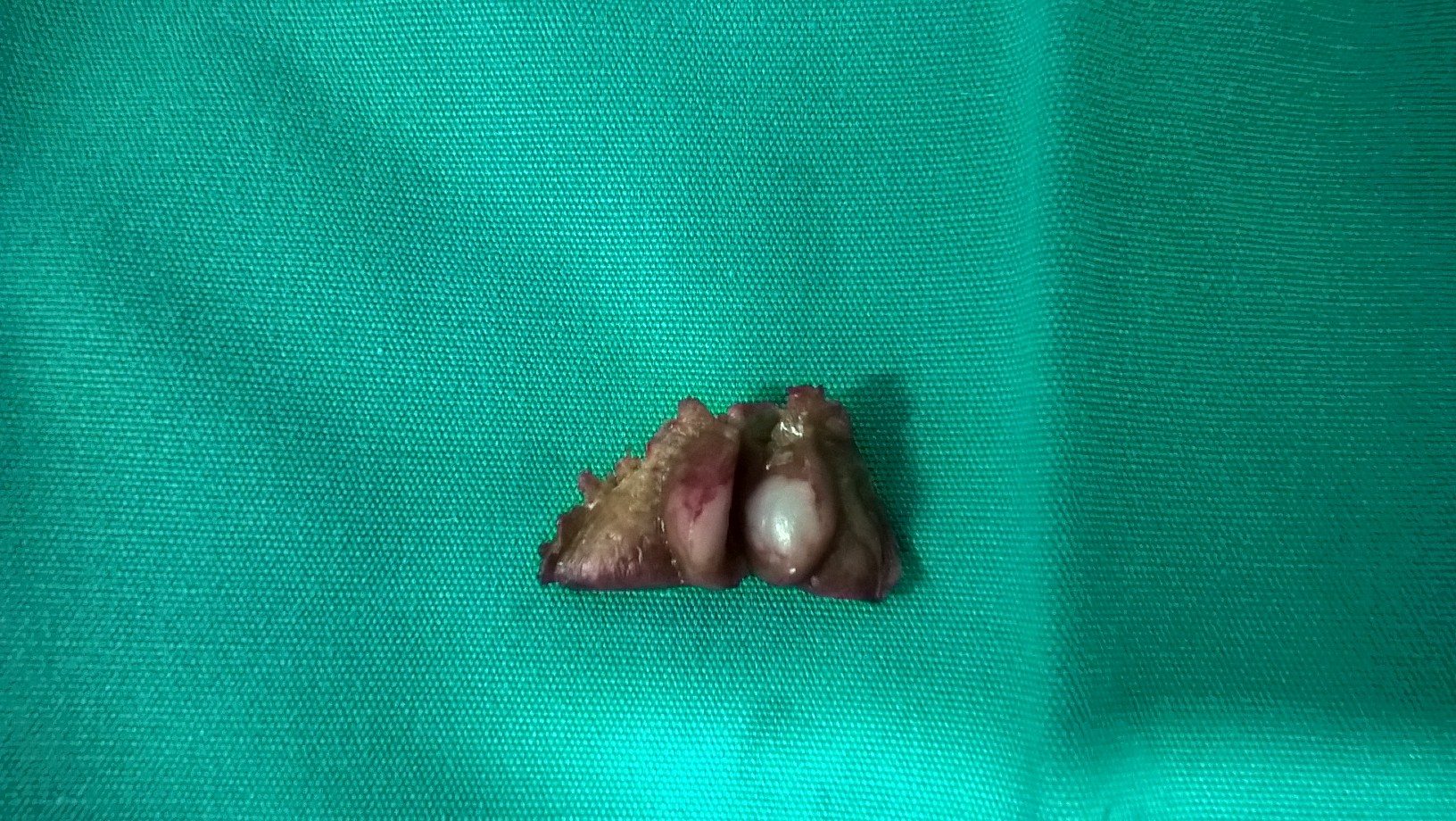
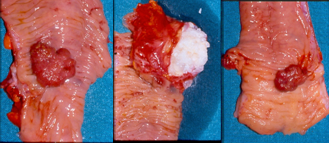
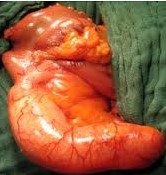
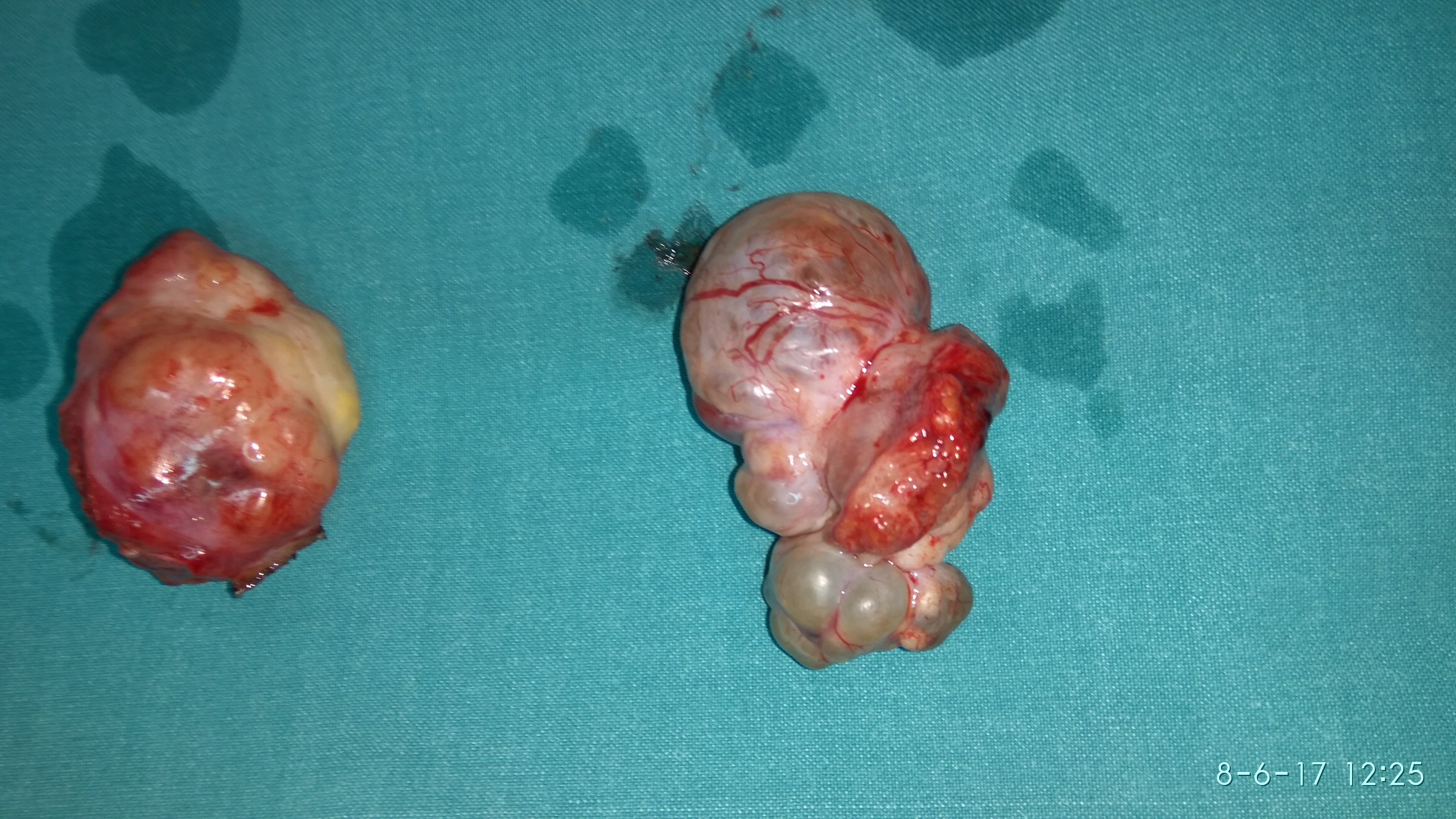
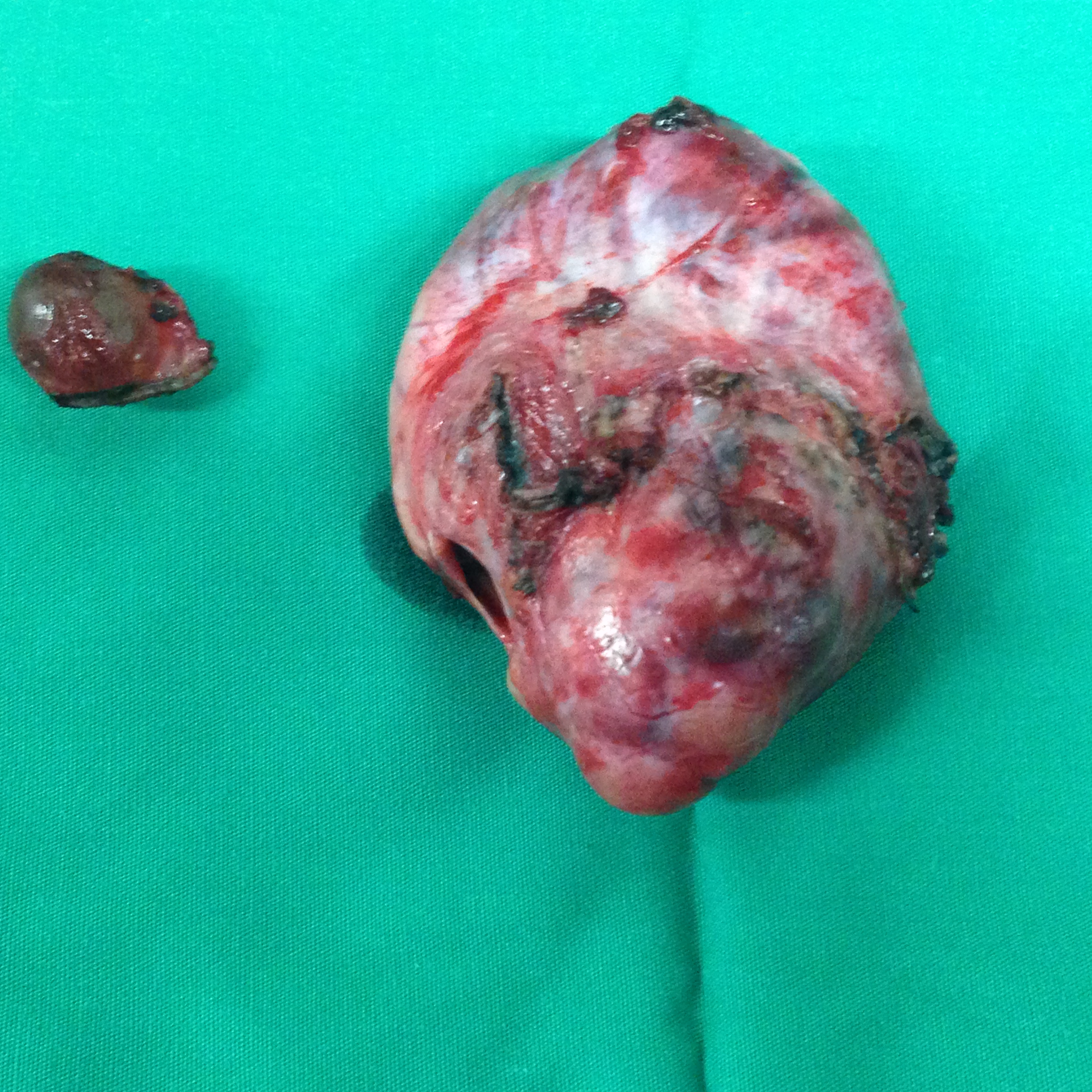
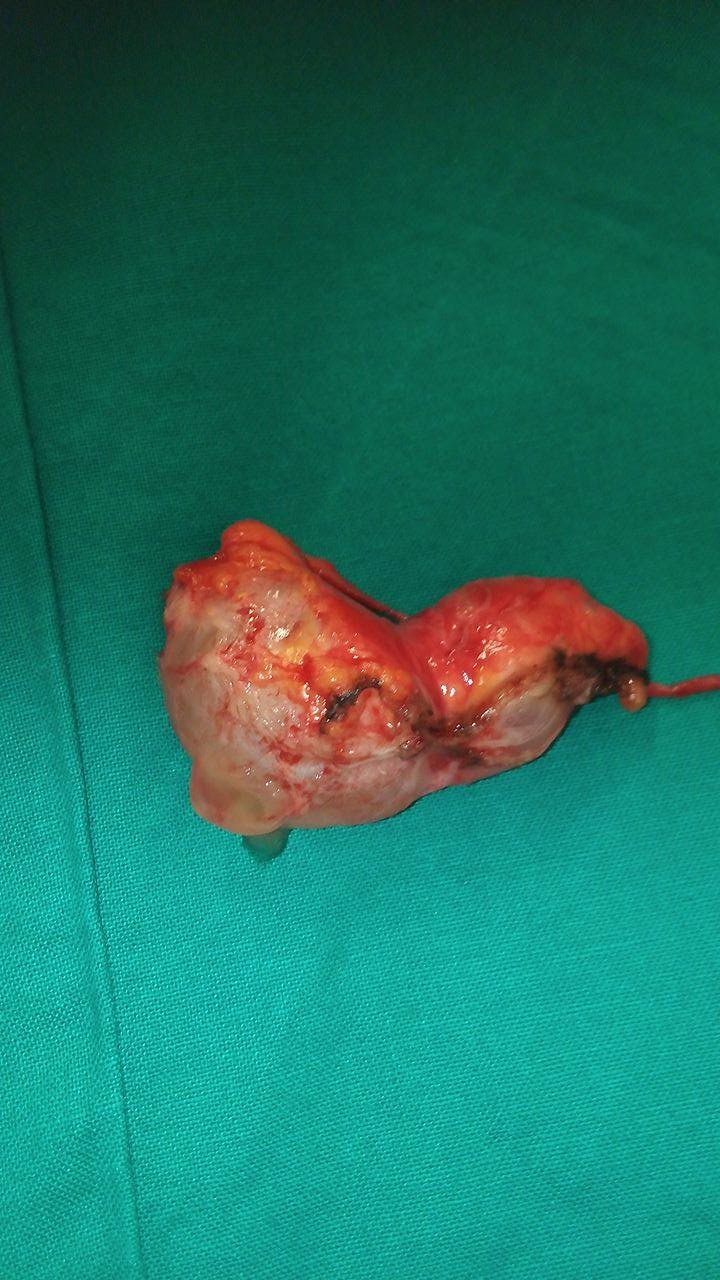
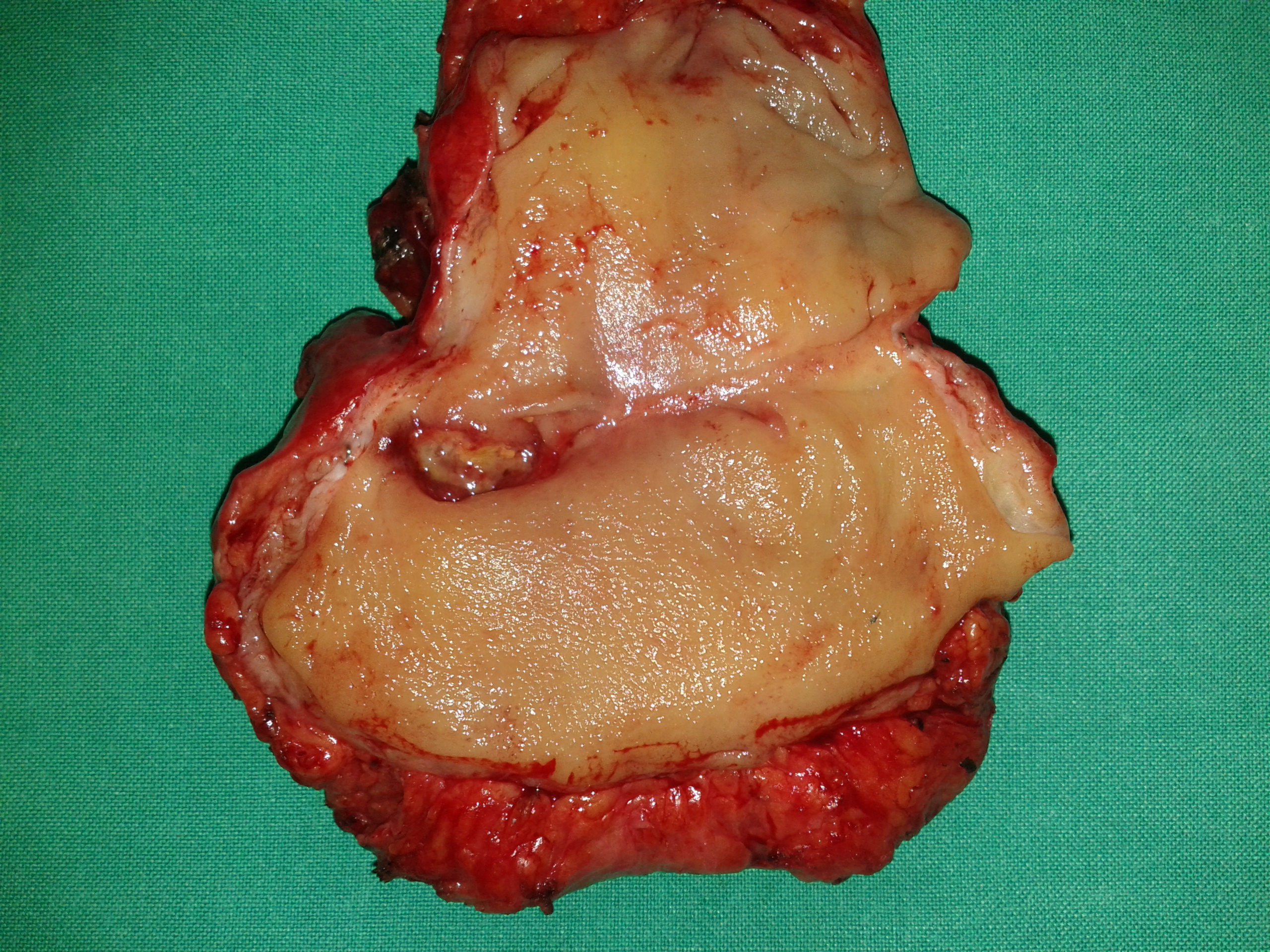
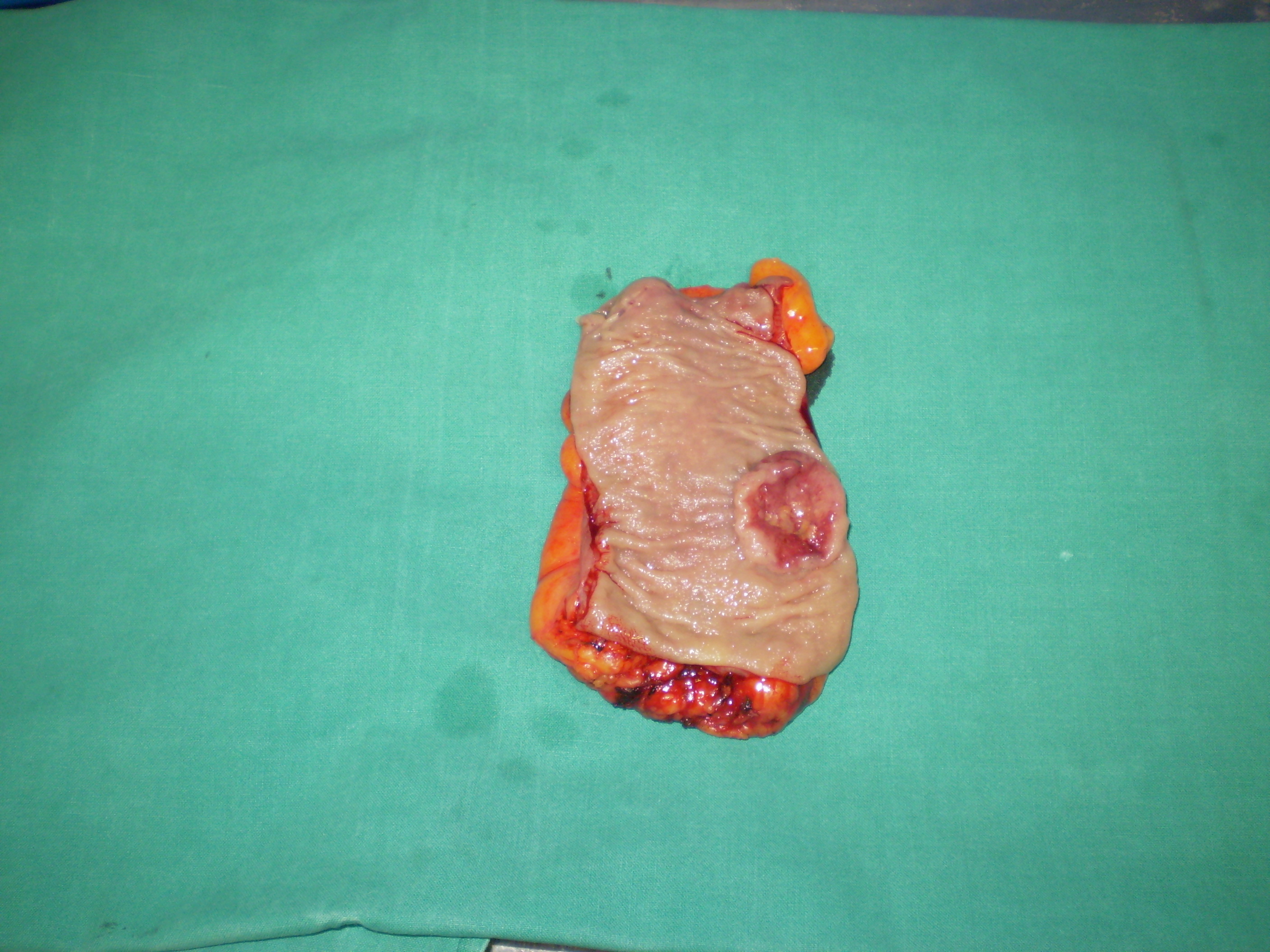
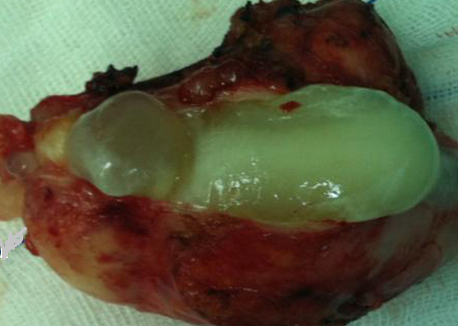
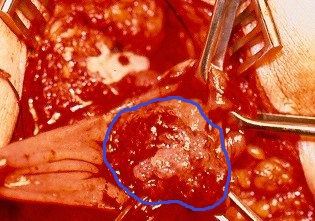
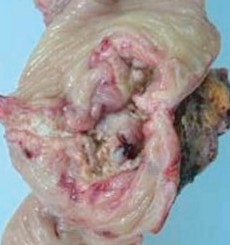
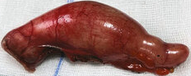
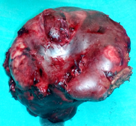
The excised fibroma. A white, homogeneous, fibrous mass is observed (Courtesy Dr. V. Penopoulos)
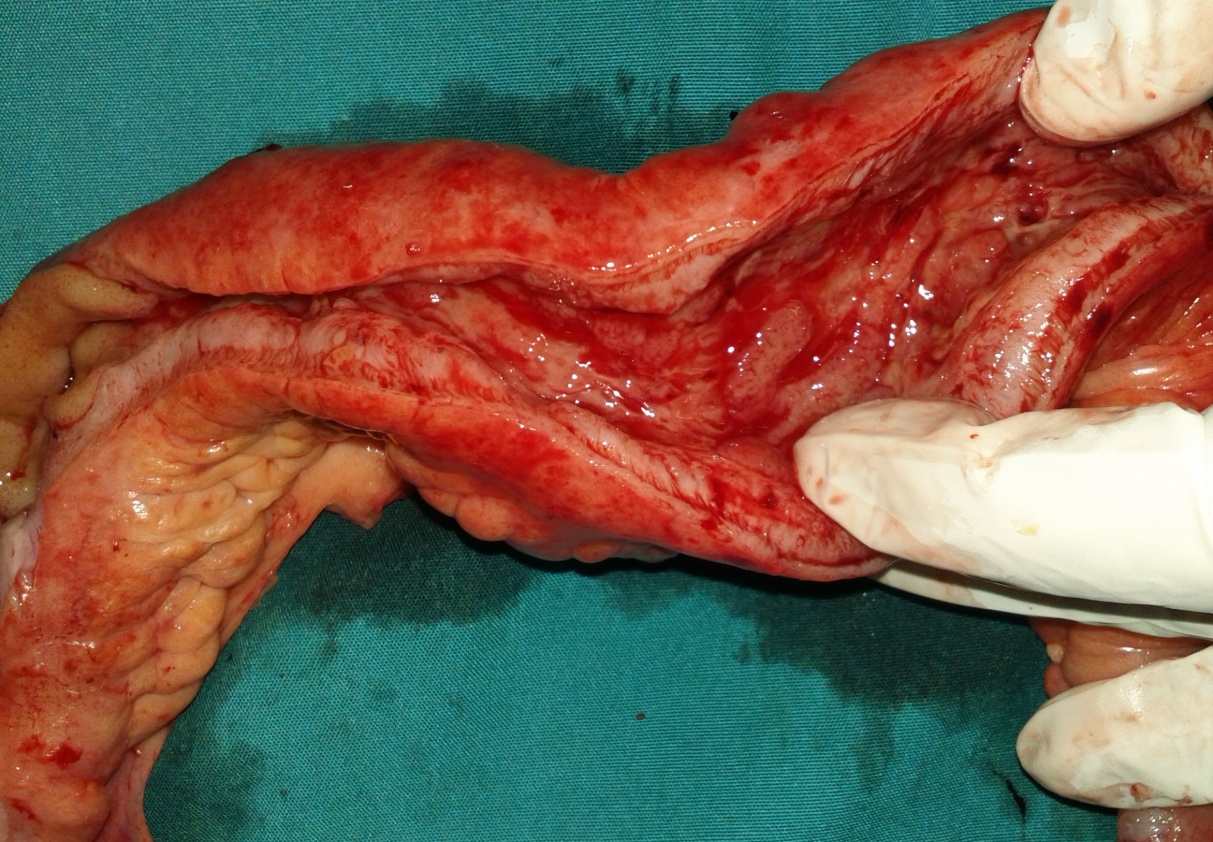
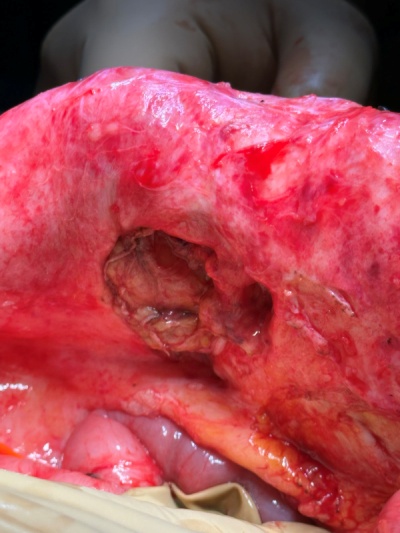
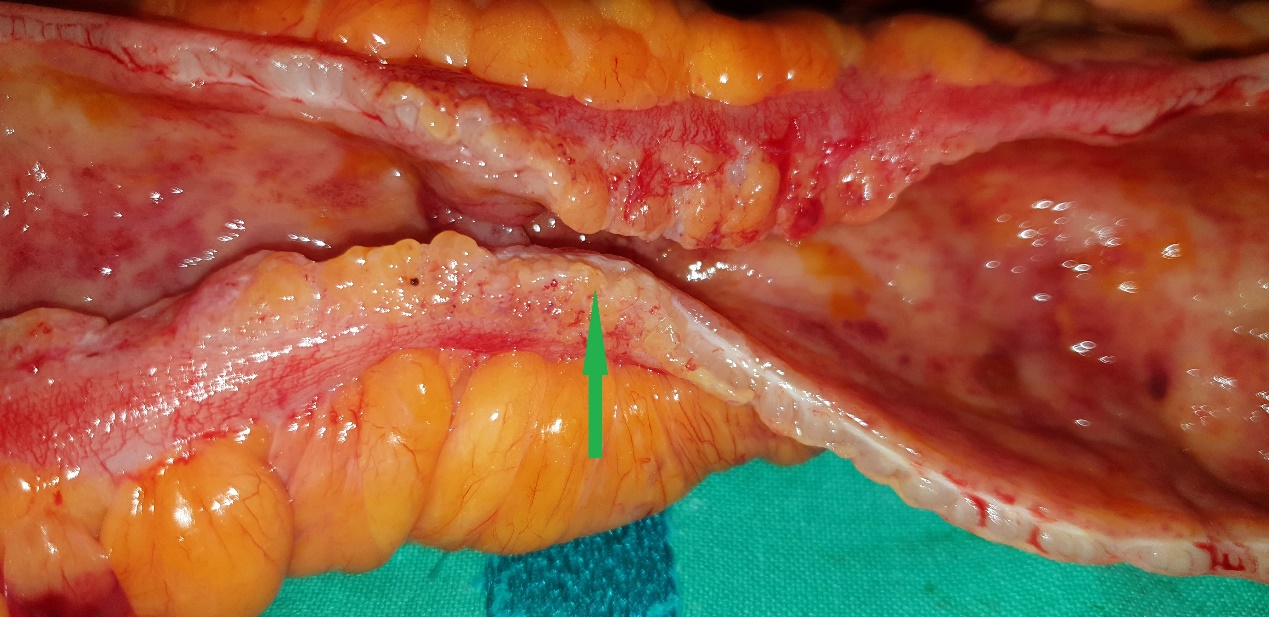
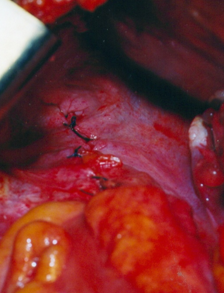
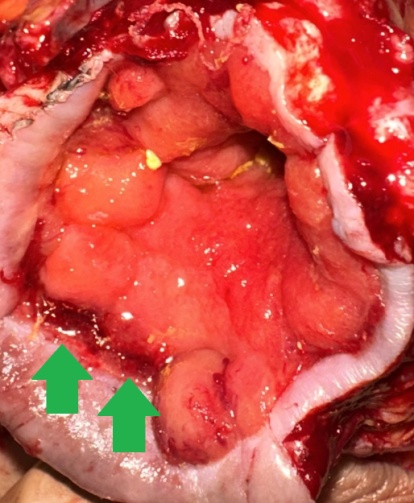
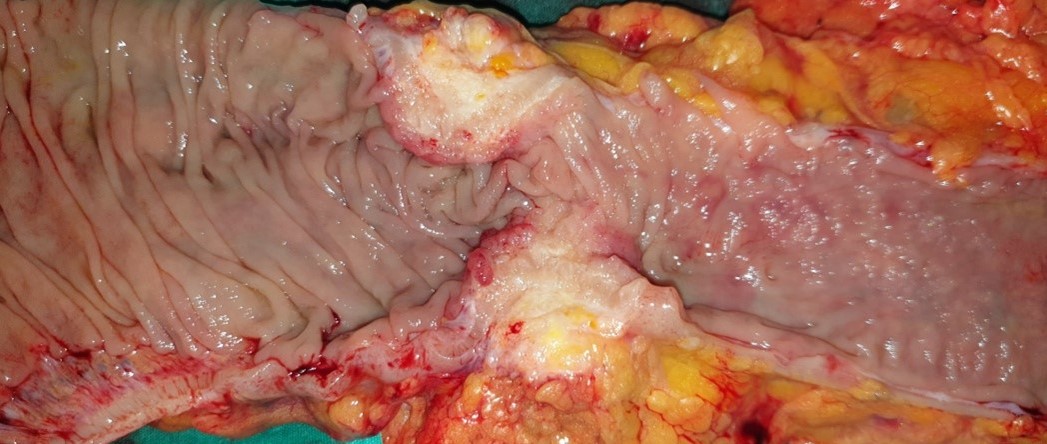
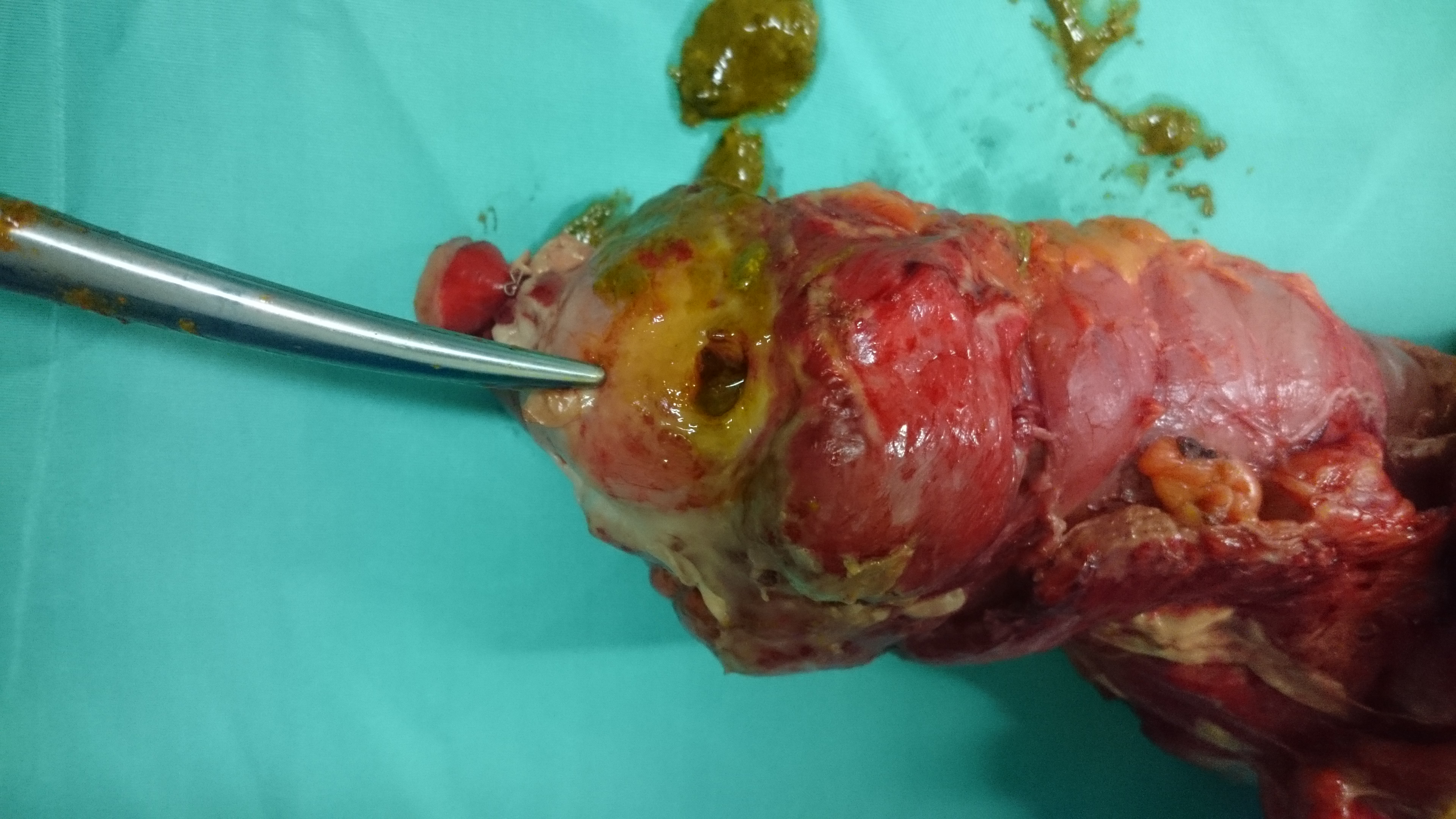
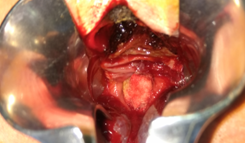
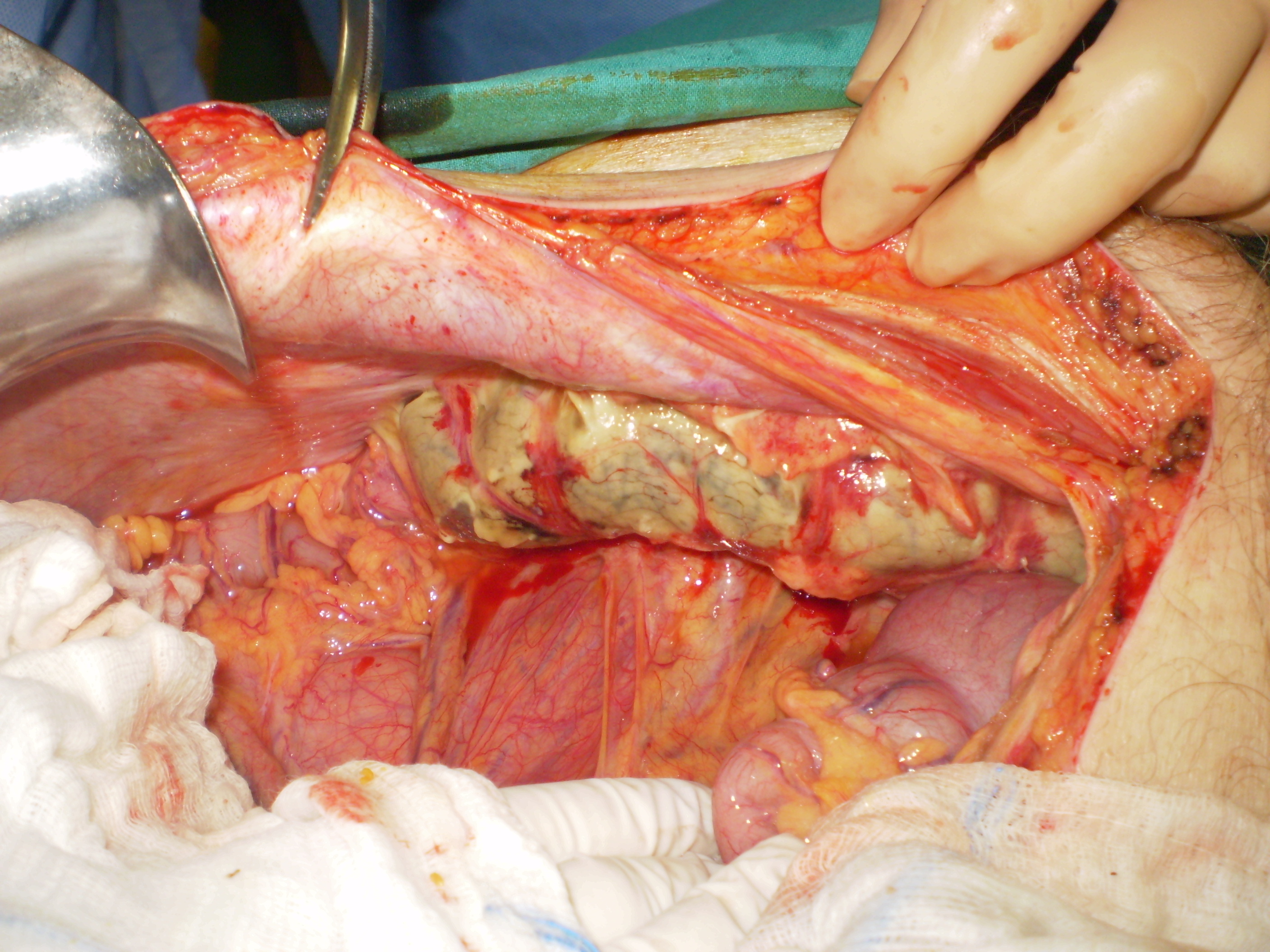
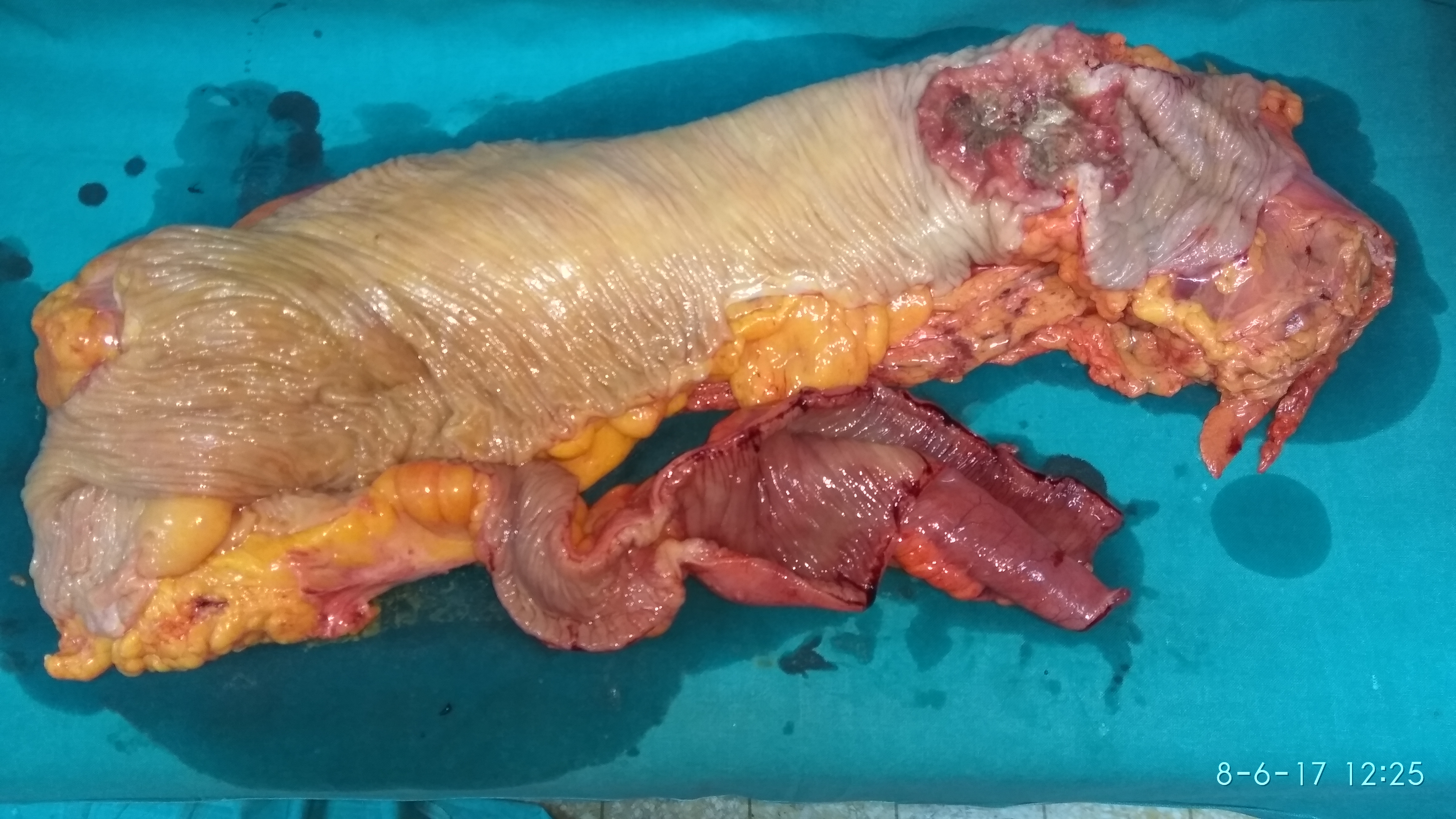
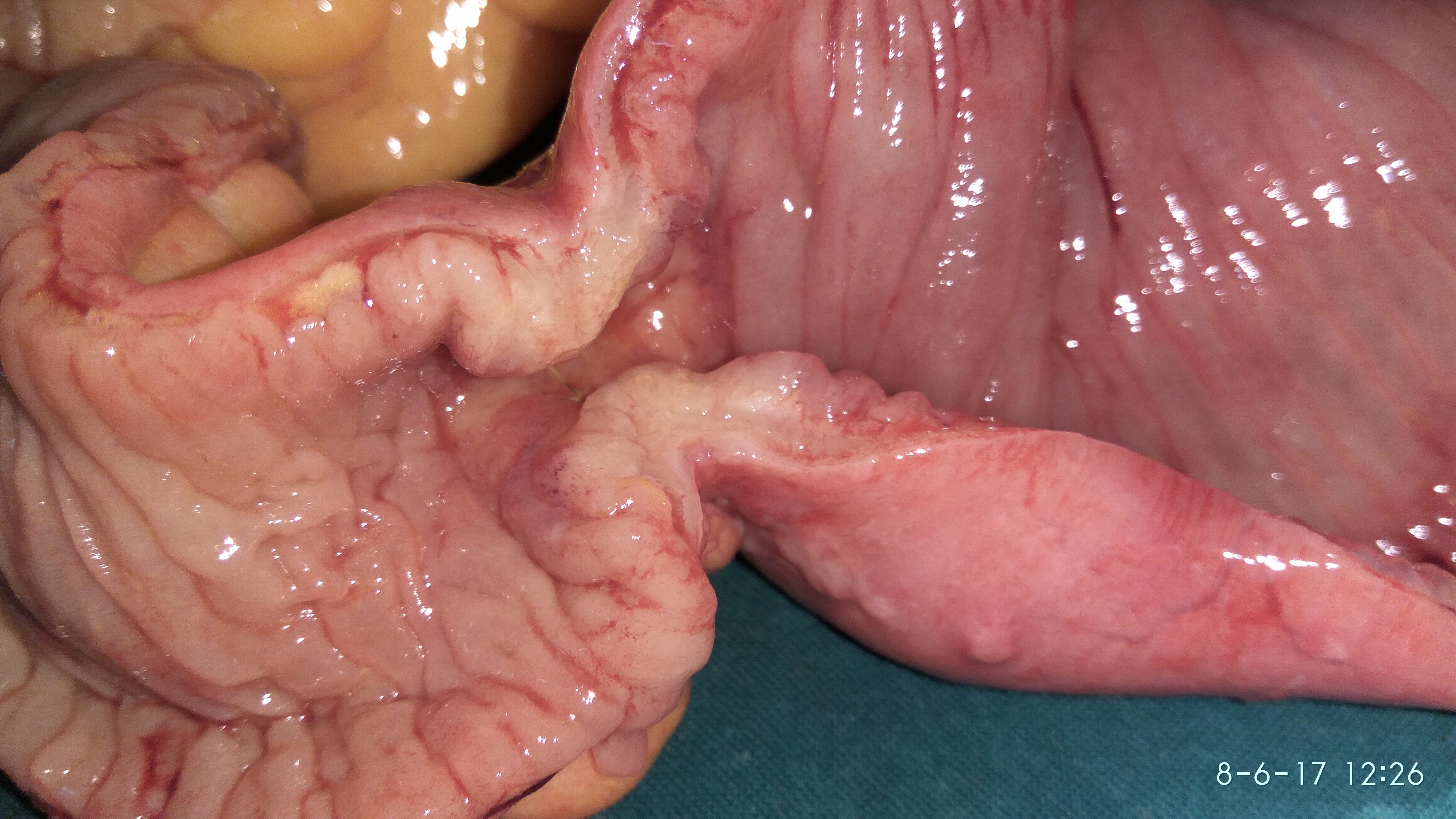
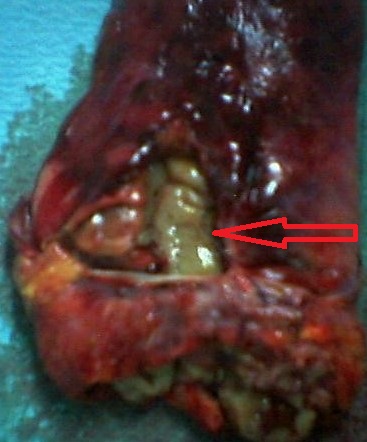
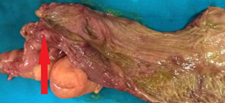
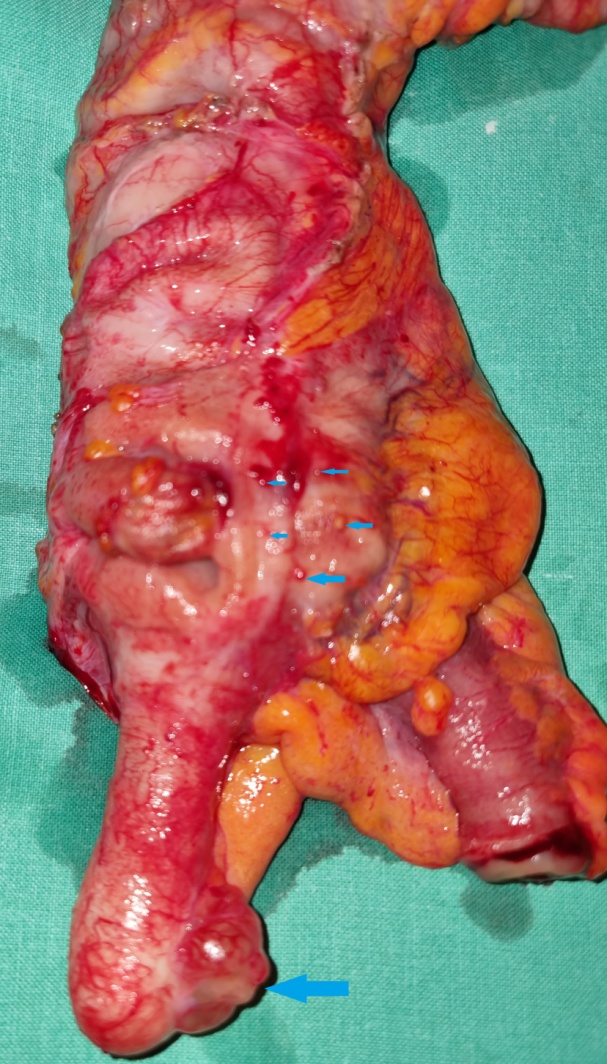
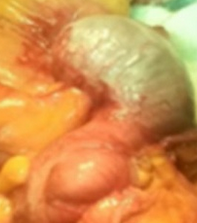
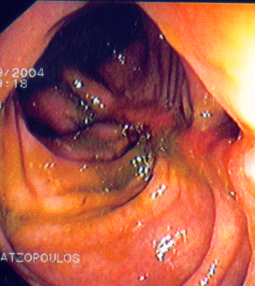
The terminal ileal stricture is evident between the surgeon's fingers (Courtesy Dr. V. Penopoulos)
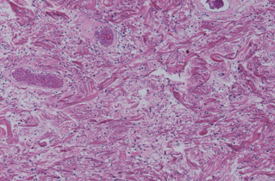
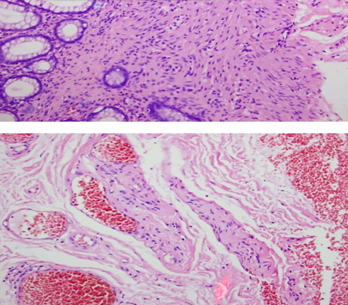
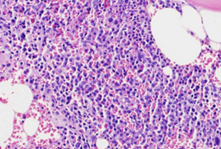
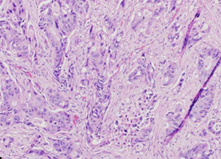
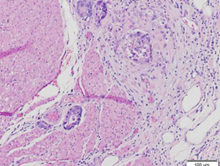
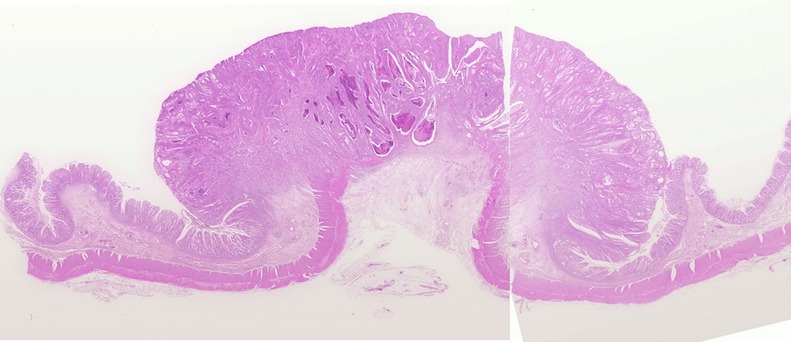
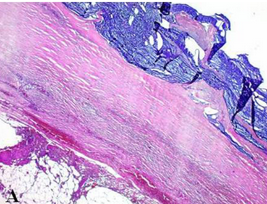
Microscopic image after Hematoxylin and Eosin staining, showing fibrous connective tissue without atypia, resembling skin fibroma (Courtesy Dr. V. Penopoulos)
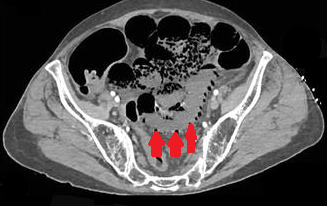
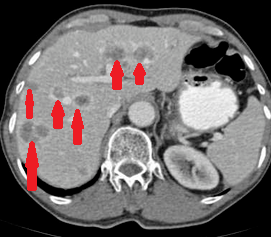
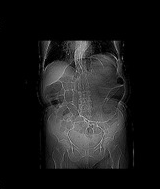
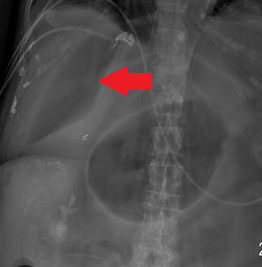
Presence of air in the portal venous system, secondary to ischemic colitis (Courtesy Dr. V. Penopoulos)
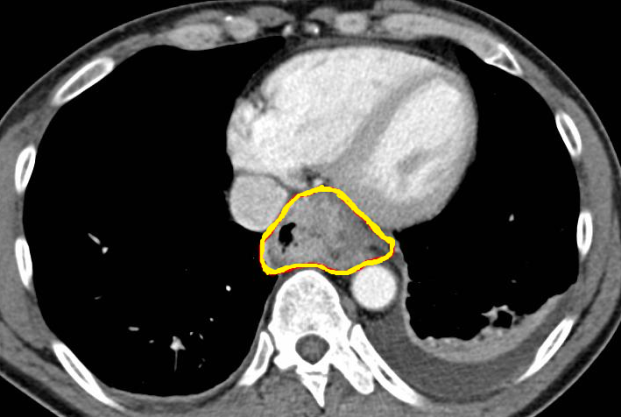
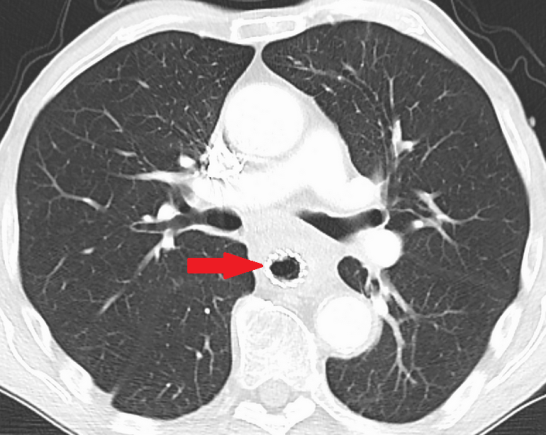
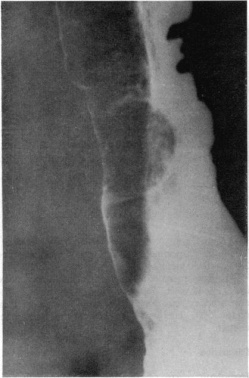
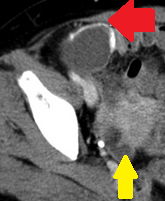
Chest CT — Esophageal adenocarcinoma with extraluminal extension (Courtesy Dr. V. Penopoulos)
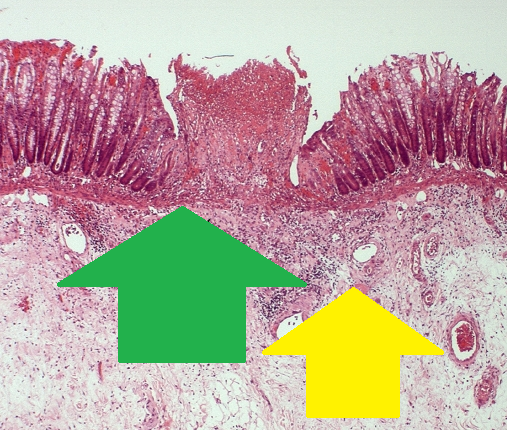
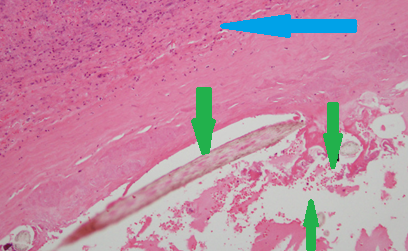
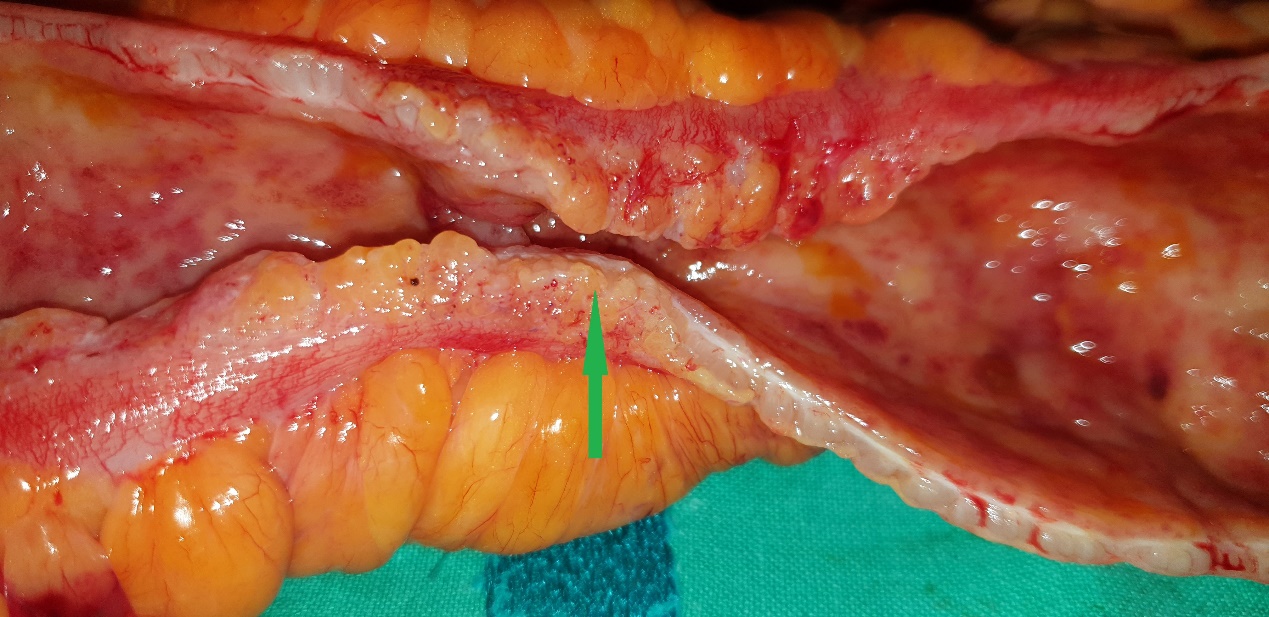
Green arrow – perivenular lymphocytic infiltration in a submucosal location (Courtesy Dr. V. Penopoulos)

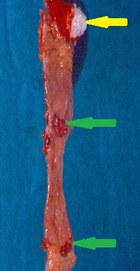
Green arrow – focal ulceration of the colonic mucosa. Yellow arrow – edema and lymphocytic infiltration of the submucosa (Courtesy Dr. V. Penopoulos)
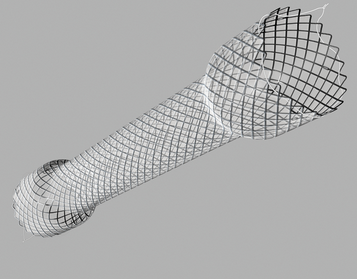
Endoscopy after stent expulsion. Mild response of adenocarcinoma to chemotherapy (Courtesy Dr. V. Penopoulos)
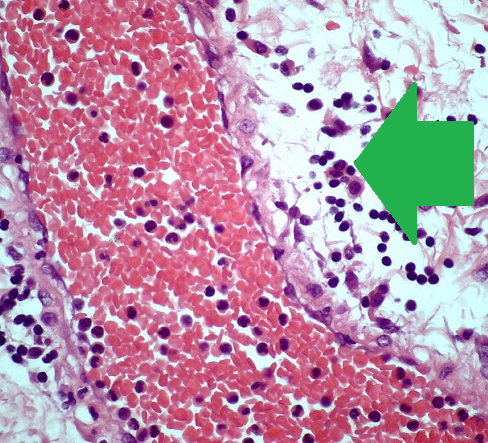
Green arrow – perivenular lymphocytic infiltration in a submucosal location (Courtesy Dr. V. Penopoulos)

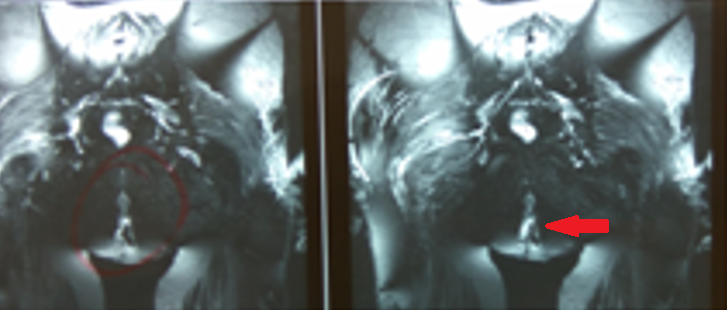
Postoperative imaging of ileorectal anastomosis (modified Duhamel). The anastomosis of the terminal ileum to the anterior wall of the remaining rectal stump is evident (Courtesy Dr. V. Penopoulos)

Postoperative imaging of ileorectal anastomosis (modified Duhamel). The anastomosis of the terminal ileum to the anterior wall of the remaining rectal stump is evident (Courtesy Dr. V. Penopoulos)
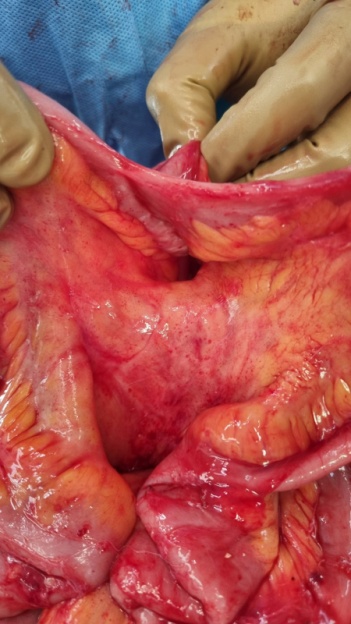
Total colectomy specimen. Red arrow: previous colocolonic anastomosis (Courtesy Dr. V. Penopoulos)

Postoperative imaging of ileorectal anastomosis (modified Duhamel). The anastomosis of the terminal ileum to the anterior wall of the remaining rectal stump is evident (Courtesy Dr. V. Penopoulos)
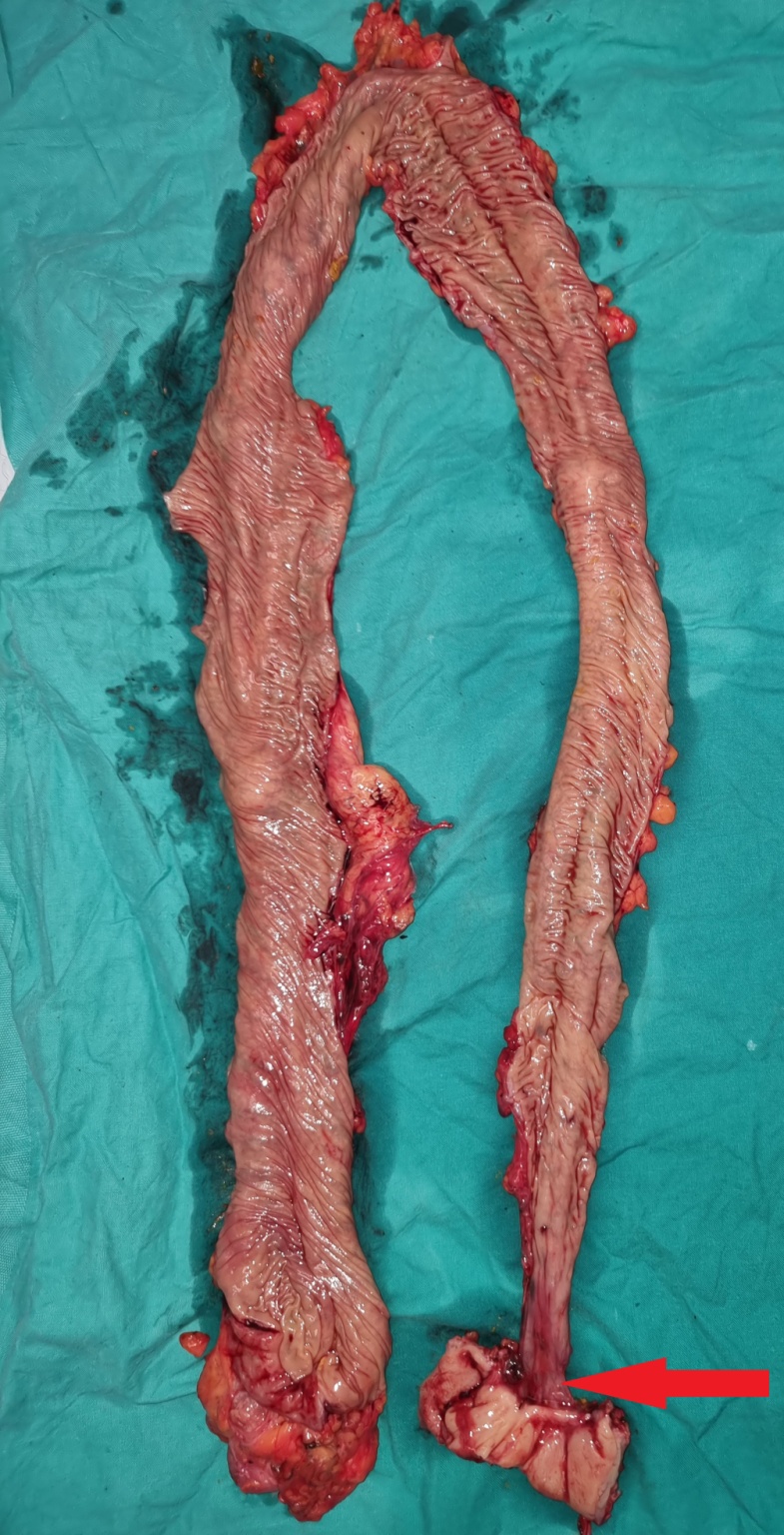
Total colectomy specimen. Red arrow: previous colocolonic anastomosis (Courtesy Dr. V. Penopoulos)

Postoperative imaging of ileorectal anastomosis (modified Duhamel). The anastomosis of the terminal ileum to the anterior wall of the remaining rectal stump is evident (Courtesy Dr. V. Penopoulos)

Postoperative imaging of ileorectal anastomosis (modified Duhamel). The anastomosis of the terminal ileum to the anterior wall of the remaining rectal stump is evident (Courtesy Dr. V. Penopoulos)

Postoperative imaging of ileorectal anastomosis (modified Duhamel). The anastomosis of the terminal ileum to the anterior wall of the remaining rectal stump is evident (Courtesy Dr. V. Penopoulos)

Postoperative imaging of ileorectal anastomosis (modified Duhamel). The anastomosis of the terminal ileum to the anterior wall of the remaining rectal stump is evident (Courtesy Dr. V. Penopoulos)
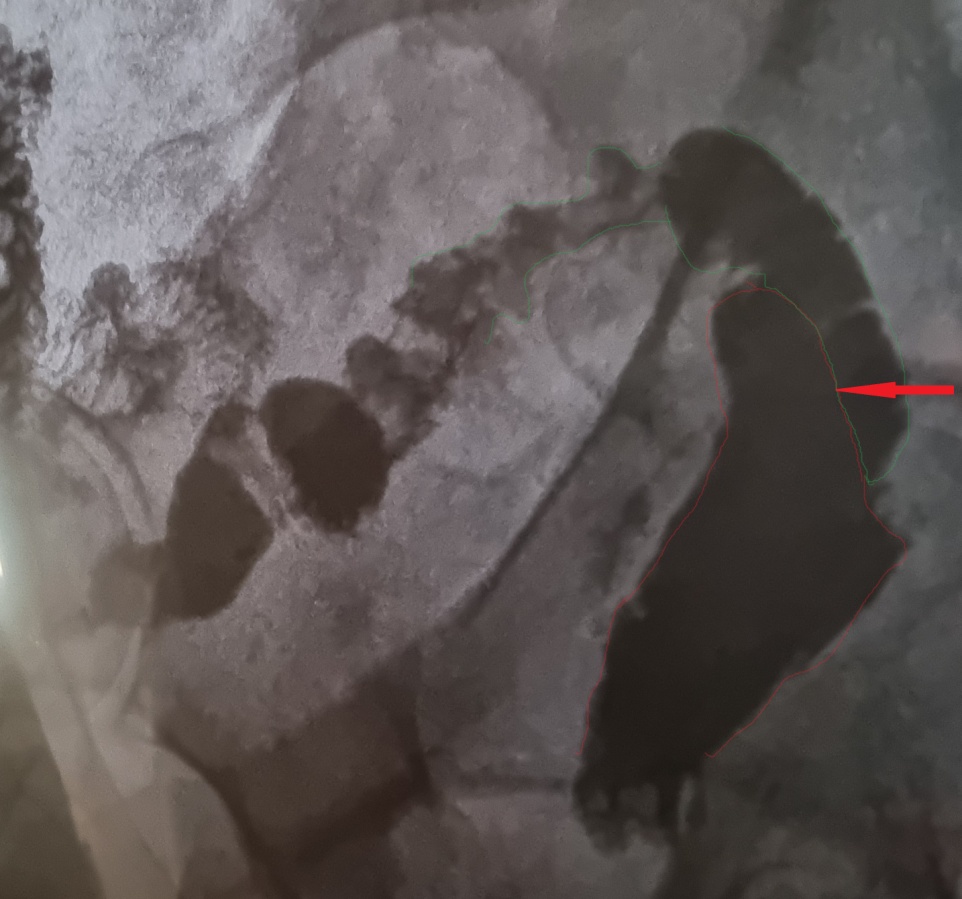
Postoperative imaging of ileorectal anastomosis (modified Duhamel). The anastomosis of the terminal ileum to the anterior wall of the remaining rectal stump is evident (Courtesy Dr. V. Penopoulos)
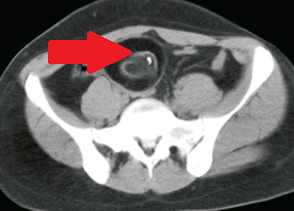
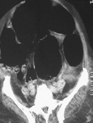
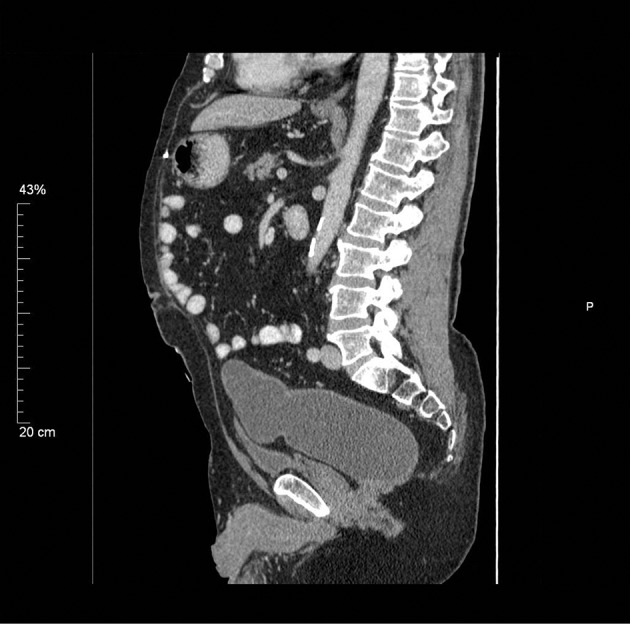
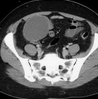
Abdominal CT scan. Presence of calcifications, cystic-solid areas, and adipose tissue, suggestive of a right-sided teratoma (Courtesy Dr. V. Penopoulos)
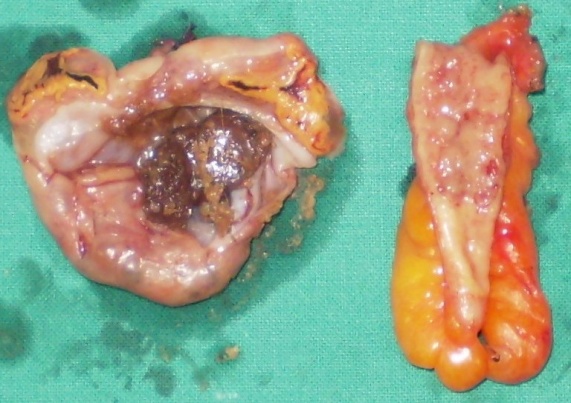
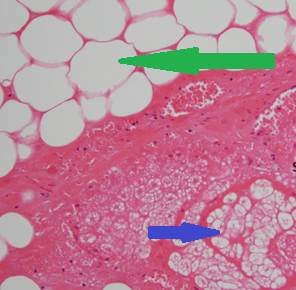
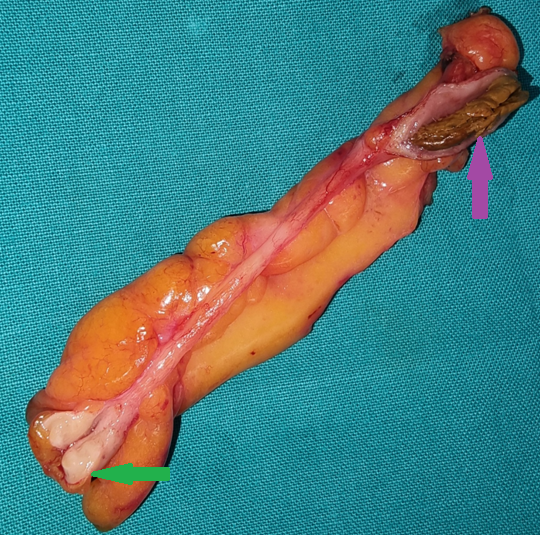
Green arrow: Adipose tissue. Purple arrow: Sebaceous glands (Courtesy Dr. V. Penopoulos)
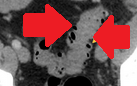
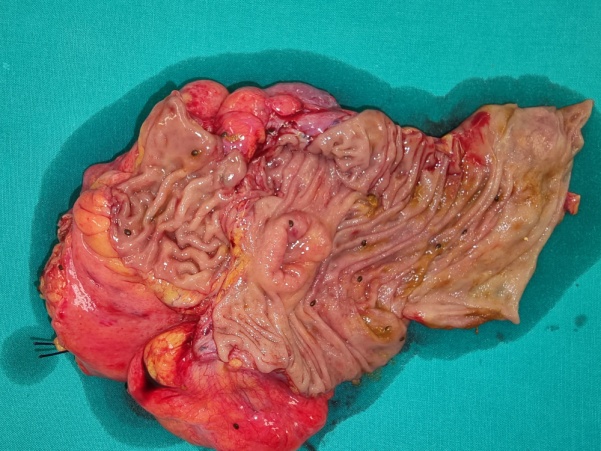
Non-inflamed diverticula in the colon segment immediately beneath the exteriorized end colostomy (Courtesy Dr. V. Penopoulos)
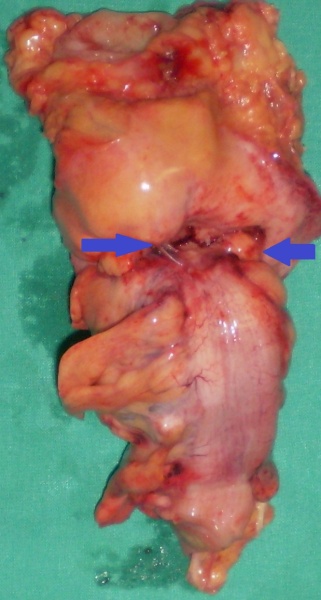
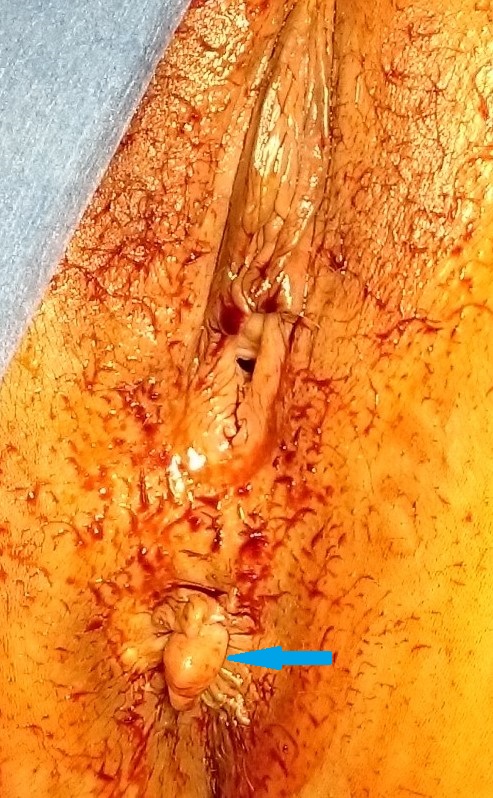
Excised end colostomy segment. Blue arrows — Diverticular sites (Courtesy Dr. V. Penopoulos)
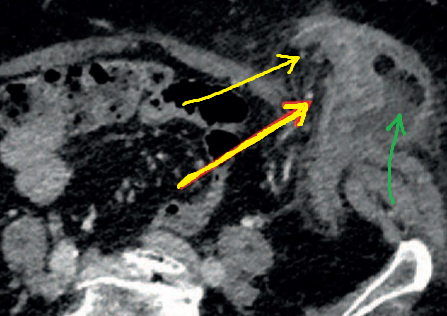
Yellow arrows — Inflamed diverticula in the extra-abdominal bowel segment. Green arrow — Fluid collection (Courtesy Dr. V. Penopoulos)
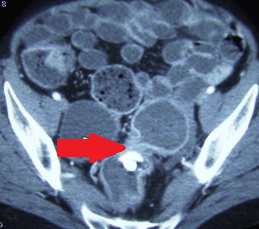
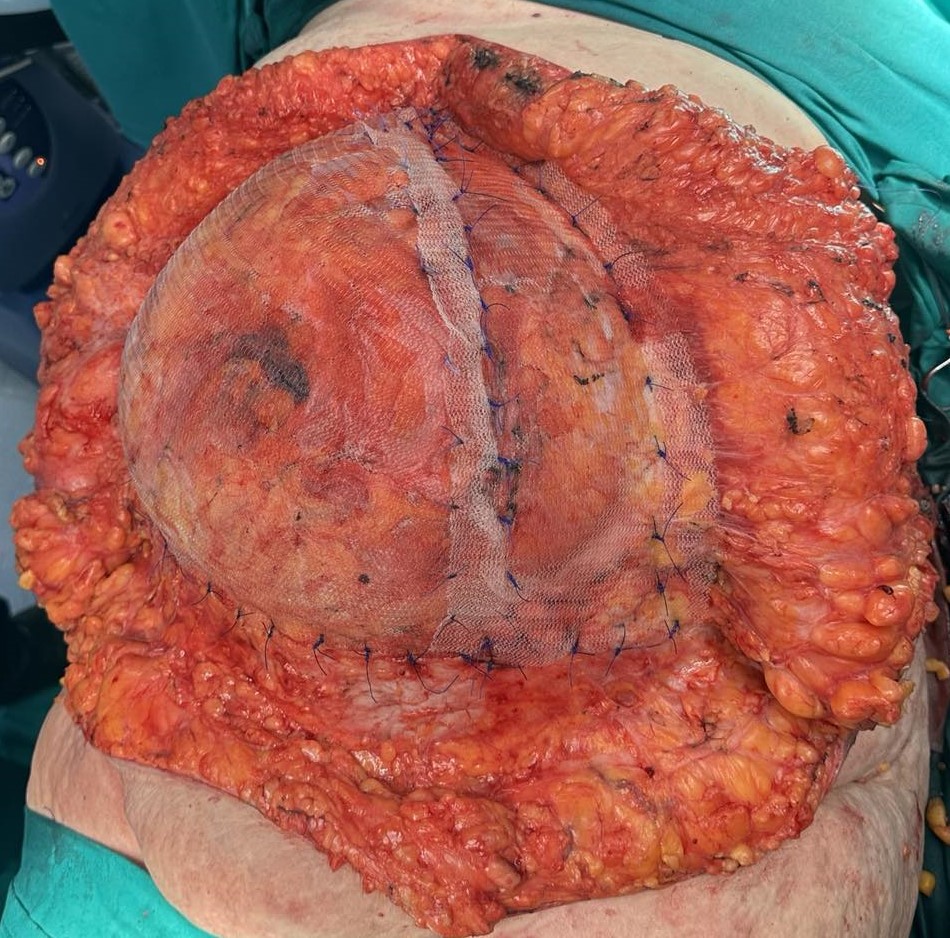
Abdominal CT scan. Erosion/migration of the mesh within the rectum (Courtesy Dr. V. Penopoulos)
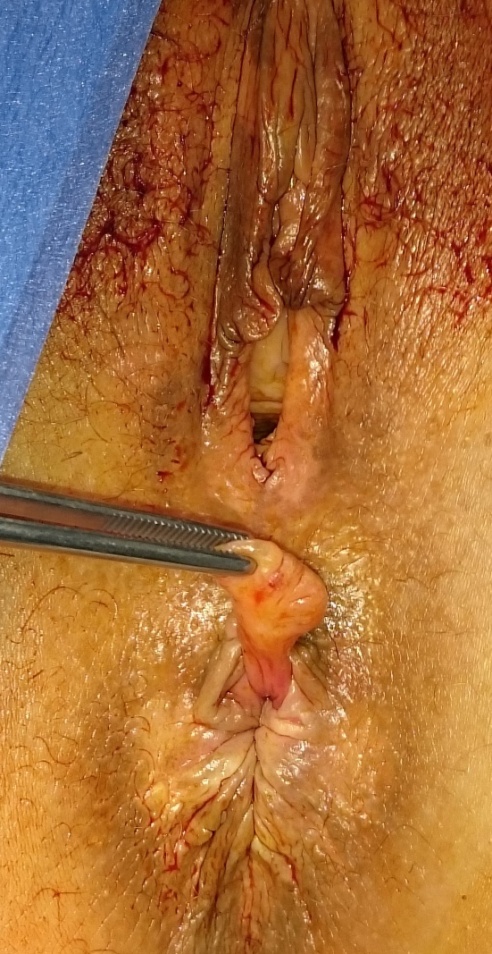
Inflammatory cloacogenic polyp with inflammatory fibromuscular stroma and hyperplastic epithelium (Courtesy Dr. V. Penopoulos)
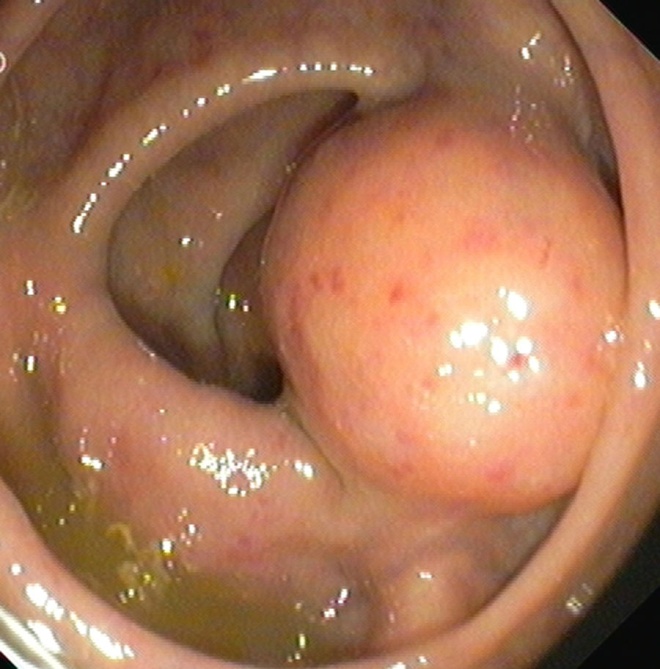
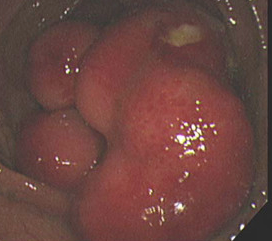
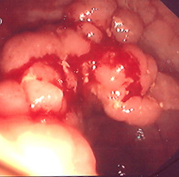
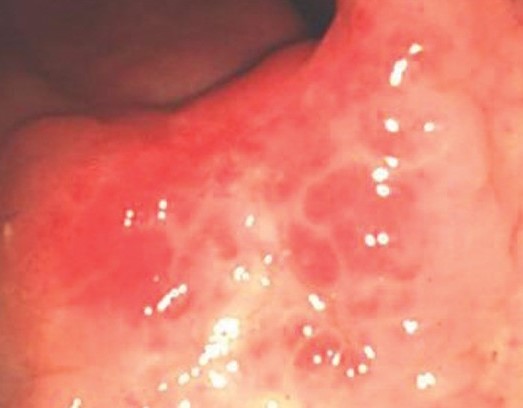
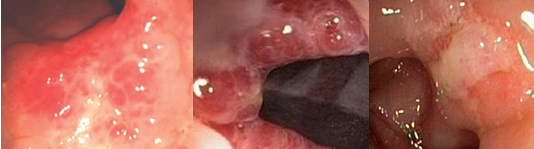
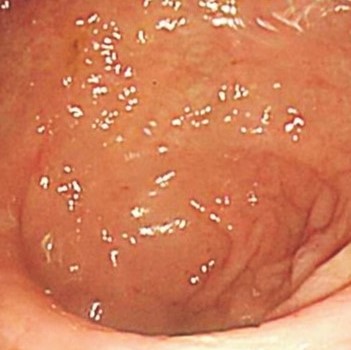
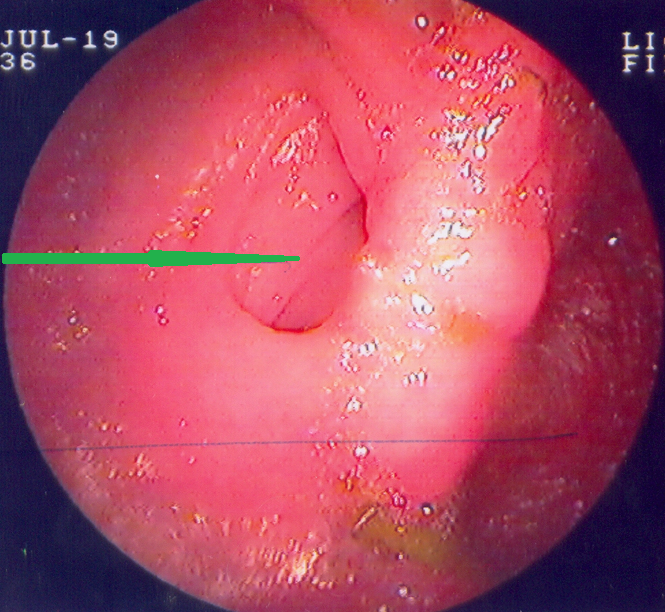
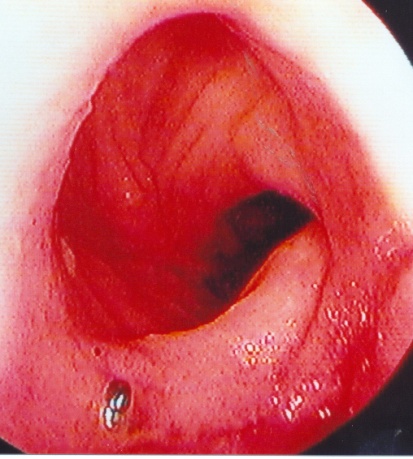
Colonoscopy revealing a polypoid mass protruding in the medial aspect of the left colonic flexure
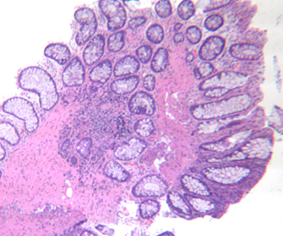
Inflammatory cloacogenic polyp with inflammatory fibromuscular stroma and hyperplastic epithelium (Courtesy Dr. V. Penopoulos)
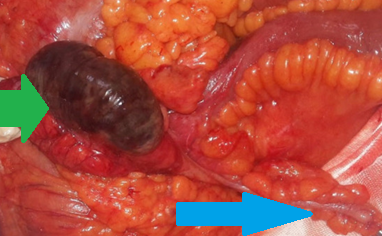
Green arrow: necrosis of the cecum. Blue arrow: normal appendix (Courtesy Dr. V. Penopoulos)
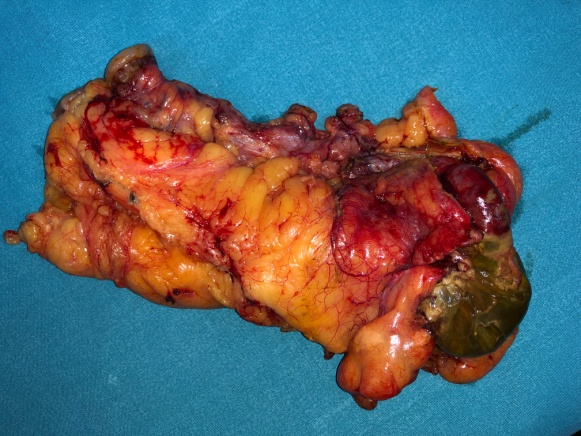
Surgical specimen. Necrosis of a portion of the cecum is evident (Courtesy Dr. V. Penopoulos)
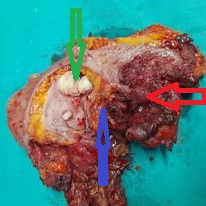
Excised specimen en bloc . Red arrow rectosigmoid adenocarcinoma . Green arrow uterus – uterine fibroids . Purple arrow , hidden left ovarian psammocarcinoma (Courtesy Dr. V. Penopoulos)
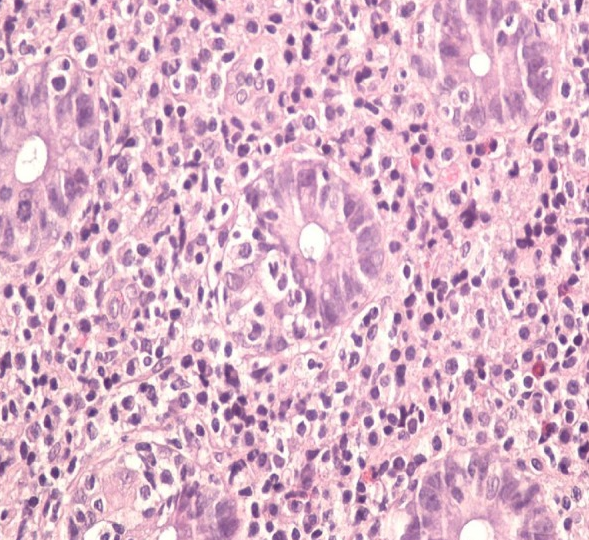
Microscopic picture showing extensive psammoma body formation (Courtesy Dr. V. Penopoulos)
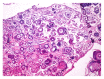
Microscopic picture showing extensive psammoma body formation (Courtesy Dr. V. Penopoulos)
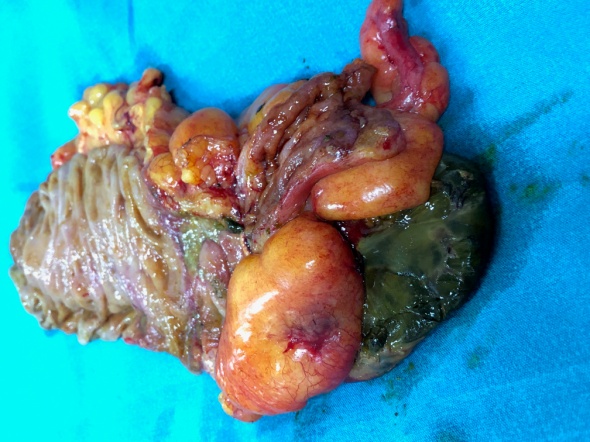
Surgical specimen. Necrosis of a portion of the cecum is evident (Courtesy Dr. V. Penopoulos)

Microscopic picture showing extensive psammoma body formation (Courtesy Dr. V. Penopoulos)
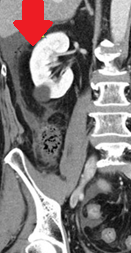
Green arrow: necrosis of the cecum. Blue arrow: normal appendix (Courtesy Dr. V. Penopoulos)
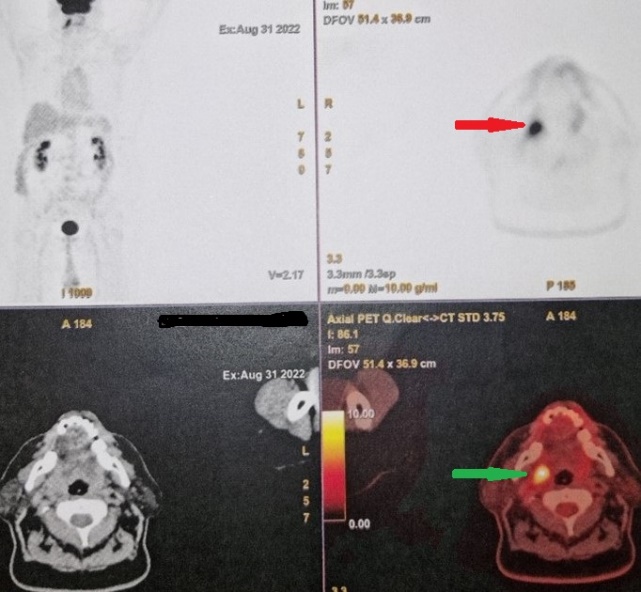
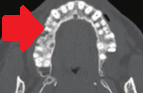
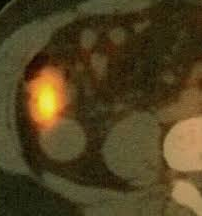
PET Scan . Metastatic carcinoma in the right palatine tonsil (Courtesy Dr. V. Penopoulos).
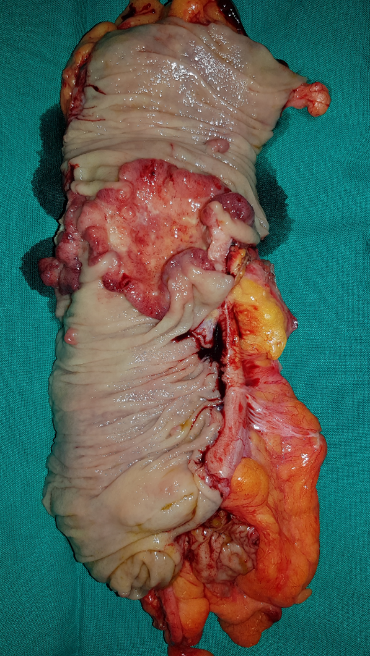
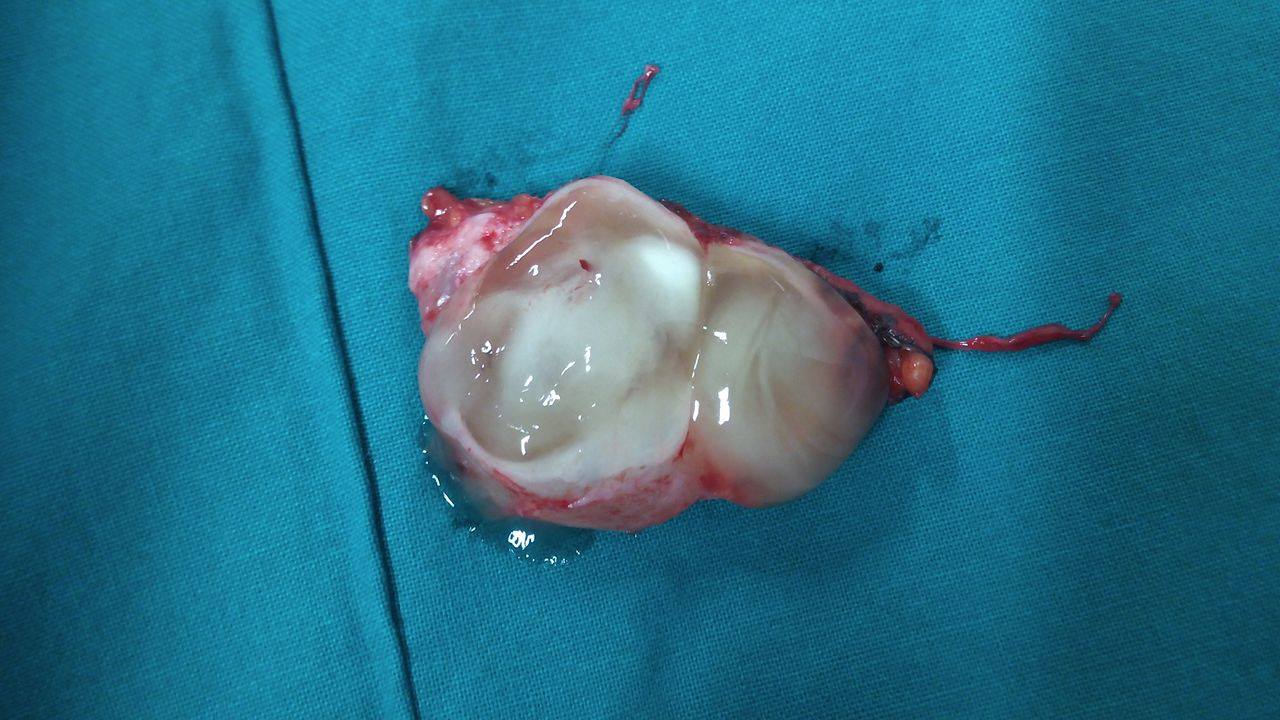
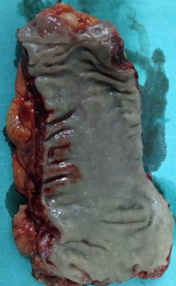
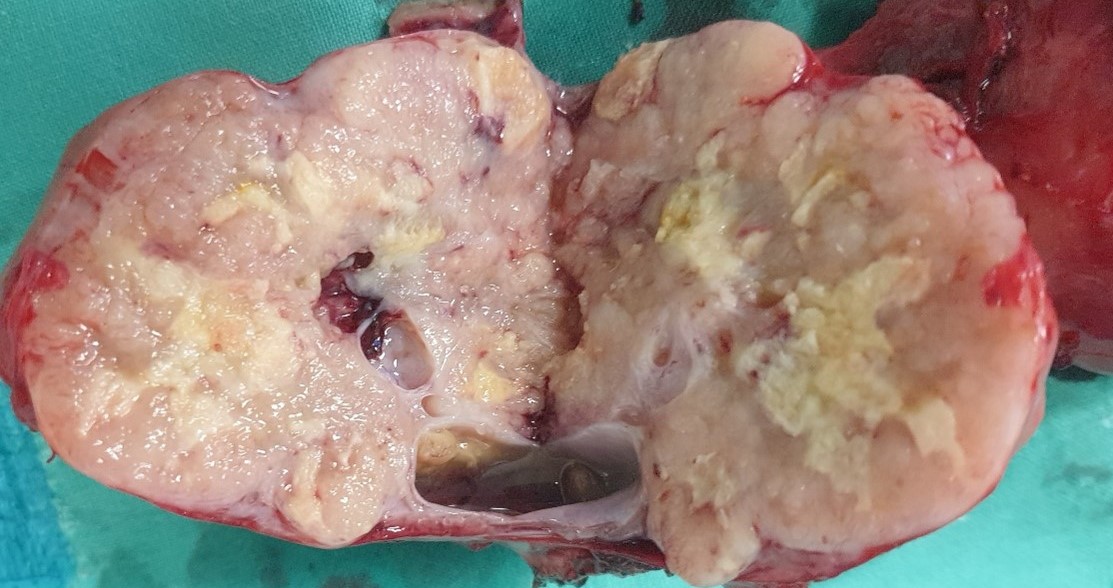
Macroscopic appearance of the ovary following total hysterectomy in a 46-year-old woman with metachronous ovarian metastases diagnosed two years after right hemicolectomy for ascending colon carcinoma (CRC). The macroscopic appearance of the ovarian tumor shows cystic and solid areas (Courtesy Dr. V. Penopoulos)
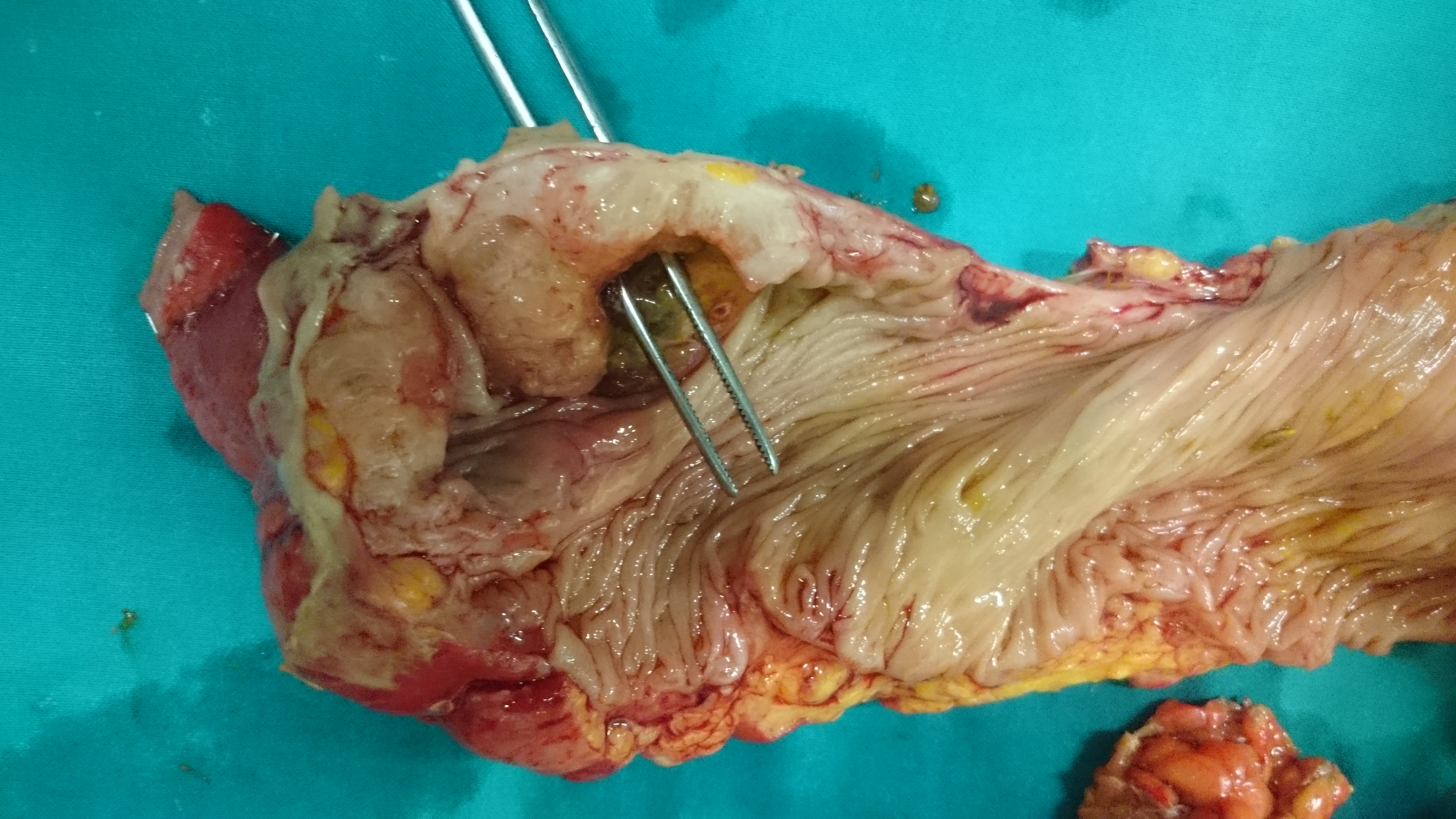
Perforation of caecum secondary to coexisting descending sigmoid colon stenosis obstruction (Courtesy Dr. V. Penopoulos)
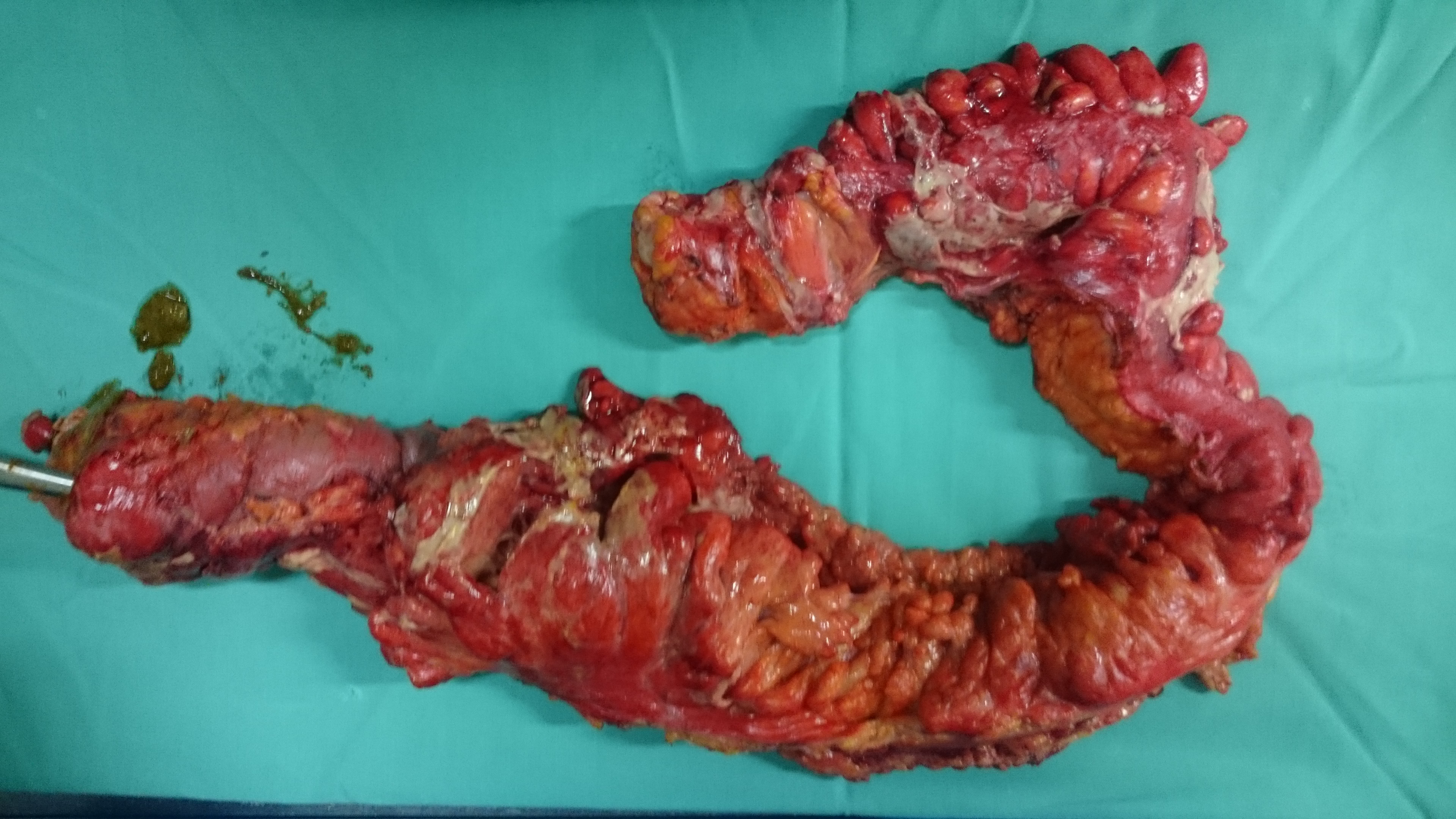
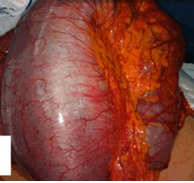
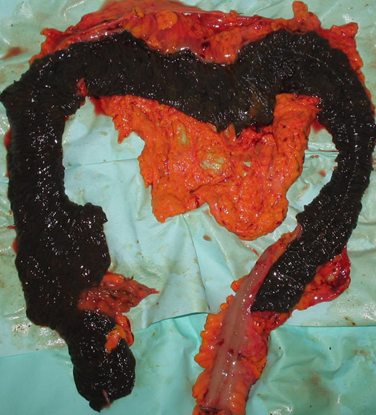
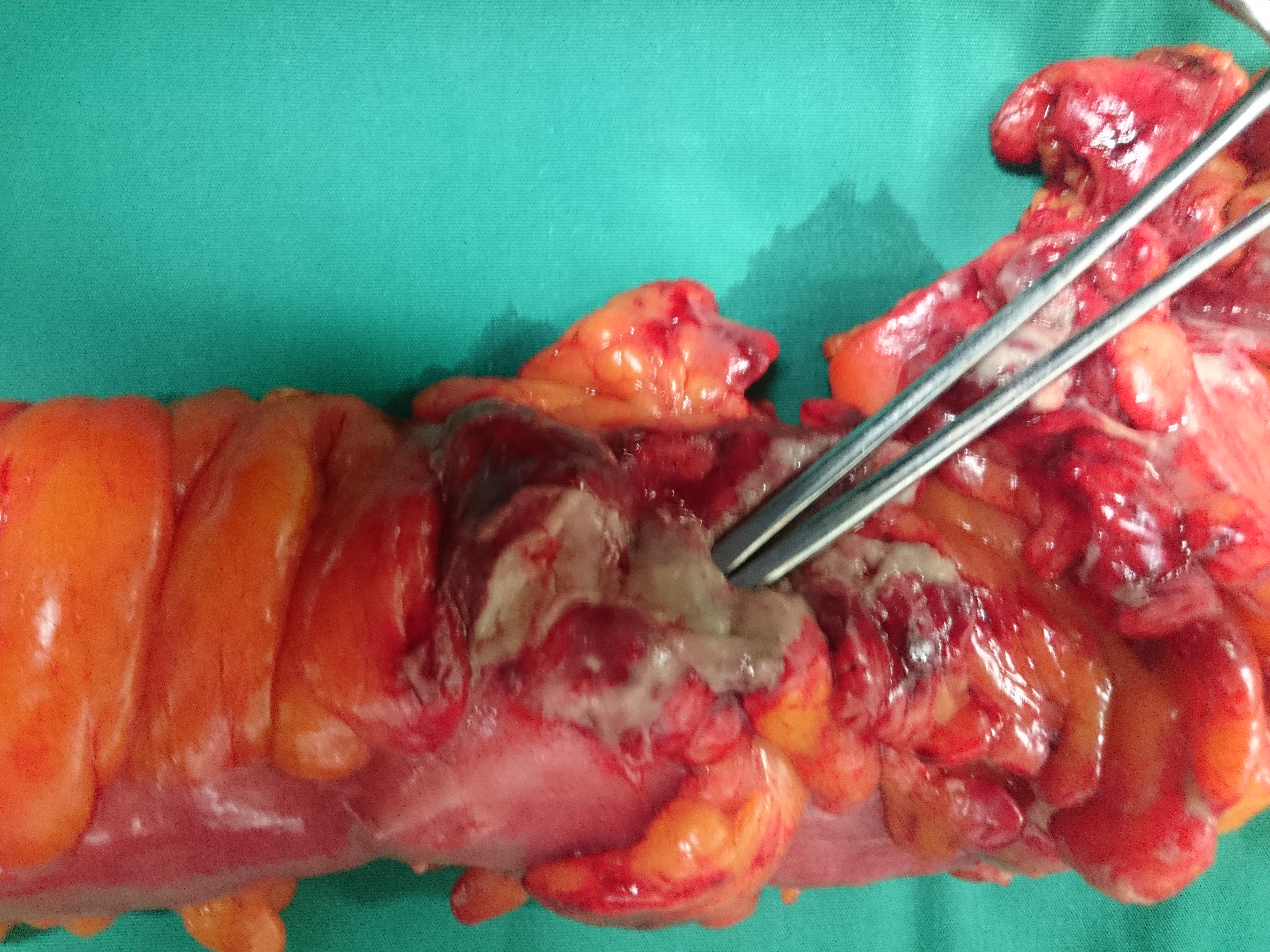
Extreme inflammation of left hemicolon secondary to diverticulitis and covered perforations (Courtesy Dr. V. Penopoulos)
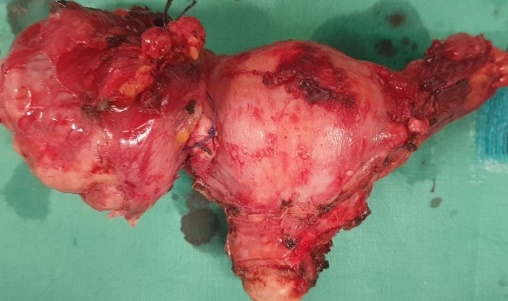
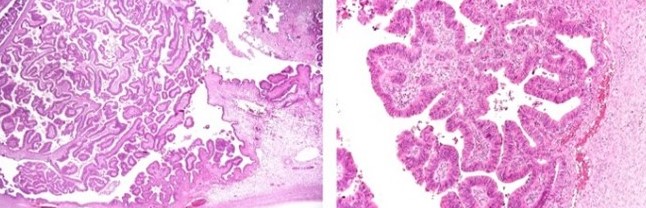
Photomicrographs of the histopathology of the ovarian tumor tissue shows solid areas consisting mainly of papillary structures and few glands that are covered by a layer of malignant epithelial cells (Courtesy Dr. V. Penopoulos)
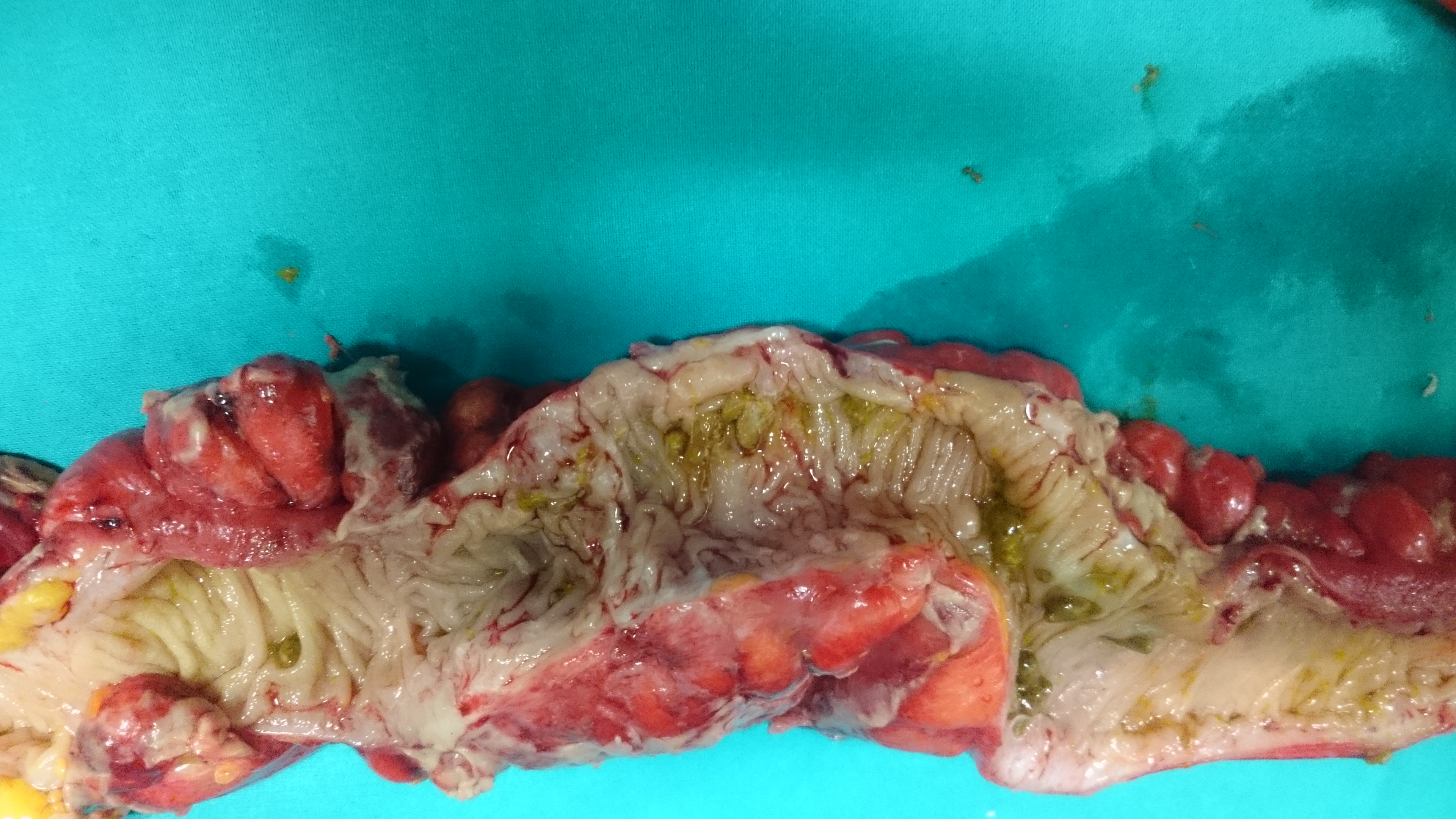
Extreme inflammation of left hemicolon secondary to diverticulitis and covered perforations (Courtesy Dr. V. Penopoulos)
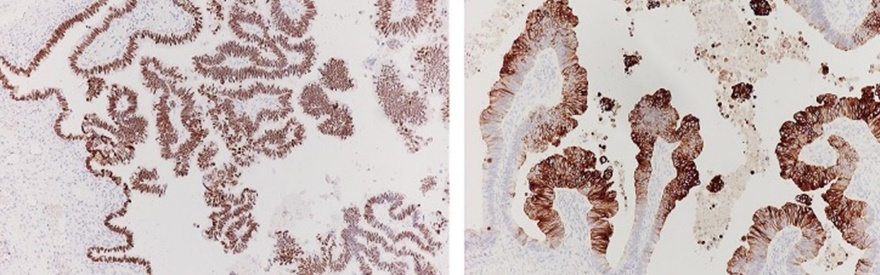
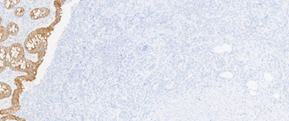
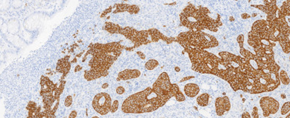
Positive immunohistochemistry for CDX2 and cytokeratin 20 of the ovarian tumor (Courtesy Dr. V. Penopoulos)
Positive immunohistochemistry for CDX2 and cytokeratin 20 of the ovarian tumor (Courtesy Dr. V. Penopoulos)
Positive immunohistochemistry for CDX2 and cytokeratin 20 of the ovarian tumor (Courtesy Dr. V. Penopoulos)
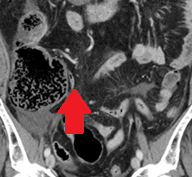
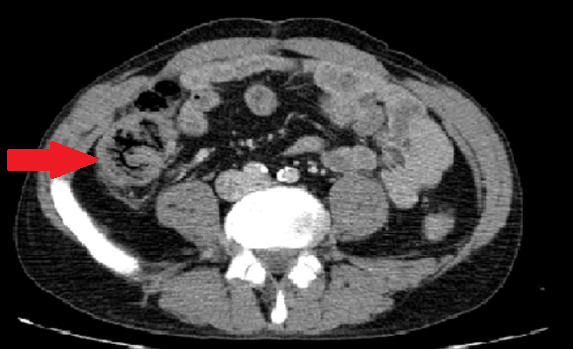
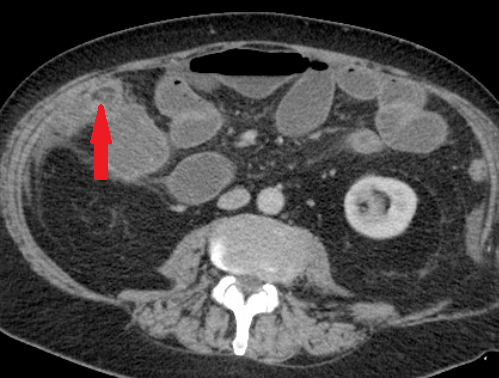
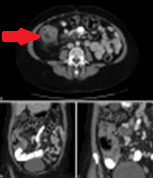
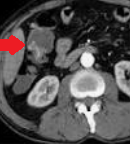
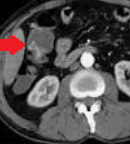
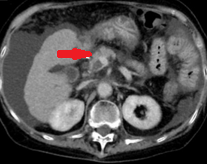
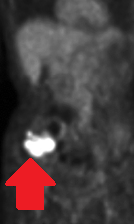
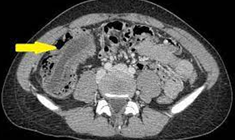
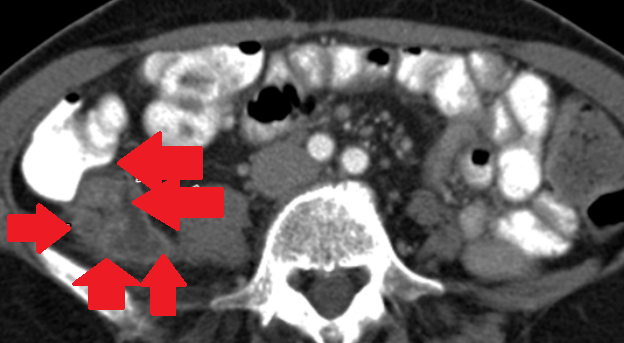
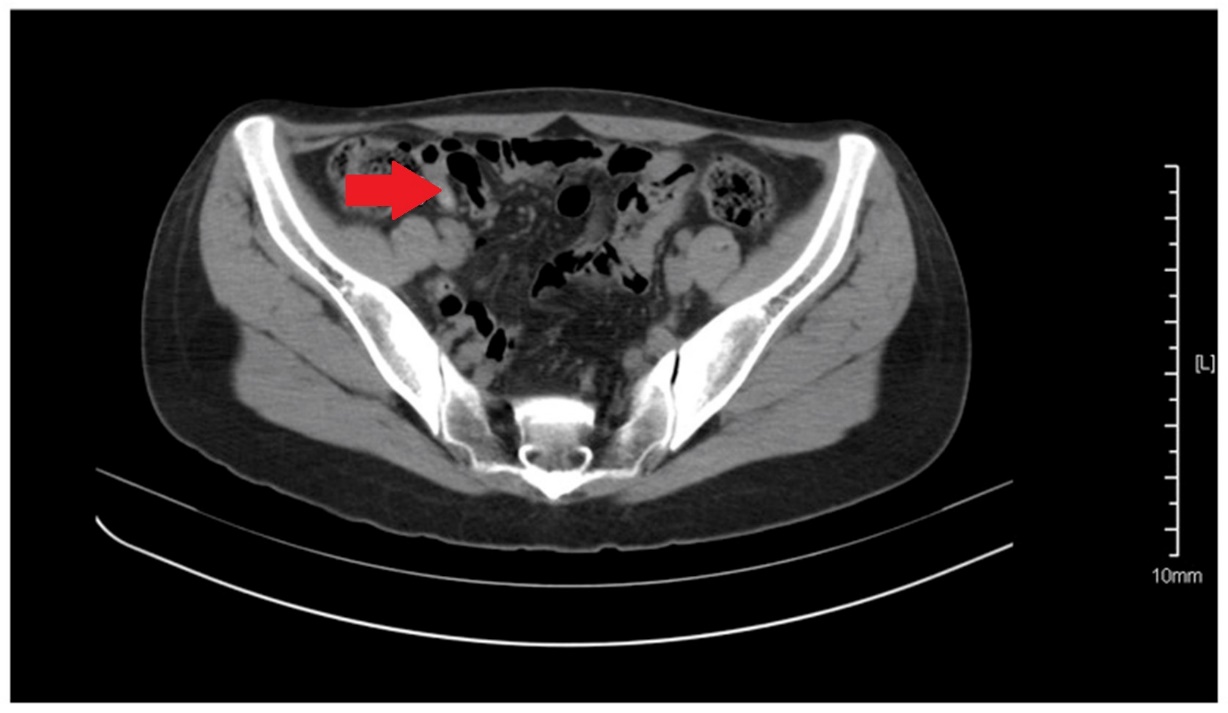
Abdominal CT. Red arrow — Typhlitis. Significant cecal wall thickening (Courtesy Dr. V. Penopoulos)
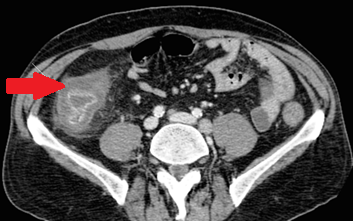
Abdominal CT. Red arrow — Typhlitis. Significant cecal wall thickening (Courtesy Dr. V. Penopoulos)
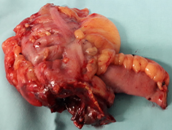
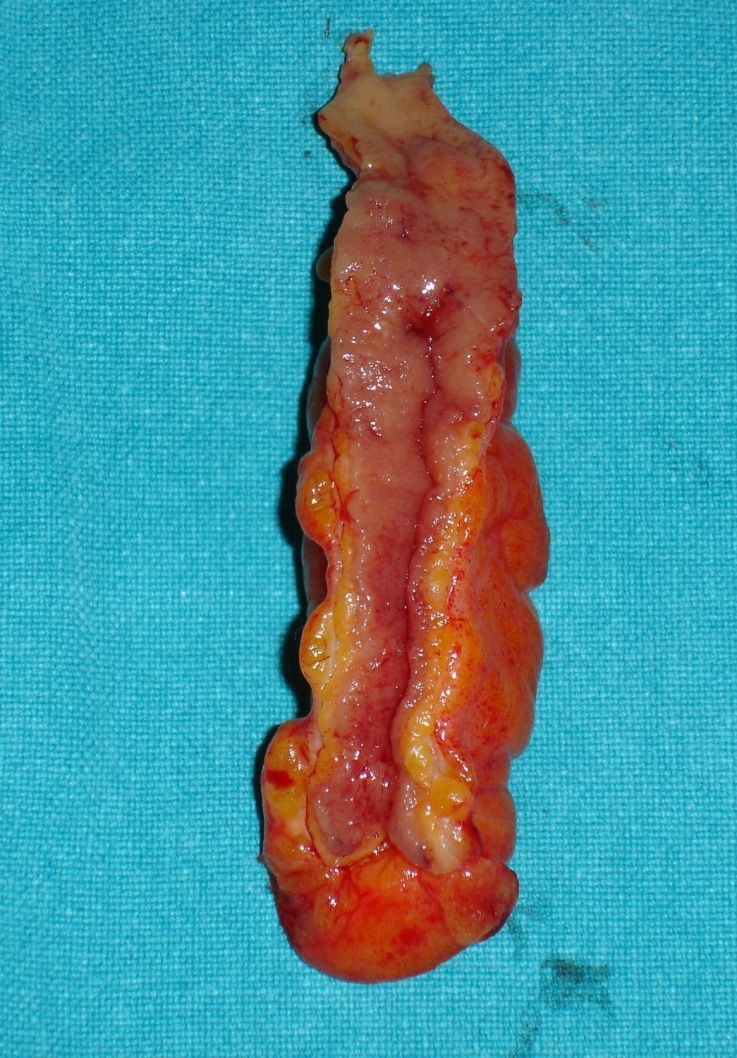
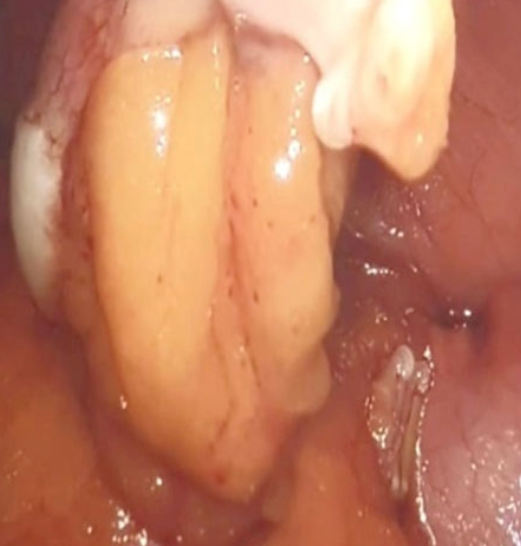
Meckel's diverticulum — Presence of ectopic gastric mucosa (Courtesy Dr. V. Penopoulos)
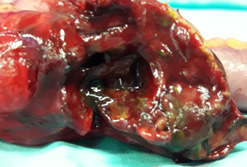
Abdominal CT. Red arrow — Typhlitis. Significant cecal wall thickening (Courtesy Dr. V. Penopoulos)
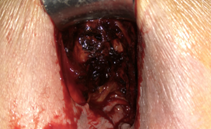
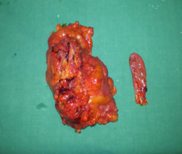
Mini right hemicolectomy specimen — Cecal necrosis and perforation are evident (Courtesy Dr. V. Penopoulos)
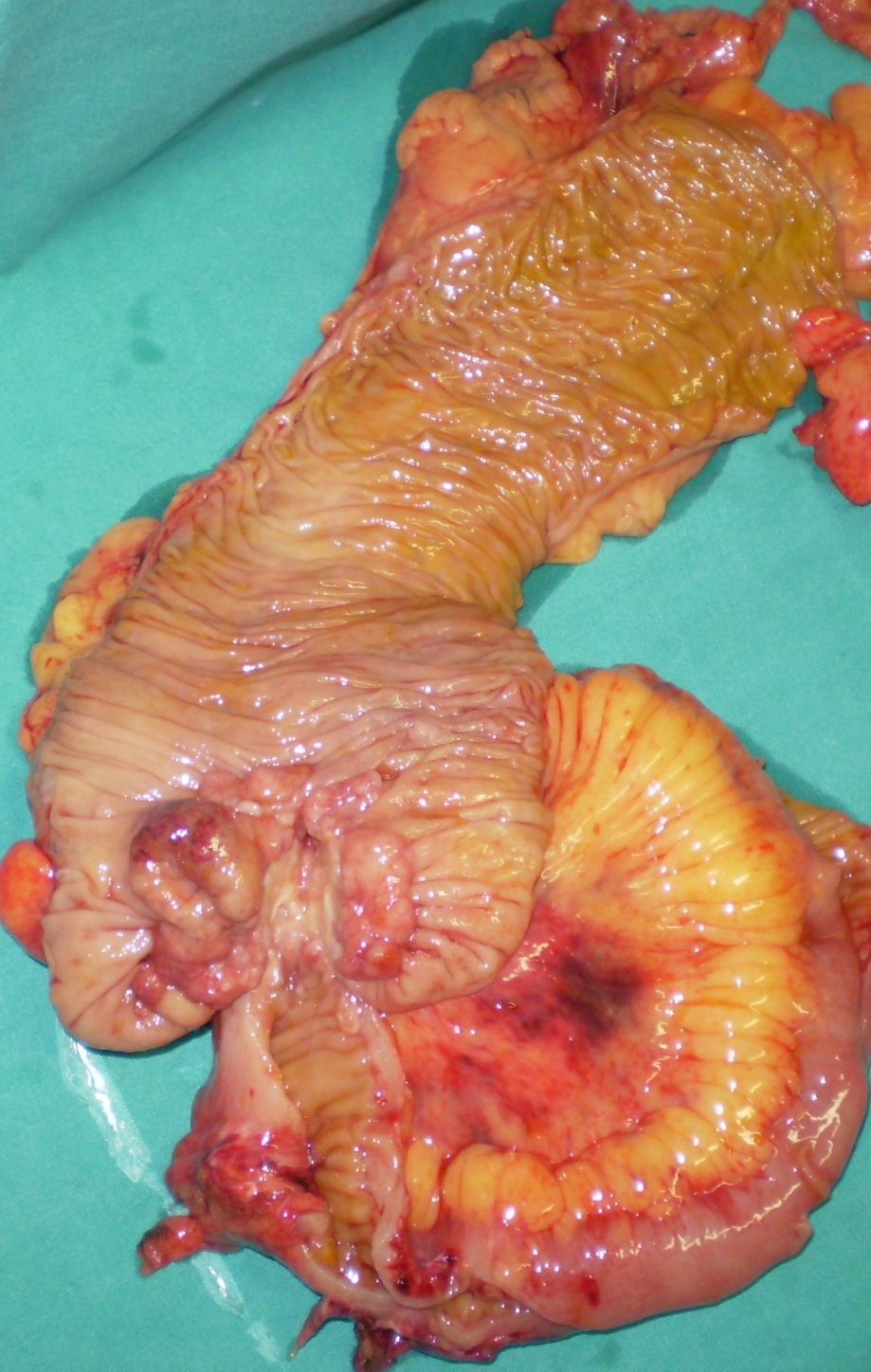
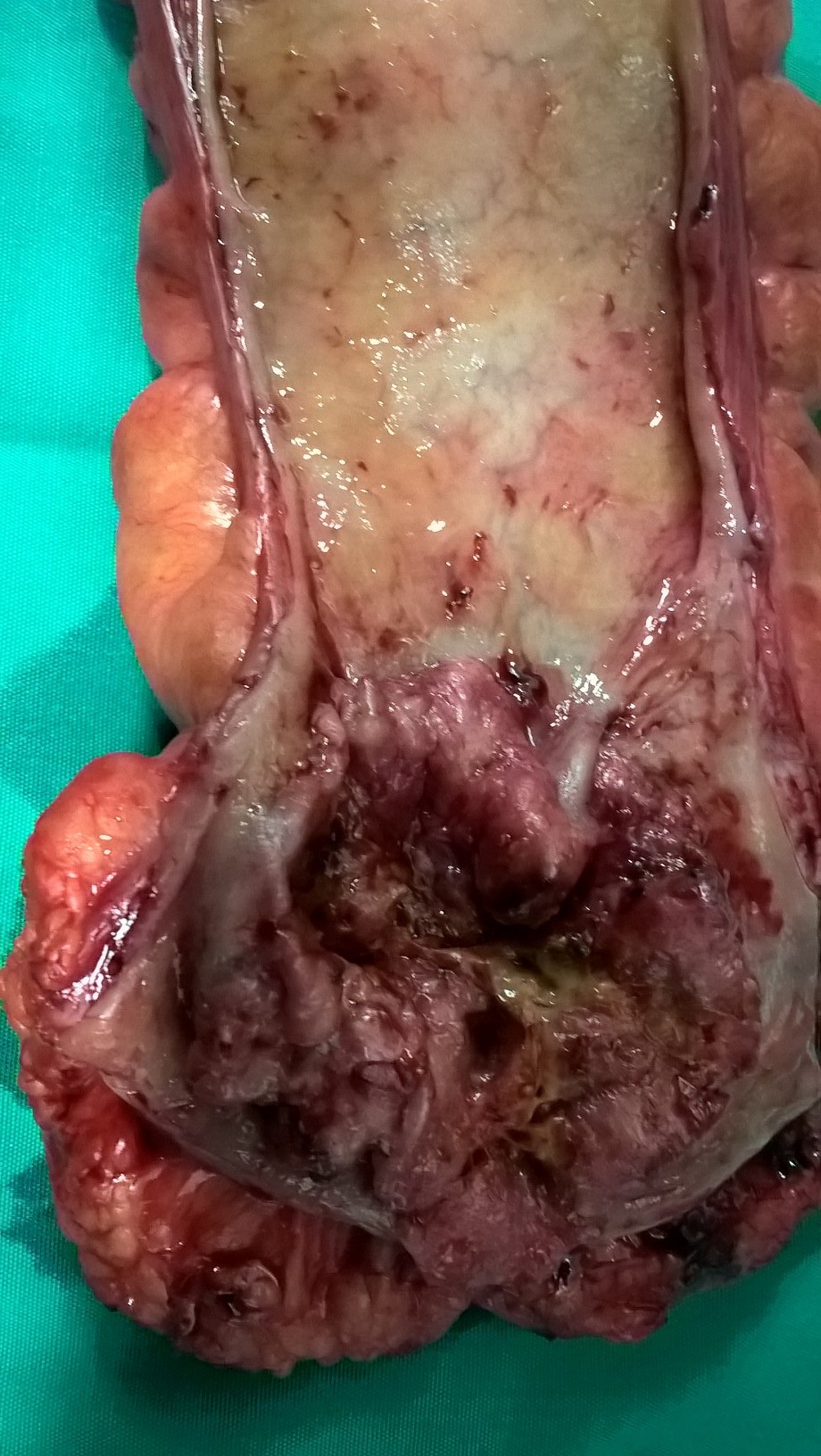
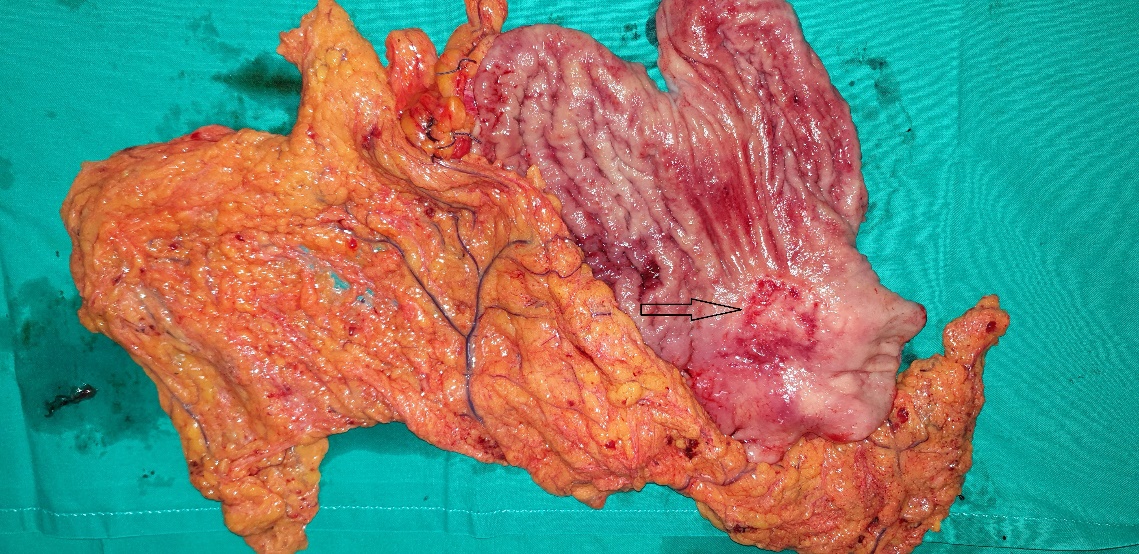
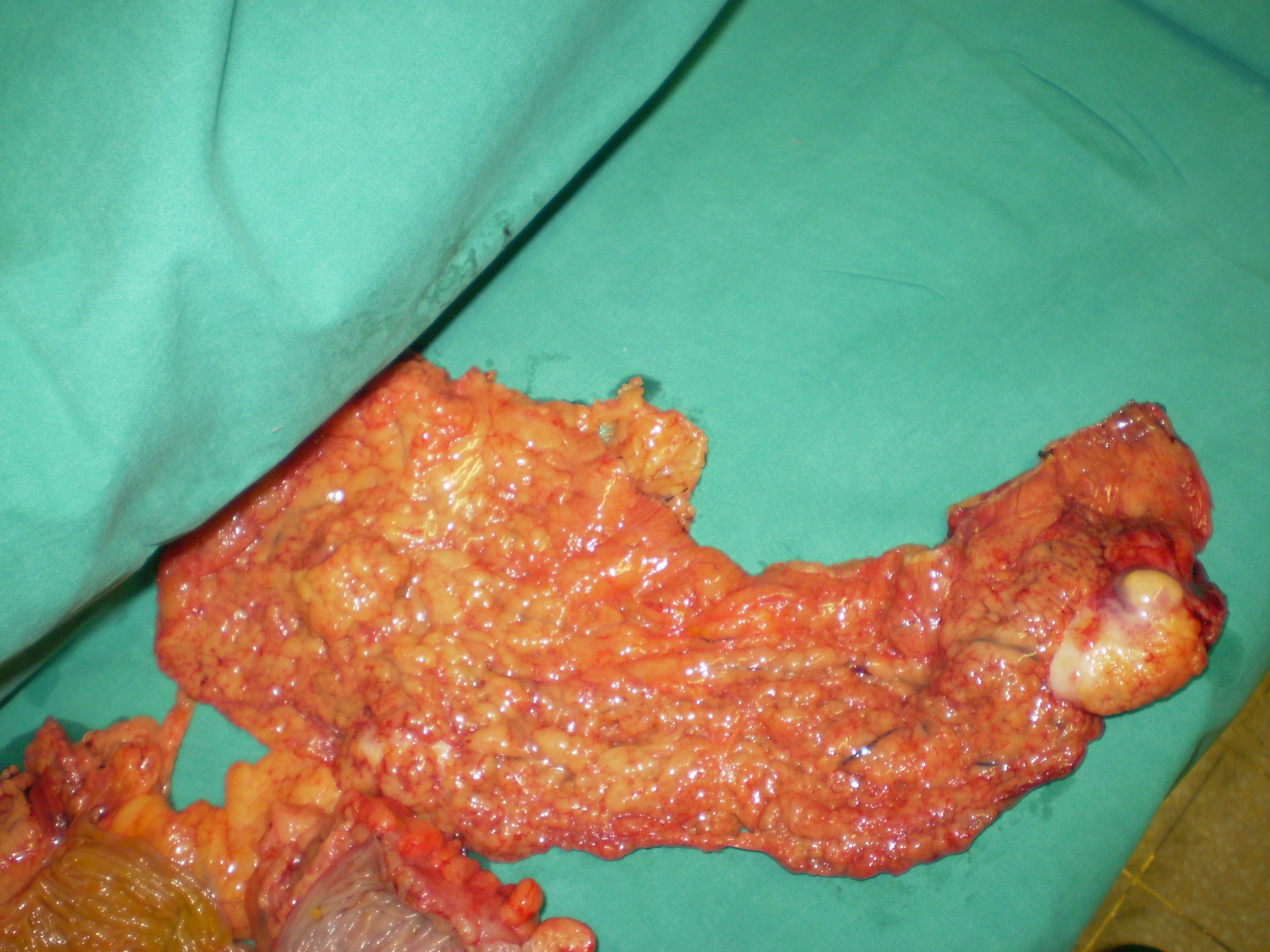
Right hemicolectomy specimen. The cecal neoplasm is clearly visible (Courtesy Dr. V. Penopoulos).
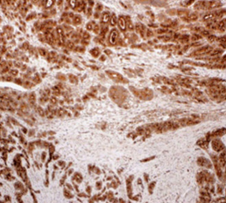
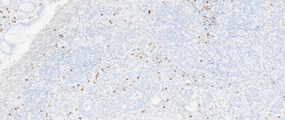
Immunohistochemical examination. Positivity for Chromogranin B (Courtesy Dr. V. Penopoulos).
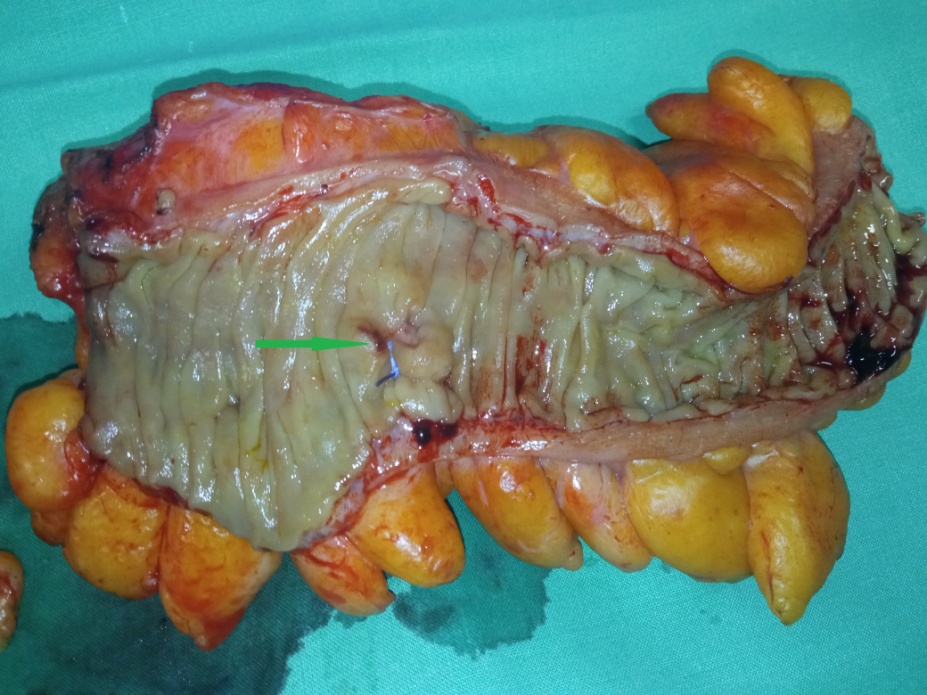
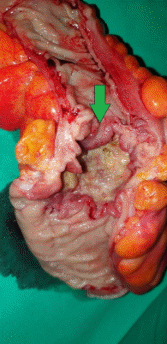
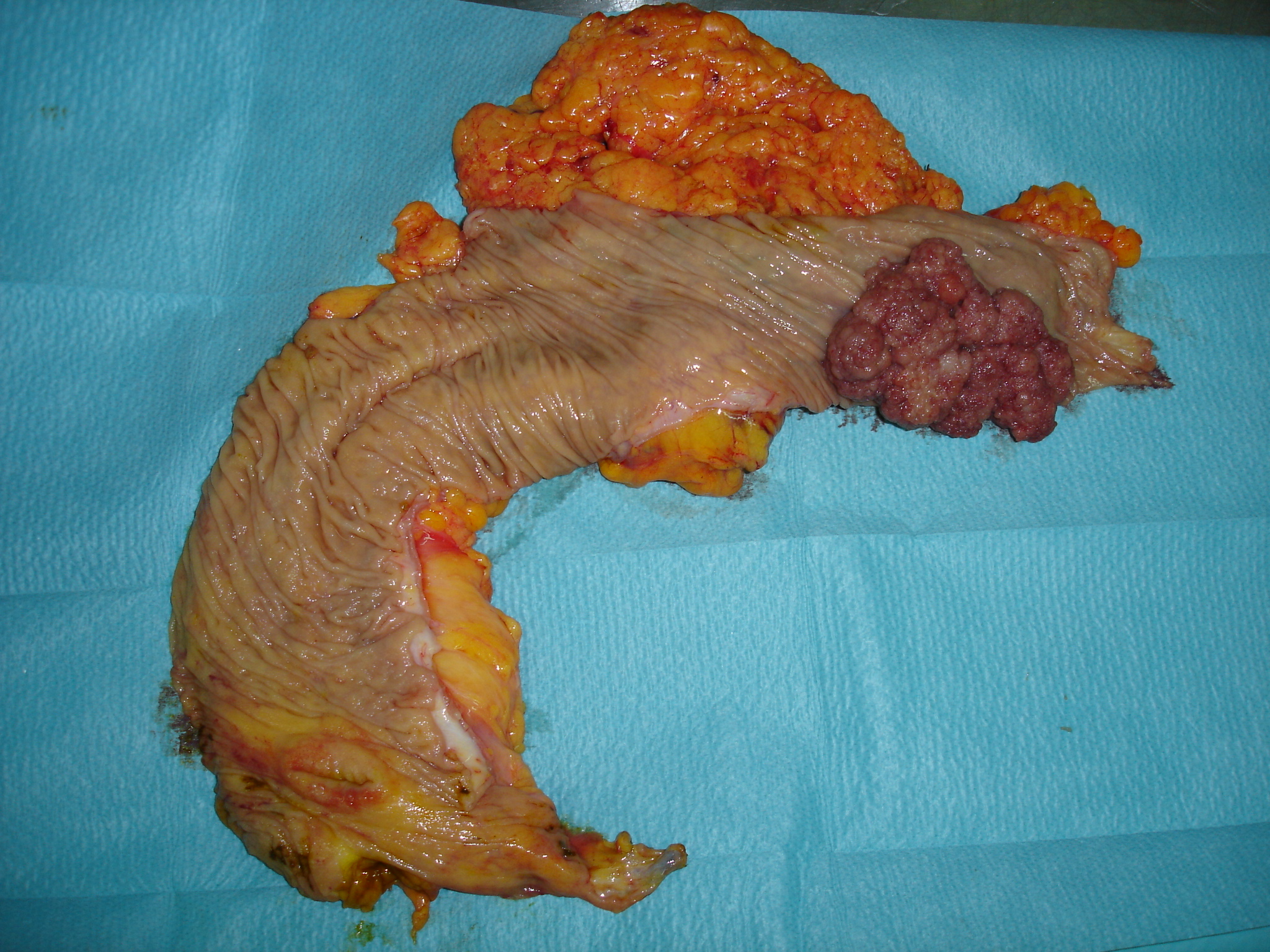
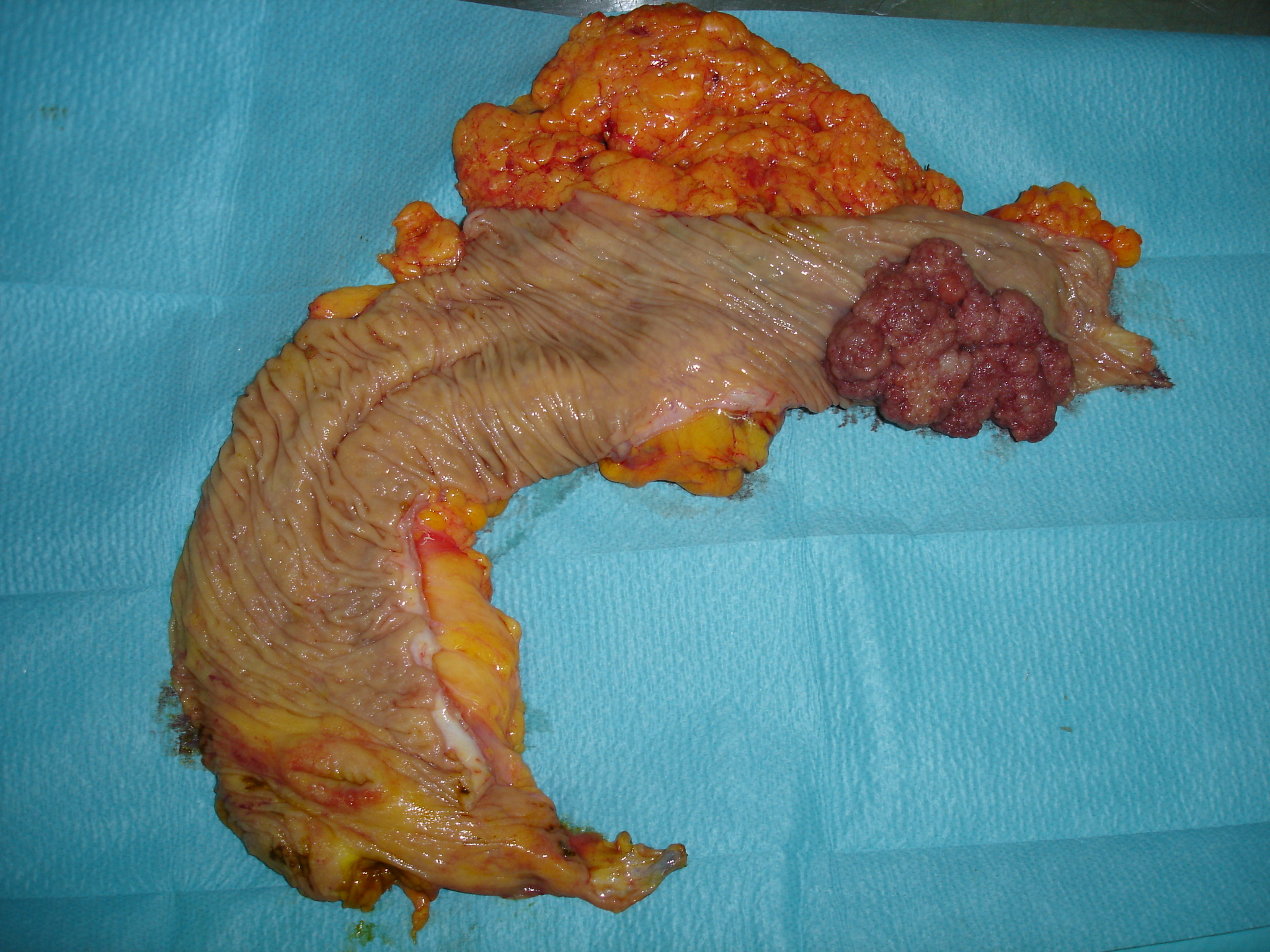
Sigmoid specimen. Green arrow: tubulovillous adenoma that has transformed into adenocarcinoma (Courtesy Dr. V. Penopoulos)
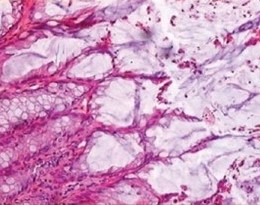
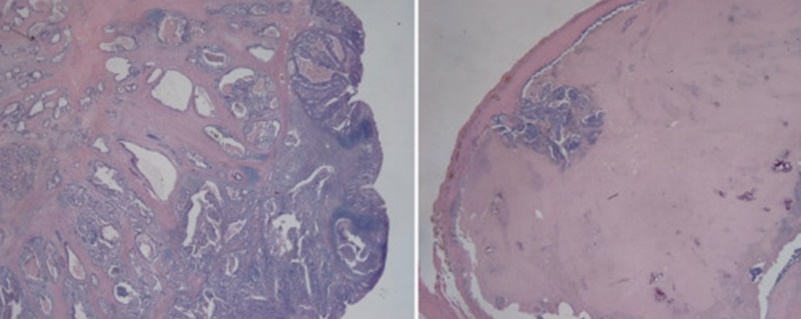
Histological findings of mucinous cystadenoma of the appendix. Cylindrical epithelium and mucin production. Note the absence of atypia and mitotic figures
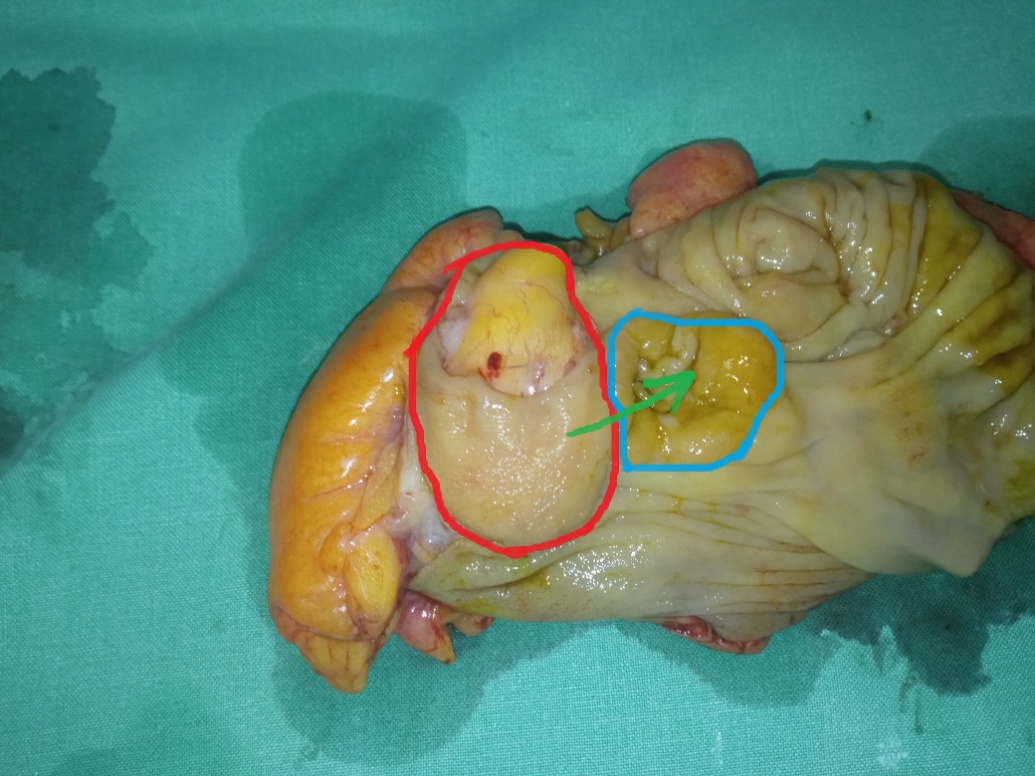
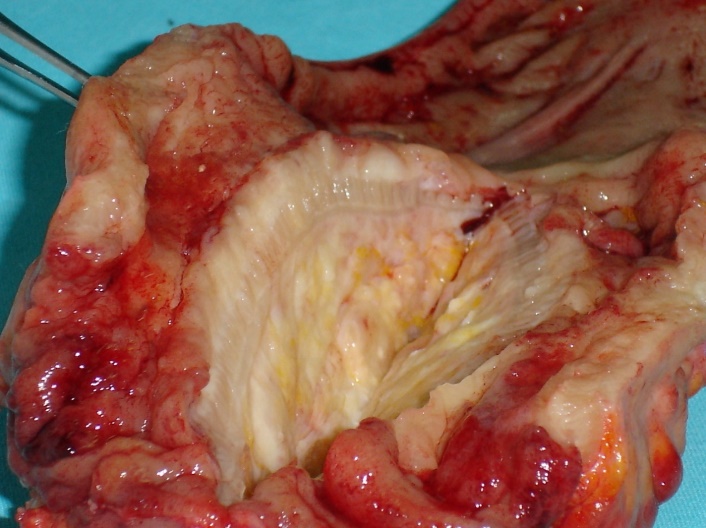
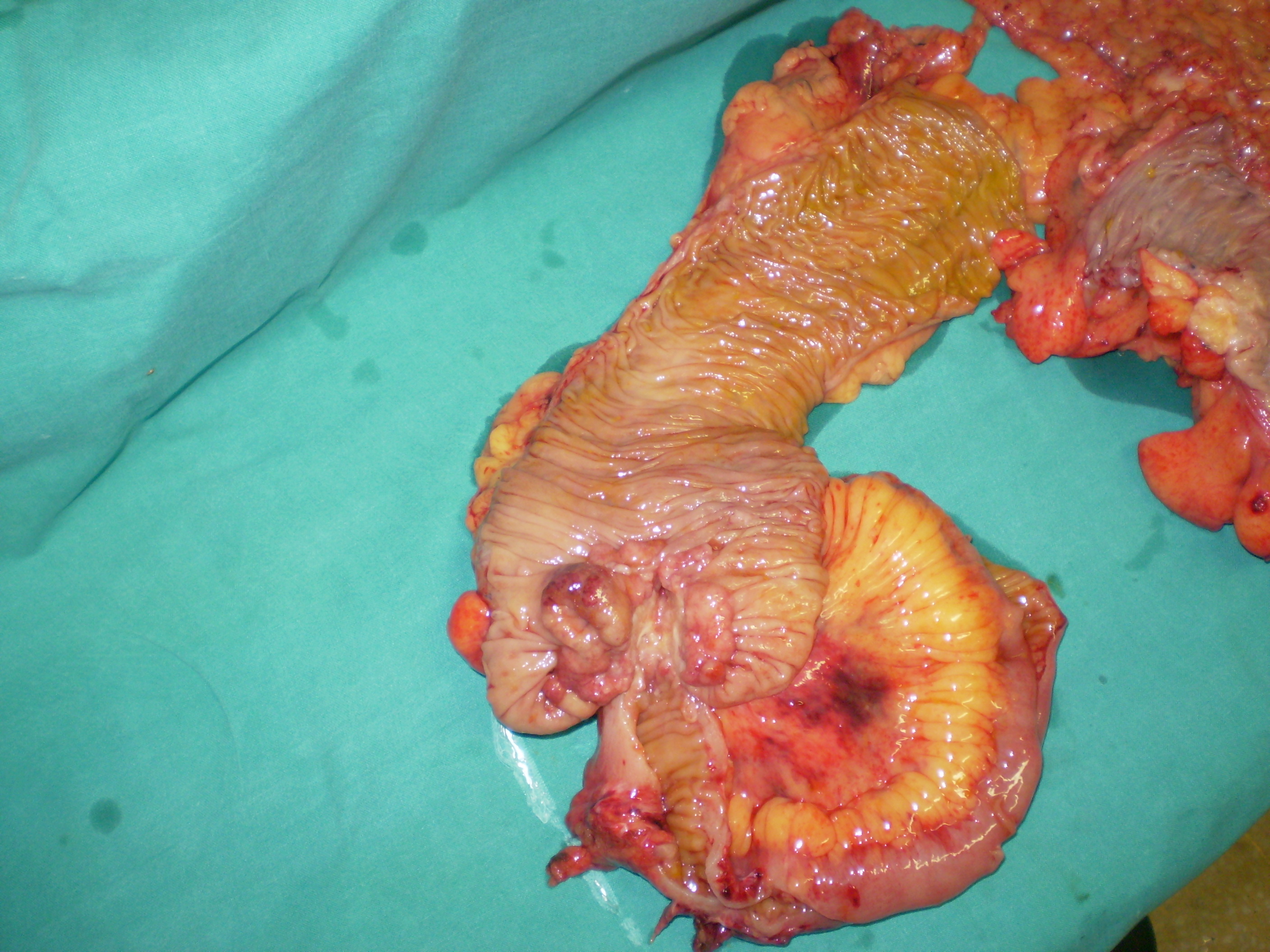
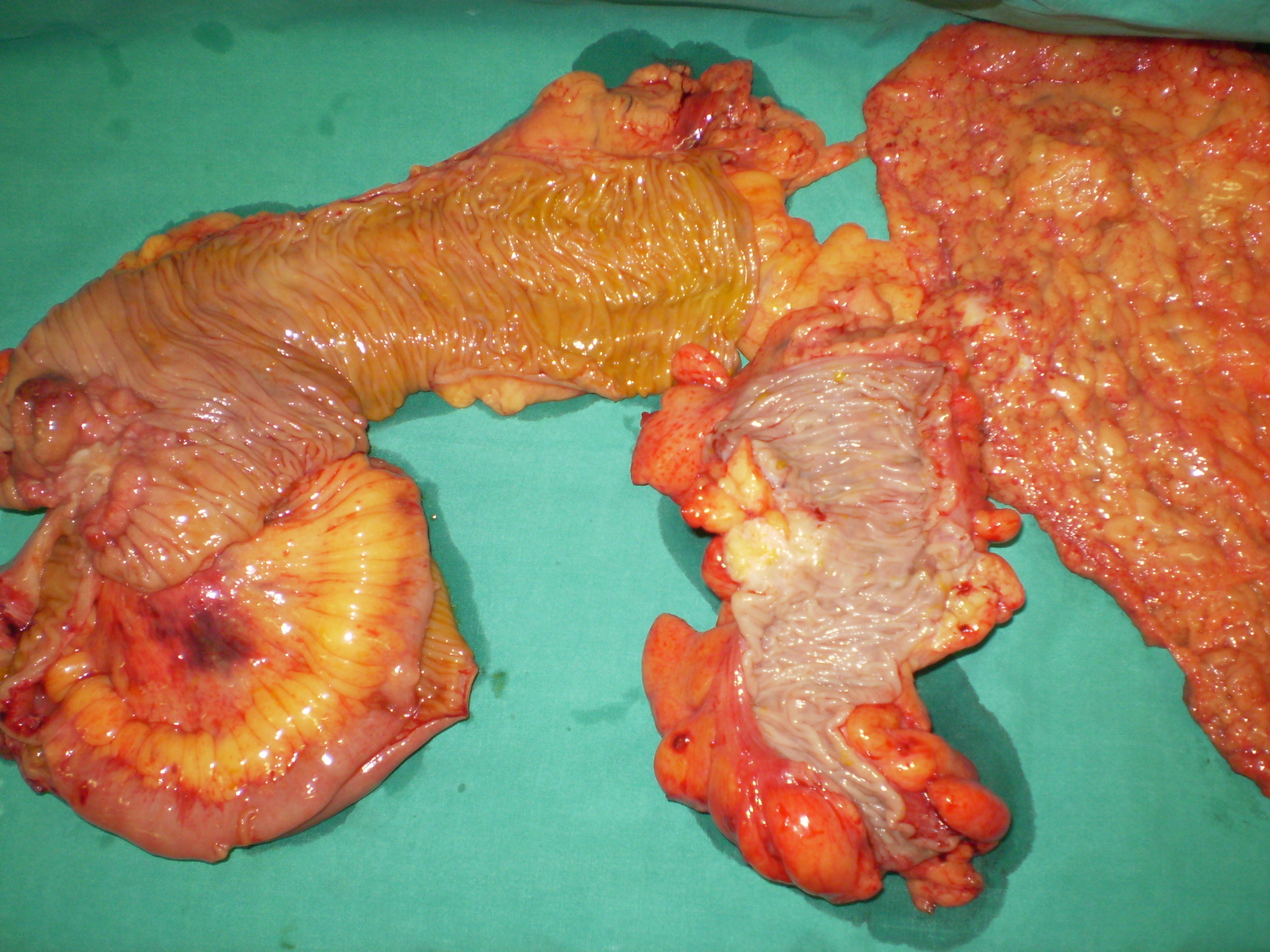
Mini right hemicolectomy specimen. Red outline: lipoma. Blue outline: ileocecal valve. Green arrow: shows the course of the lipoma, resulting in complete obstruction of the ileocecal valve (Courtesy Dr. V. Penopoulos)
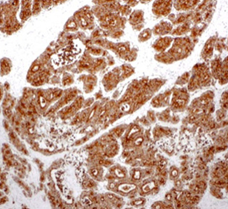
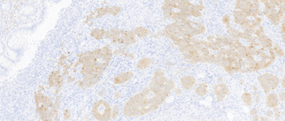
Immunohistochemical examination. Positivity for Synaptophysin (Courtesy Dr. V. Penopoulos).
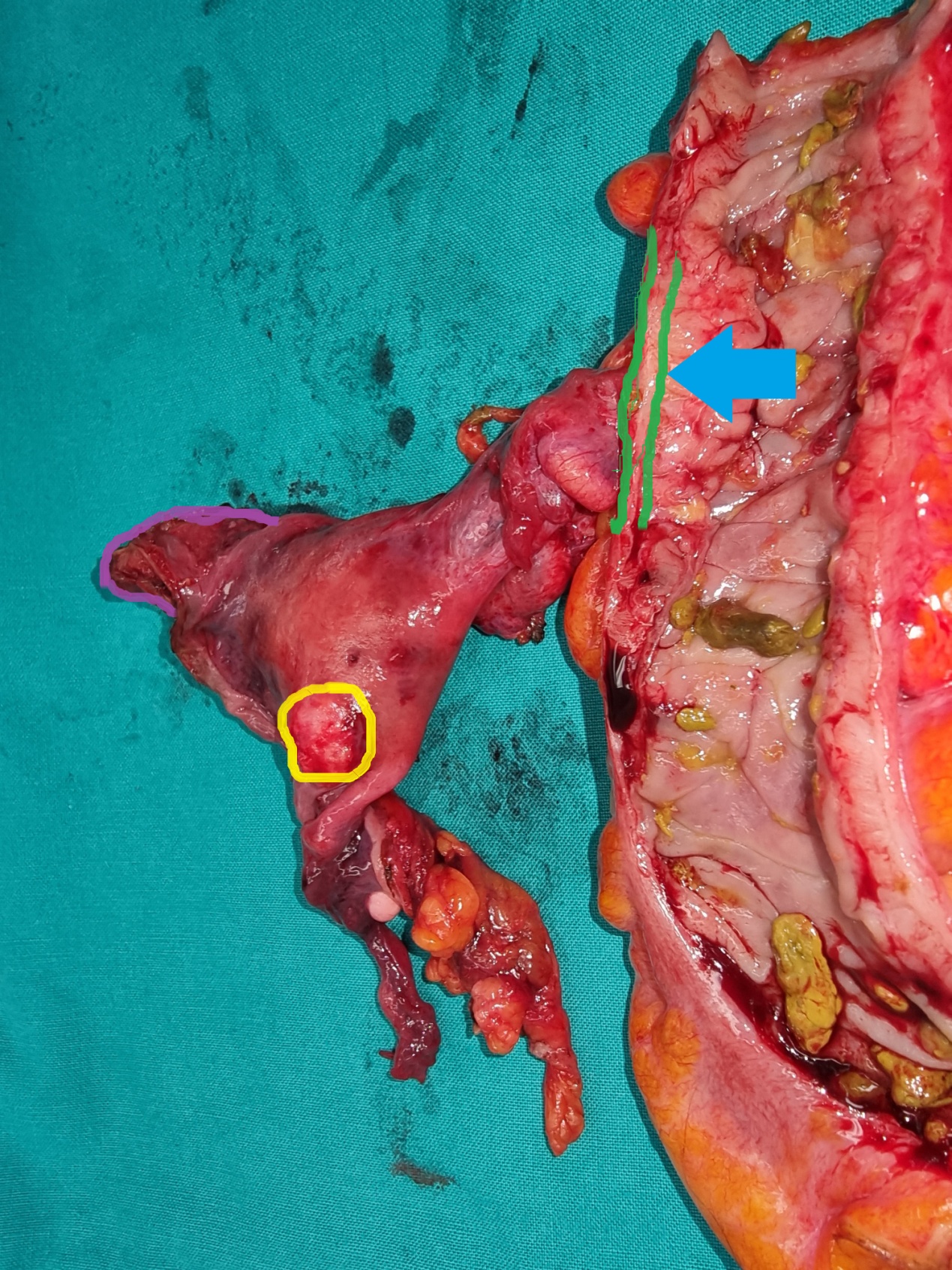
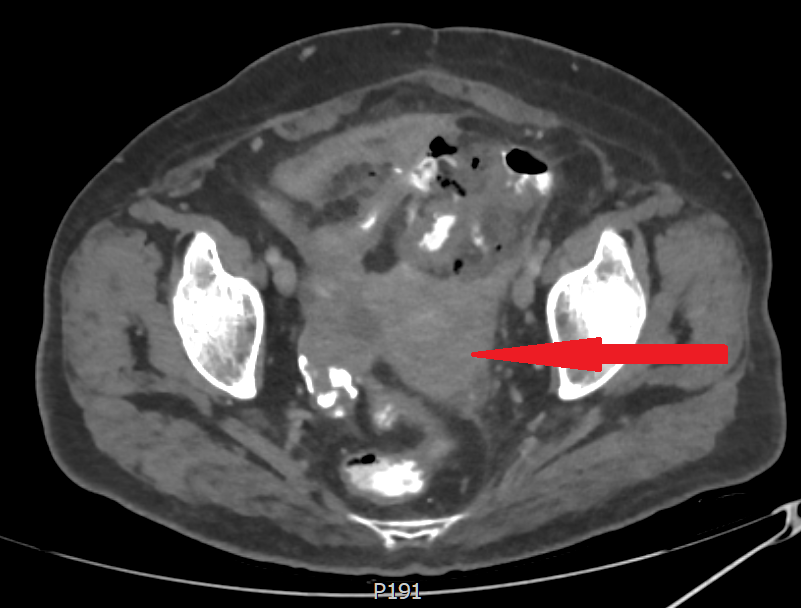
En bloc rectosigmoidectomy plus total hysterectomy. Blue arrow: Utero-colic fistula. Yellow circle: Uterine leiomyoma (Courtesy Dr. V. Penopoulos).
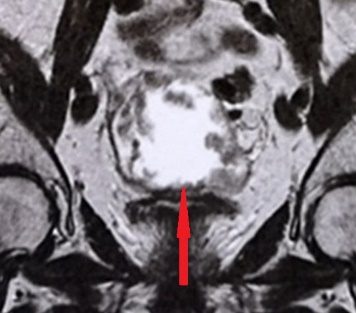
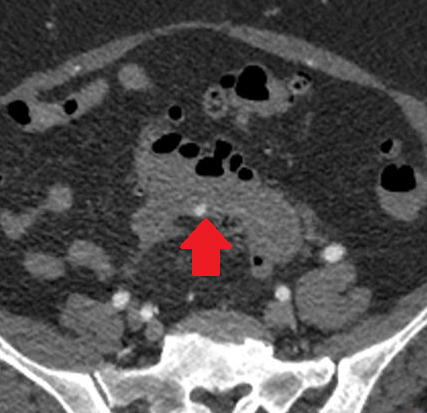
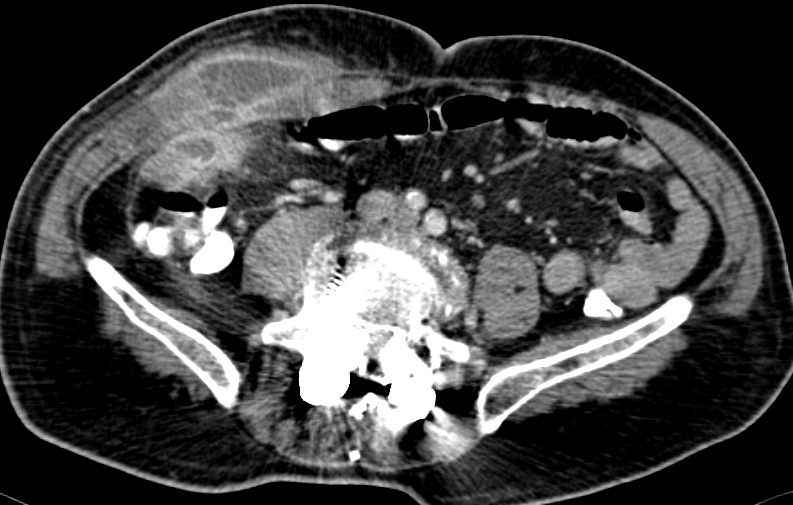
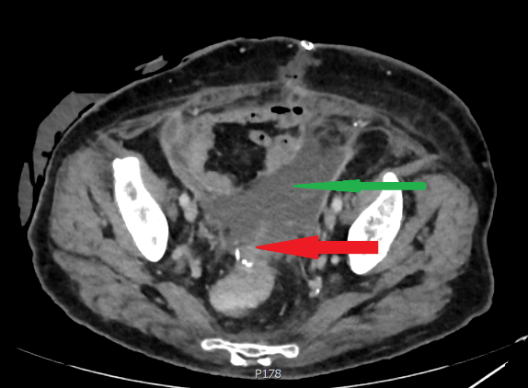
Figure 5 . CT demonstrated a retroperitoneal mass surrounding the left lumbar ureter and causing uretero-hydronephrosis: This lesion was suggestive of recurrence . ( Courtesy Dr . V . Penopoulos ) .
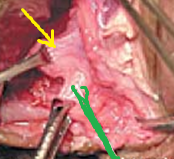
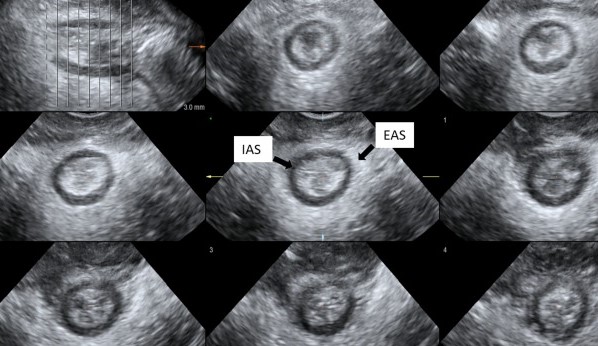
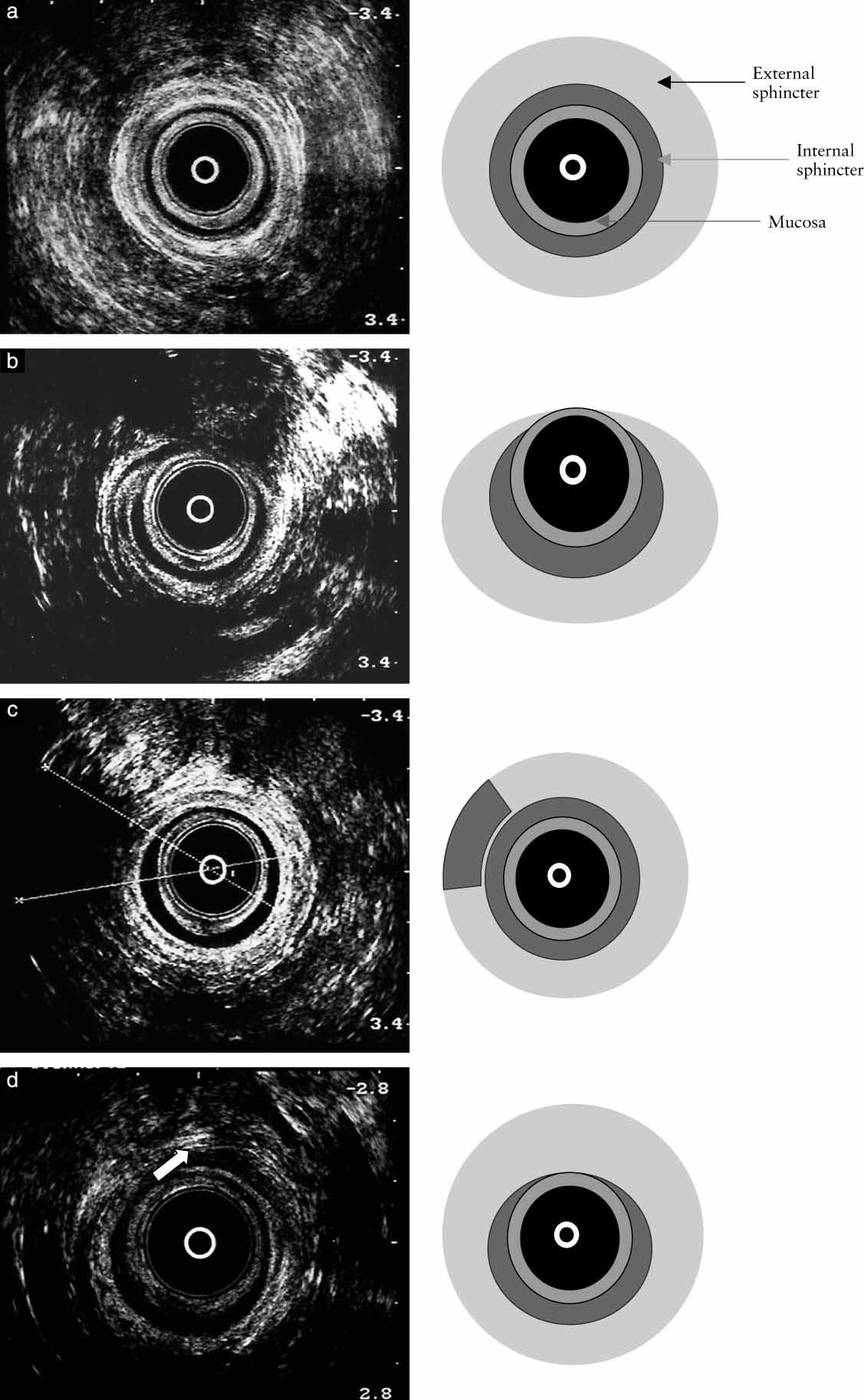
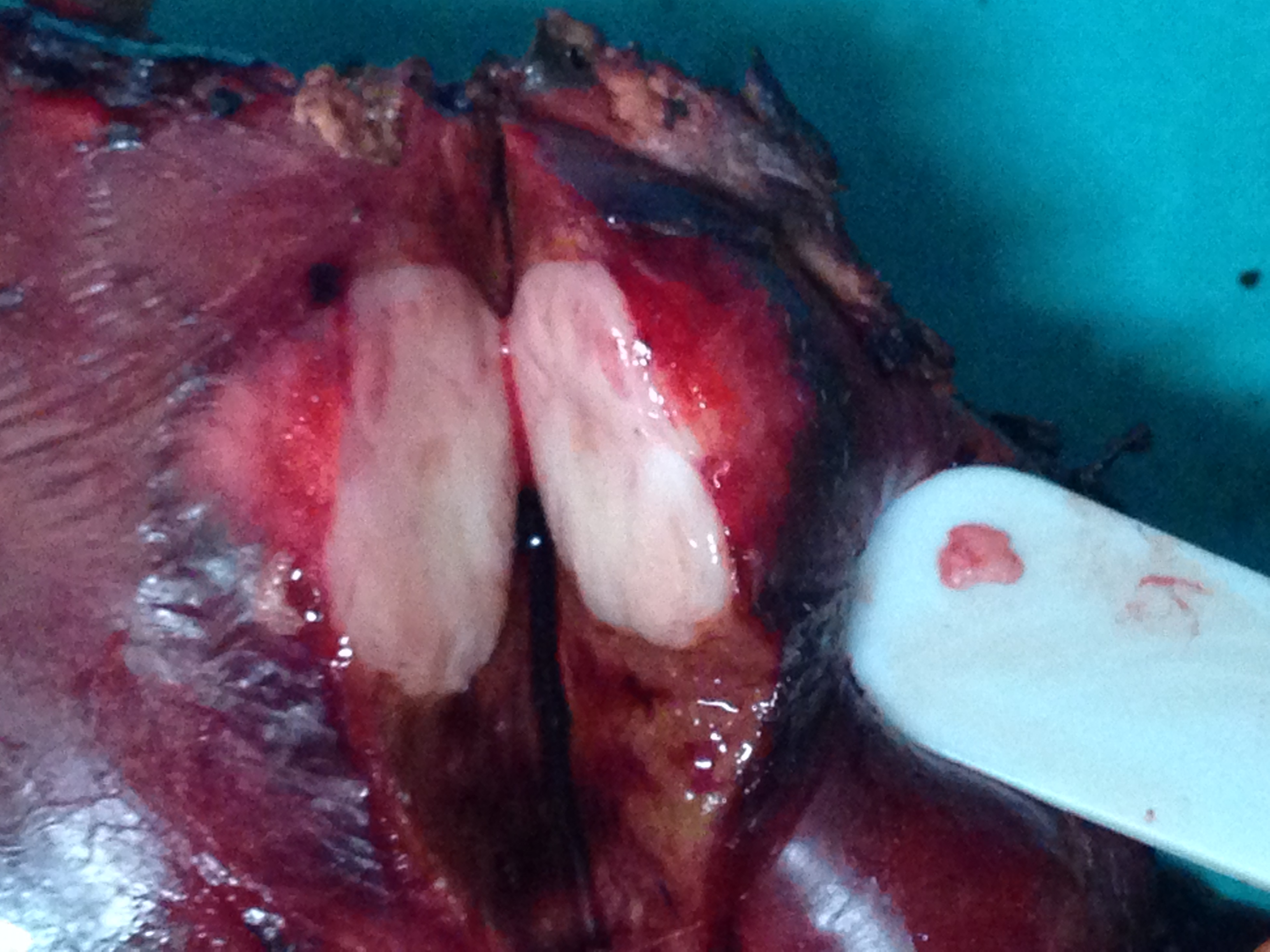
Green arrow - Internal and Yellow arrow external sphincters following meticulous dissection (Courtesy Dr. V. Penopoulos)
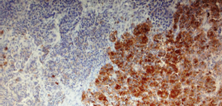
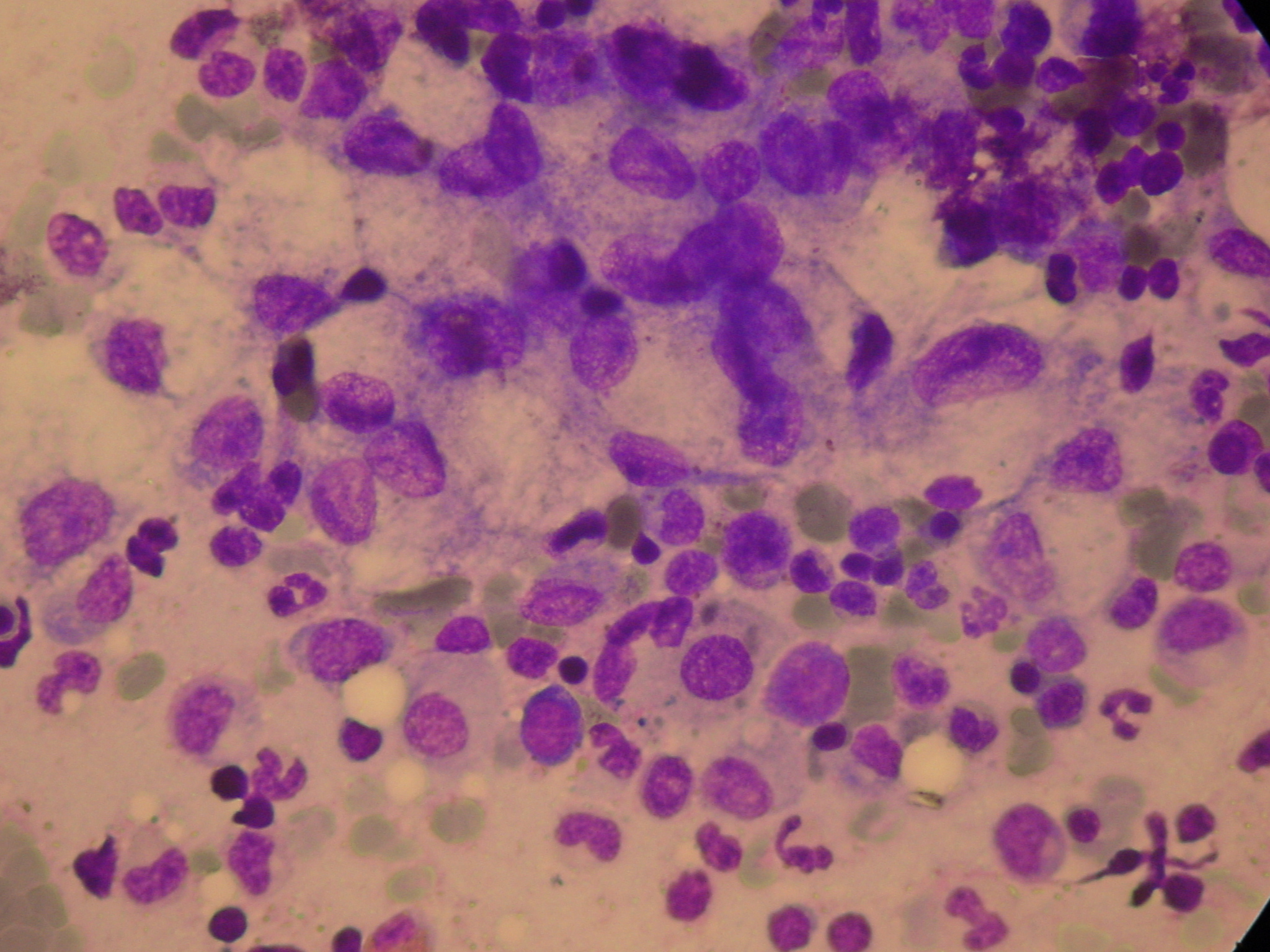
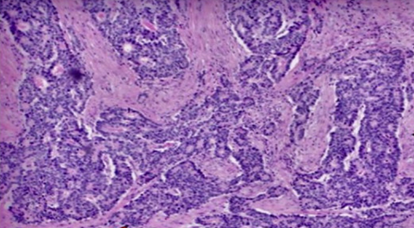
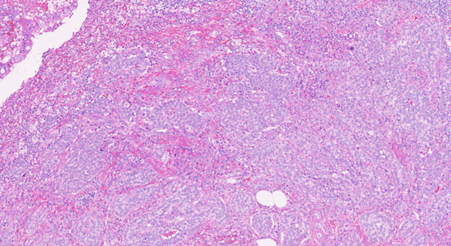
Figure 2 . Large cell neuroendocrine carcinoma, positive for Chromogranin A, and moderately differentiated adenocarcinoma in a collision pattern.
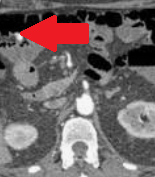
Red arrow - Bleeding diverticulum of the transverse colon (Courtesy Dr. V. Penopoulos)
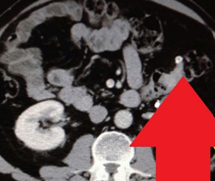
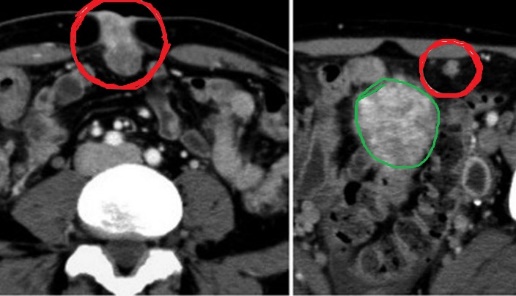
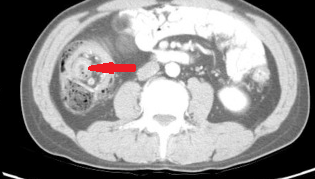
Figure 1 . Contrast enhanced CT showed an irregular circumferential mass in the left half of transverse colon with fat stranding adjacent to thickened bowel wall. ( Courtesy Dr . V . Penopoulos ) .
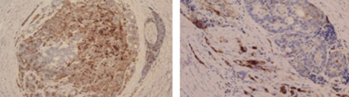
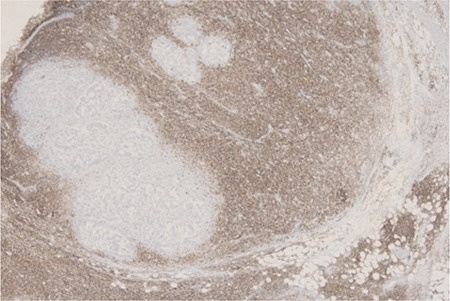
Figure 6 . Recurrence retroperitoneal mass with a size of 3 × 2.5 cm size composed of adenocarcinoma and neuroendocrine (GIII). Immunohistochemical study revealed neuroendocrine cells positive for chromogranin A . ( Courtesy Dr. V . Penopoulos ) .
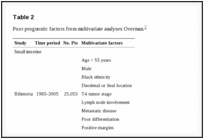

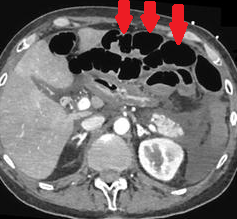
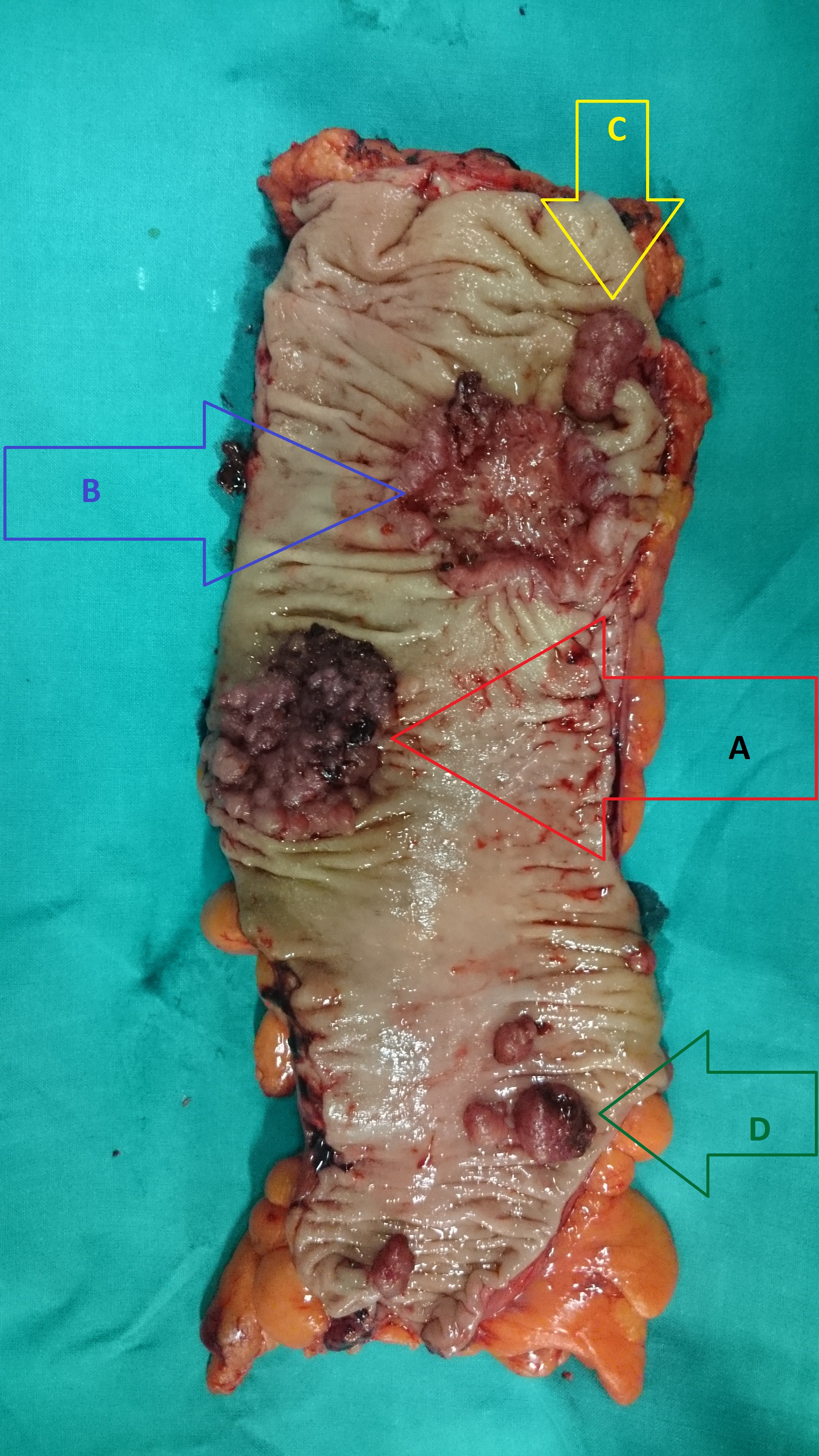
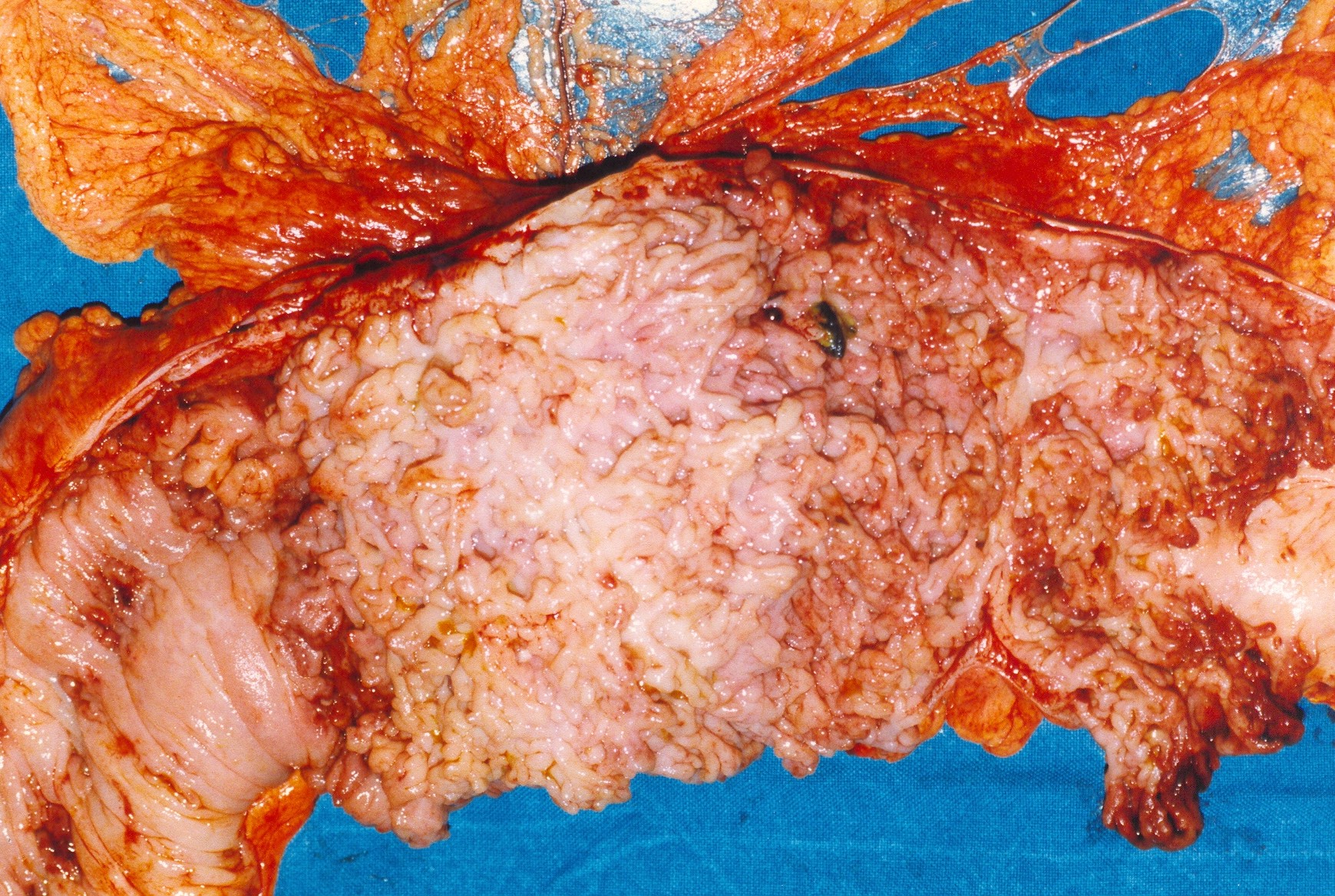
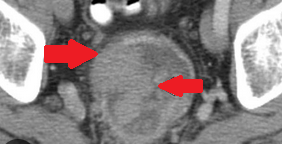
2017 : Metachronous jejunal adenocarcinoma with lymph nodes metastases (Courtesy Dr. V. Penopoulos)
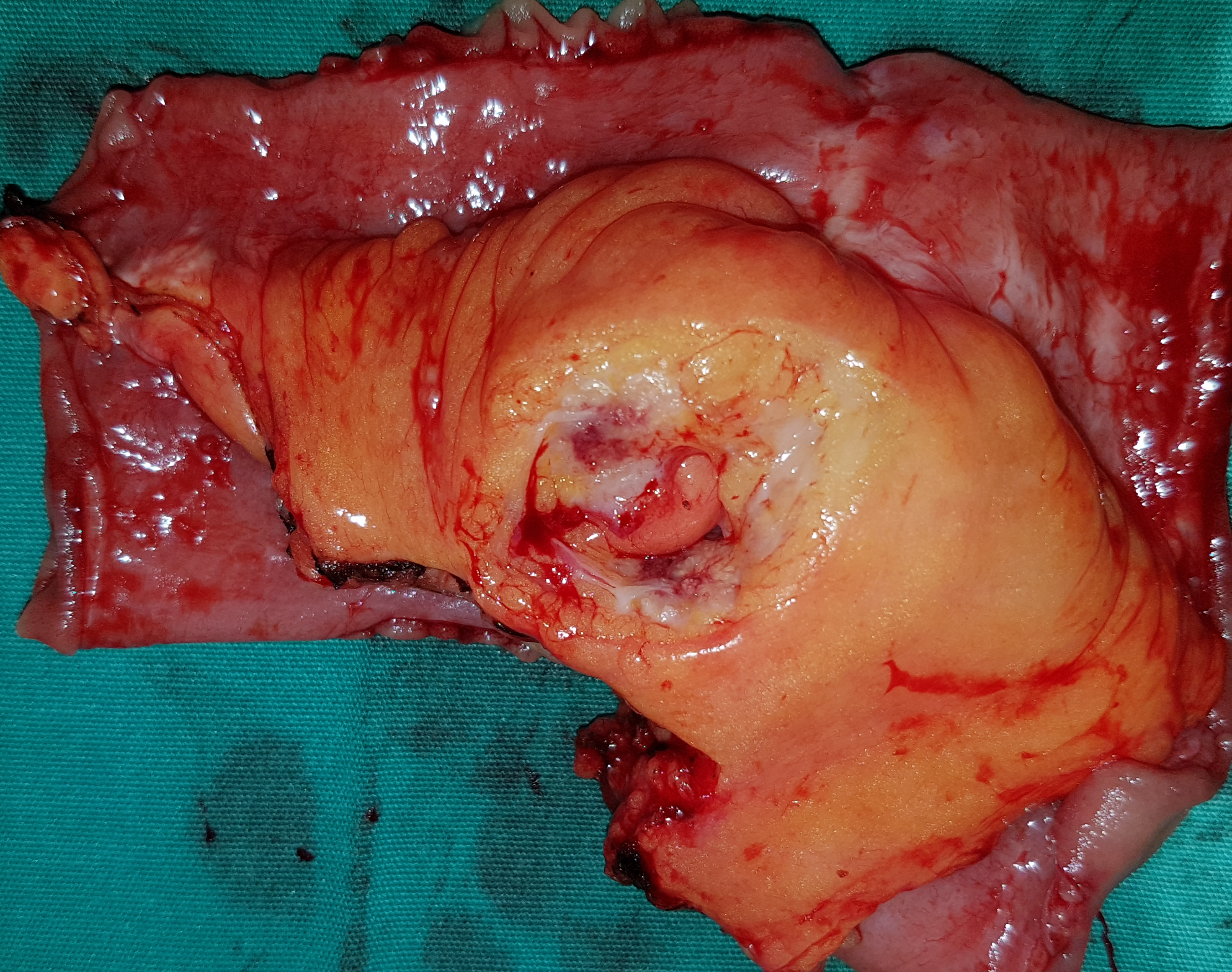
2017 : Metachronous jejunal adenocarcinoma with lymph nodes metastases (Courtesy Dr. V. Penopoulos)
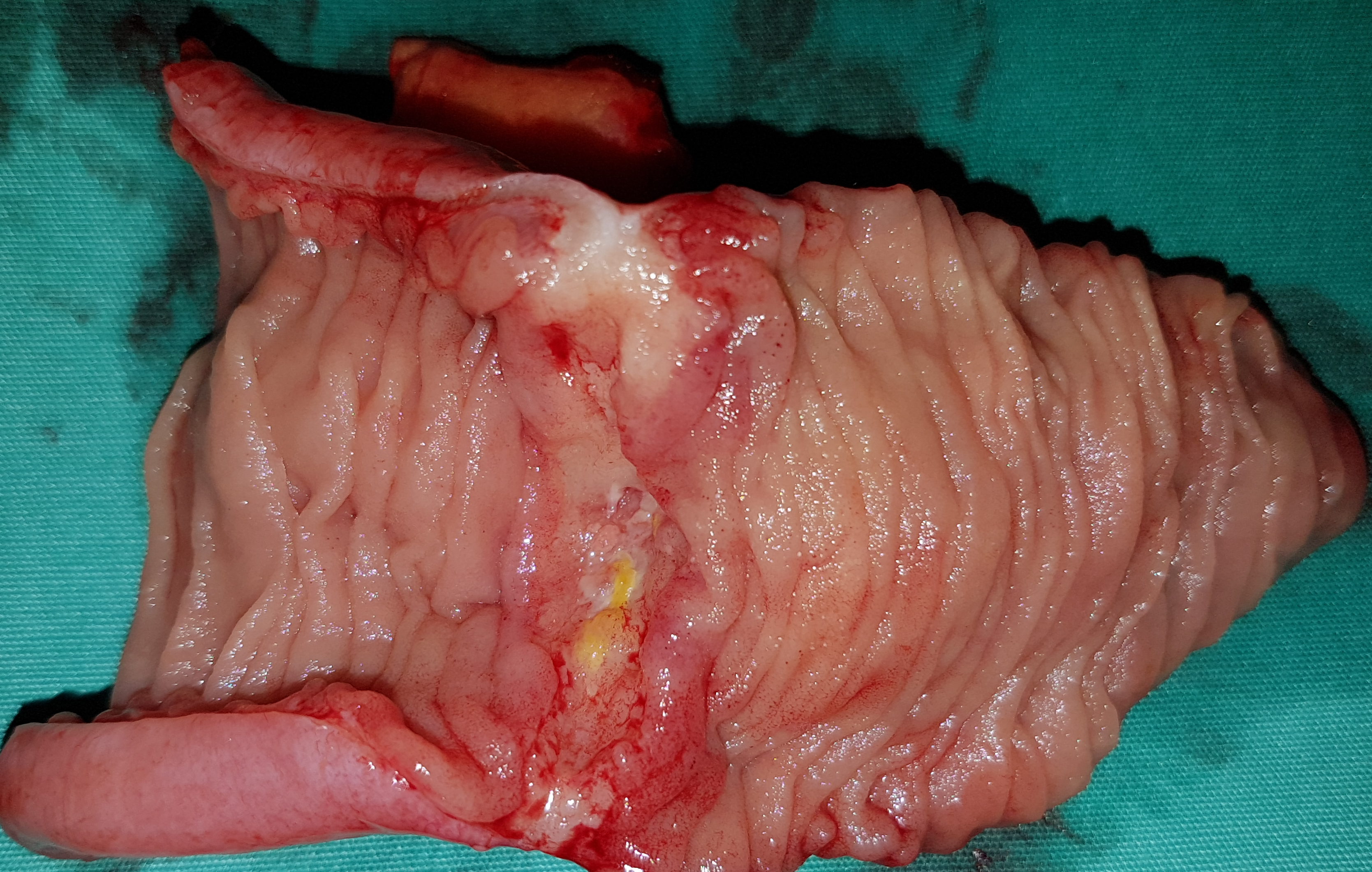
2017 : Metachronous jejunal adenocarcinoma with lymph nodes metastases (Courtesy Dr. V. Penopoulos)
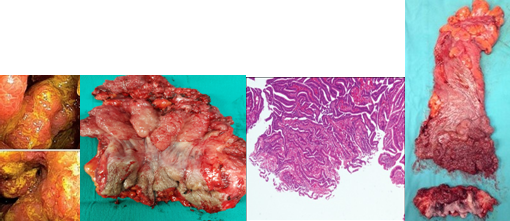
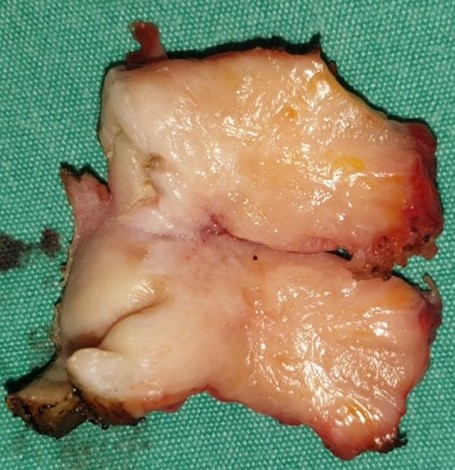
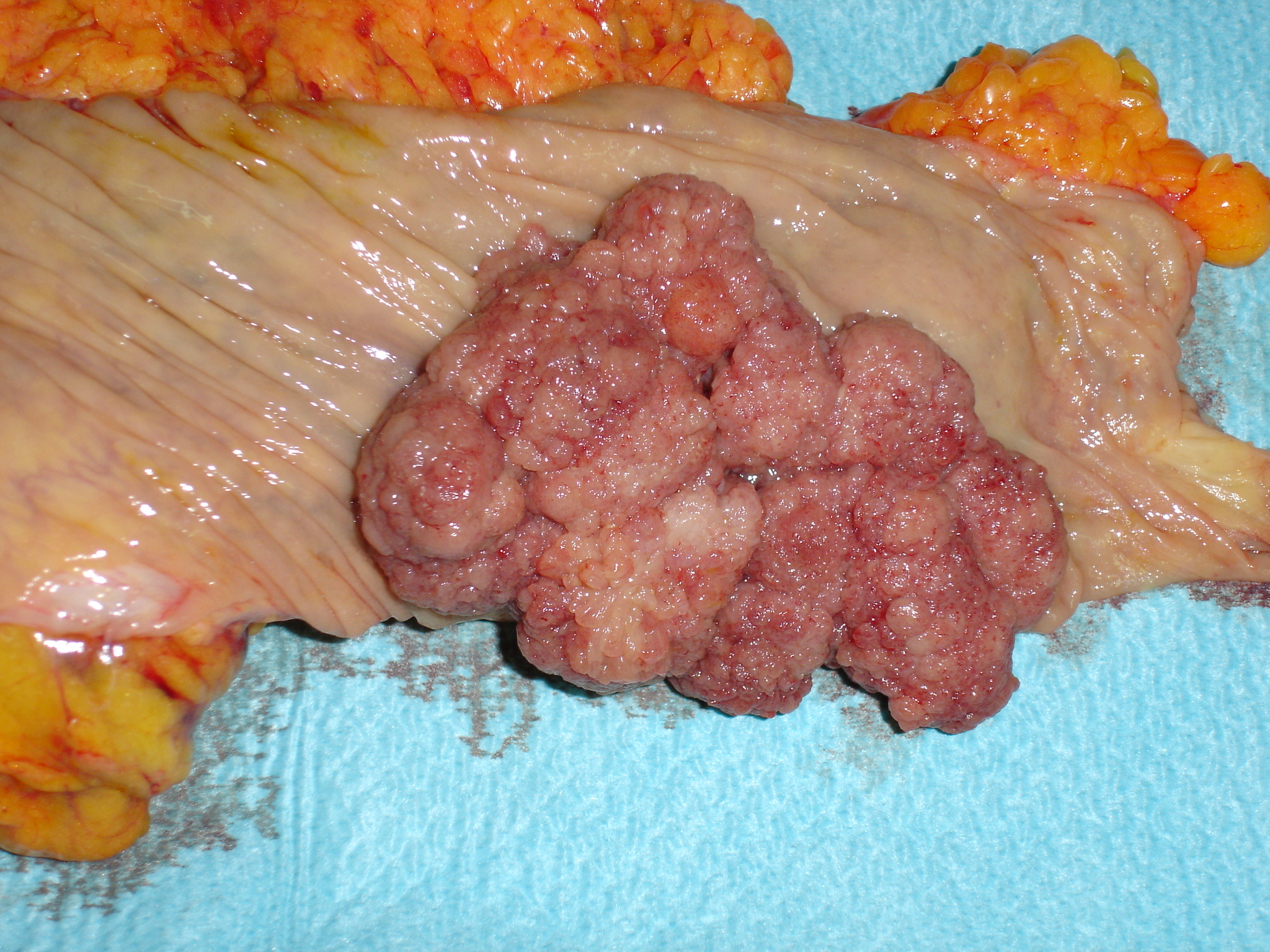
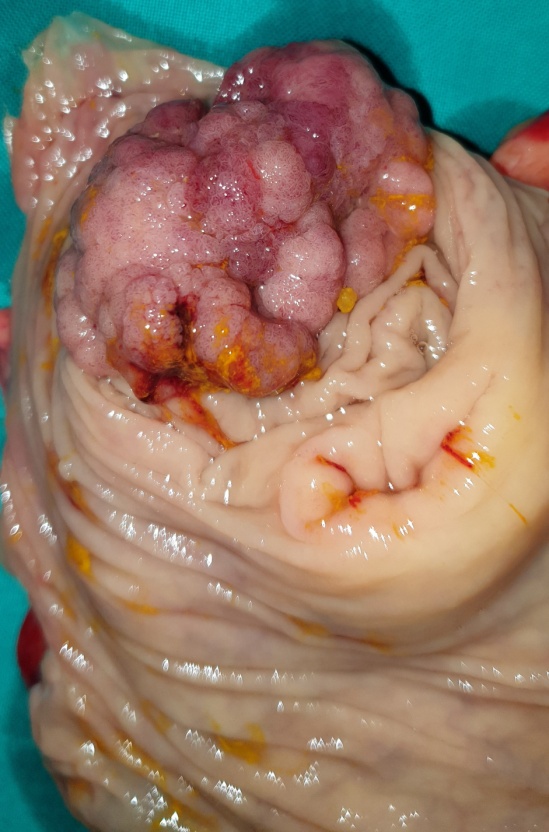
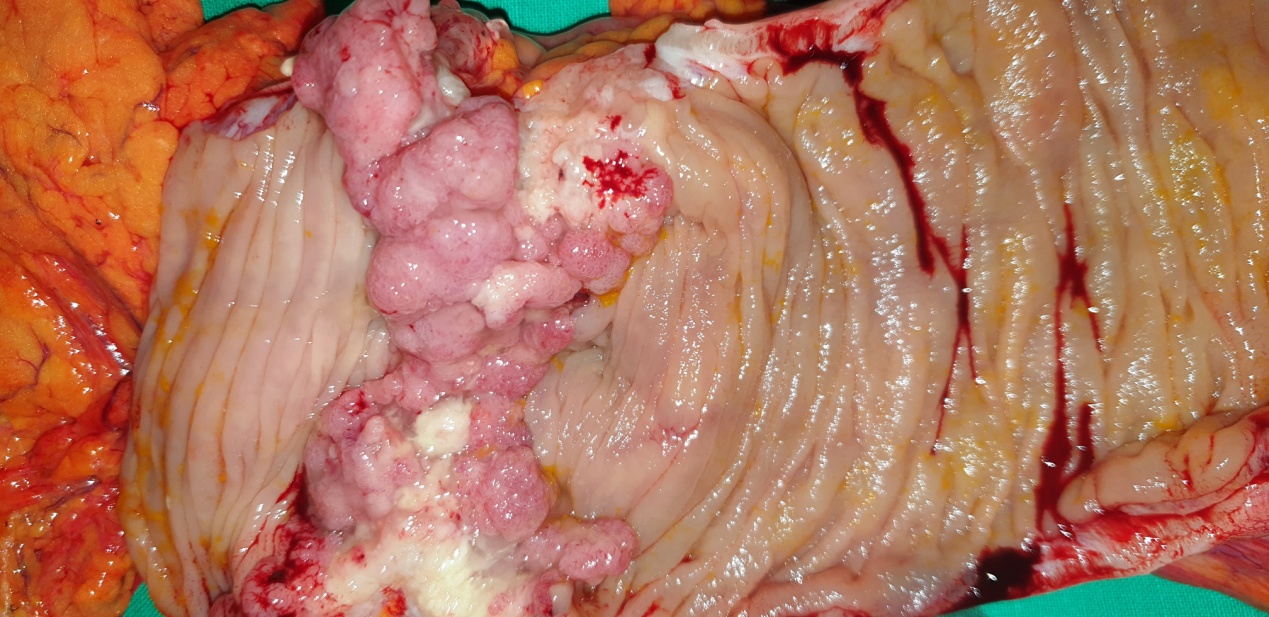
Figure 1 . Giant villous adenoma fully excised with AP resection . ( Courtesy Dr . V . Penopoulos ) .
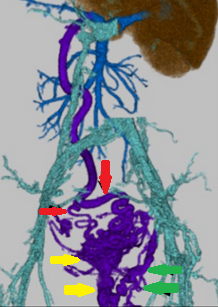
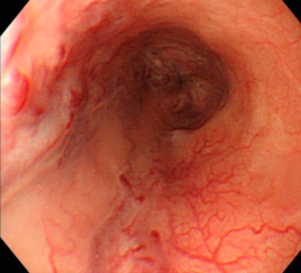
Esophageal varices at the 2 o'clock position. Thick vessel protrusion on the varix representing a hematocystic spot (Courtesy Dr. V. Penopoulos)
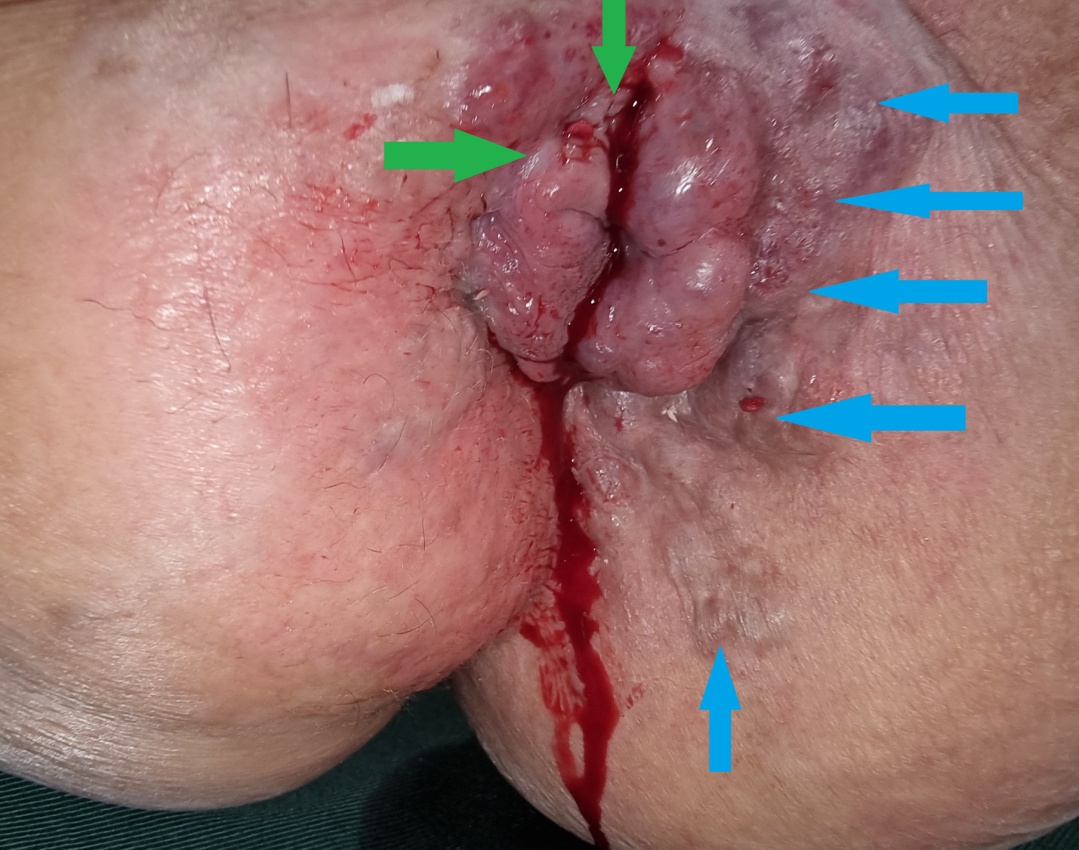
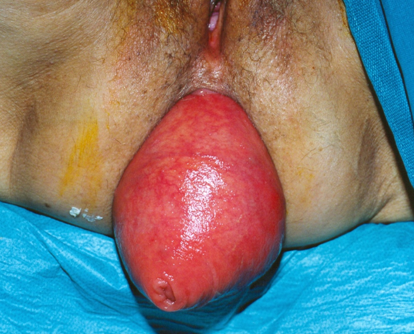
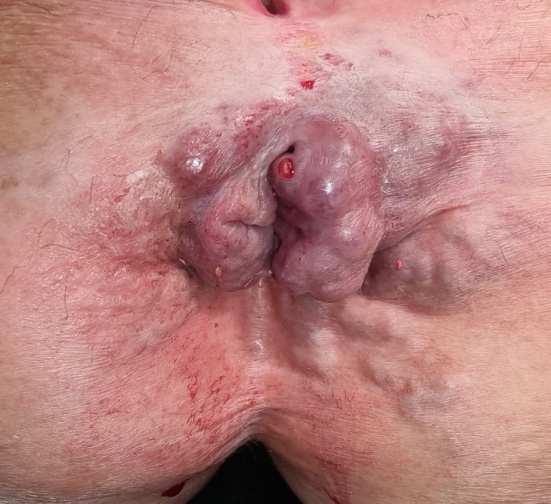
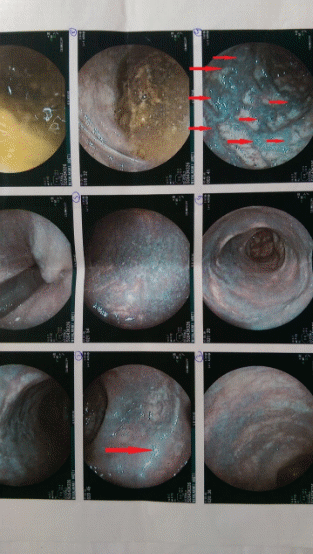
Bleeding anorectal varices (green arrows). Marked dilatation of the external hemorrhoidal venous plexus, communicating with the rectal varices (blue arrows) (Courtesy Dr. V. Penopoulos)
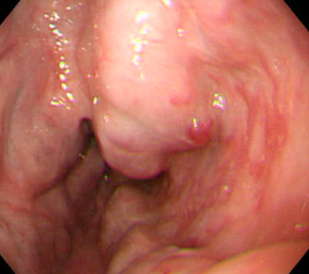
Anorectal varices. Marked dilatation of the external hemorrhoidal venous plexus, with obvious communication with the venous network of the rectal varices. Incipient variceal rupture at the 12 o'clock position is highlighted (Courtesy Dr. V. Penopoulos)
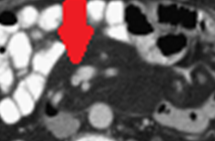
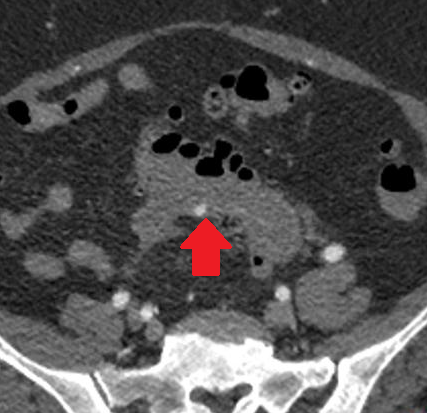
Pseudo-tumor of the mesenteric root - Mesenteric panniculitis (Courtesy Dr. V. Penopoulos)
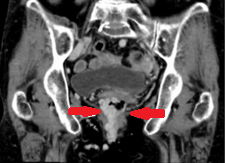
Red arrows: massive dilatation of the right superior rectal vein. Collateral circulation between the superior rectal veins (red arrows) and the anorectal varices (yellow and green arrows) (Courtesy Dr. V. Penopoulos)
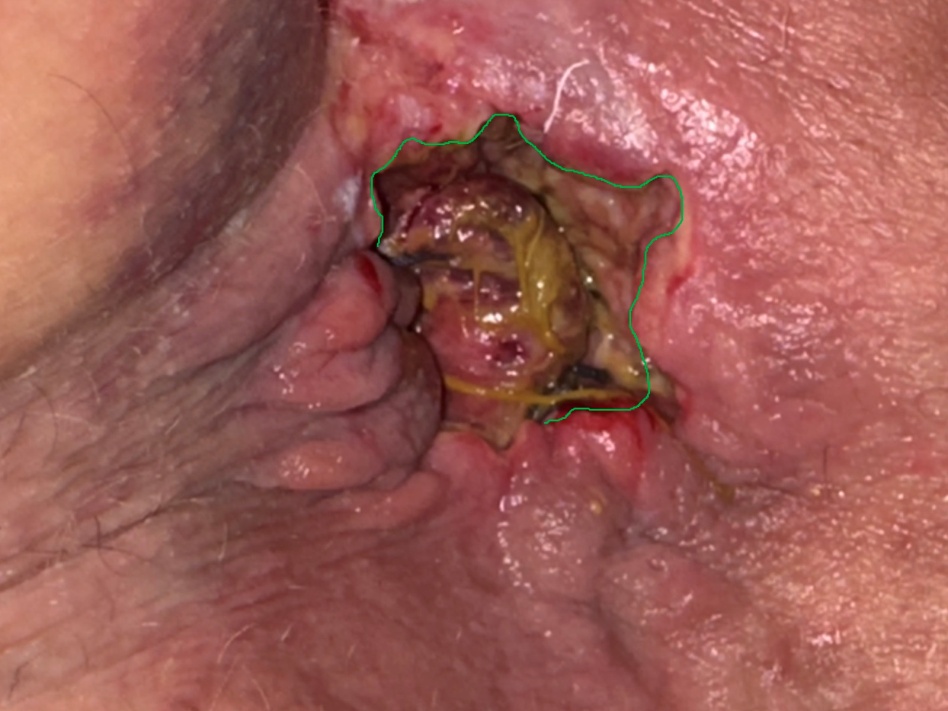
Macroscopic view on the 2nd postoperative day. Green outline: area of excised bleeding varices (Courtesy Dr. V. Penopoulos)
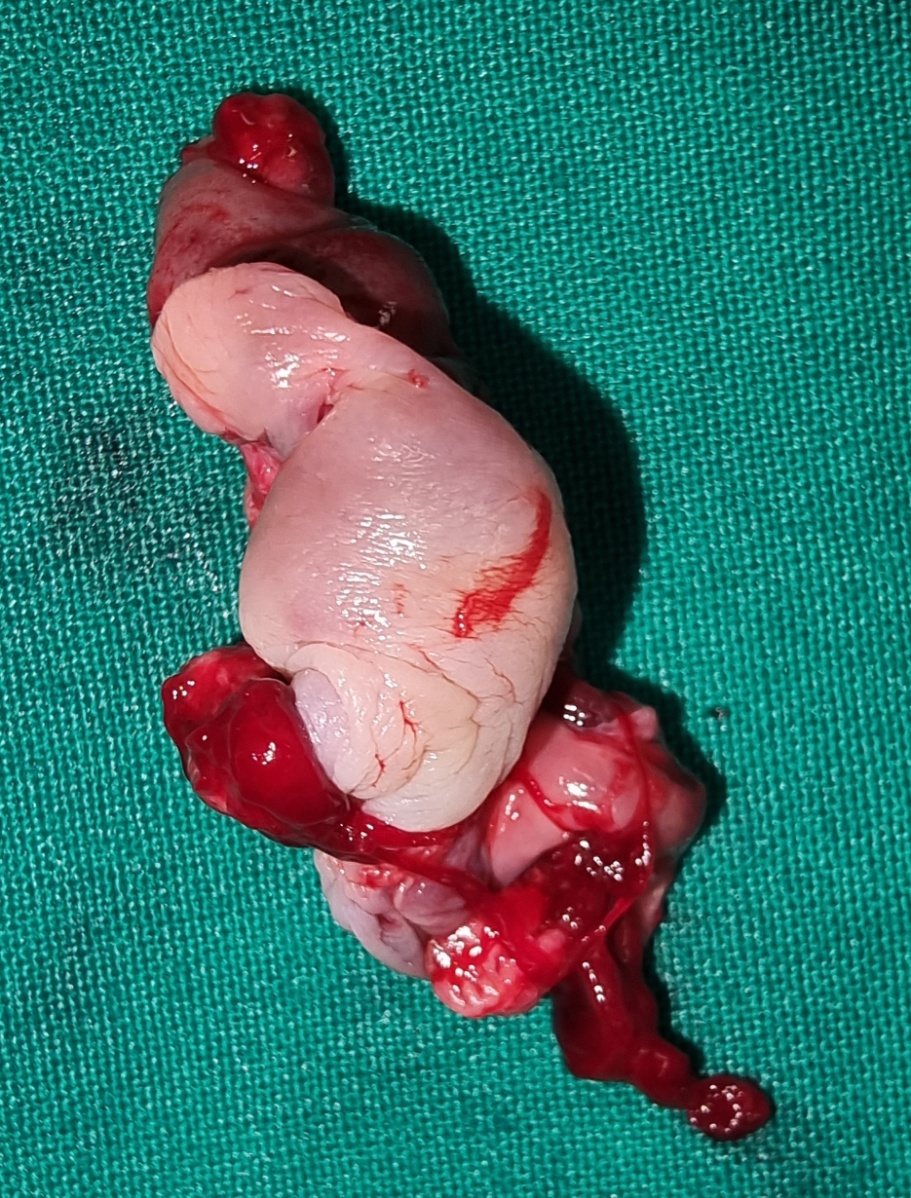
Macroscopic view on the 2nd postoperative day. Green outline: area of excised bleeding varices (Courtesy Dr. V. Penopoulos)
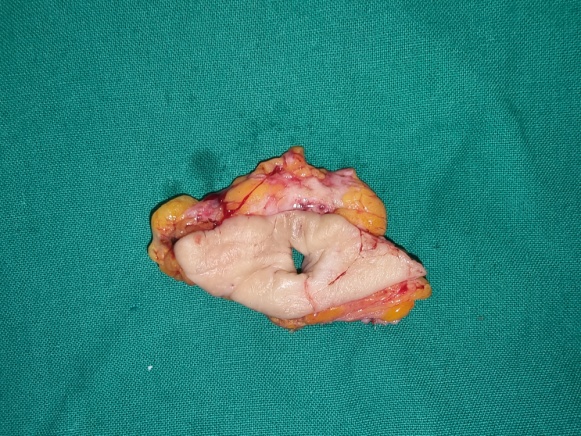
Bleeding anorectal varices (green arrows). Marked dilatation of the external hemorrhoidal venous plexus, communicating with the rectal varices (blue arrows) (Courtesy Dr. V. Penopoulos)
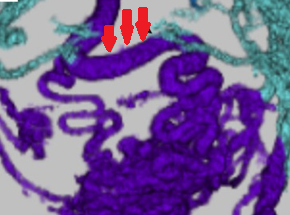
Esophageal varices at the 6 and 9 o'clock positions. Cherry-red spots at the 9 o'clock position. Red wale markings at the 6 o'clock position, as well as hematocystic spots (Courtesy Dr. V. Penopoulos)
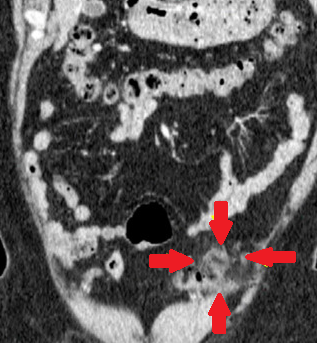
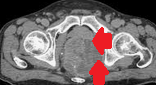
Abdominal CT scan. Red arrows - Inflamed epiploic appendage with hyperattenuated peripheral rim (Courtesy Dr. V. Penopoulos)
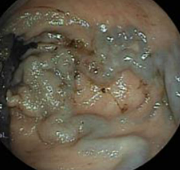
Excised fistulous tract, together with a cystic formation of subcutaneous fat (Courtesy Dr. V. Penopoulos)
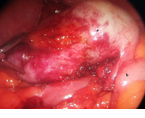
Right adnexa excision, en bloc with parietal peritoneum. Green circles — Microscopic implants (Courtesy Dr. V. Penopoulos)
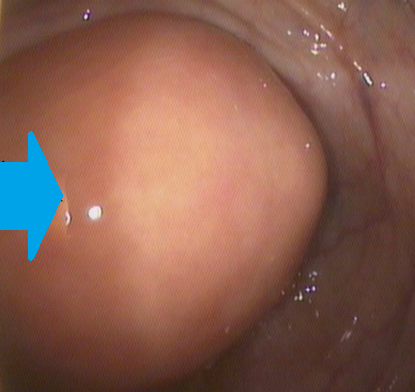
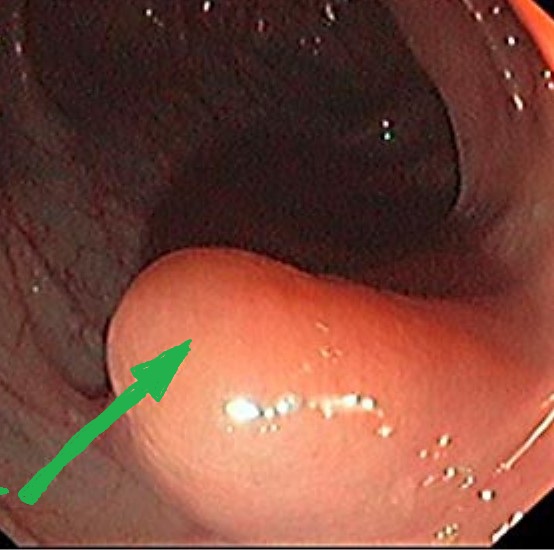
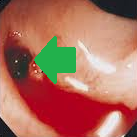
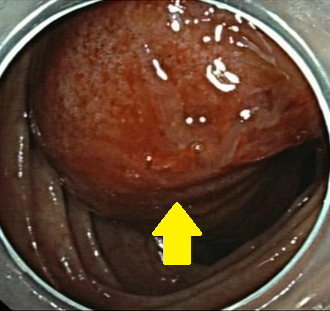
Colonoscopic image of mucocele — Submucosal mass. Blue arrow — "Volcano sign" (Courtesy Dr. V. Penopoulos)
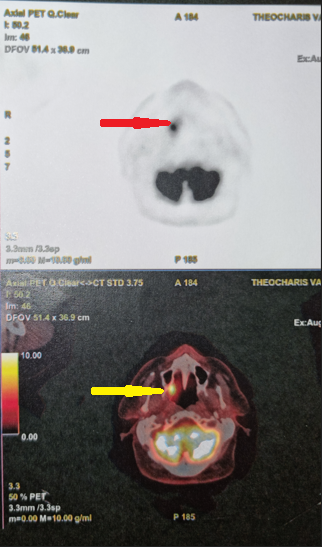
Whole-body PET scan. Pathological uptake in the right palatine tonsil (Courtesy Dr. V. Penopoulos)
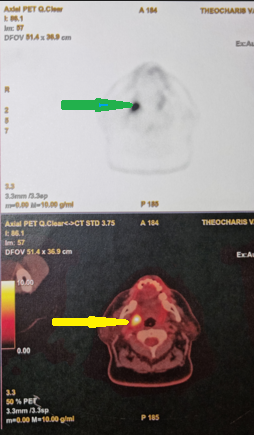
Whole-body PET scan. Pathological uptake in the right palatine tonsil (Courtesy Dr. V. Penopoulos)
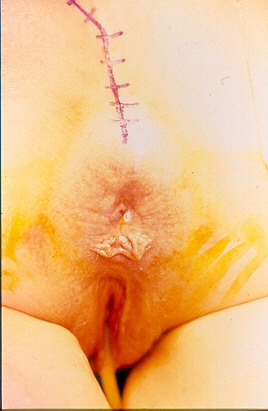
Blue arrow — Exposure of the rectum. Entry into the presacral space from the right (Courtesy Dr. V. Penopoulos)
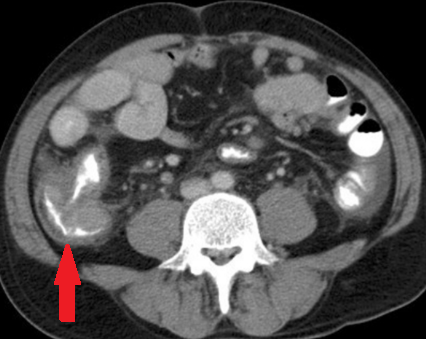
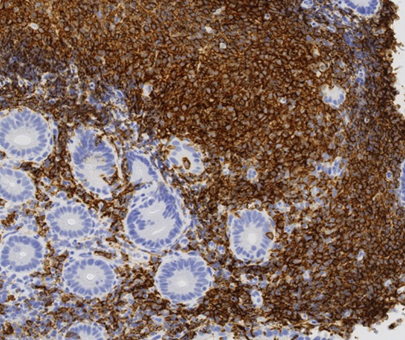
Abdominal CT scan - Cecal MALToma and paracolic lymph node (Courtesy Dr. V. Penopoulos)
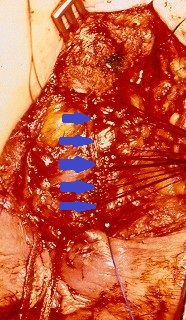
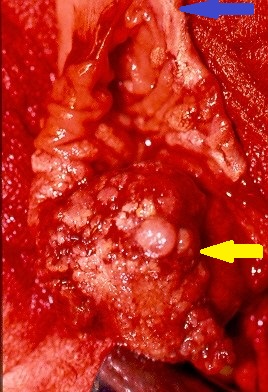
Adenocarcinoma — Abdominoperineal resection of the rectum. Yellow arrow — Site of excised neoplasm (Courtesy Dr. V. Penopoulos)
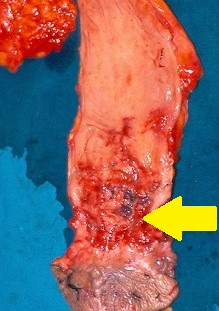
Adenocarcinoma — Abdominoperineal resection of the rectum. Yellow arrow — Site of excised neoplasm (Courtesy Dr. V. Penopoulos)
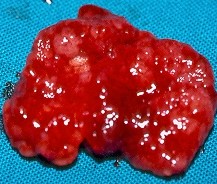
Adenocarcinoma — Abdominoperineal resection of the rectum. Yellow arrow — Site of excised neoplasm (Courtesy Dr. V. Penopoulos)
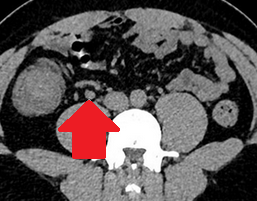
Abdominal CT scan - Cecal MALToma and paracolic lymph node (Courtesy Dr. V. Penopoulos)
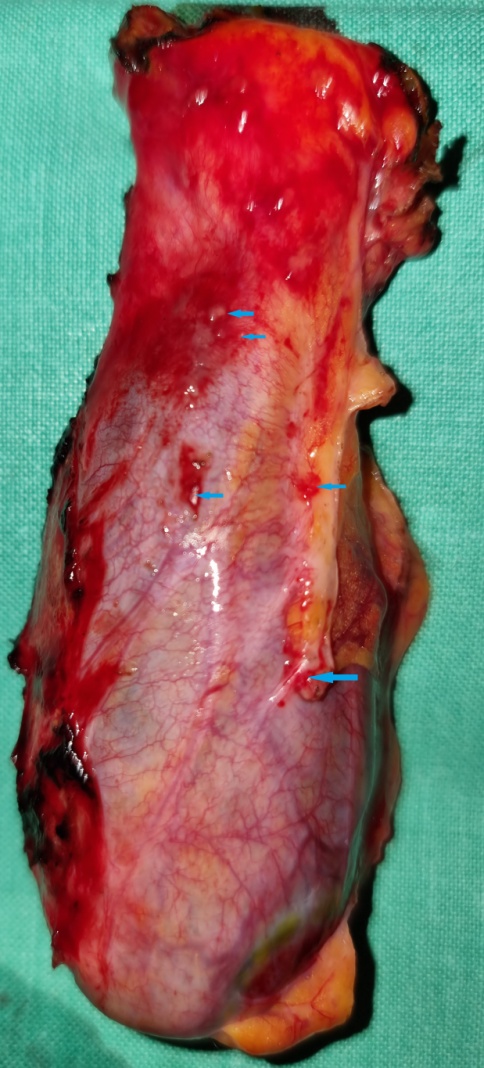
Greater omentum specimen. Presence of multiple microscopic implants (Courtesy Dr. V. Penopoulos)
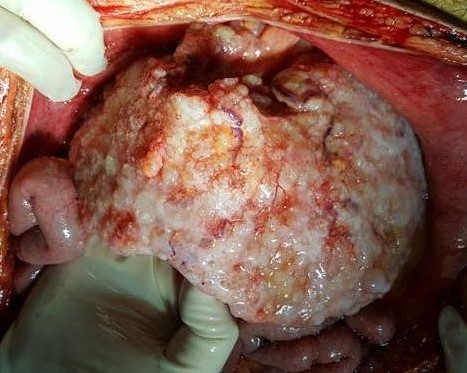
Pseudomyxoma peritonei — Complete involvement of the greater omentum (Courtesy Dr. V. Penopoulos)
Green arrow — Anus. Blue arrow — Rectum. Rose arrow — Tape encircling the rectum (Courtesy Dr. V. Penopoulos)
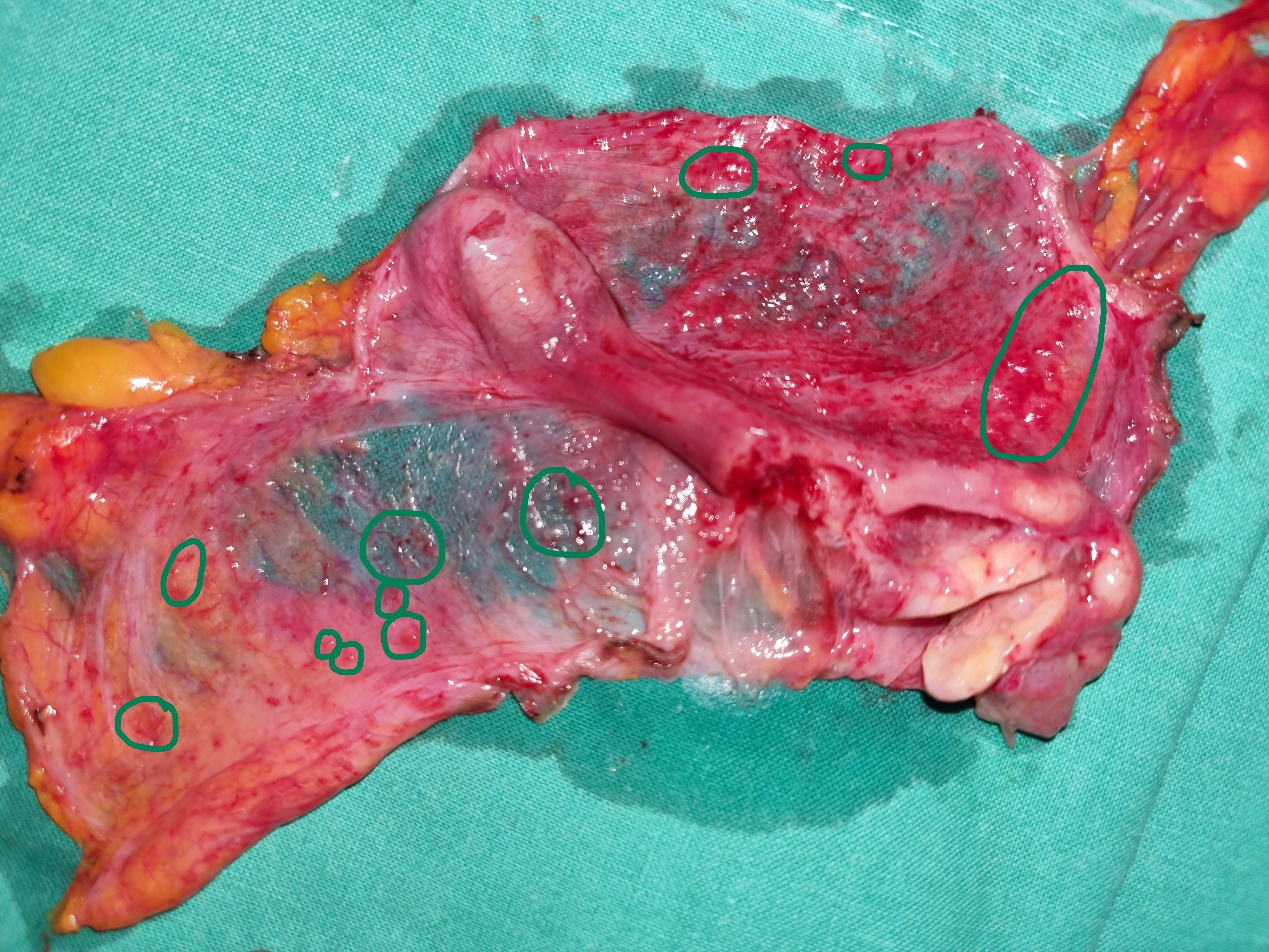
Histopathological examination of appendiceal mucocele. Extensive mucin in the appendiceal lumen, mucosal atrophy, wall thinning, and chronic inflammatory cell infiltration (Courtesy Dr. V. Penopoulos)
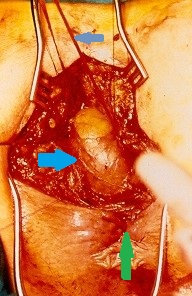
Blue arrow — Upper edge of proctotomy. Yellow arrow — Rectal neoplasm (Courtesy Dr. V. Penopoulos)

Whole-body PET scan. Pathological uptake in the right palatine tonsil (Courtesy Dr. V. Penopoulos)
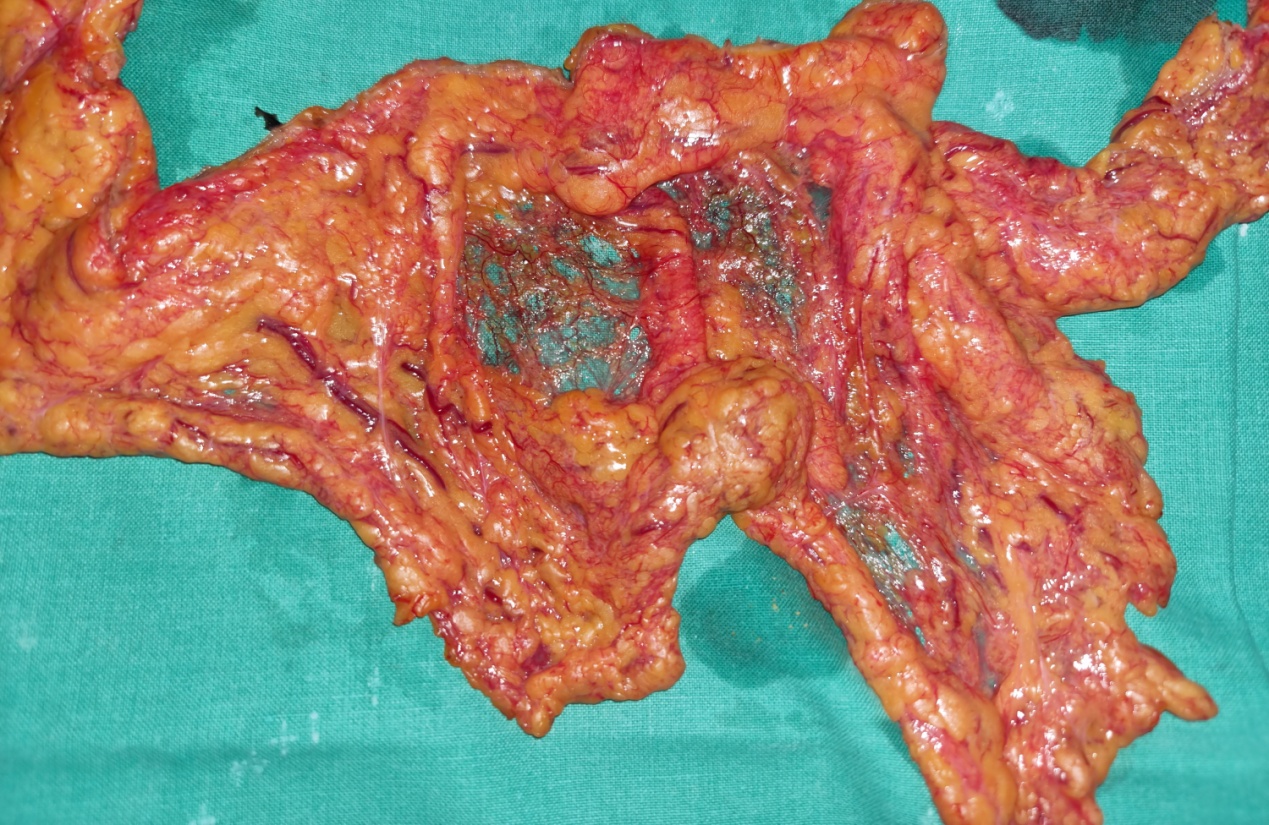
Histopathological examination of appendiceal mucocele. Extensive mucin in the appendiceal lumen, mucosal atrophy, wall thinning, and chronic inflammatory cell infiltration (Courtesy Dr. V. Penopoulos)
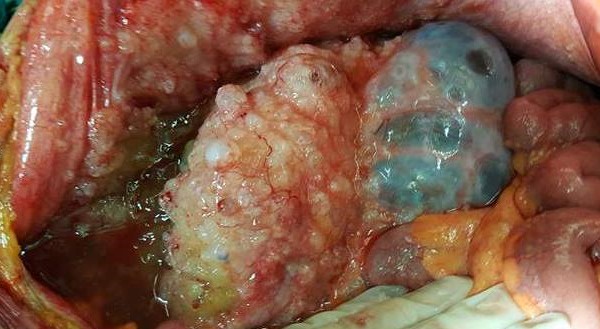
Removal of disseminated gelatinous material from the peritoneal cavity (Courtesy Dr. V. Penopoulos)
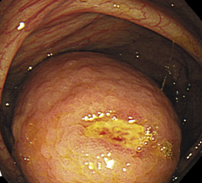
Colonoscopic image of appendiceal mucocele intussusception (Courtesy Dr. V. Penopoulos)
Colonoscopic image of mucocele — Submucosal mass. Blue arrow — "Volcano sign" (Courtesy Dr. V. Penopoulos)
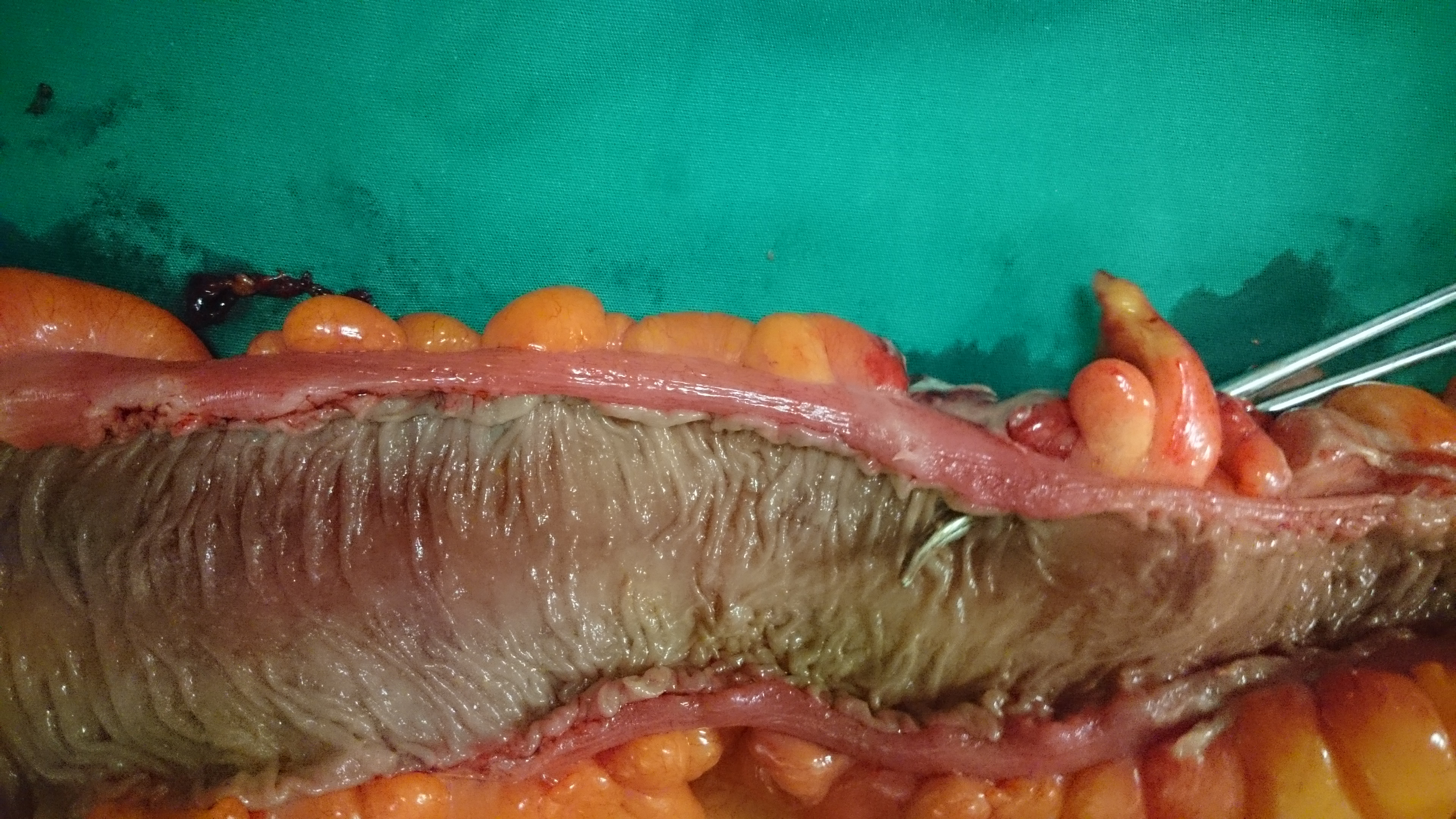
Resected rectosigmoid colon. The site of the perforated diverticular abscess is evident
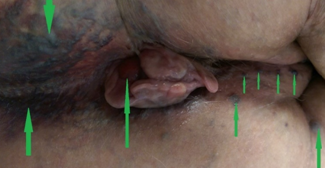
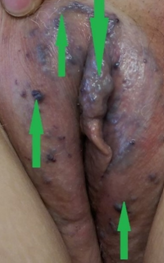
Figure 5 . Lumbar region and perianal varices together with prolapsed hemorrhoids prior to surgery . No anomaly in the iliac vessels was detected . (Courtesy Dr . V . Penopoulos) .
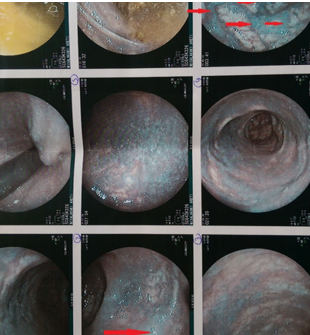
Figure 1 . Rectal submucosal varices are clearly seen . ( Courtesy Dr . V . Penopoulos ) .
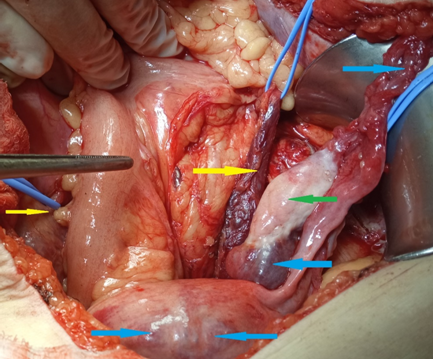
Figure 2 . Pelvic congestion syndrome . Dilated left ovarian veins , left ureteric veins , ovarian varix and para-uterine veins . ( Courtesy Dr . V . Penopoulos ) .
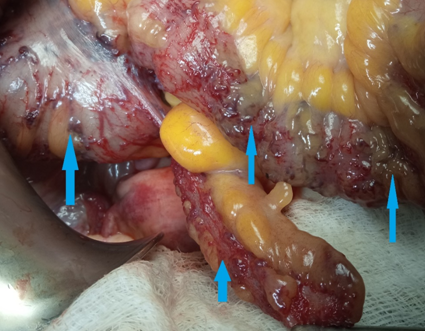
Figure 3 . Subserosal ileocolic varices of no significance . ( Courtesy Dr . V . Penopoulos ) .
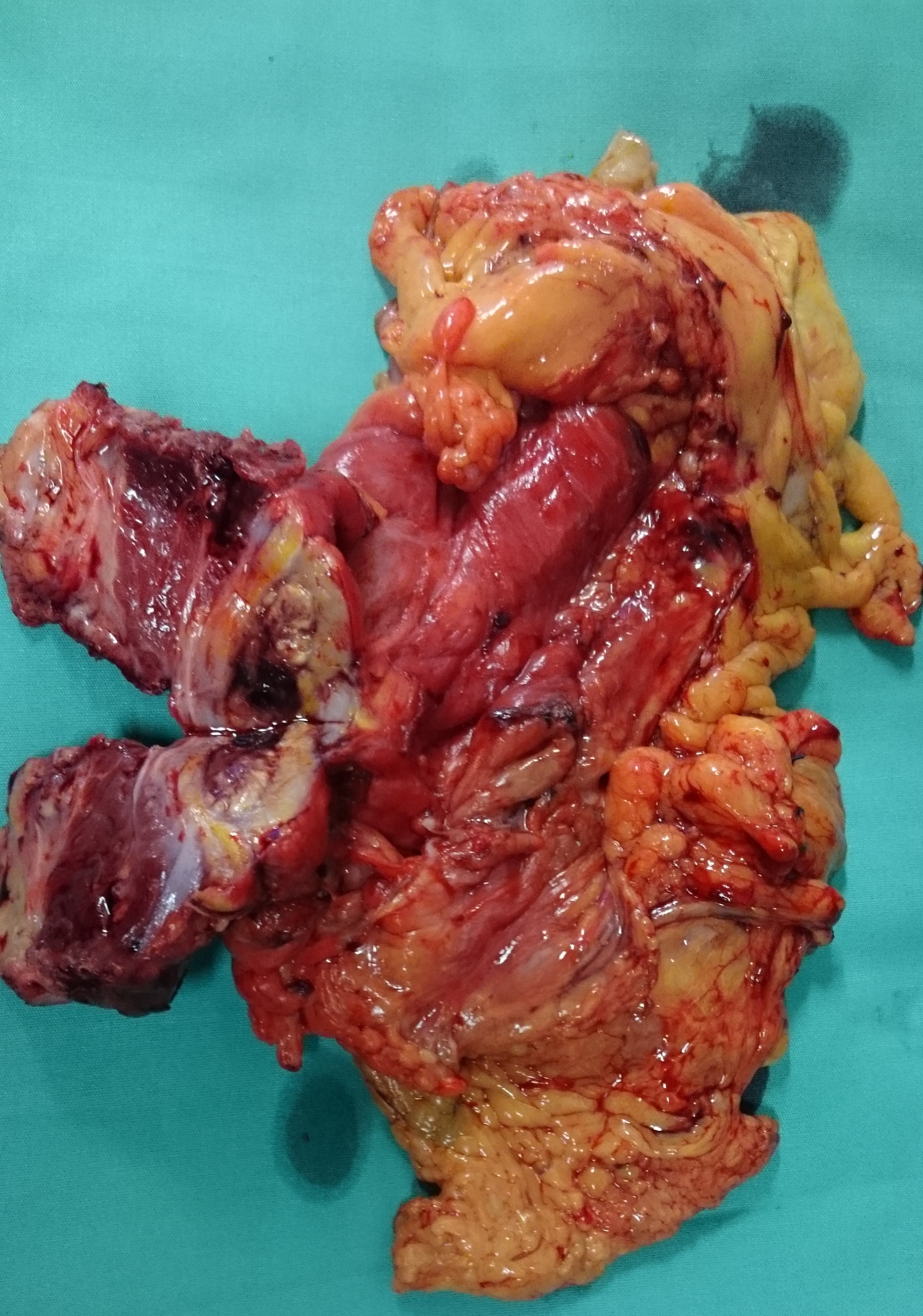
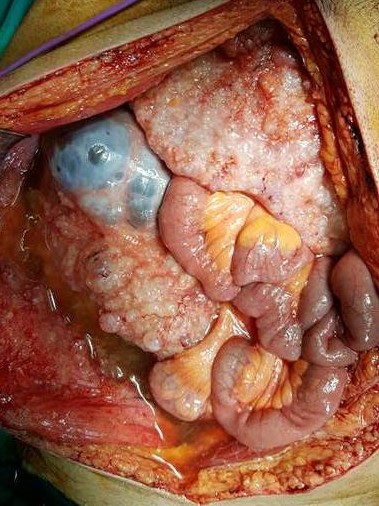
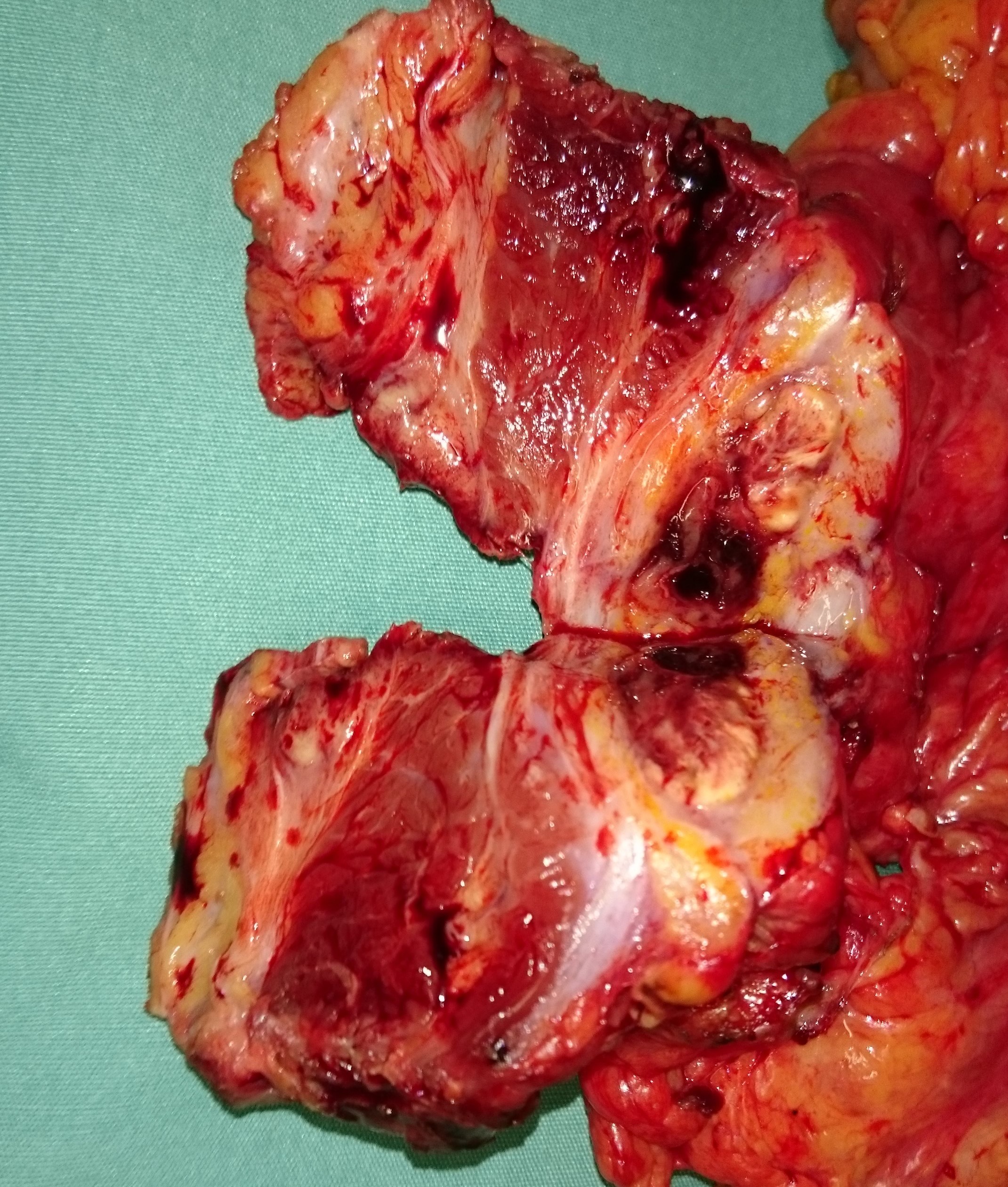
The excised mass together with right hemi colon and abdominal wall (Courtesy Dr. V. Penopoulos)
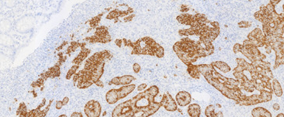
Immunohistochemical examination positive for neuron-specific enolase (Courtesy Dr. V. Penopoulos)
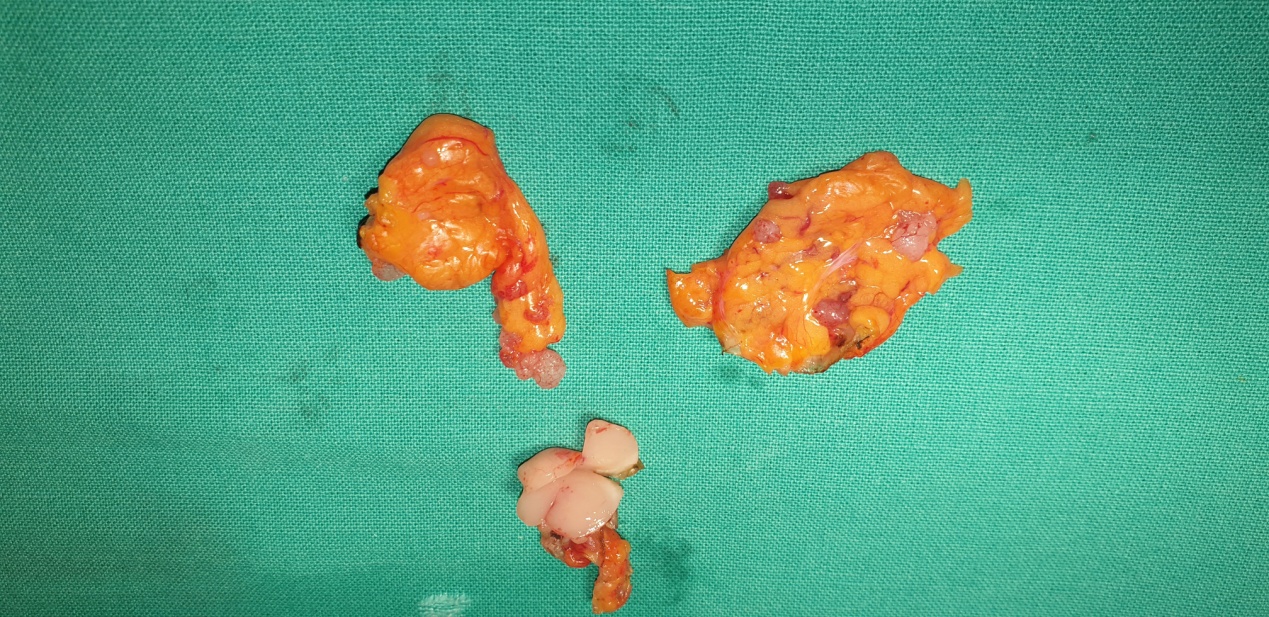
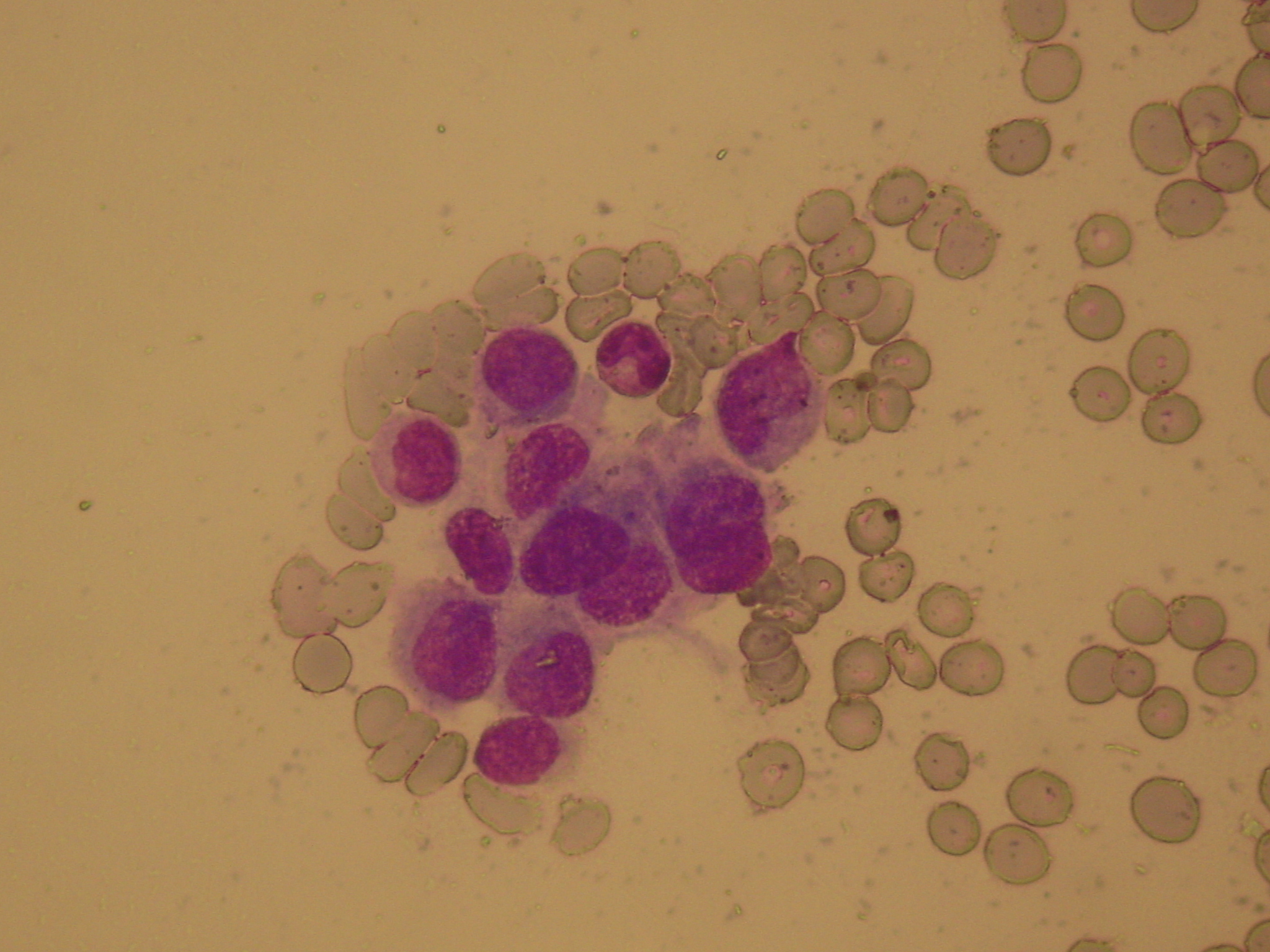
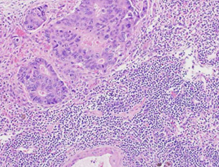
Infiltrated lymph nodes with both cancerous and atypical lymphocytes (Courtesy Dr. V. Penopoulos)
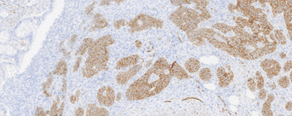
Immunohistochemical examination positive for chromogranin (Courtesy Dr. V. Penopoulos)
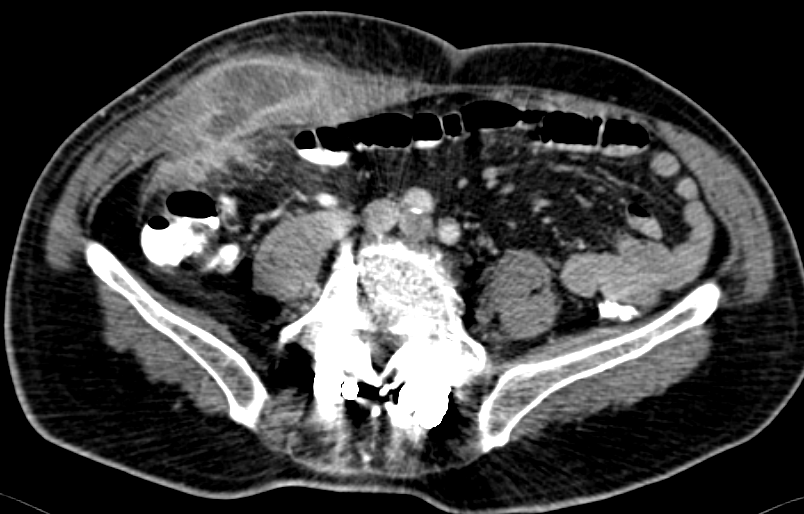
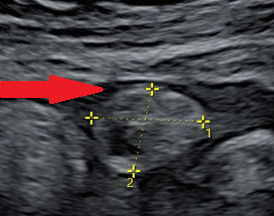
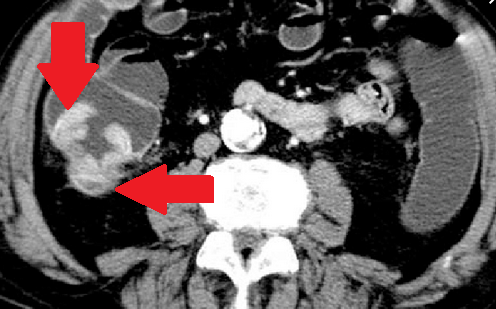
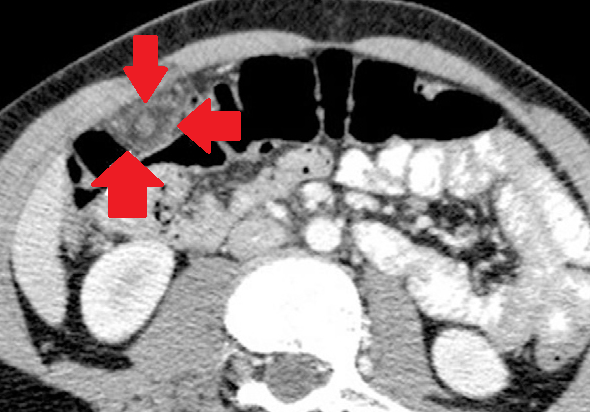
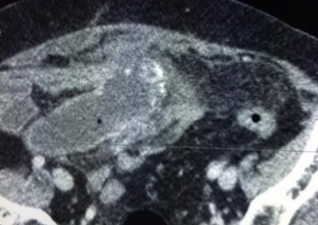
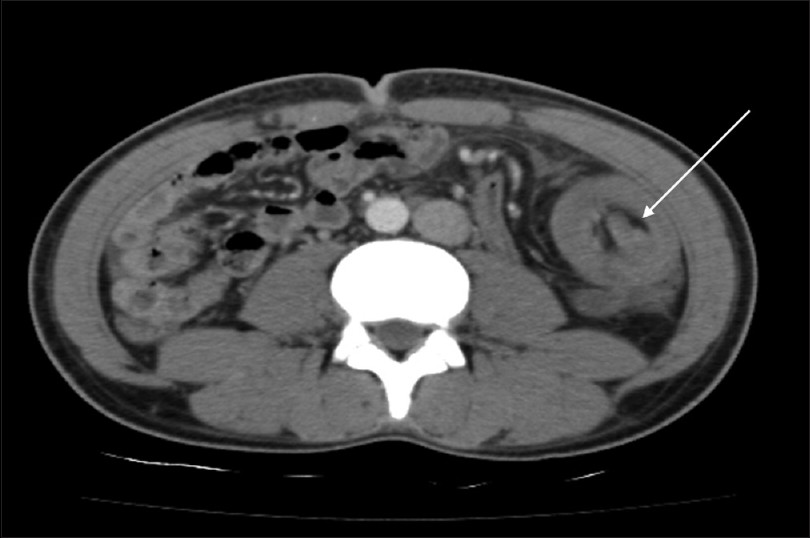
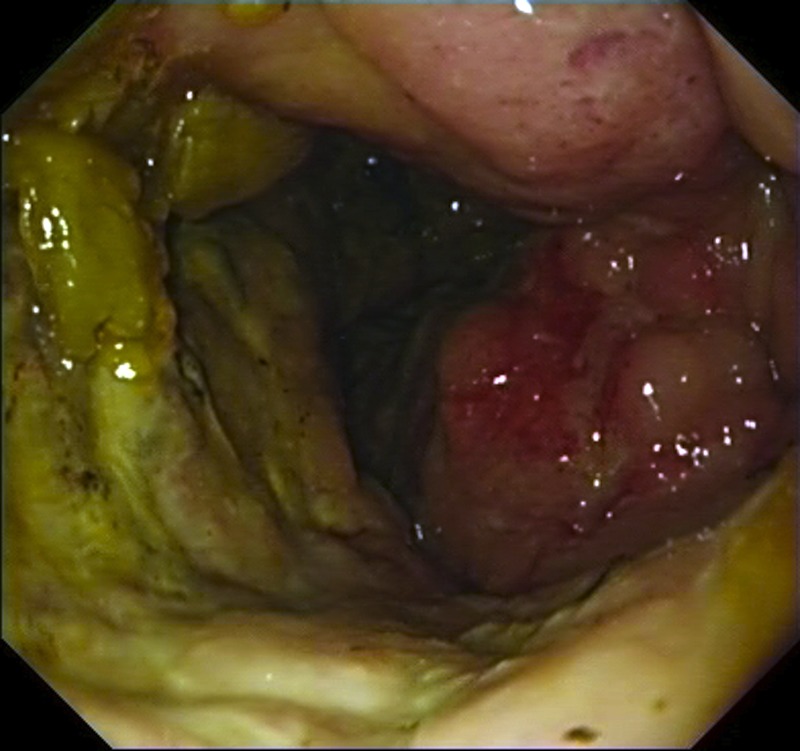
Abdominal CT Scan pictures, showing cystic type lesion, between liver and colonic hepatic flexure, in contact with the bowel outer layer expressing enriched wall and low density centre (Courtesy Dr. V. Penopoulos)
Infiltrated lymph nodes with both cancerous and atypical lymphocytes (Courtesy Dr. V. Penopoulos)
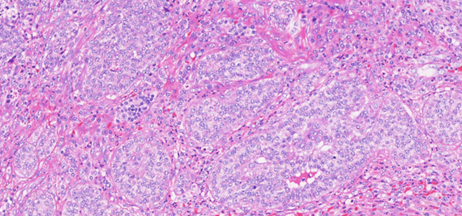
Immunohistochemical examination positive for synaptophysin (Courtesy Dr. V. Penopoulos)
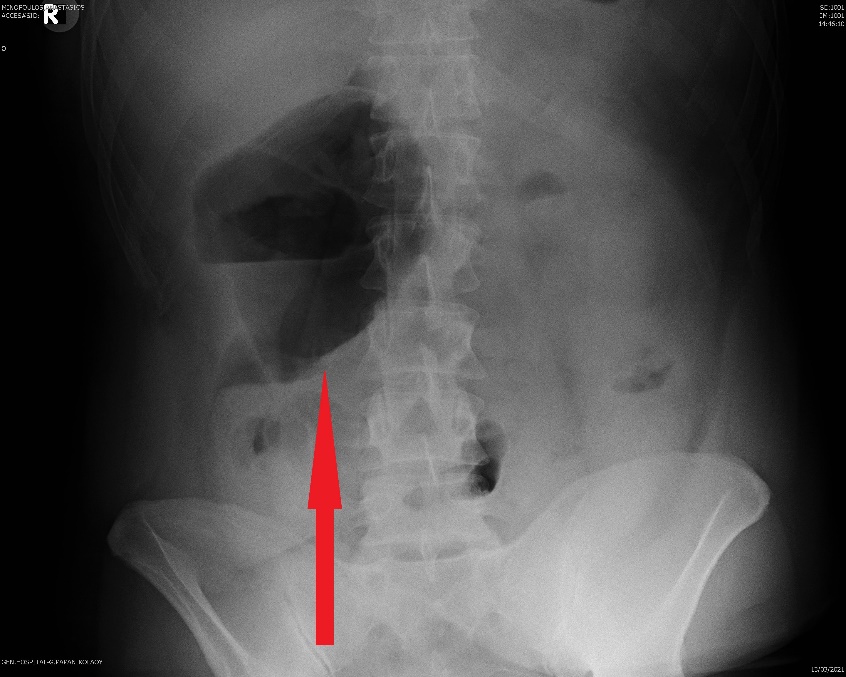
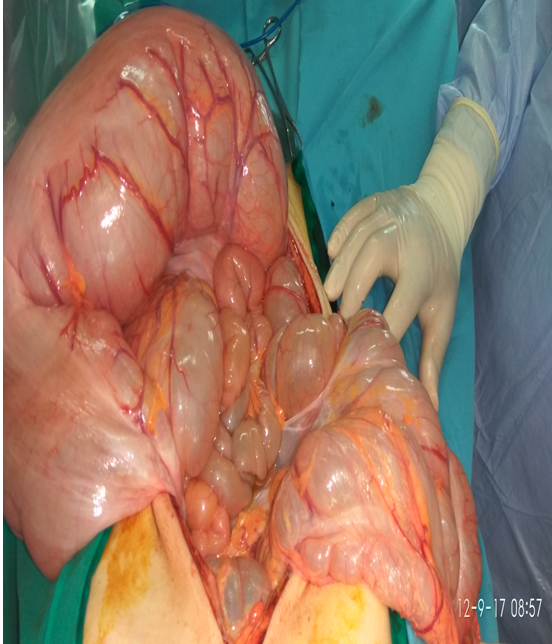
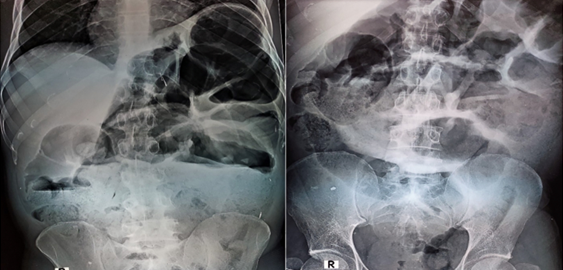
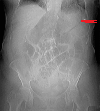
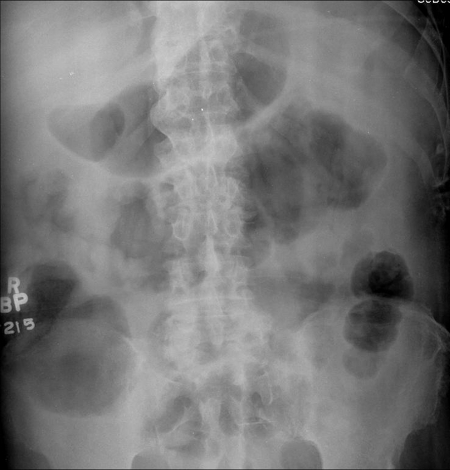
Plain abdominal radiograph. Distension of the ileal pouch and its displacement to the right side of the abdomen (Courtesy Dr. V. Penopoulos)
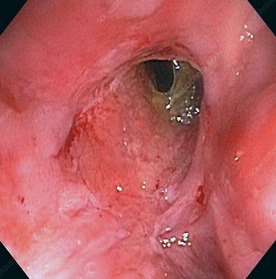
Postoperative biopsies of ileal pouch - Pouch adaptation (Courtesy Dr. V. Penopoulos)
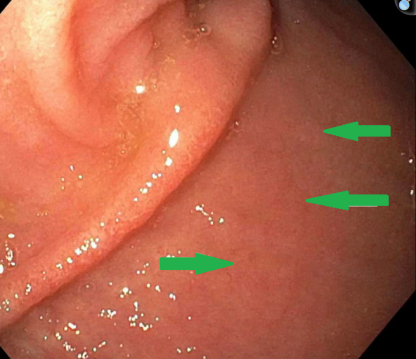
Postoperative biopsies of ileal pouch - Pouch adaptation (Courtesy Dr. V. Penopoulos)
Postoperative biopsies of ileal pouch - Pouch adaptation (Courtesy Dr. V. Penopoulos)
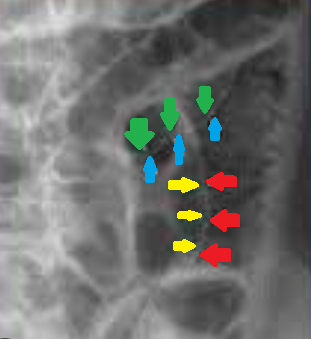
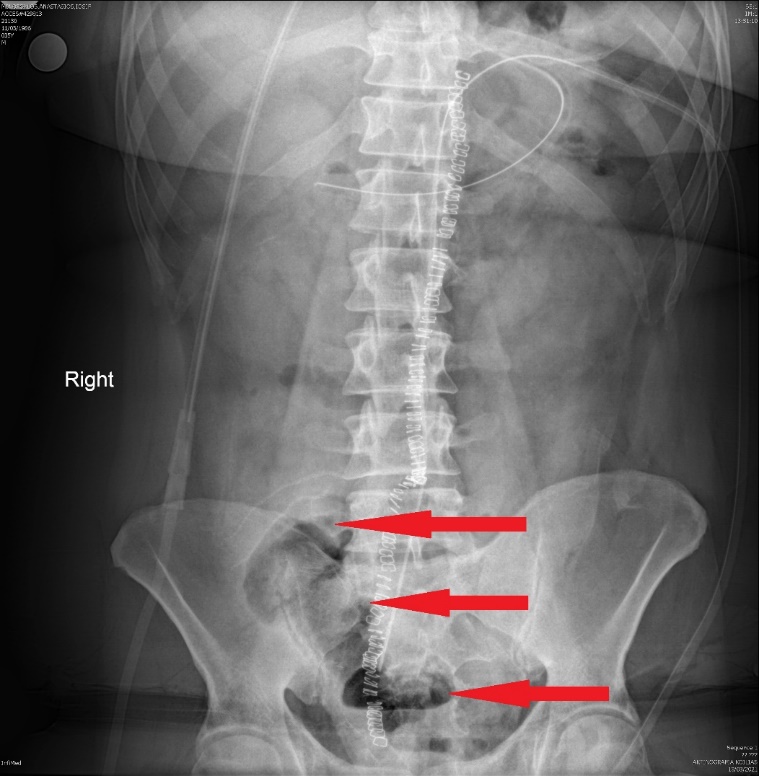
Plain abdominal radiograph - Multicolored arrows - Rigler sign (Courtesy Dr. V. Penopoulos)
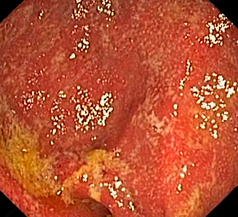
Postoperative biopsies of ileal pouch - Pouch adaptation (Courtesy Dr. V. Penopoulos)
Postoperative biopsies of ileal pouch - Pouch adaptation (Courtesy Dr. V. Penopoulos)
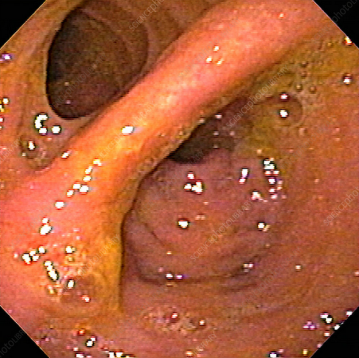
Postoperative biopsies of ileal pouch - Pouch adaptation (Courtesy Dr. V. Penopoulos)
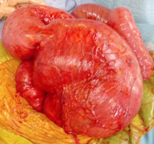
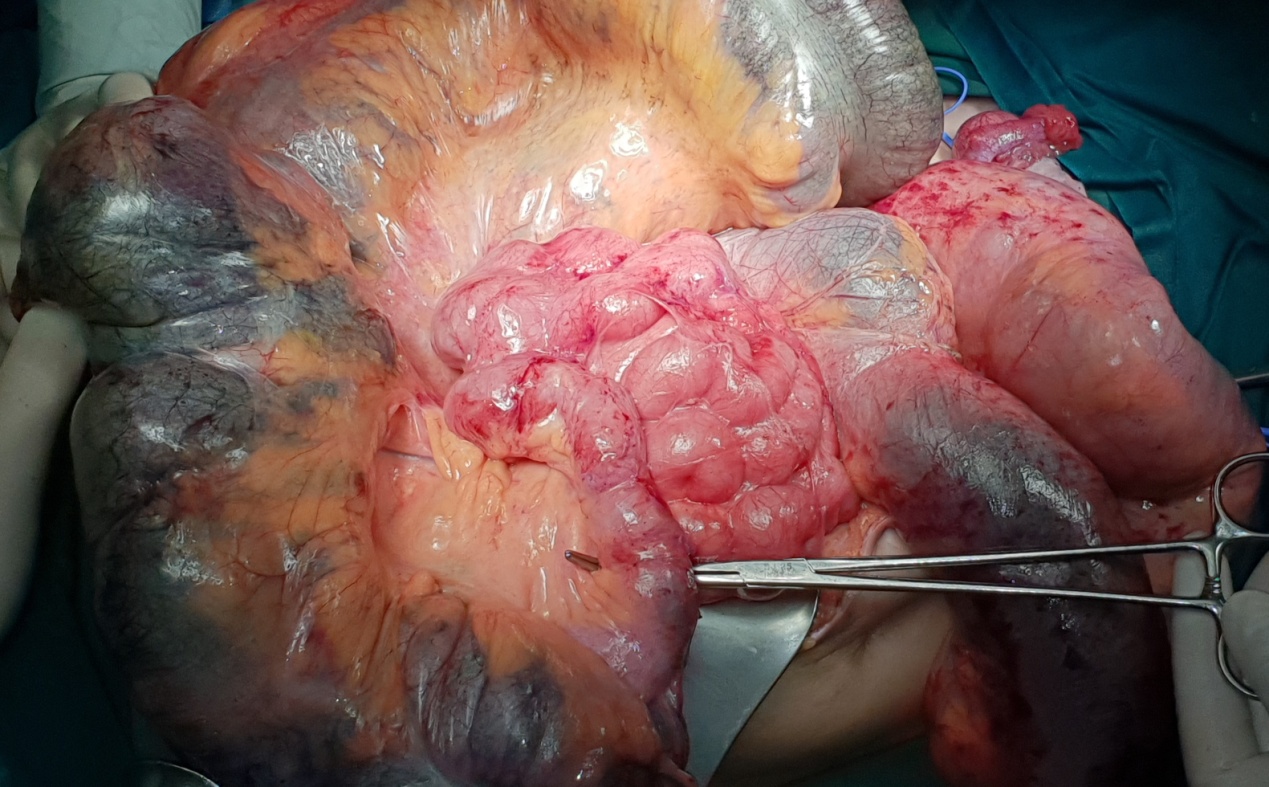
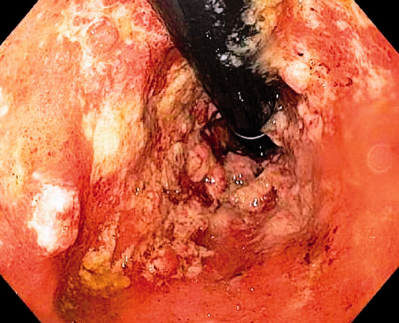
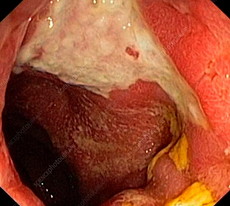
Intraoperative image of chronically inflamed, distended, dysfunctional pouch with associated proximal small bowel distension (Courtesy Dr. V. Penopoulos)
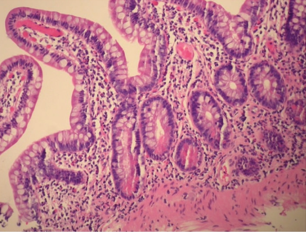
Postoperative biopsies of ileal pouch - Pouch adaptation (Courtesy Dr. V. Penopoulos)
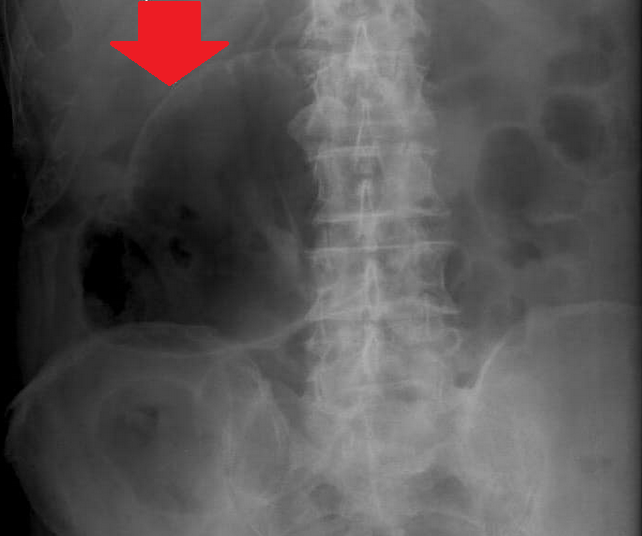
Plain abdominal radiograph - Multicolored arrows - Rigler sign (Courtesy Dr. V. Penopoulos)
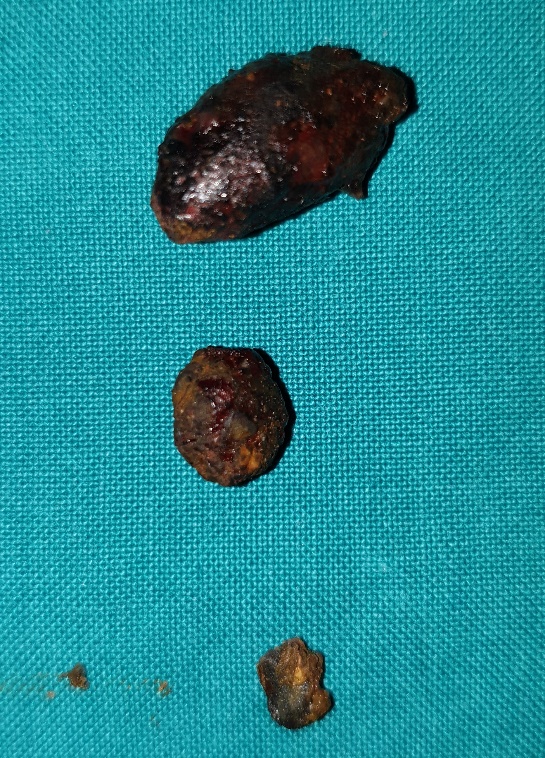
Photomicrograph of a hematoxylin and eosin-stained tissue section revealing the neuroendocrine tumor cells (Courtesy Dr. V. Penopoulos)
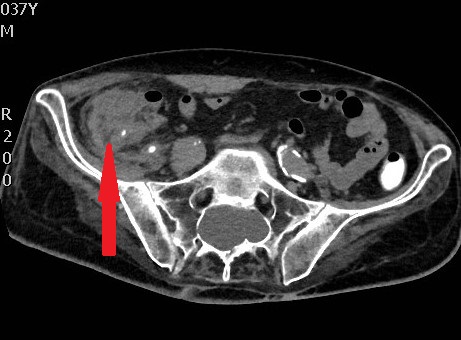
Photomicrograph of a hematoxylin and eosin-stained tissue section revealing the neuroendocrine tumor cells (Courtesy Dr. V. Penopoulos)
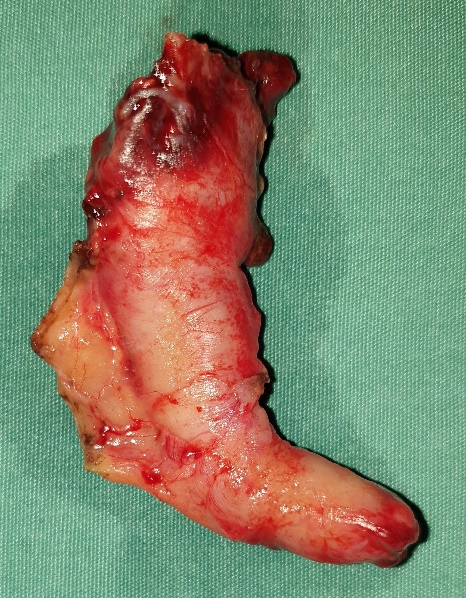
Photomicrograph of a hematoxylin and eosin-stained tissue section revealing the neuroendocrine tumor cells (Courtesy Dr. V. Penopoulos)
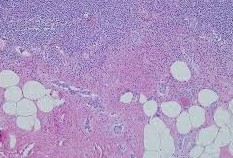
Photomicrograph of a hematoxylin and eosin-stained tissue section revealing the neuroendocrine tumor cells (Courtesy Dr. V. Penopoulos)
Colectomies
(0 images)No images in this chapter yet.
Proctectomies
(0 images)No images in this chapter yet.