Small Intestine
Λεπτό Έντερο
180 images
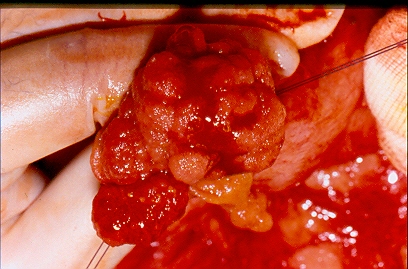
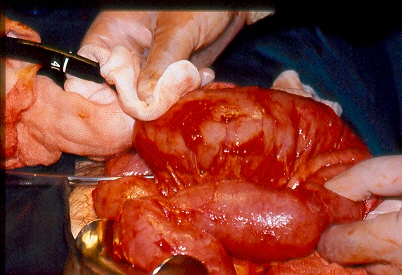
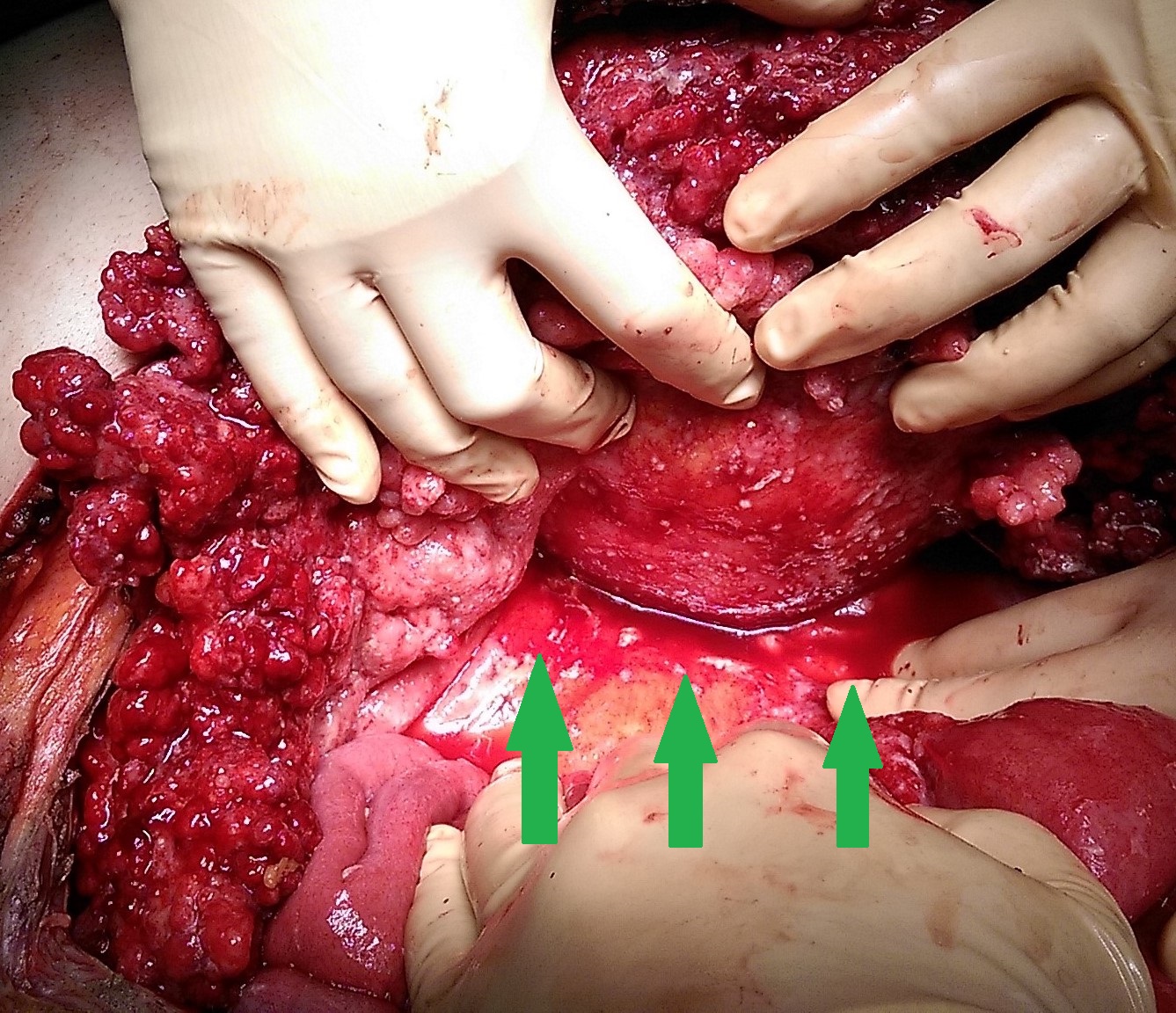
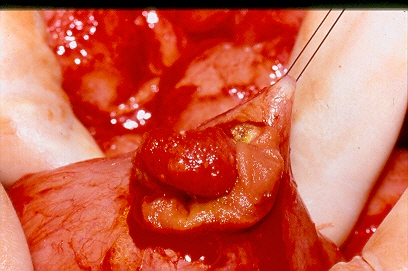
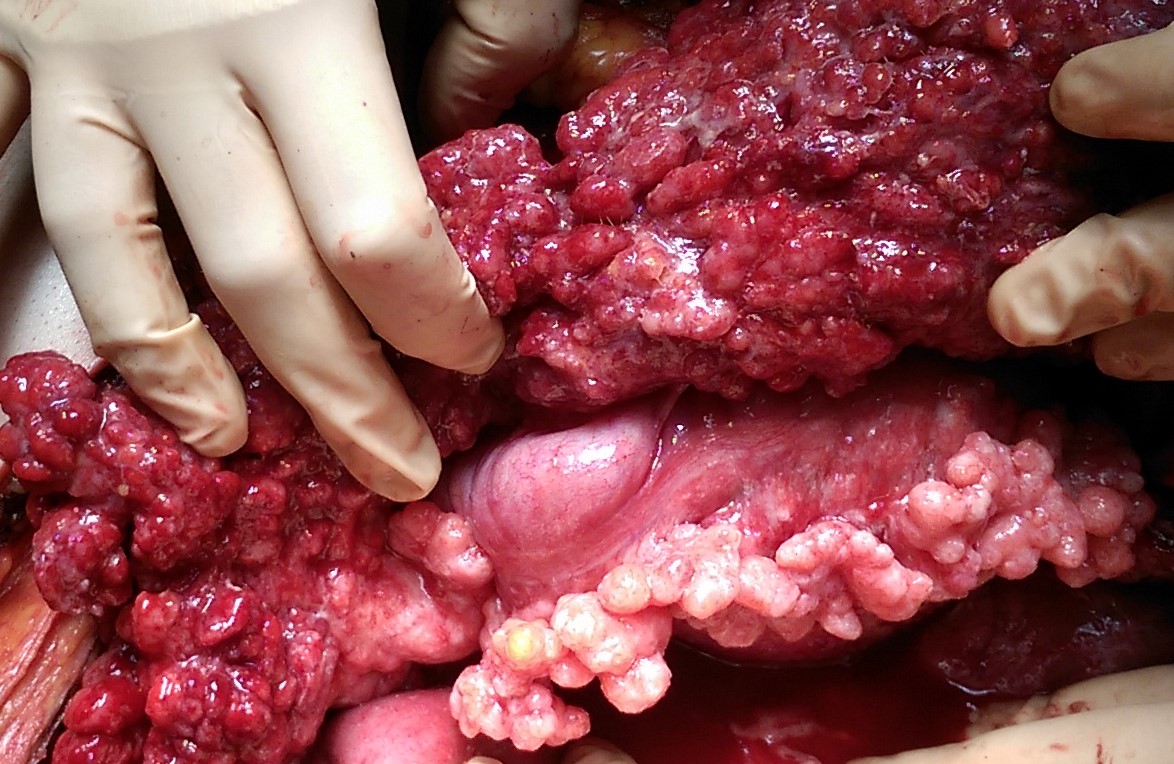
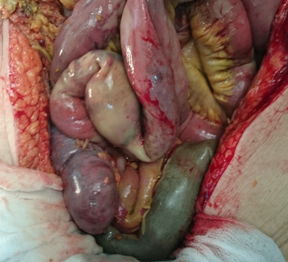
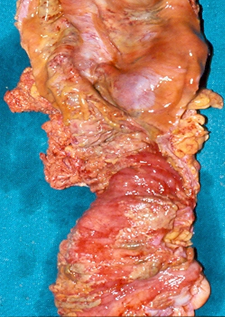
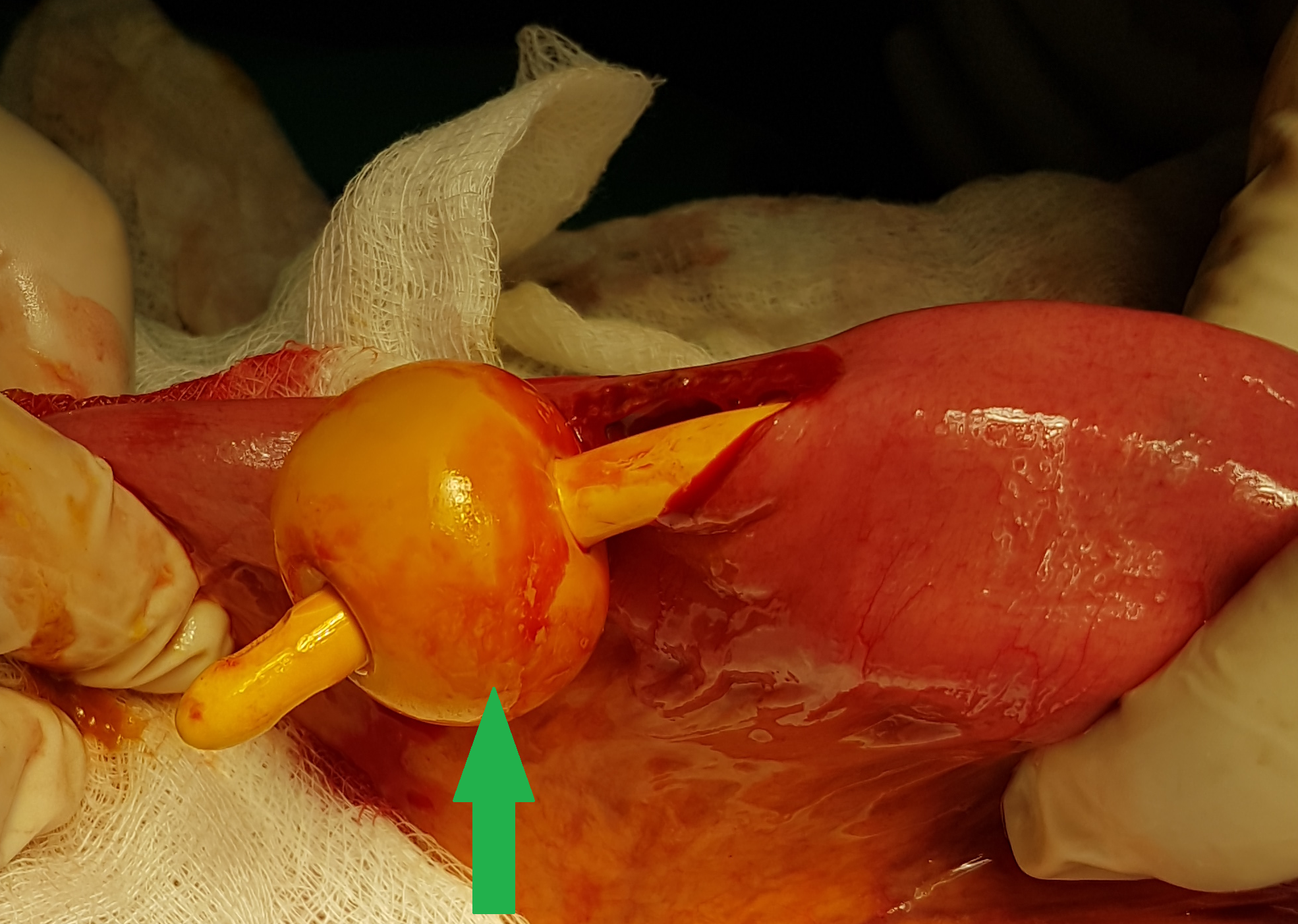
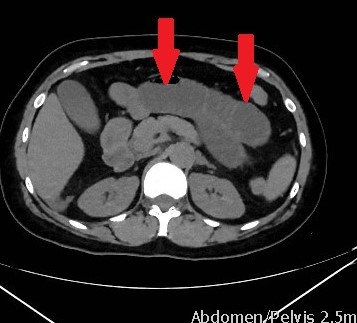
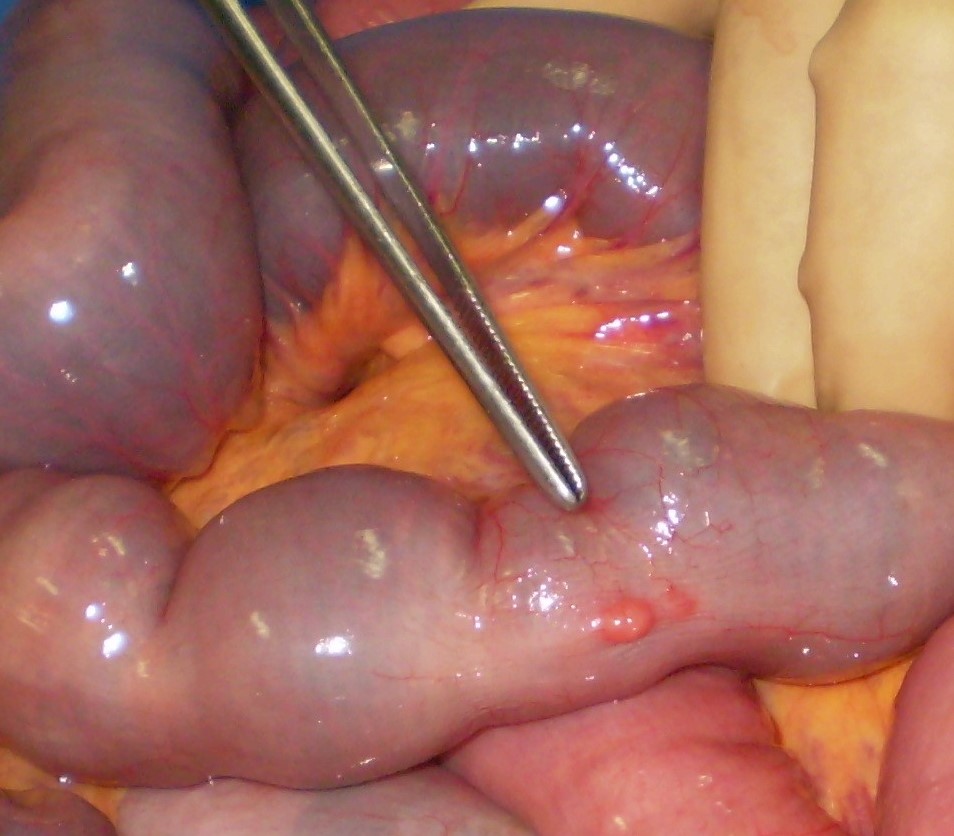
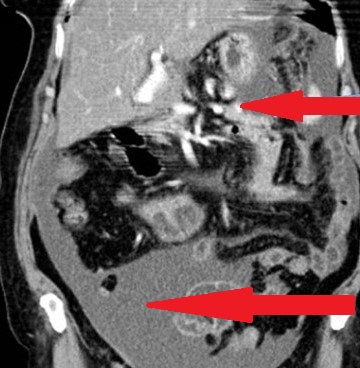
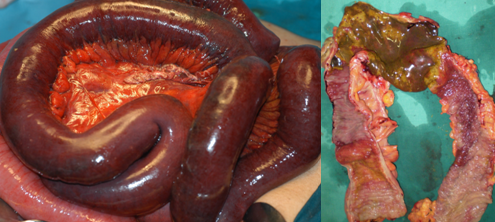
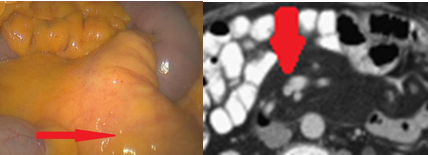
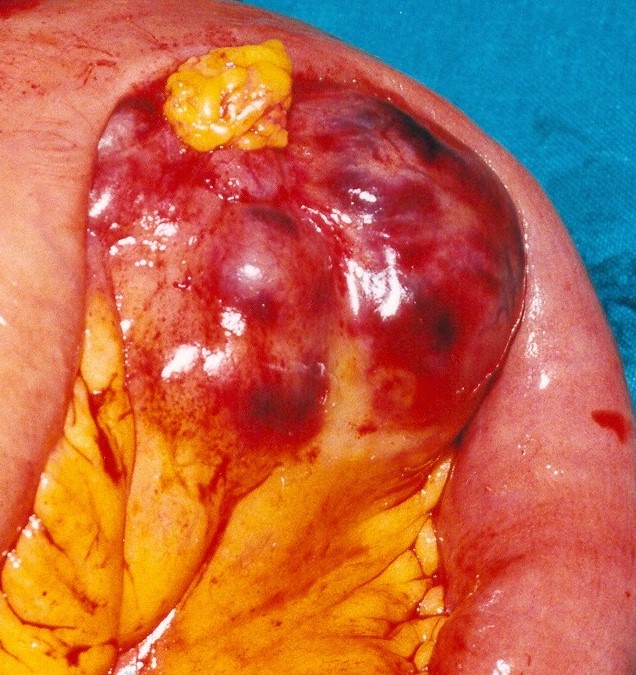
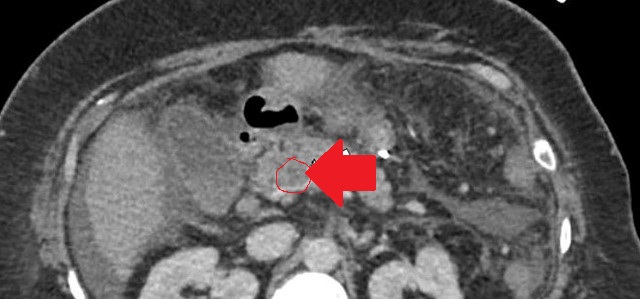
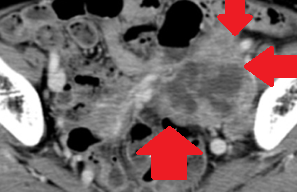
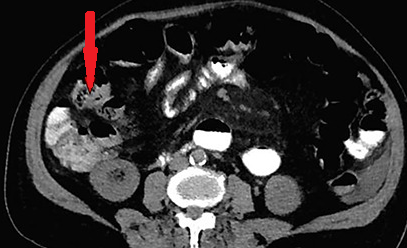
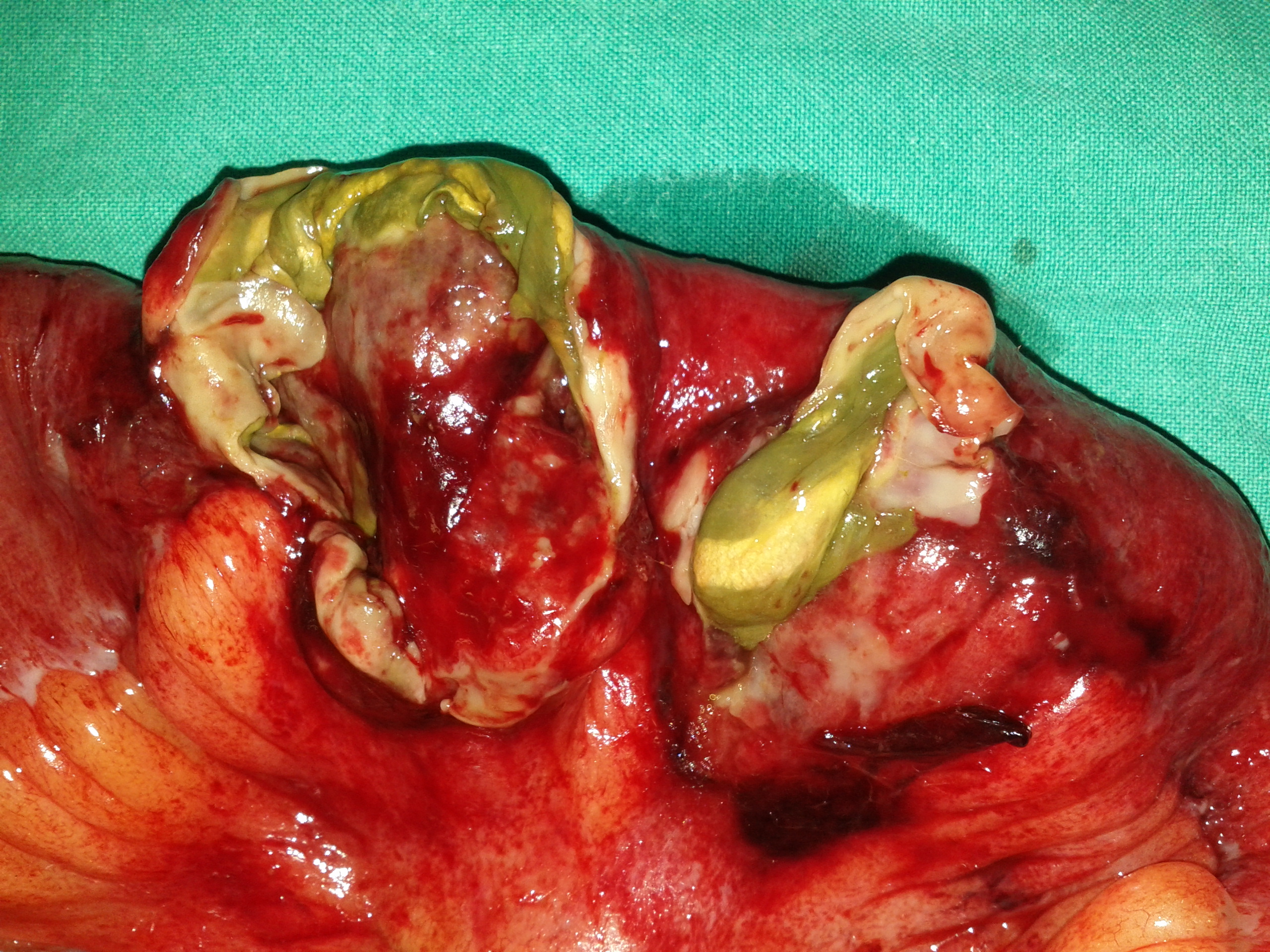
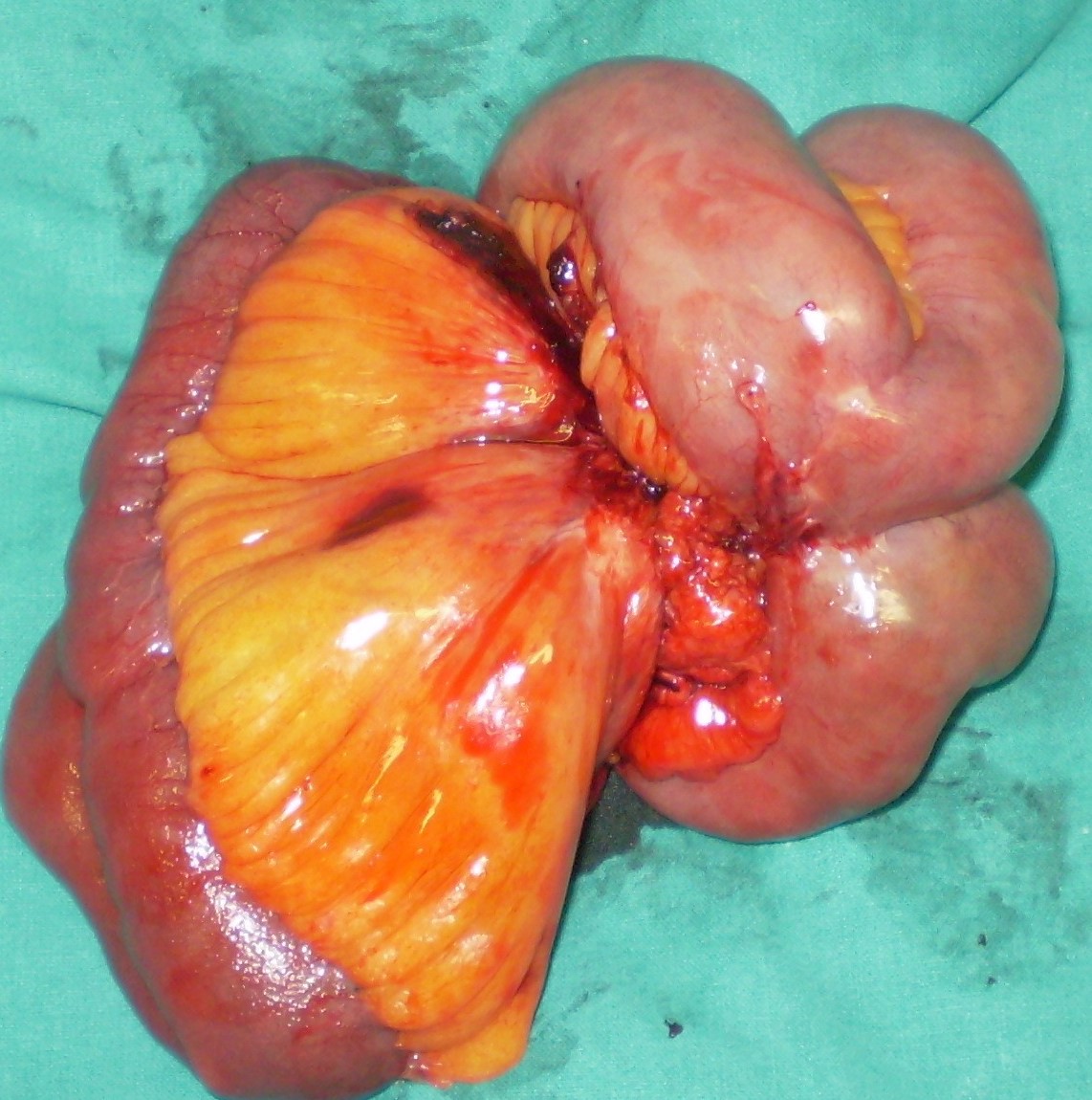
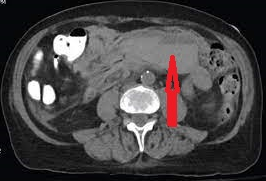
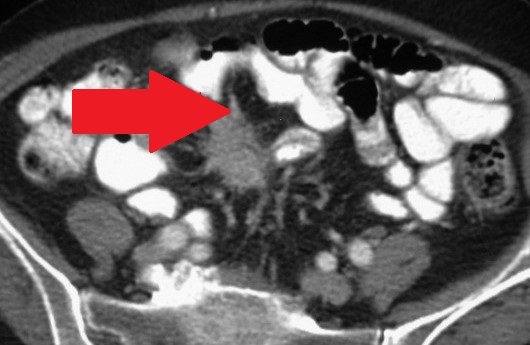
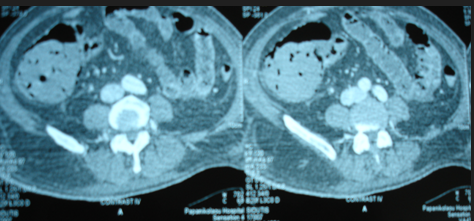
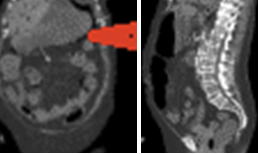
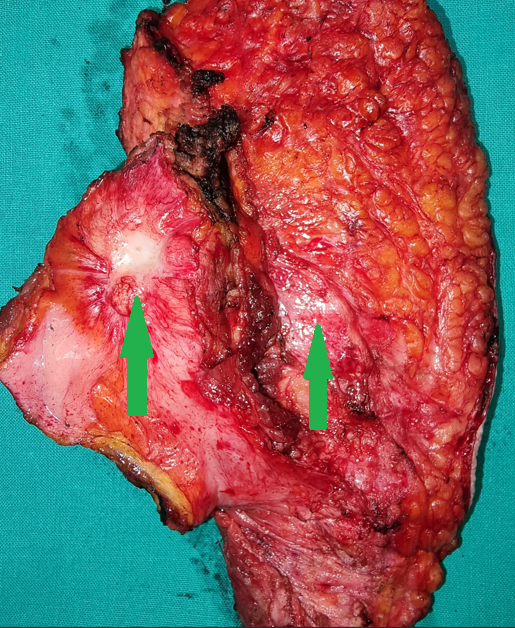
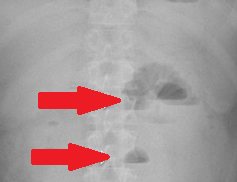
The two metastatic foci causing stenosis and bowel obstruction are clearly visible (Courtesy Dr. V. Penopoulos)
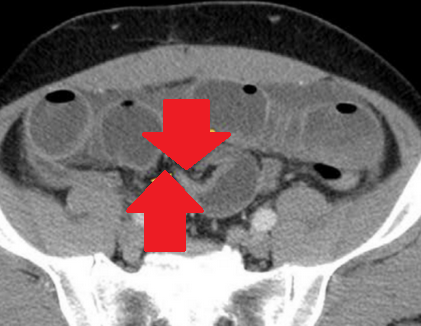
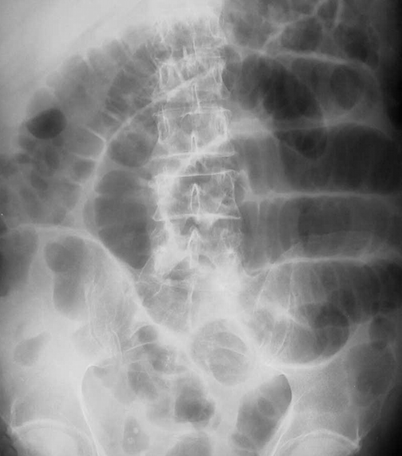
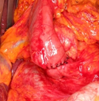
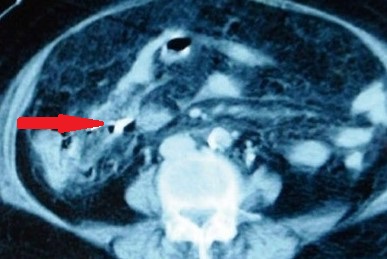
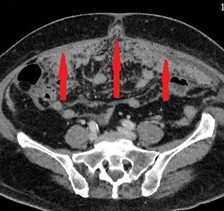
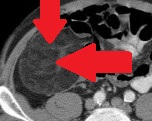
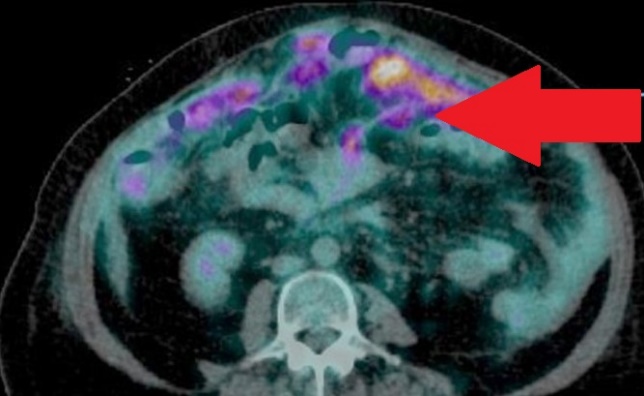
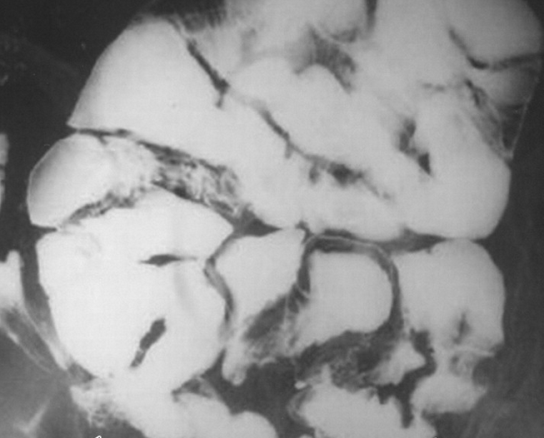
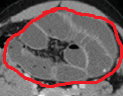
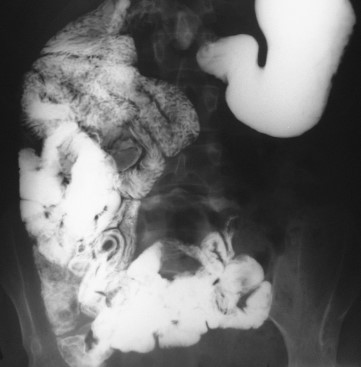
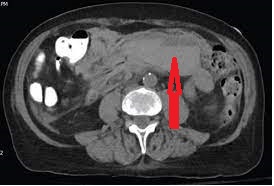
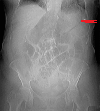
Red arrows — transition point. Multiple air-fluid levels (Courtesy Dr. V. Penopoulos)
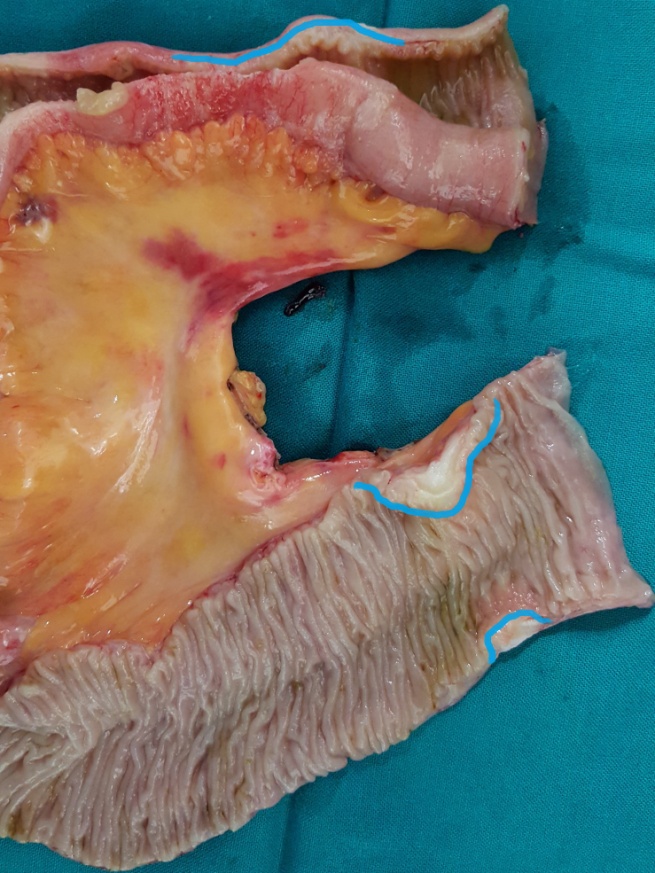
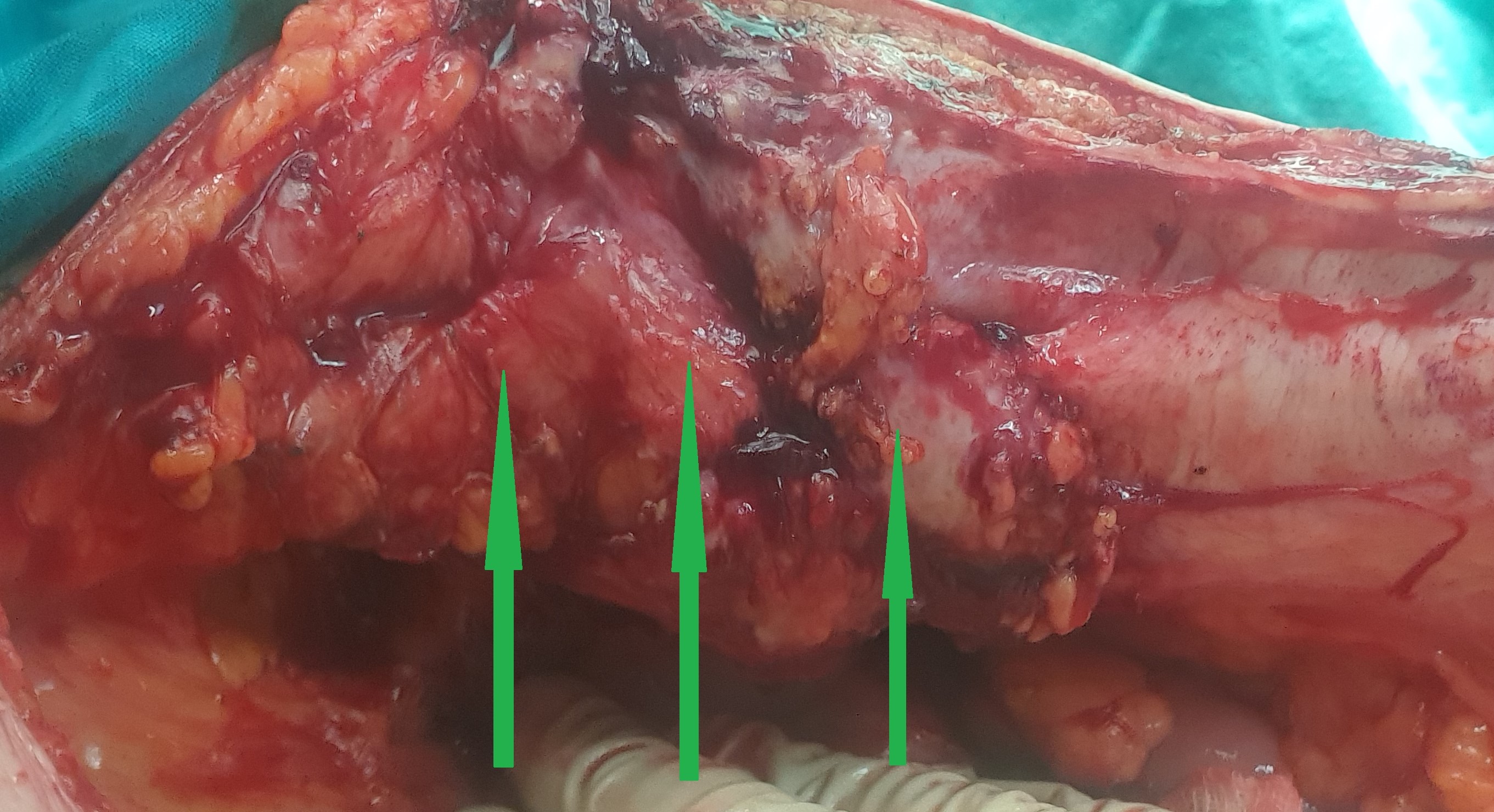
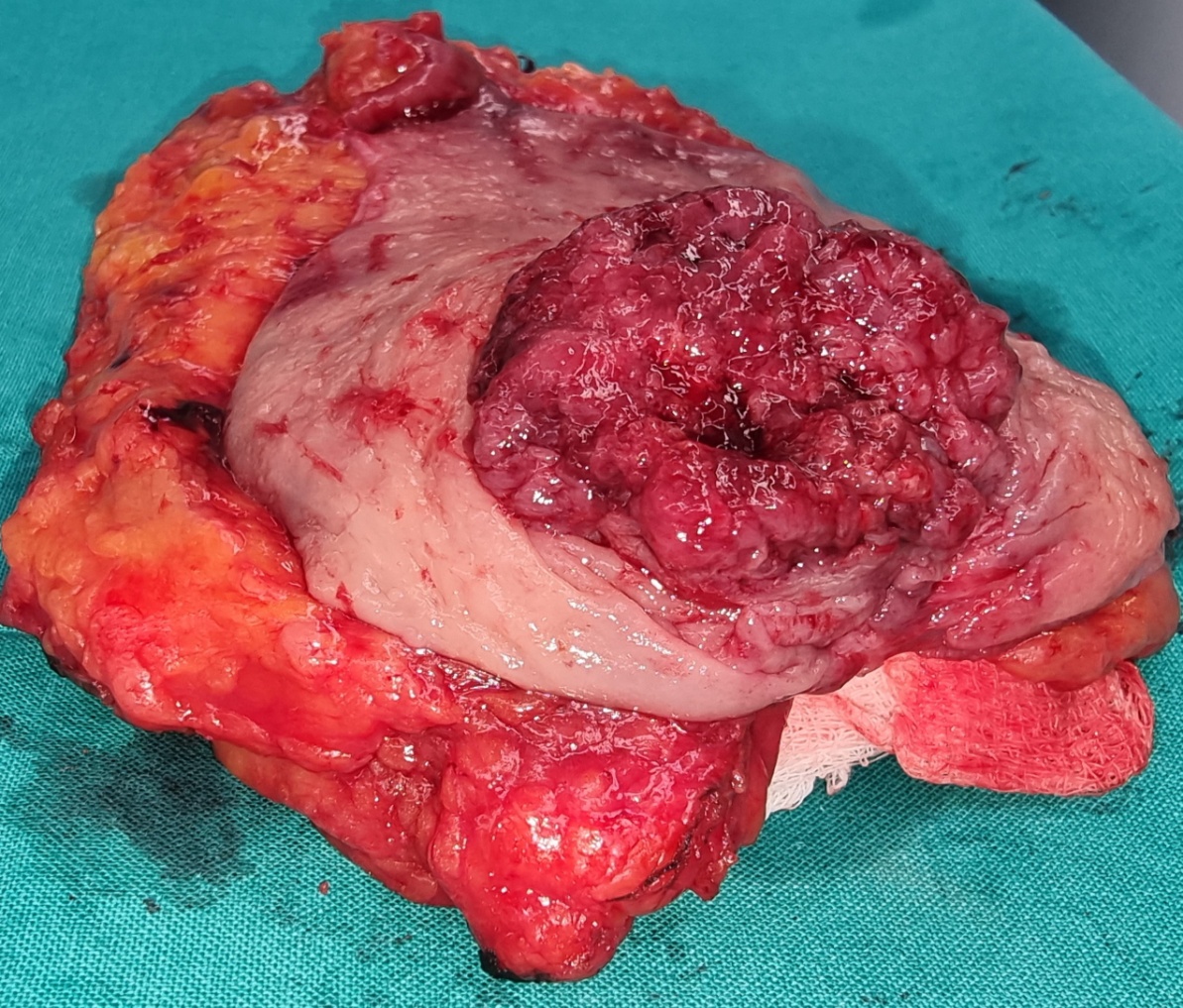
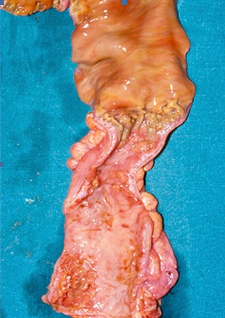
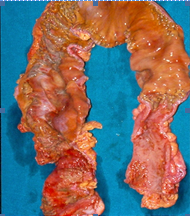
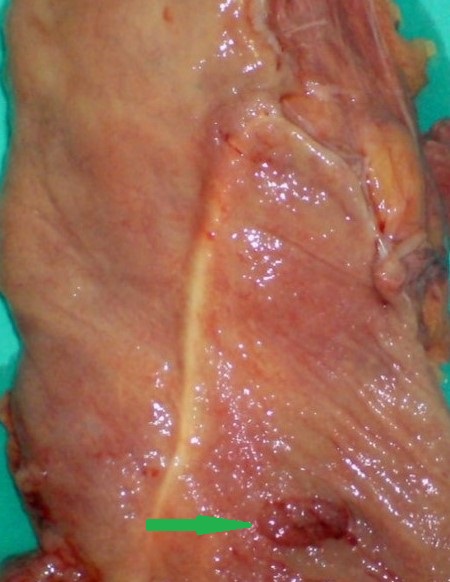
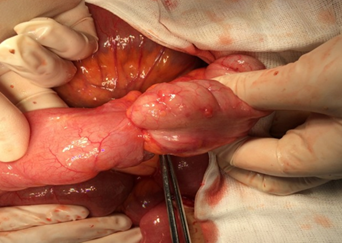
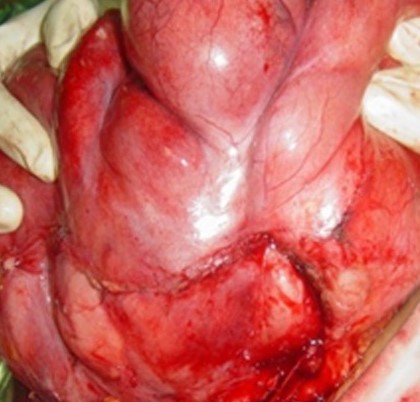
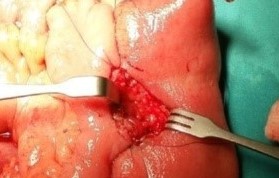
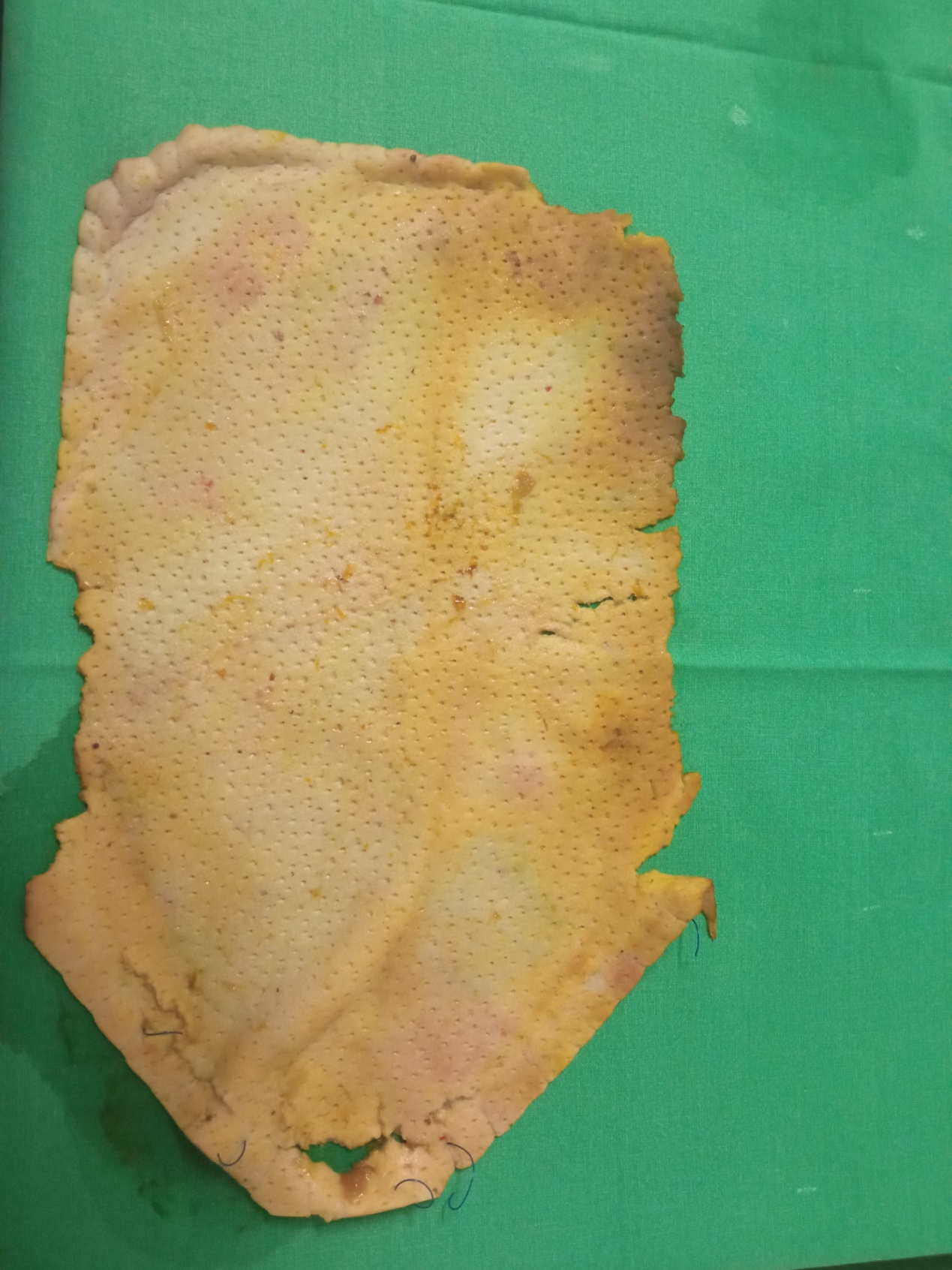
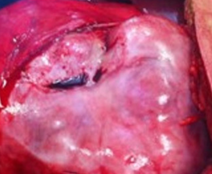
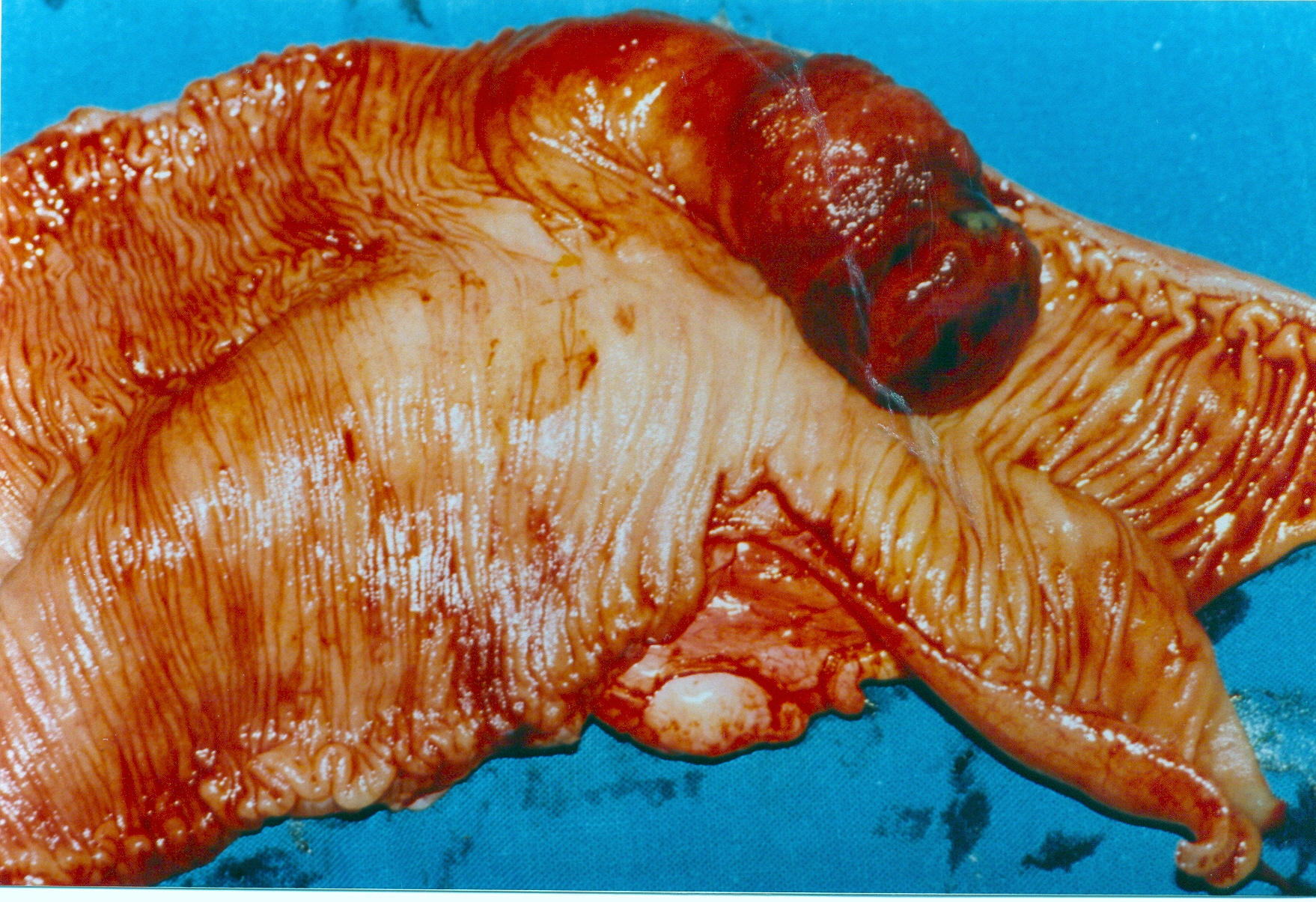
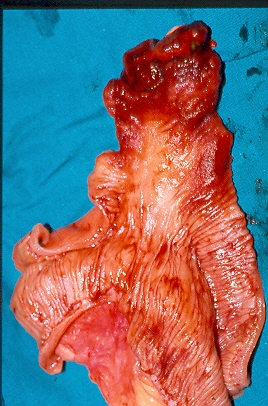
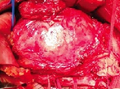
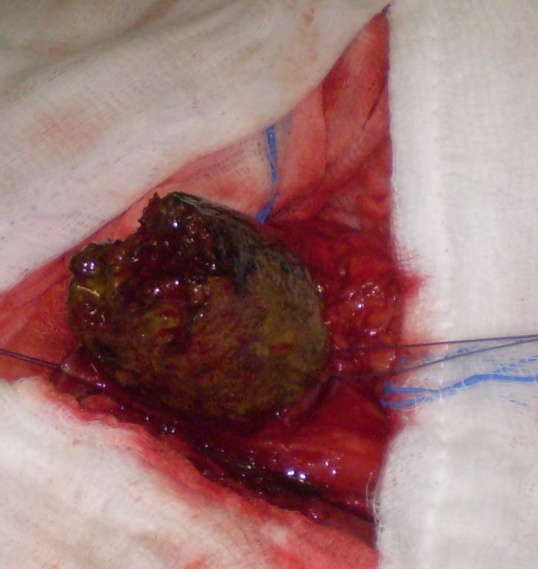
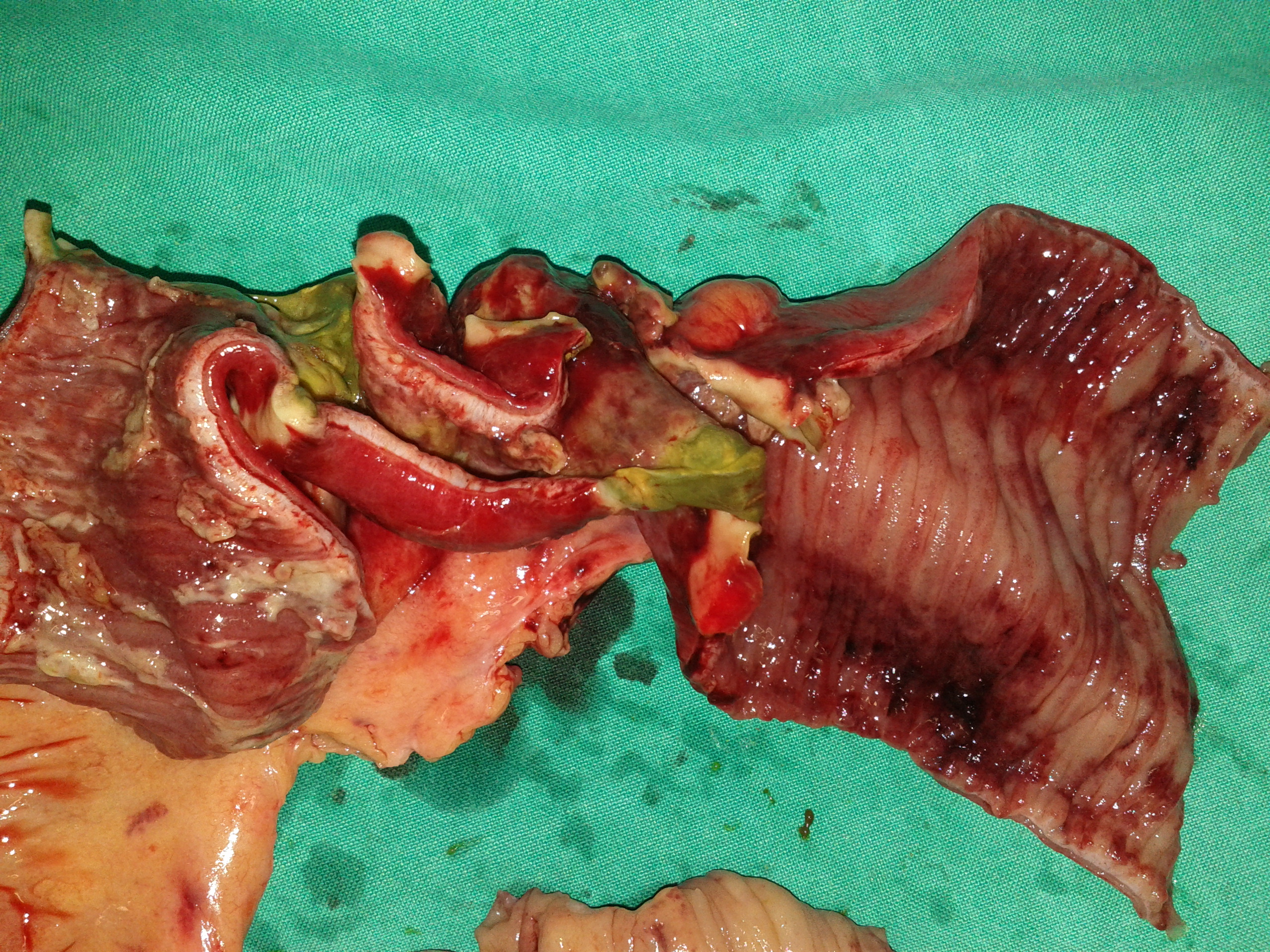
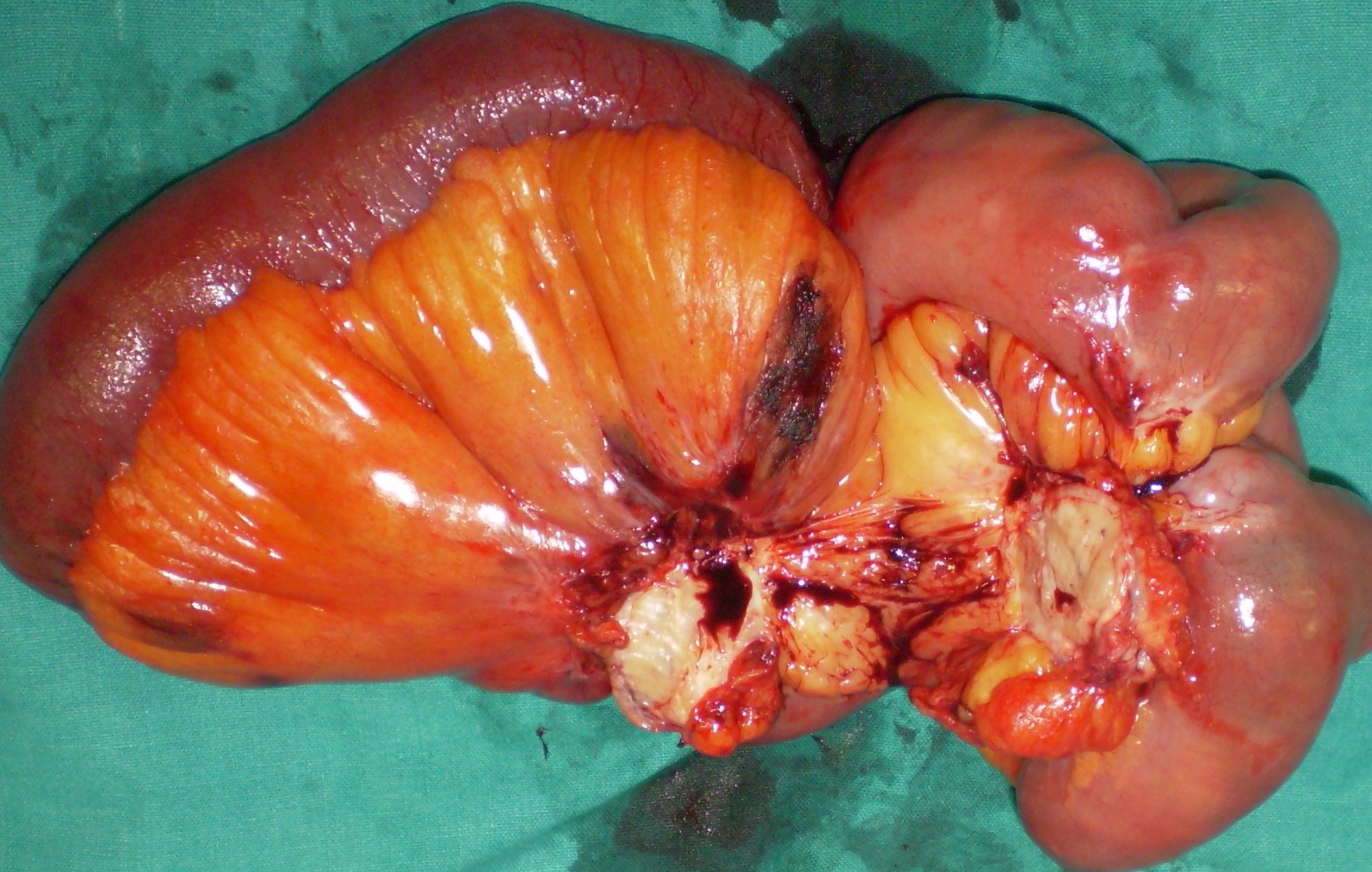
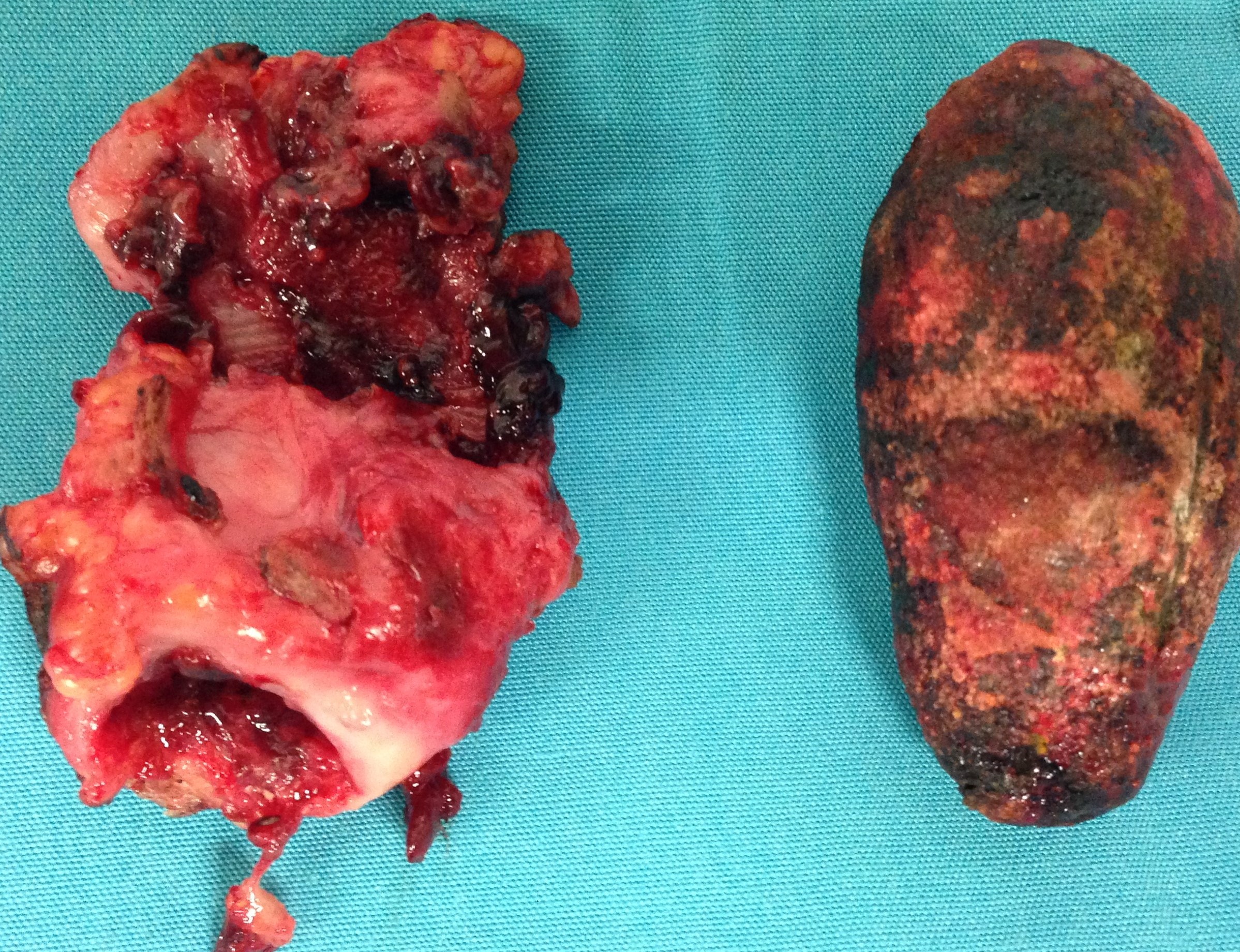
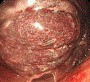
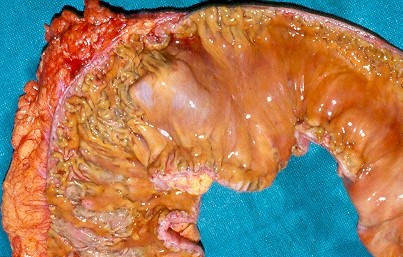
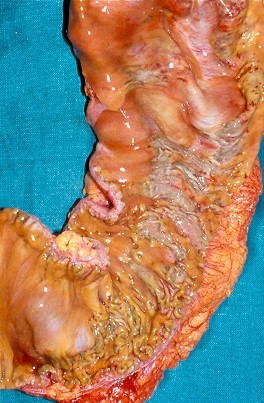
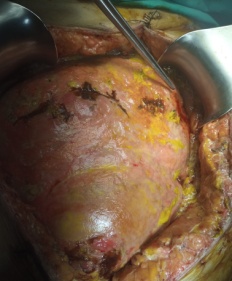
After opening the specimen, the metastatic foci are clearly visible (Courtesy Dr. V. Penopoulos)
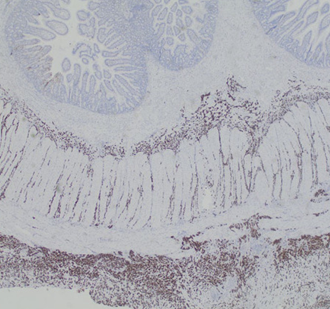
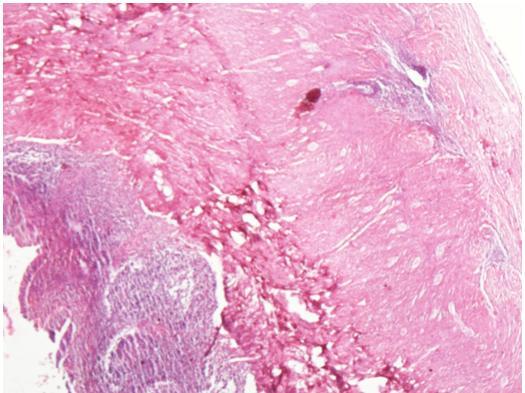
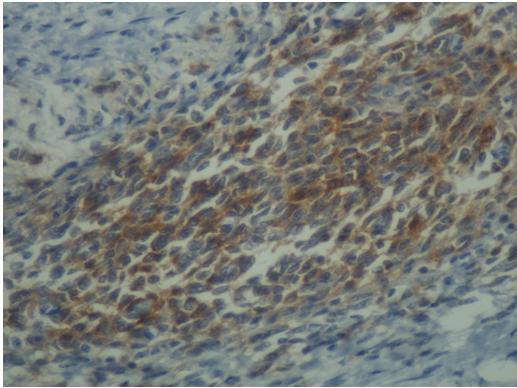
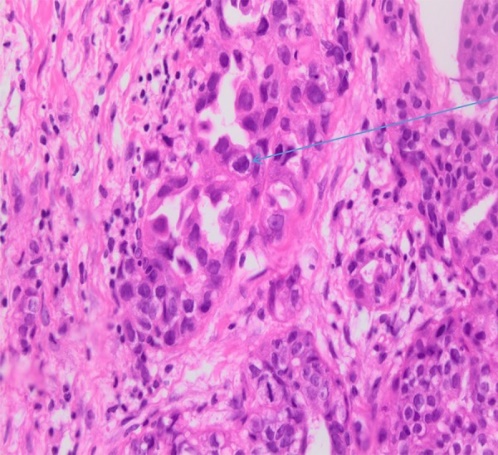
Immunohistochemical staining for Cytokeratin 7, demonstrating the diffusely infiltrating carcinoma in the submucosa, muscular wall, mesenteric adipose tissue, and serosa (Courtesy Dr. V. Penopoulos)
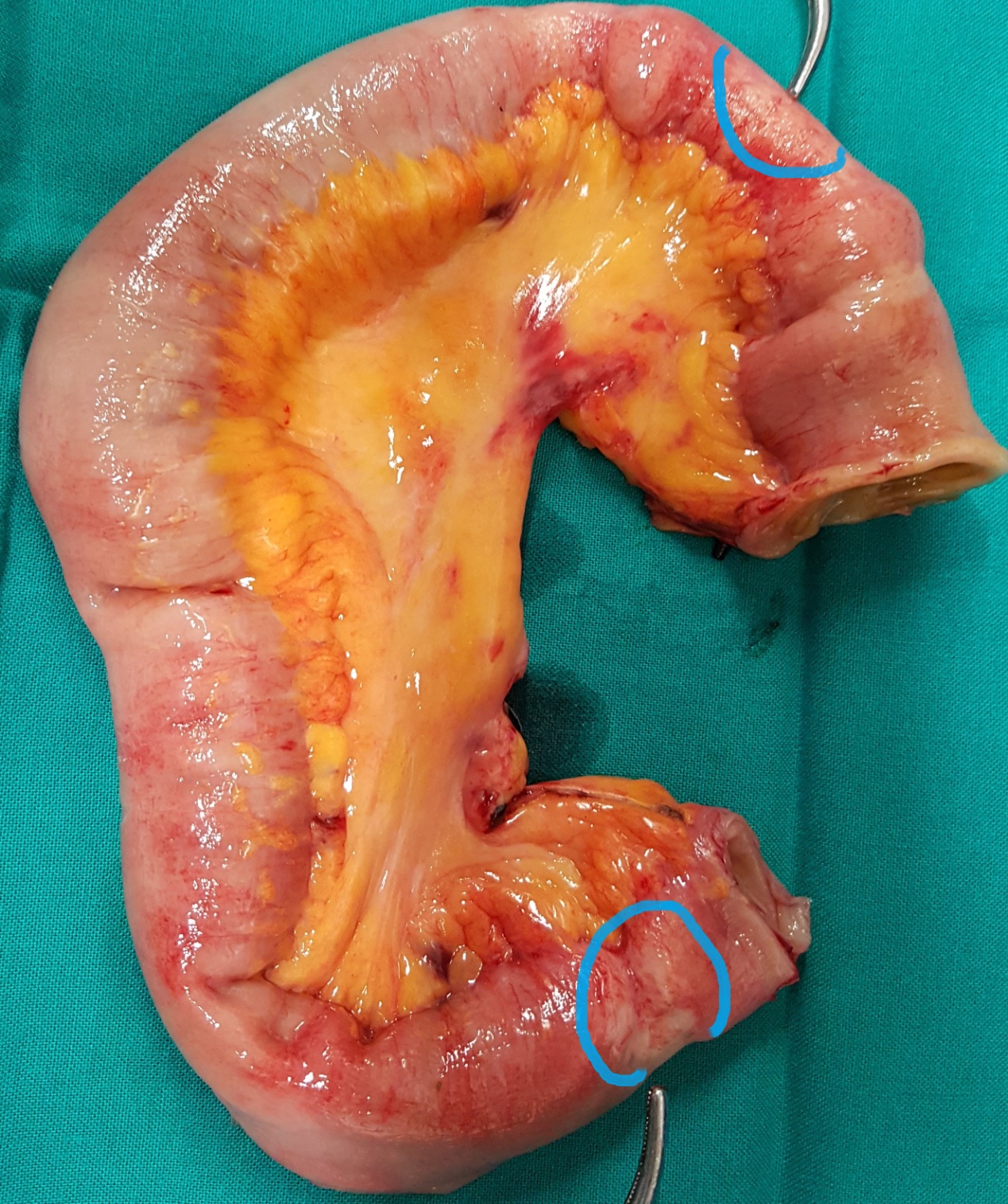
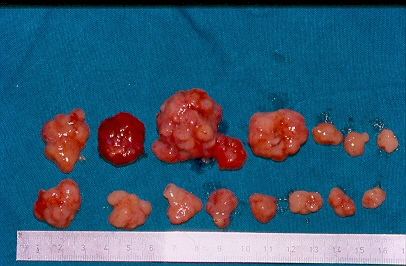
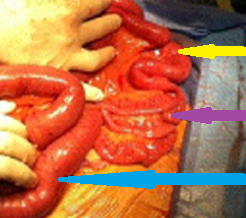
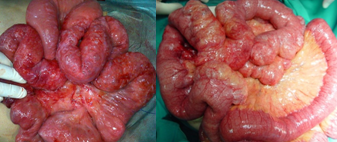
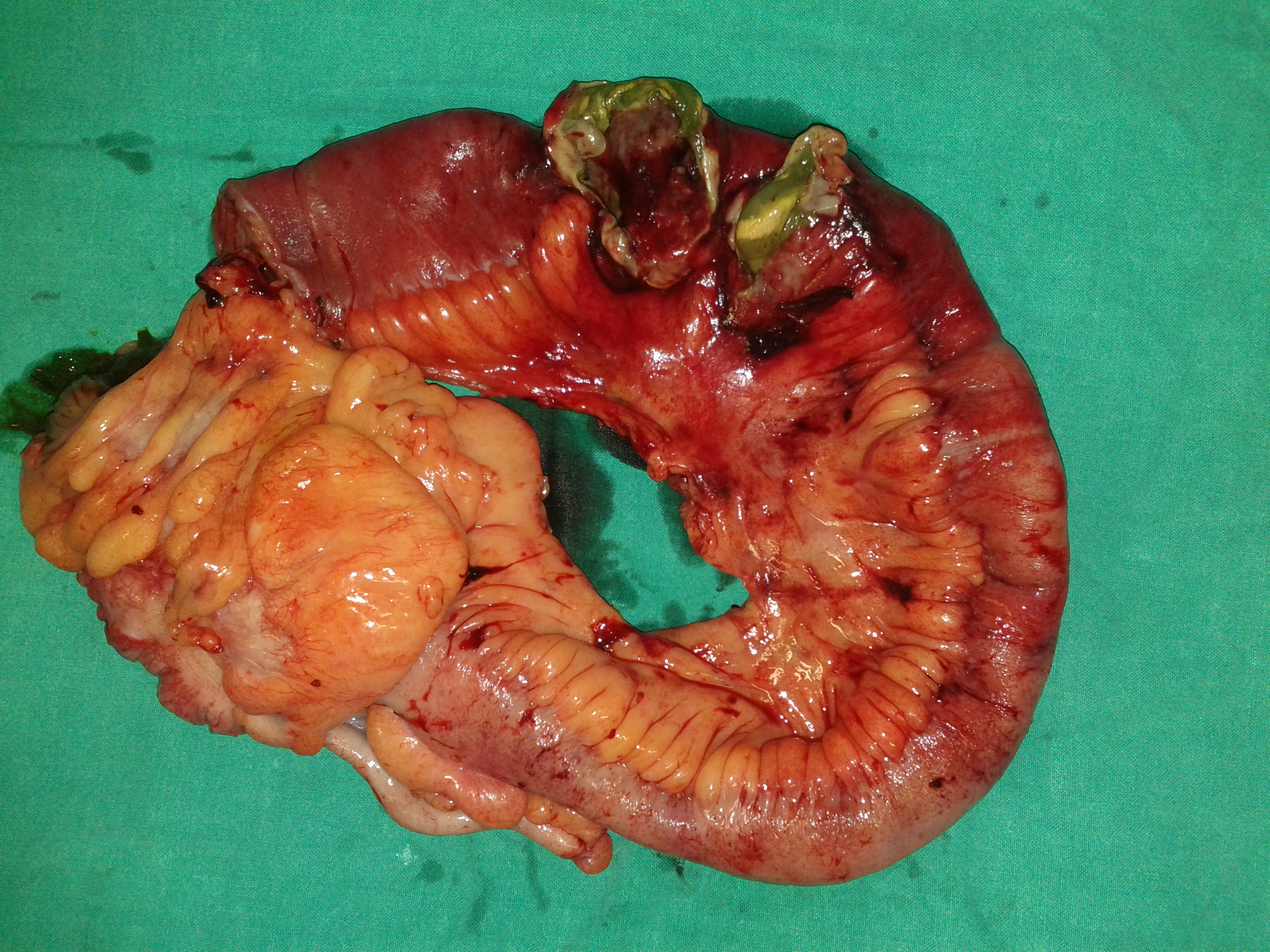
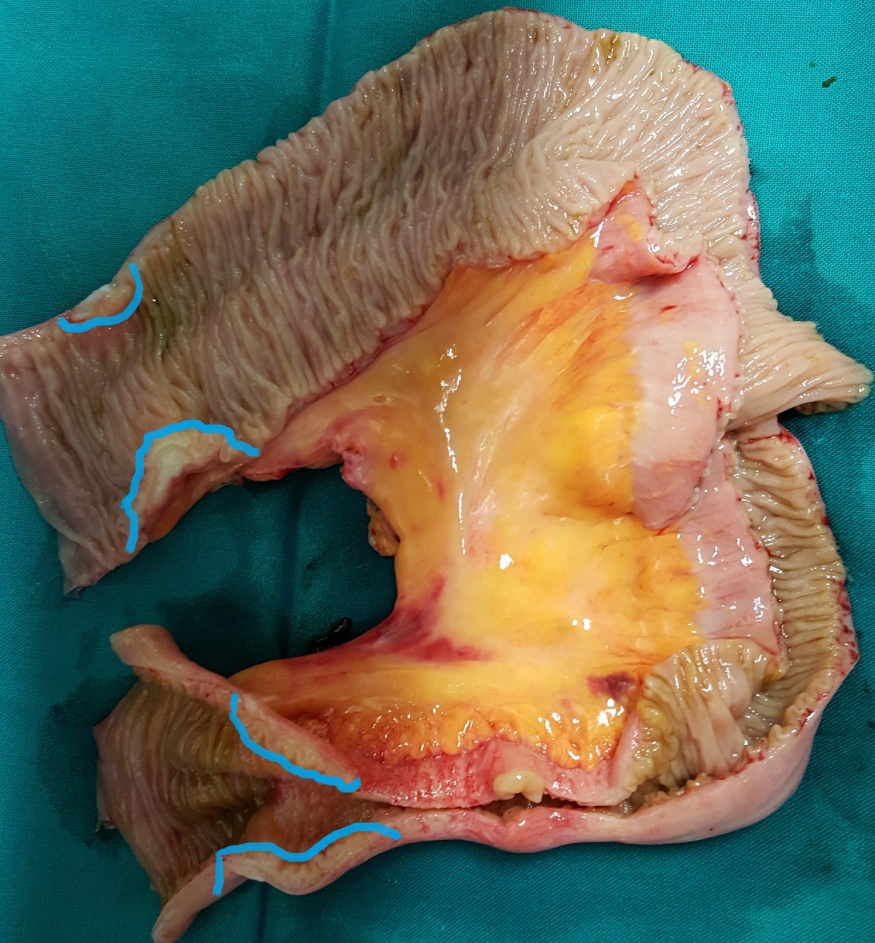
Resected obstructed ileal loop. Blue circles enclose the metastatic foci (Courtesy Dr. V. Penopoulos)
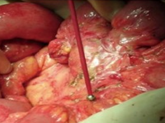
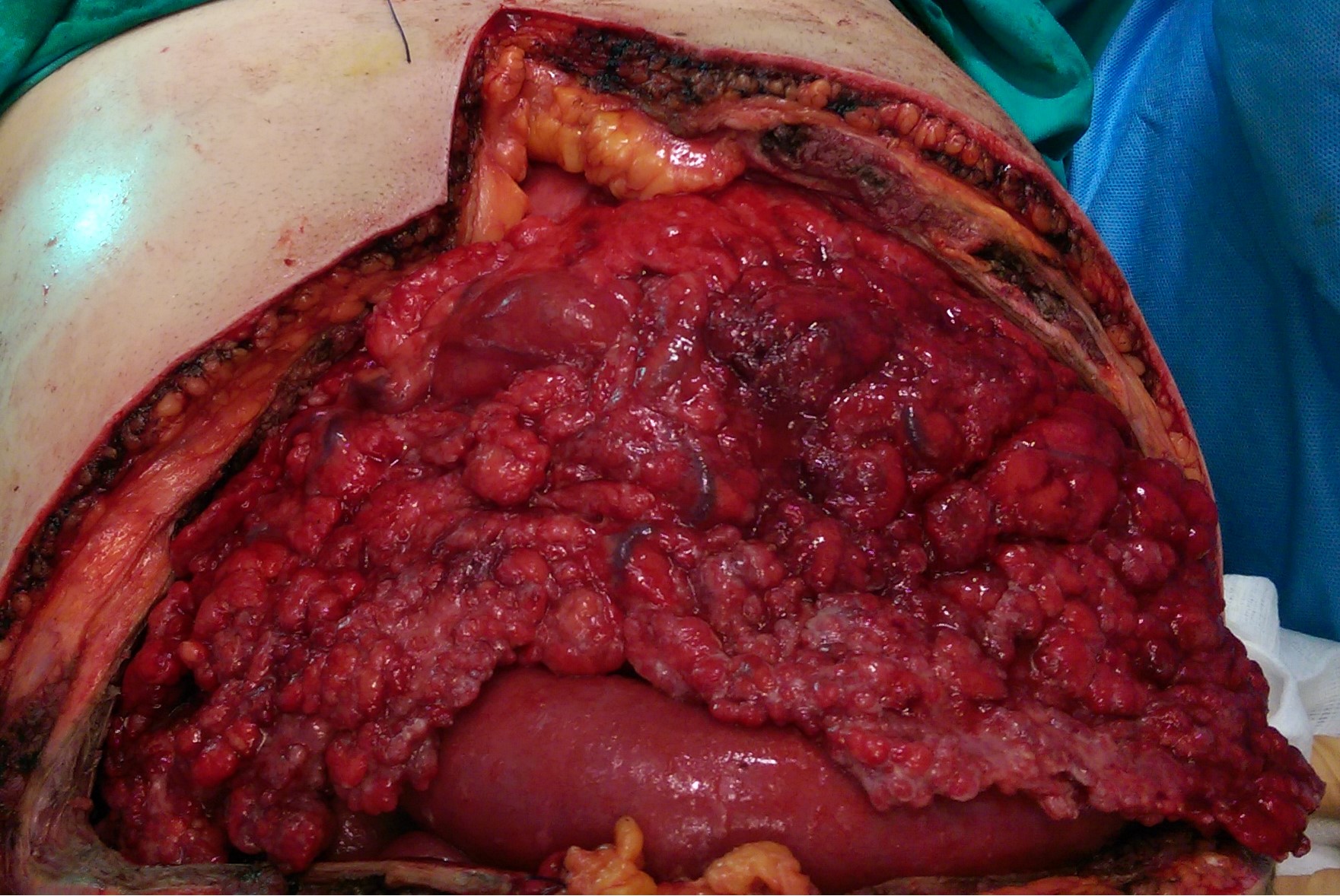
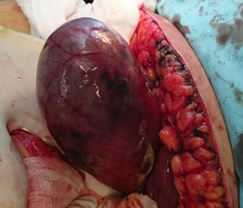
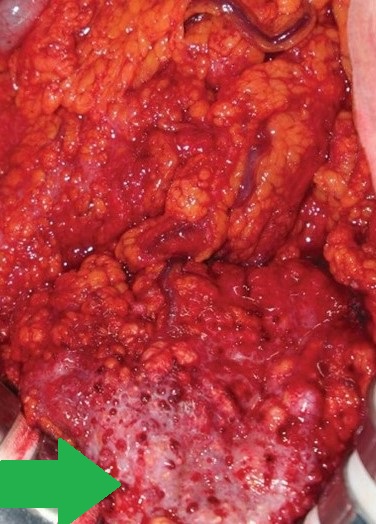
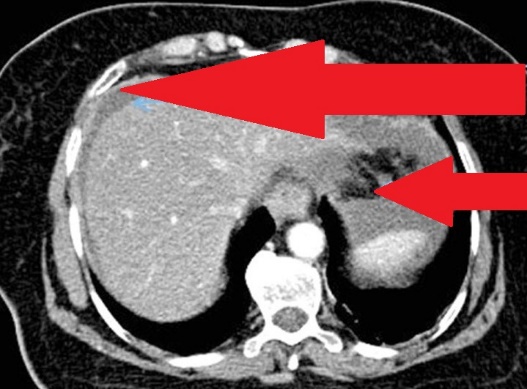
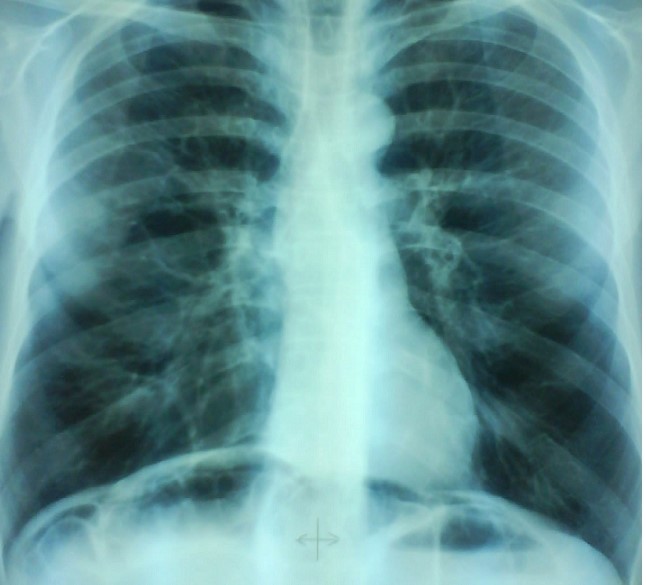
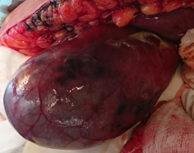
Multiple hepatic metastases — Absolute contraindication for cytoreductive surgery (Courtesy Dr. V. Penopoulos)
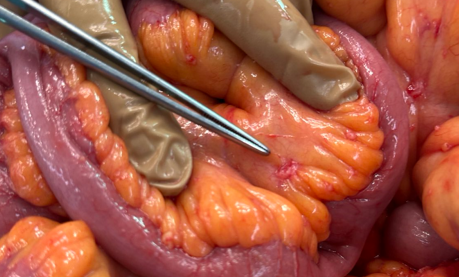
Multiple hepatic metastases — Absolute contraindication for cytoreductive surgery (Courtesy Dr. V. Penopoulos)
Multiple hepatic metastases — Absolute contraindication for cytoreductive surgery (Courtesy Dr. V. Penopoulos)
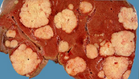
Multiple hepatic metastases — Absolute contraindication for cytoreductive surgery (Courtesy Dr. V. Penopoulos)
Closed systems for hyperthermic intraperitoneal chemotherapy (Courtesy Dr. V. Penopoulos)
Multiple hepatic metastases — Absolute contraindication for cytoreductive surgery (Courtesy Dr. V. Penopoulos)
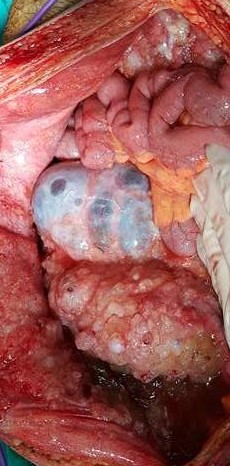
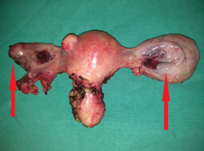
Peritoneal carcinomatosis (gallbladder ca). Ovarian metastases (Courtesy Dr. V. Penopoulos)
Multiple hepatic metastases — Absolute contraindication for cytoreductive surgery (Courtesy Dr. V. Penopoulos)
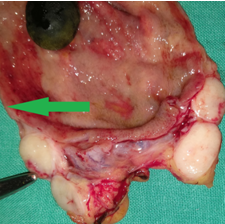
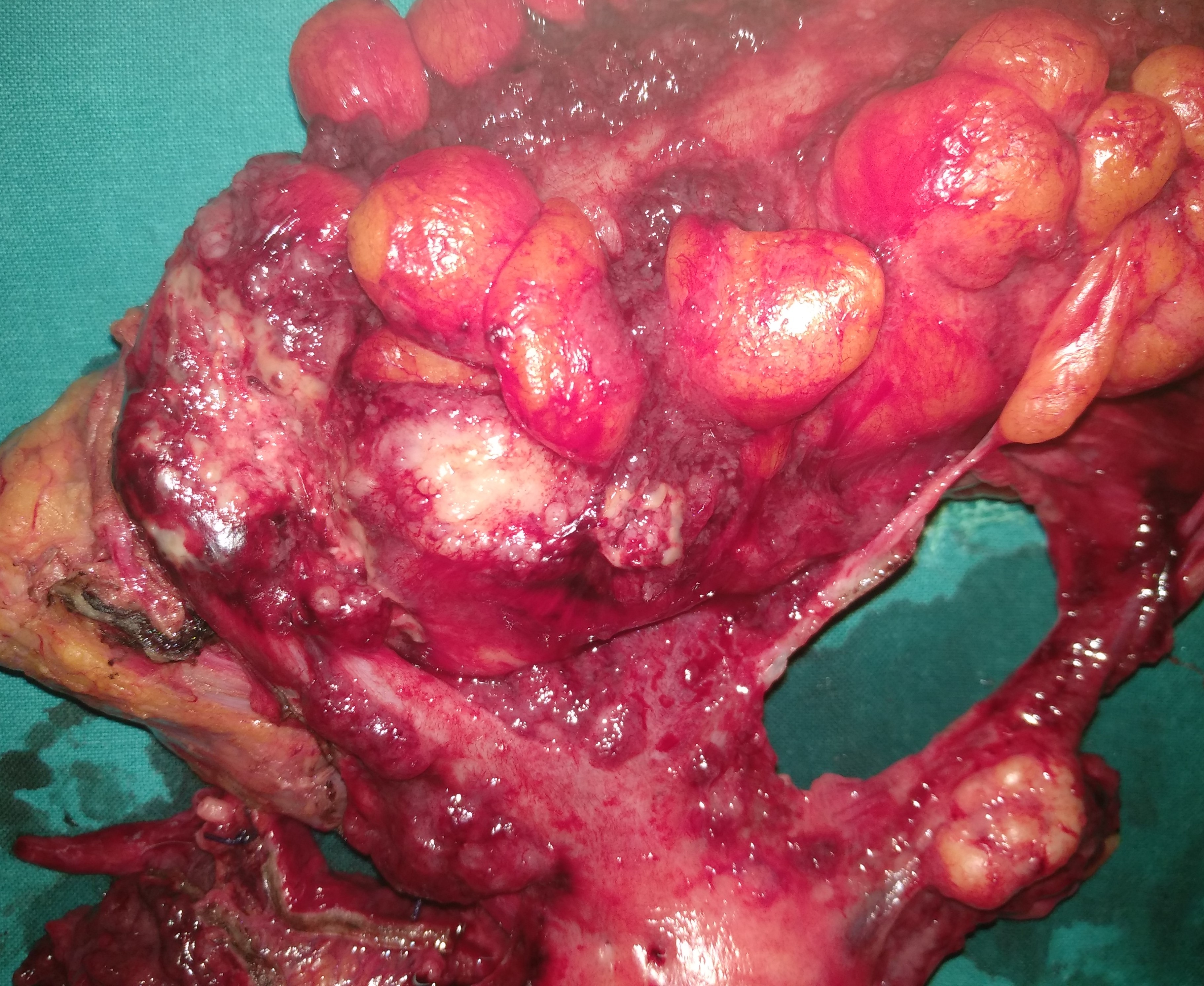
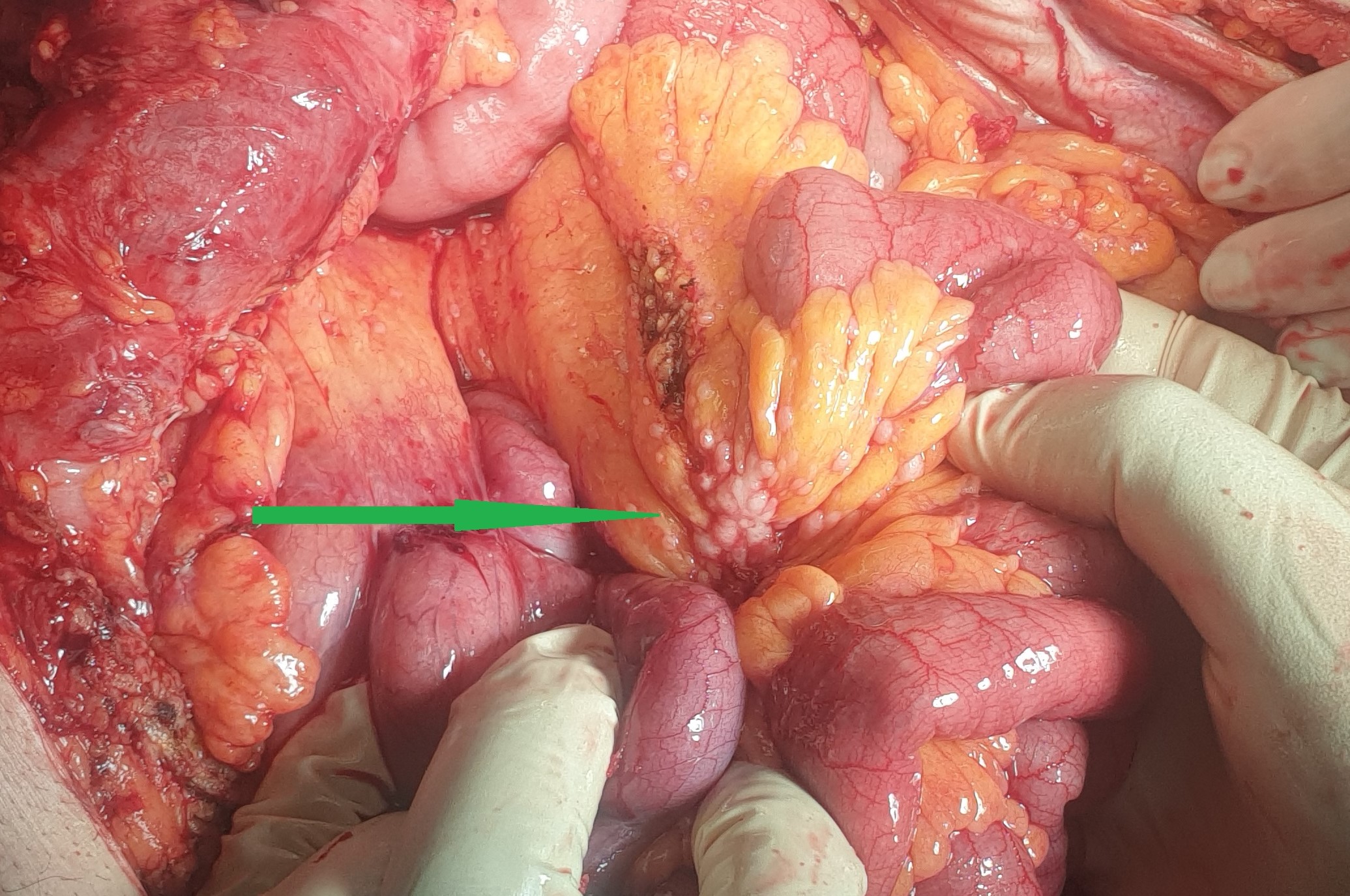
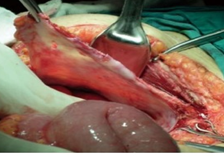
Mesenteric root infiltration — Absolute contraindication for cytoreductive surgery (Courtesy Dr. V. Penopoulos)
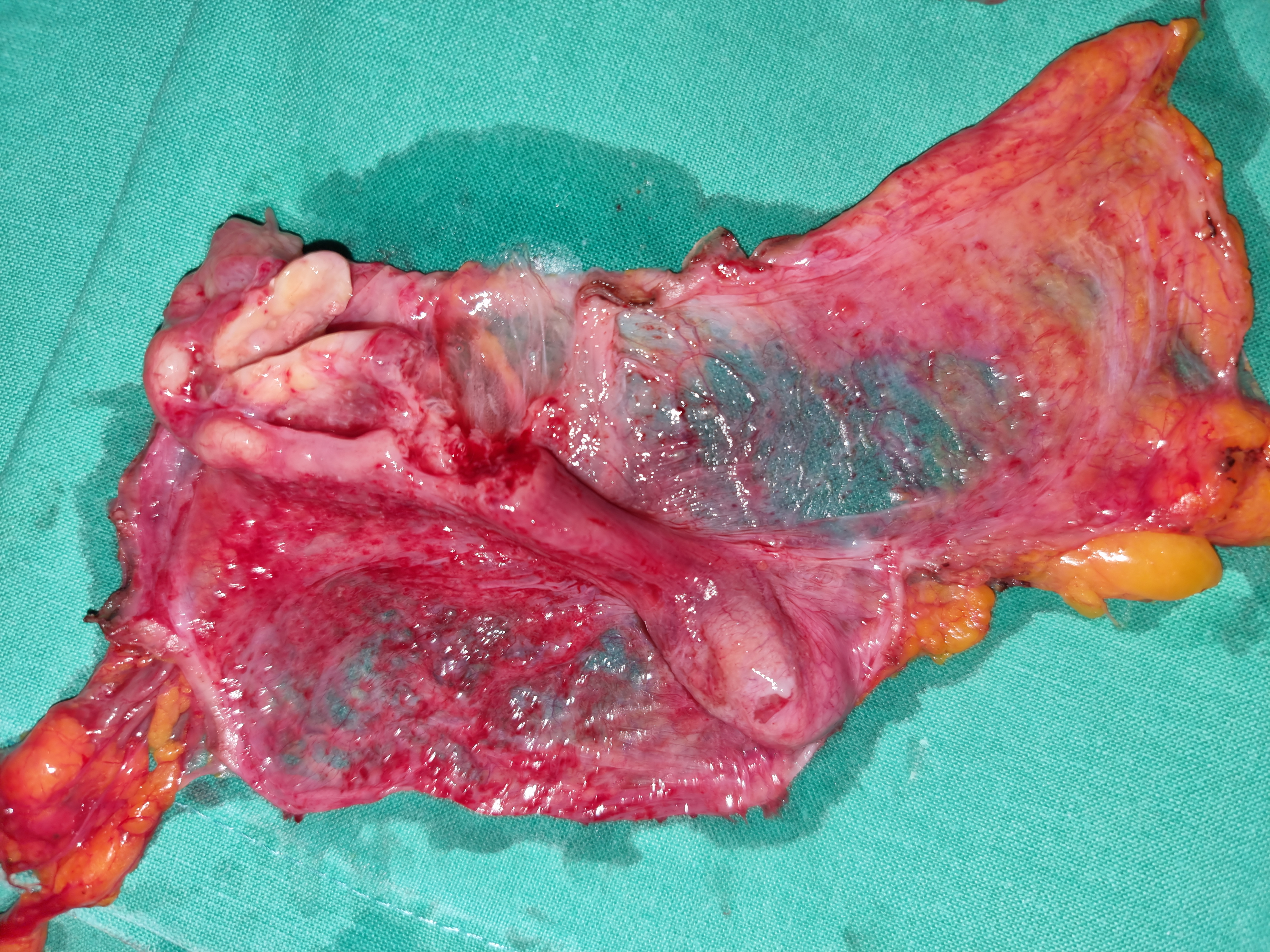
Multiple hepatic metastases — Absolute contraindication for cytoreductive surgery (Courtesy Dr. V. Penopoulos)
Multiple hepatic metastases — Absolute contraindication for cytoreductive surgery (Courtesy Dr. V. Penopoulos)
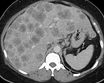
Multiple hepatic metastases — Absolute contraindication for cytoreductive surgery (Courtesy Dr. V. Penopoulos)
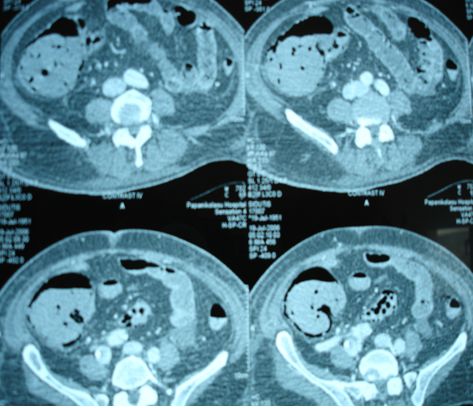
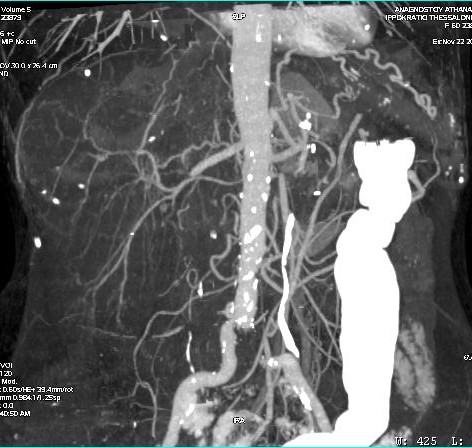
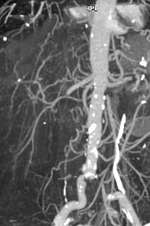
CT Angiography. Ischemic changes of the gastrointestinal tract (Courtesy Dr. V. Penopoulos)
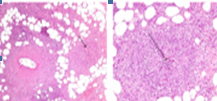
Perivenous lymphocytic infiltration and venous occlusion (Courtesy Dr. V. Penopoulos)
Perivenous lymphocytic infiltration and venous occlusion (Courtesy Dr. V. Penopoulos)
Perivenous lymphocytic infiltration and venous occlusion (Courtesy Dr. V. Penopoulos)
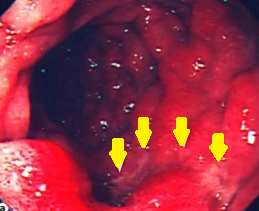
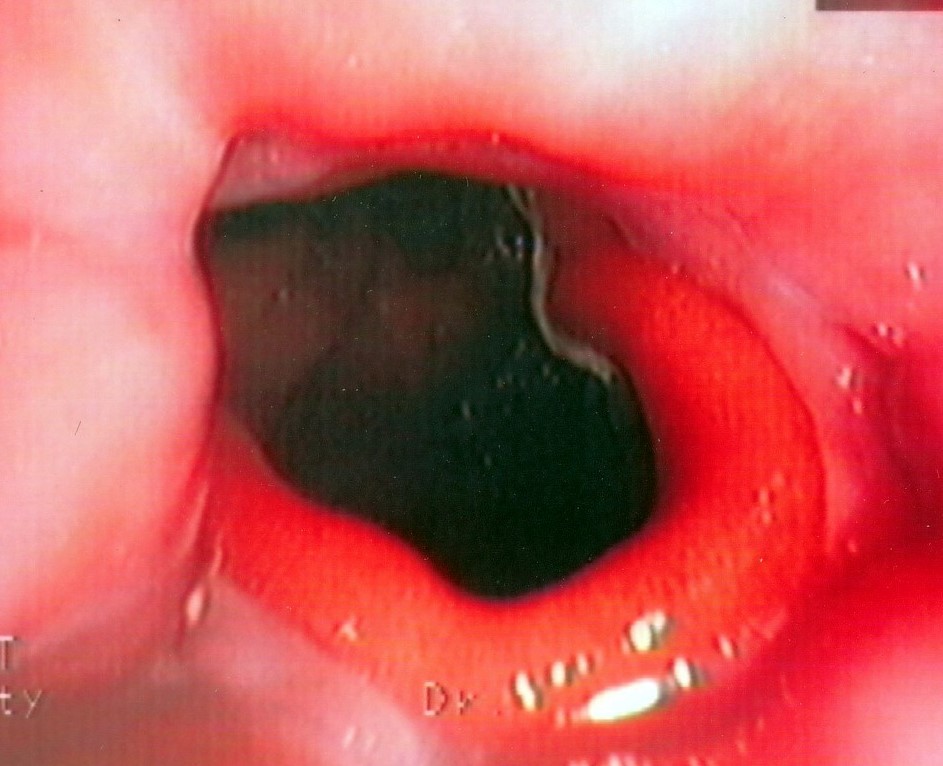
Duodenoscopy. Yellow arrows – Incipient ischemic changes of the third portion of the duodenum due to pressure from the obstruction. Courtesy Dr. V. Penopoulos.
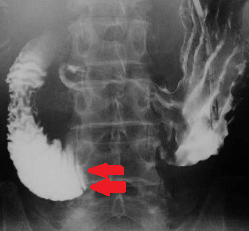
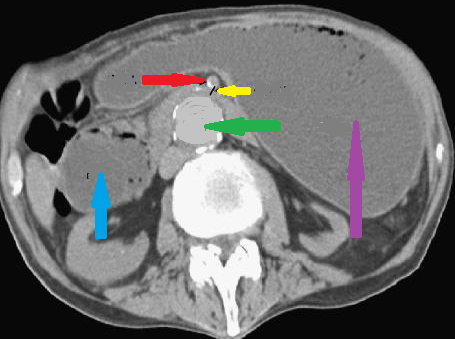
Purple arrow – Stomach. Green arrow – Aorta. Yellow arrow – Distance between the superior mesenteric artery and the aorta. Red arrow – Superior mesenteric artery. Blue arrow – Duodenum. Courtesy Dr. V. Penopoulos.
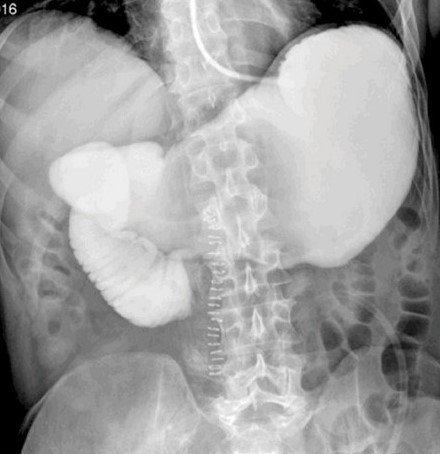
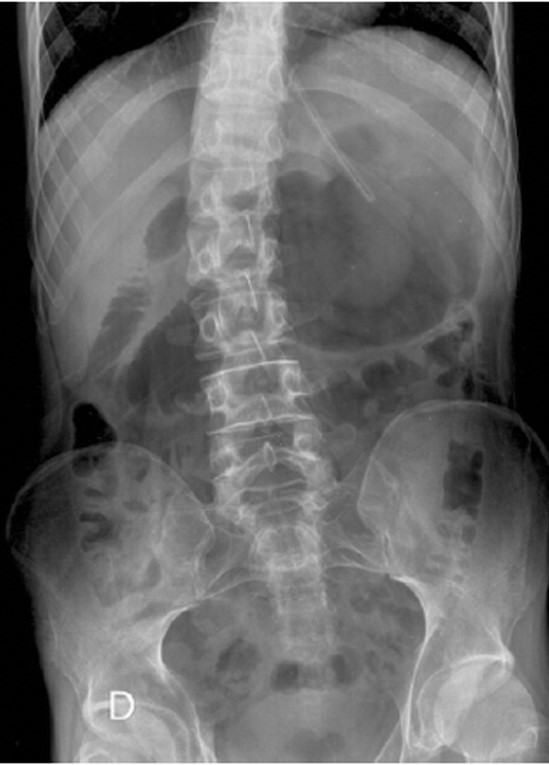
Upper gastrointestinal transit study with gastrografin swallow. Evident obstruction at the third portion of the duodenum. Courtesy Dr. V. Penopoulos.
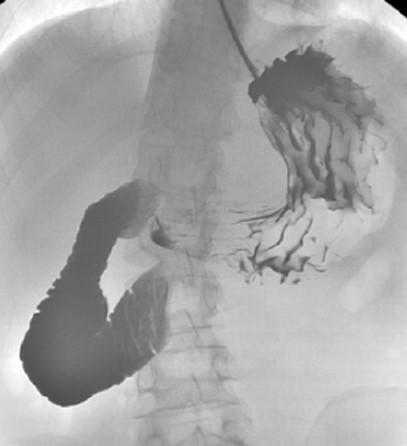
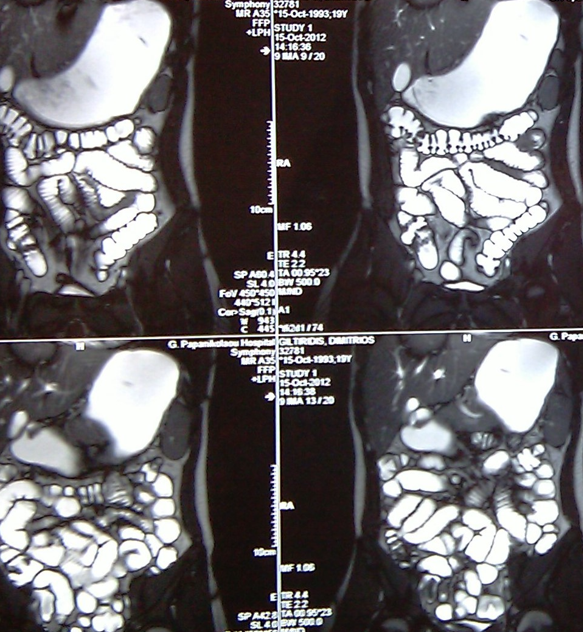
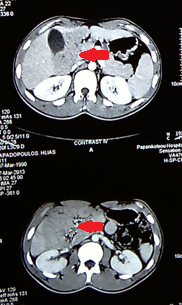
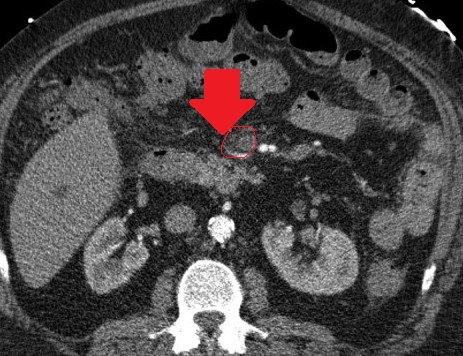
Abdominal computed tomography – Significant gastric and duodenal distension. Obstruction – severe narrowing at the third portion of the duodenum, anterior to the abdominal aorta and posterior to the superior mesenteric artery. Courtesy Dr. V. Penopoulos.
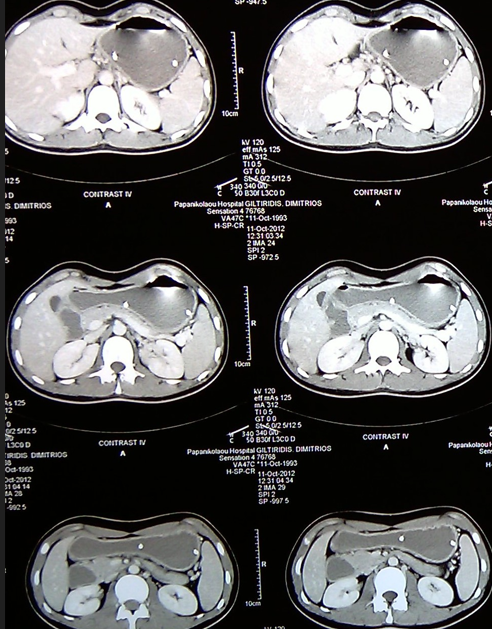
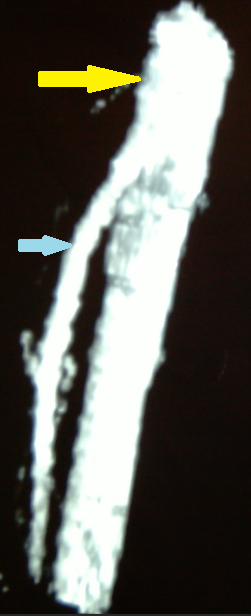
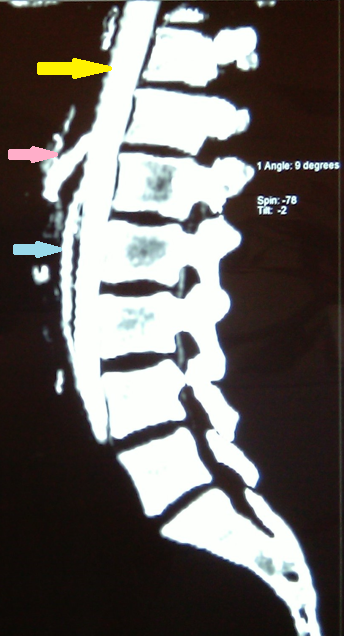
CT angiography. Yellow arrow – Aorta. Light blue arrow – Superior mesenteric artery. Pink arrow – Celiac artery (trunk of Haller). Evident significant reduction of the aortomesenteric angle to 9 degrees and the aortomesenteric distance to 4 mm. Courtesy Dr. V. Penopoulos.
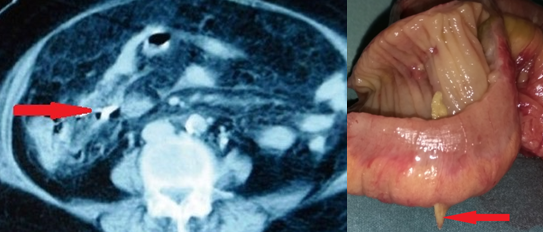
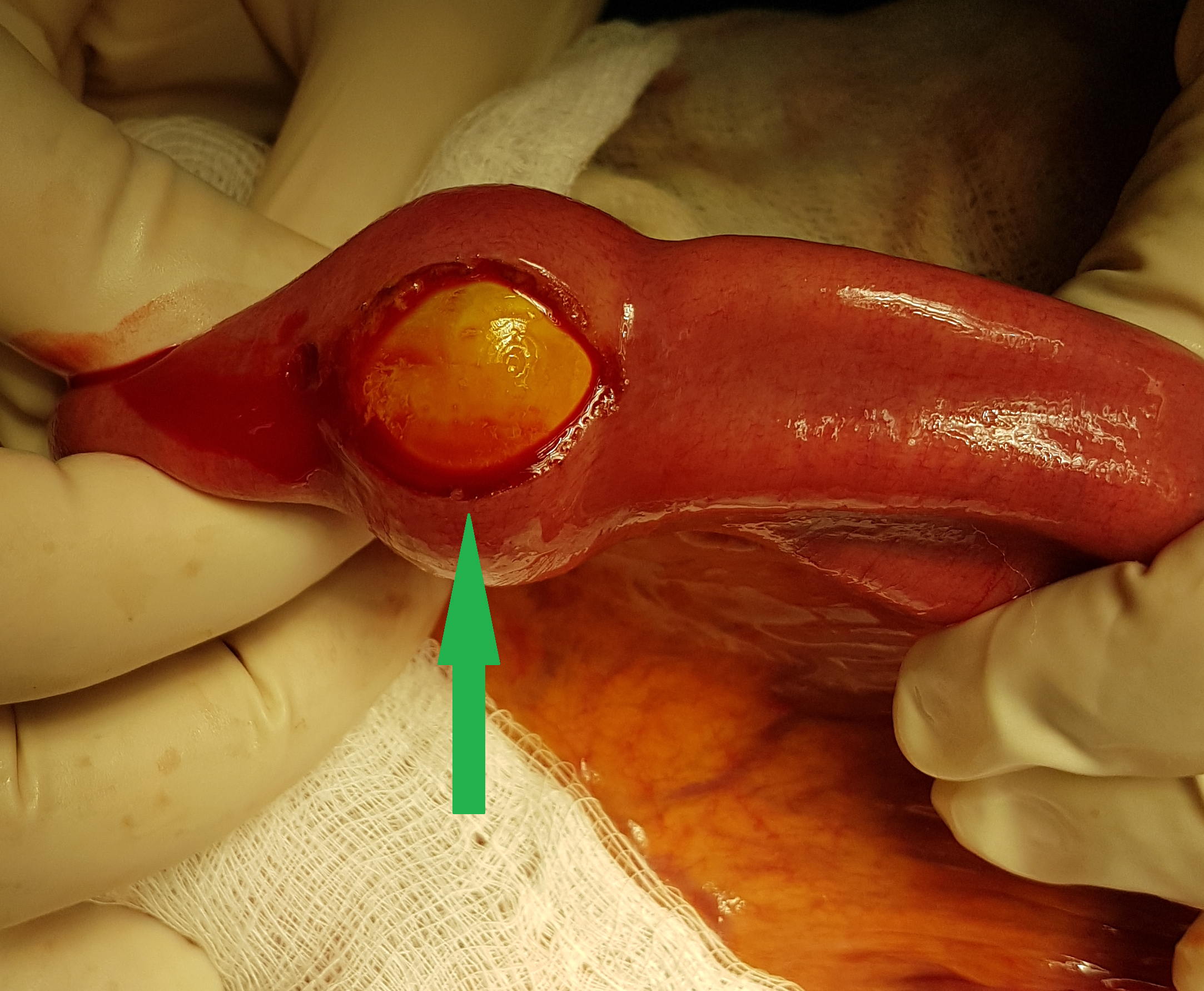
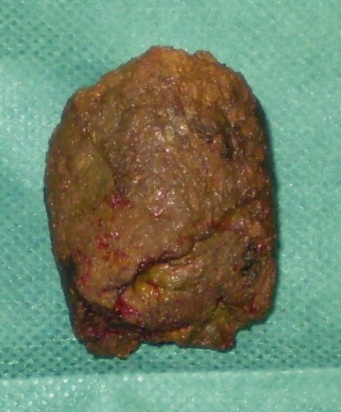
Figure 1 . Bone fragment penetrating the bowel wall . ( Courtesy Dr . V . Penopoulos ) .
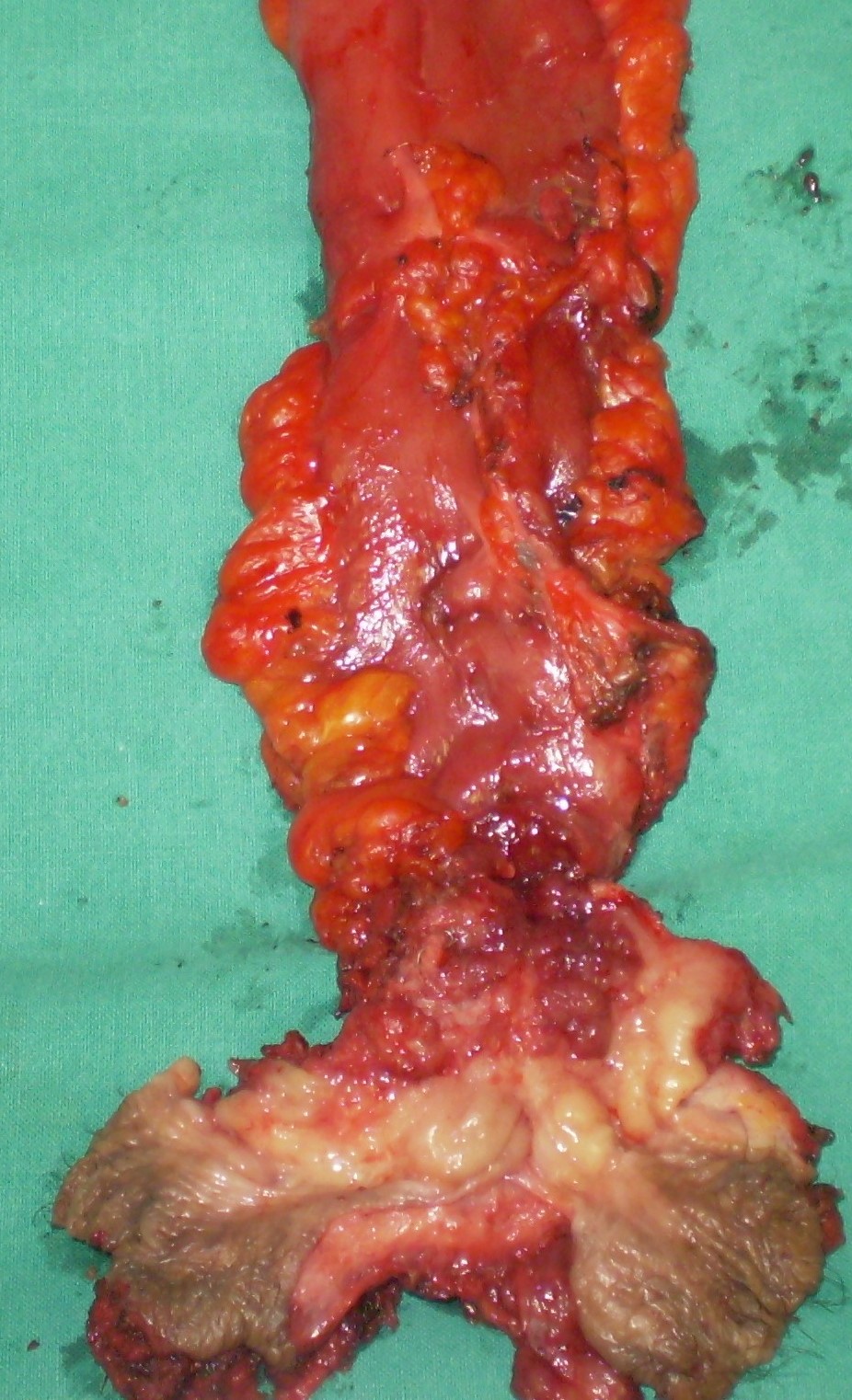
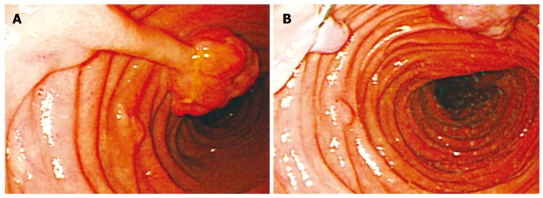
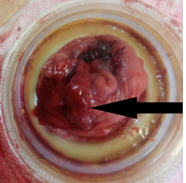
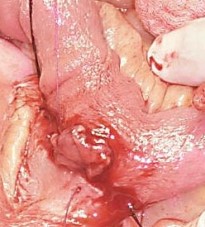
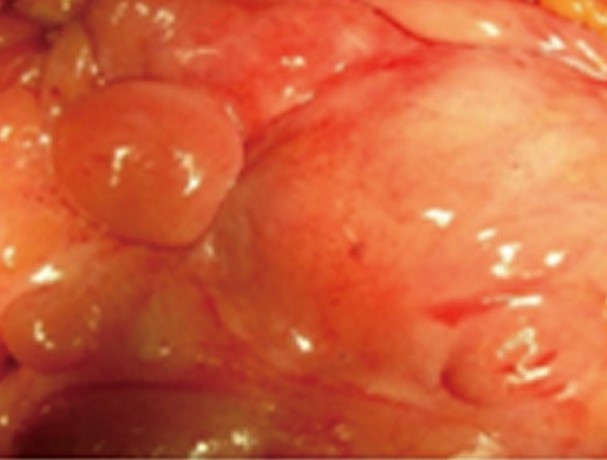
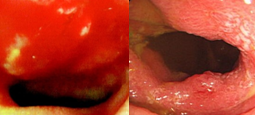
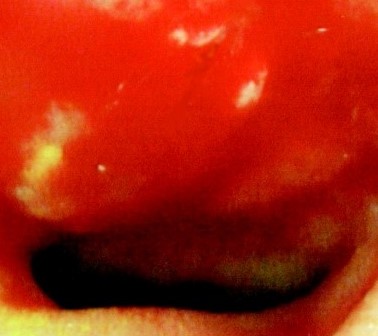
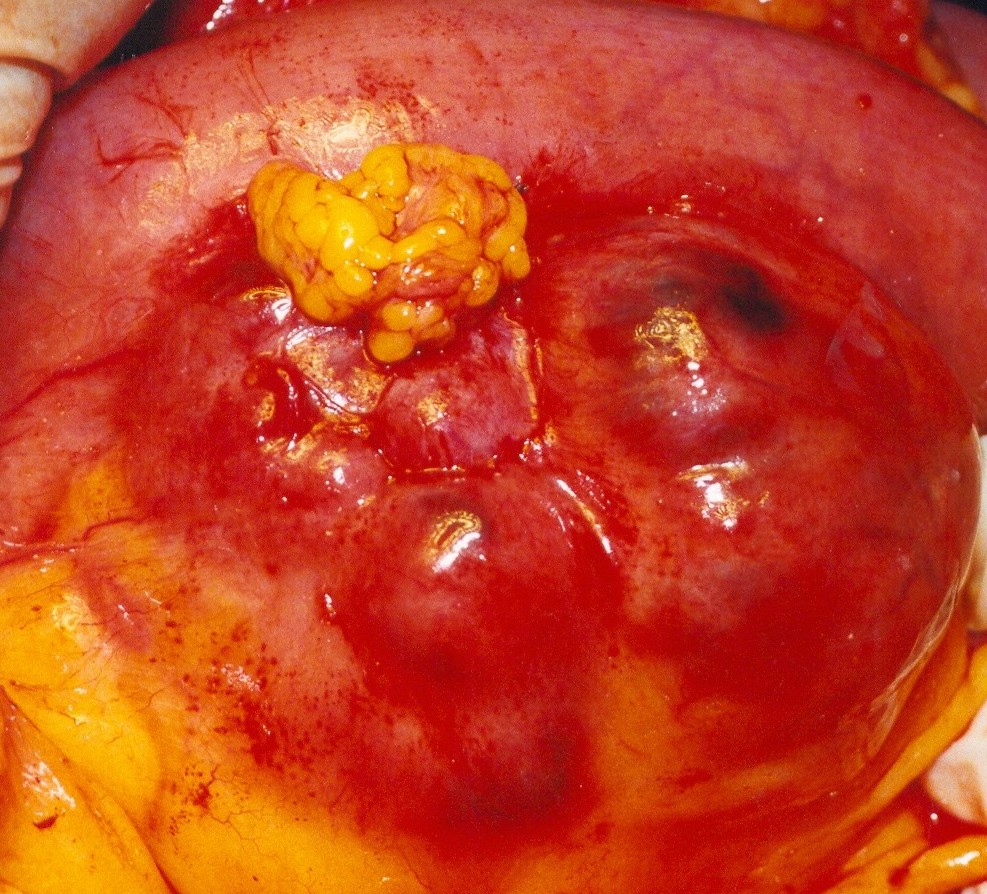
The adenocarcinoma is clearly seen nearby the ileal pouch anal anastomosis (Courtesy Dr. V. Penopoulos)
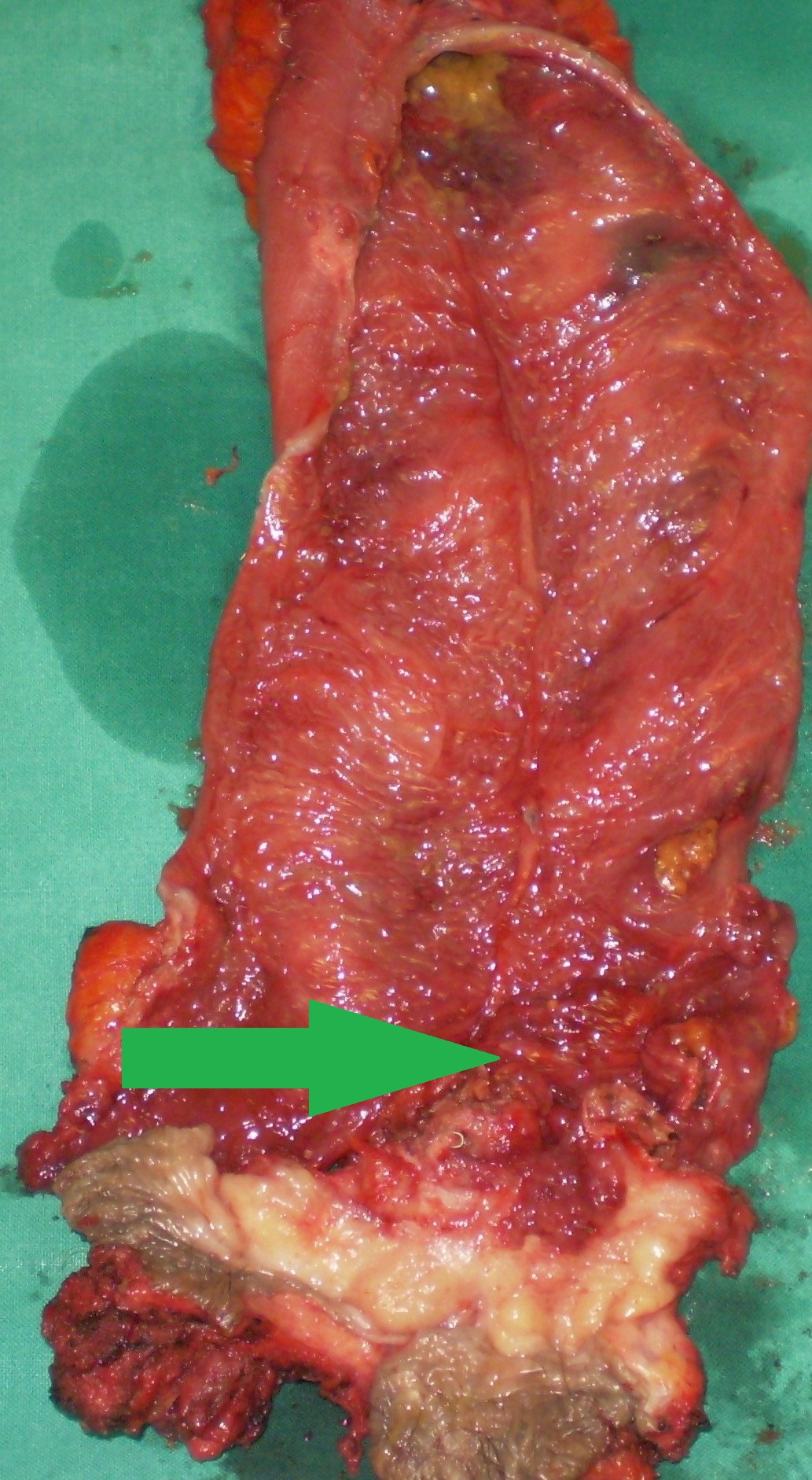
The adenocarcinoma is clearly seen nearby the ileal pouch anal anastomosis (Courtesy Dr. V. Penopoulos)
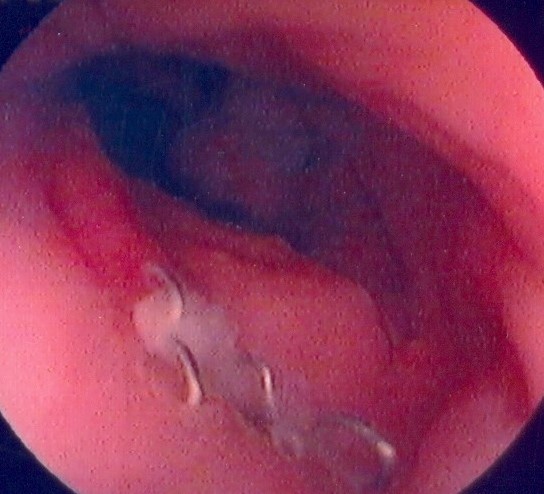
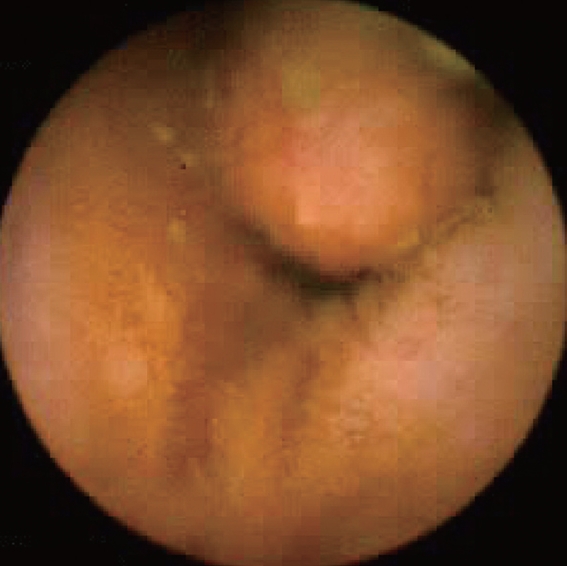
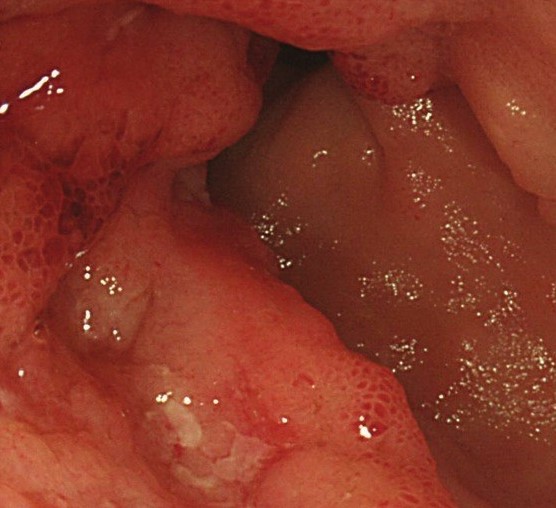
Endoscopic view of ileal pouch - anal anastomosis 3 years before the development of adenocarcinoma (Courtesy Dr. V. Penopoulos)
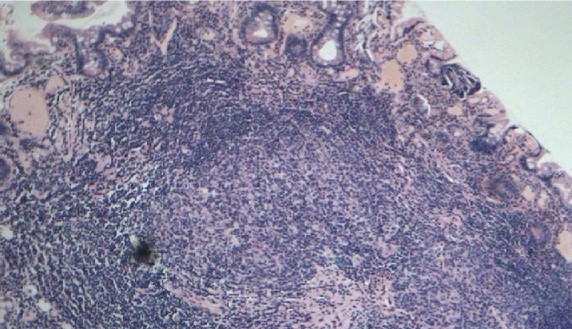
Numerous enlarged follicles with well-developed reactive germinal centres separated by a mixed infiltrate of lymphocytes, plasma cells and eosinophils (Courtesy Dr. V. Penopoulos).
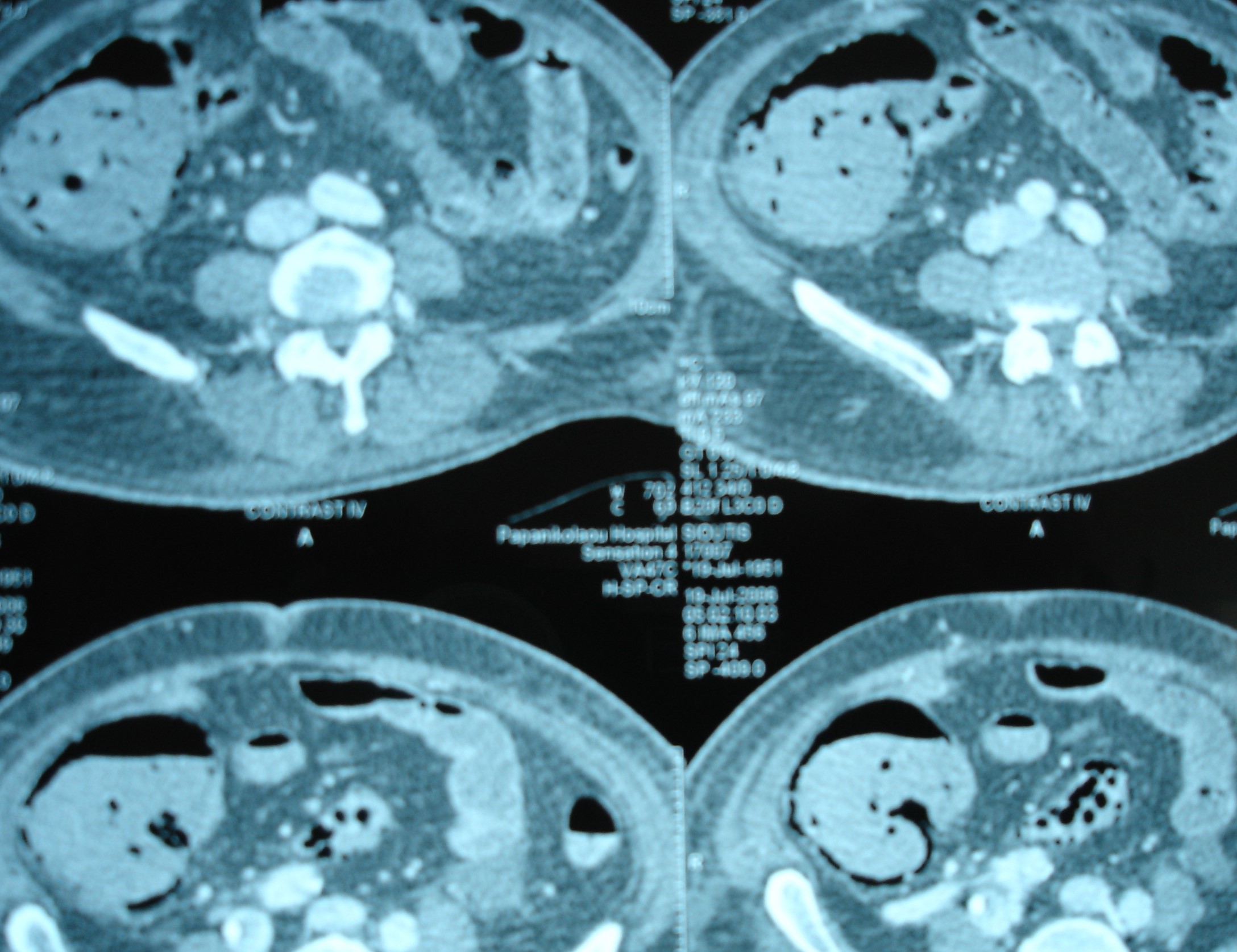
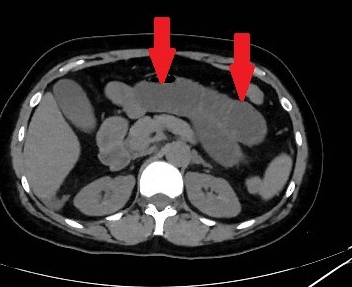
Figure 2 . Abdominal CT Scan indicative of intestinal ischemia . ( Courtesy Dr . V . Penopoulos ) .
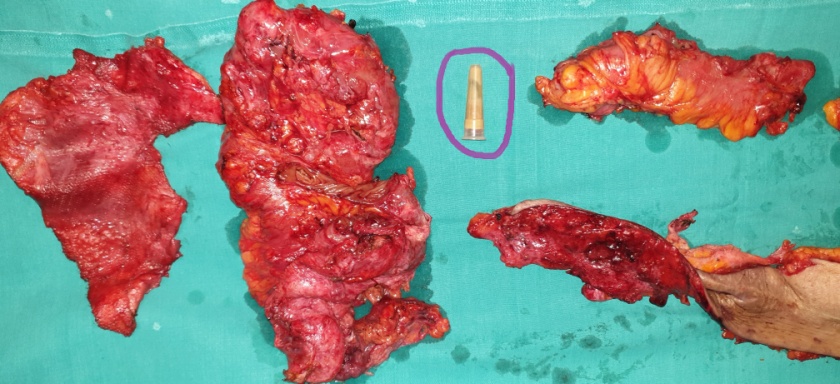
Purple circle: Removed foreign body from the right iliac fossa (most likely a severed segment of Robinson drain) (Courtesy Dr. V. Penopoulos)
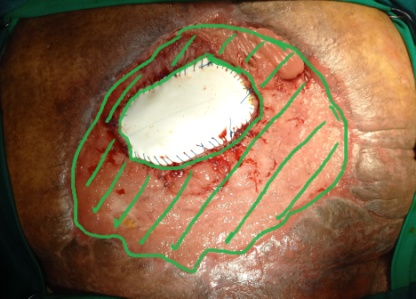
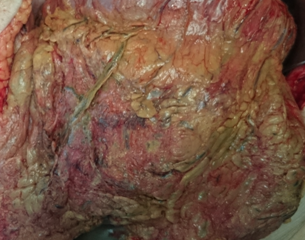
Green shading: Complete occupation of the abdomen by the peritoneal "cocoon" (Courtesy Dr. V. Penopoulos)
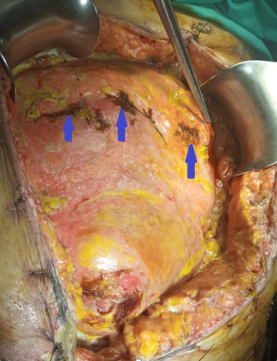
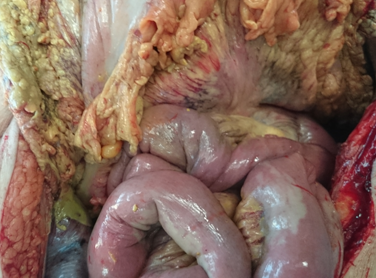
Purple arrows: Sites of small bowel perforation. Encapsulation of the entire peritoneal cavity (Courtesy Dr. V. Penopoulos)
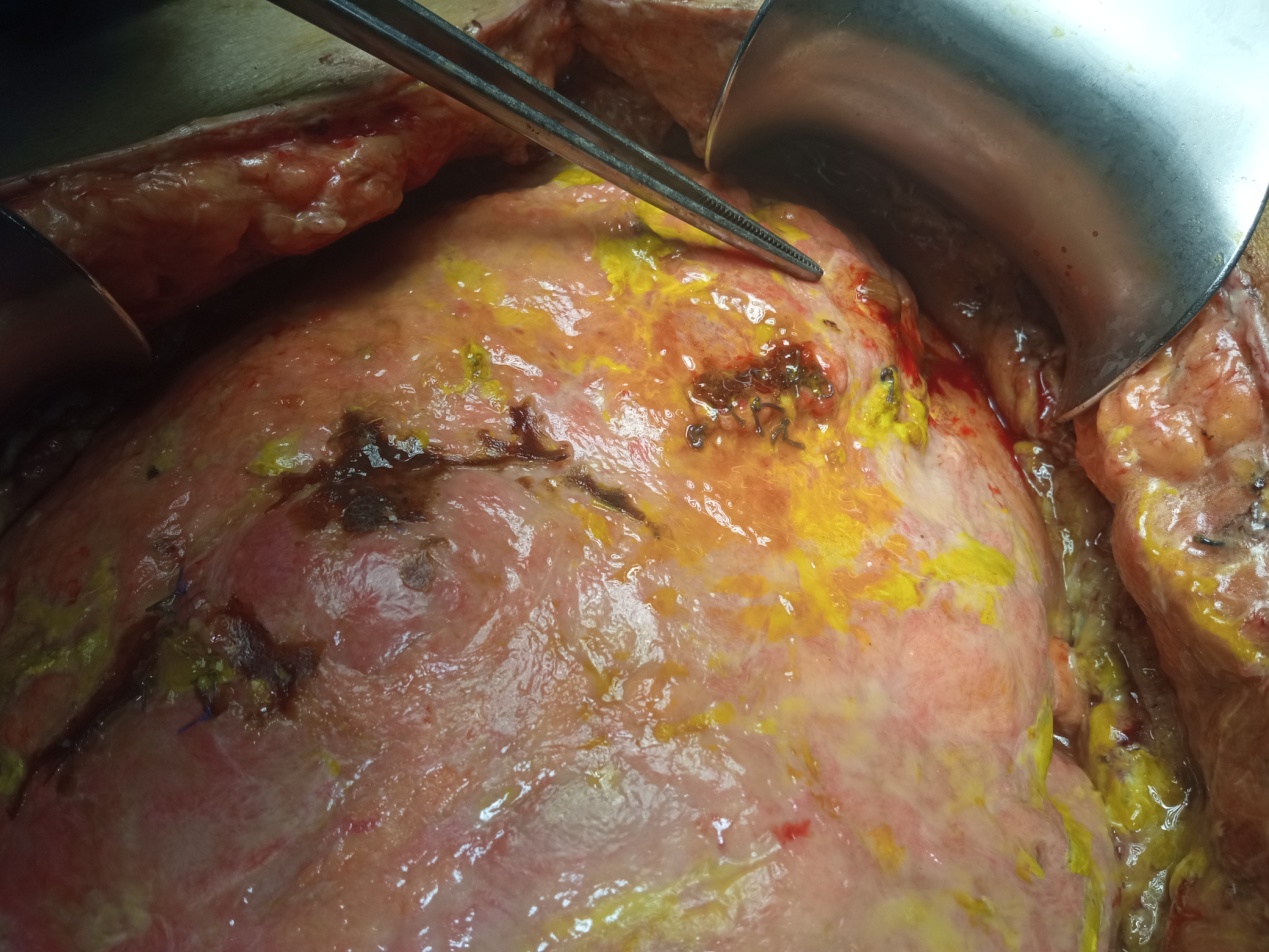
Purple arrows: Sites of small bowel perforation. Encapsulation of the entire peritoneal cavity (Courtesy Dr. V. Penopoulos)
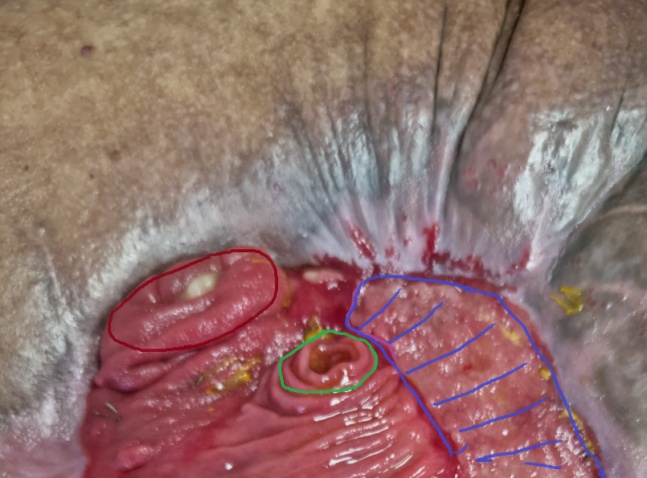
Purple outline: Complete coverage of the abdomen by the "cocoon". Green outline: Enterostomy. Brown outline: Peripheral opening of disrupted bowel loop (Courtesy Dr. V. Penopoulos)
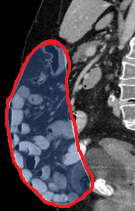
Lateral view demonstrating the size of the recurrent incisional hernia (Courtesy Dr. V. Penopoulos)
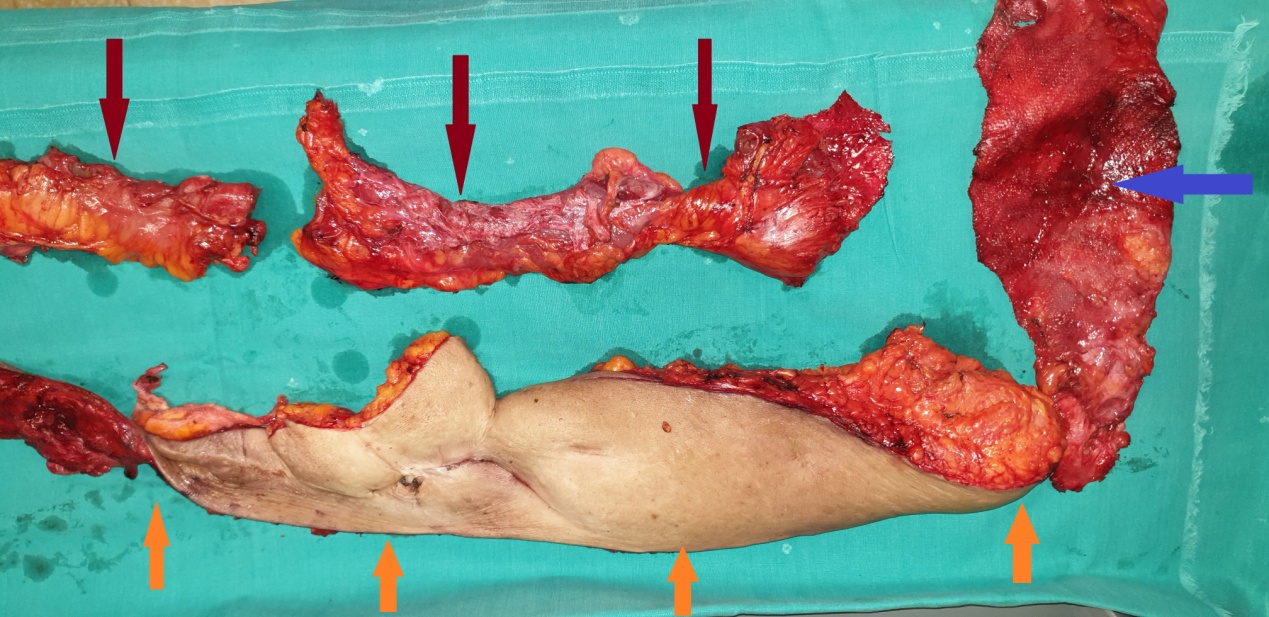
Orange arrows: Adipocutaneous flaps. Purple arrow: Removed mesh. Brown arrows: Enterectomies (Courtesy Dr. V. Penopoulos)
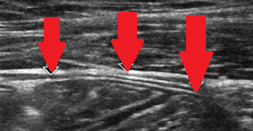
Ultrasound examination. Red arrows: Thickened peritoneum (Courtesy Dr. V. Penopoulos)
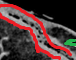
Detail of the infected mesh which had displaced to the right - green arrow - with presence of air bubbles (Courtesy Dr. V. Penopoulos)
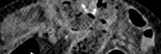
Detail of the incarcerated segment of small intestine within the hernia sac (Courtesy Dr. V. Penopoulos)
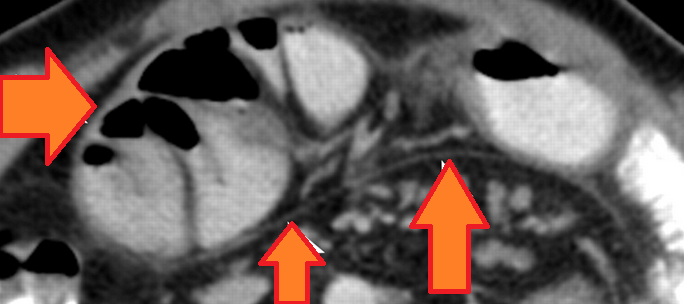
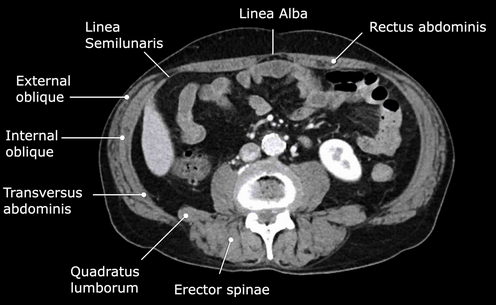
Normal abdominal CT scan. Normal anatomical structures of the abdominal walls (Courtesy Dr. V. Penopoulos)
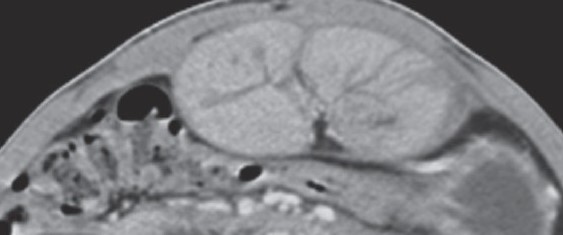
Normal abdominal CT scan. Normal anatomical structures of the abdominal walls (Courtesy Dr. V. Penopoulos)
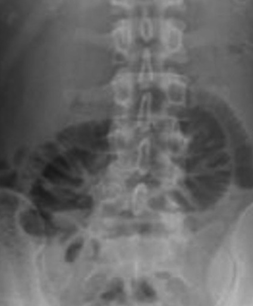
Abdominal CT. Abdominal "cocoon". Encapsulated bowel loops (Courtesy Dr. V. Penopoulos)
Abdominal CT. Abdominal "cocoon". Encapsulated bowel loops (Courtesy Dr. V. Penopoulos)
Ultrasound examination. Red arrows: Thickened peritoneum (Courtesy Dr. V. Penopoulos)
Ultrasound examination. Red arrows: Thickened peritoneum (Courtesy Dr. V. Penopoulos)
Ultrasound examination. Red arrows: Thickened peritoneum (Courtesy Dr. V. Penopoulos)
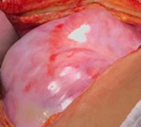
Very large incisional hernia. Red arrows - Separated abdominal walls - atrophic rectus abdominis muscle (Courtesy Dr. V. Penopoulos)
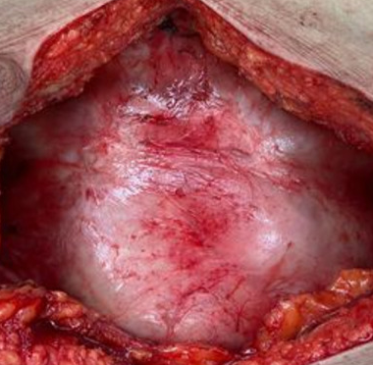
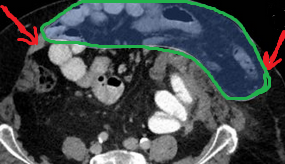
Postoperative (neglected peritonitis) development of sclerosing encapsulating peritonitis. The development of a "cocoon" encapsulating all abdominal viscera is evident (Courtesy Dr. V. Penopoulos)
Very large incisional hernia. Red arrows - Separated abdominal walls - atrophic rectus abdominis muscle (Courtesy Dr. V. Penopoulos)
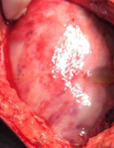
Plain abdominal radiograph. Nonspecific findings of intestinal obstruction (Courtesy Dr. V. Penopoulos)
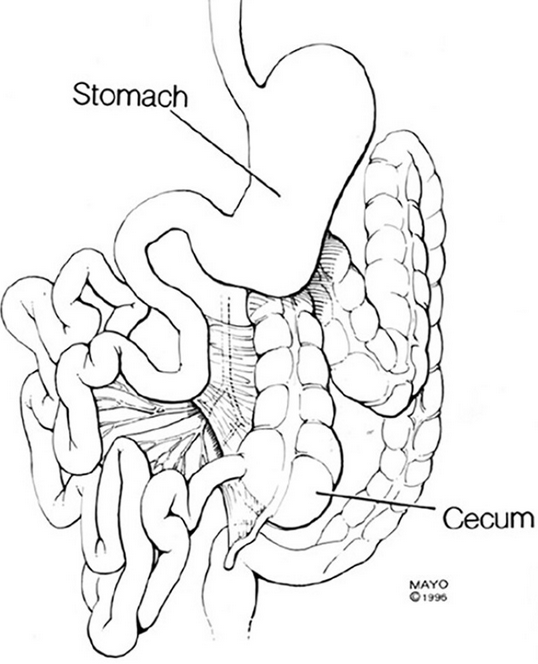
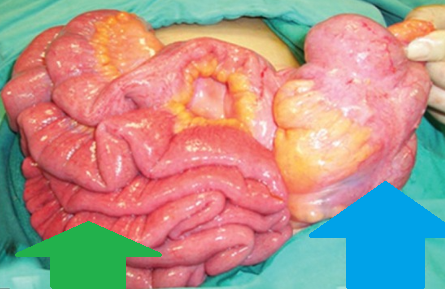
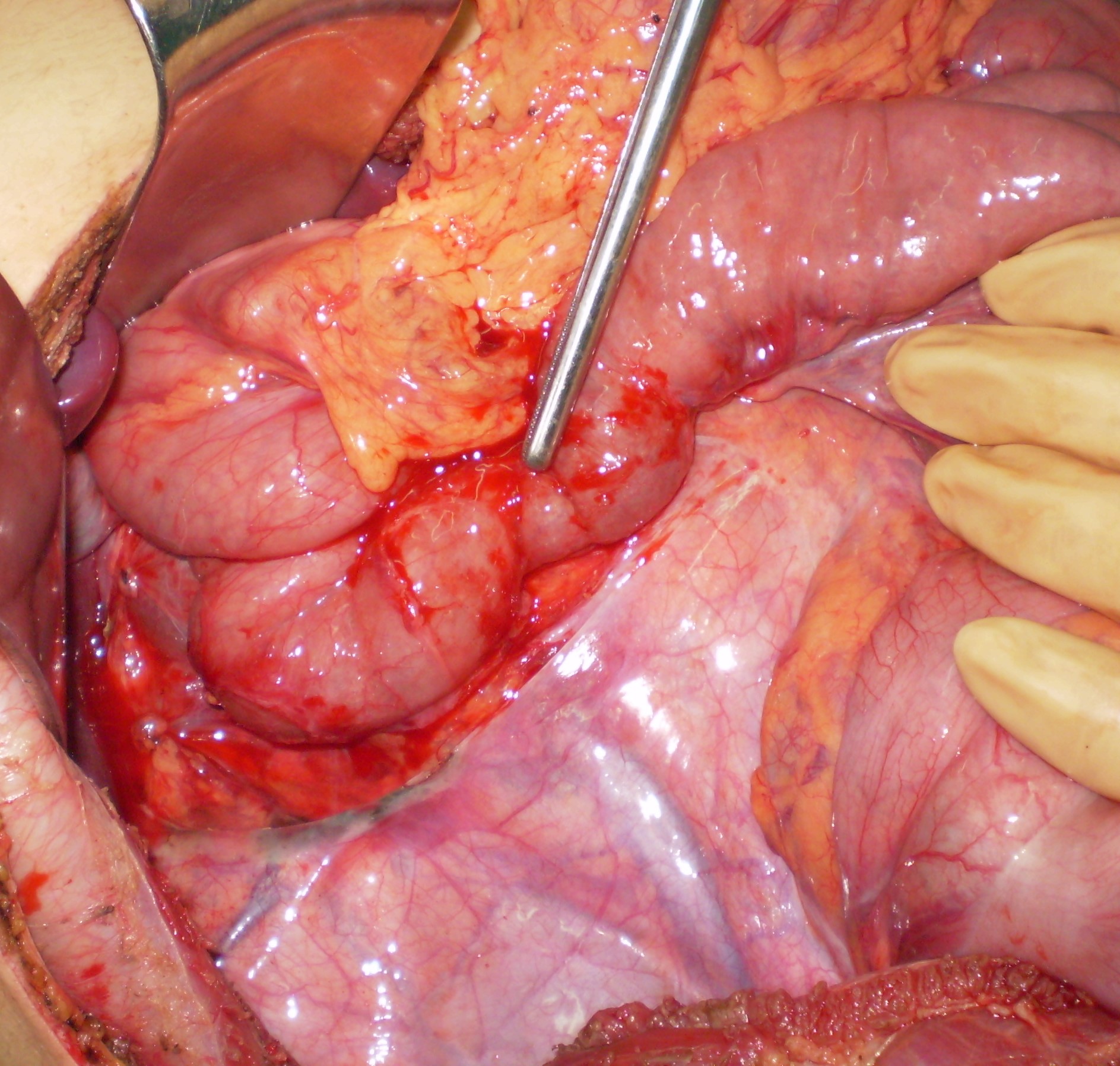
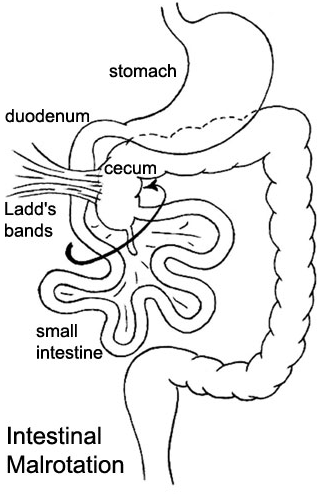
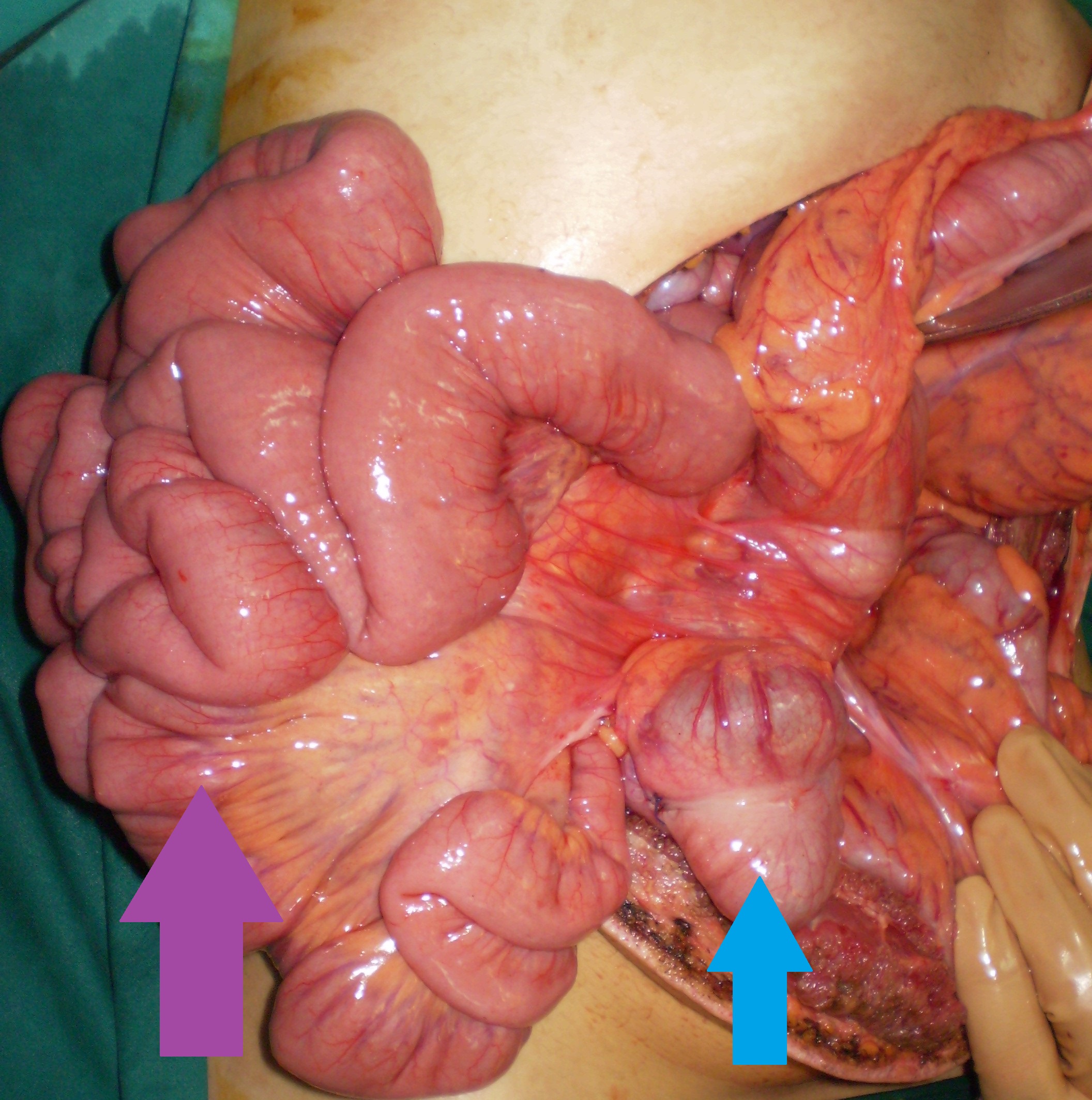
Left — Schematic representation of anomalous midgut rotation. Right — Macroscopic view after entering the abdomen. Purple arrow — Small bowel. Cyan arrow — Cecum (Courtesy Dr. V. Penopoulos)
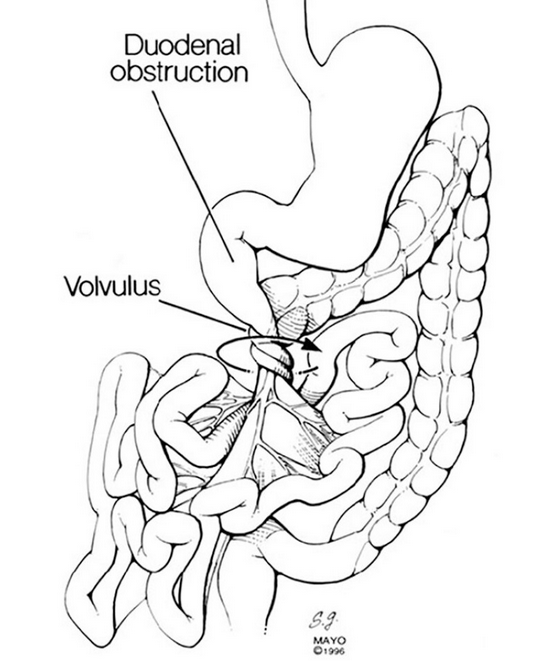
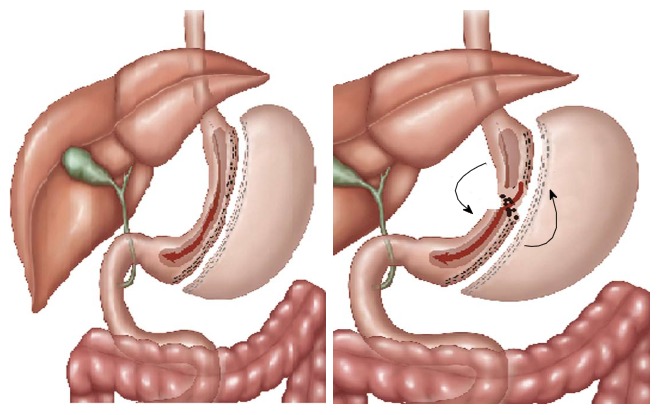
Left — Cecal volvulus and duodenal obstruction. Right — Complete reduction of cecal volvulus (Courtesy Dr. V. Penopoulos)
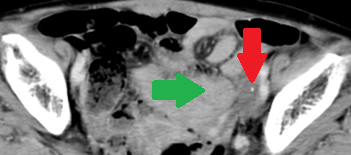
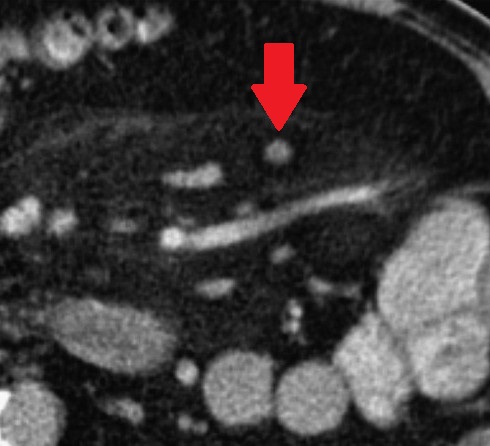
Abdominal CT scan after a 2-year interval. Red arrow – small residual neoplasm. Green arrow – small bowel loops (Courtesy Dr. V. Penopoulos)
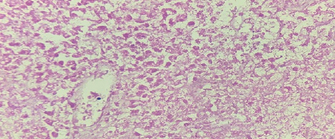
a) Presence of numerous macrophages containing hemosiderin, cholesterol clefts, intermixed with inflammatory cells and cellular debris. b) Presence of a fibrocollagenous capsule and intraluminal necrosis (Courtesy Dr. V. Penopoulos)
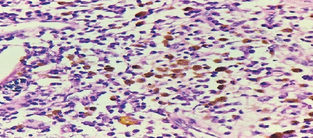
a) Presence of numerous macrophages containing hemosiderin, cholesterol clefts, intermixed with inflammatory cells and cellular debris. b) Presence of a fibrocollagenous capsule and intraluminal necrosis (Courtesy Dr. V. Penopoulos)
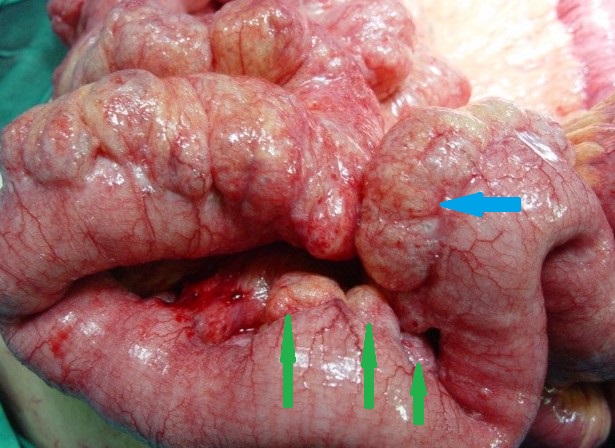
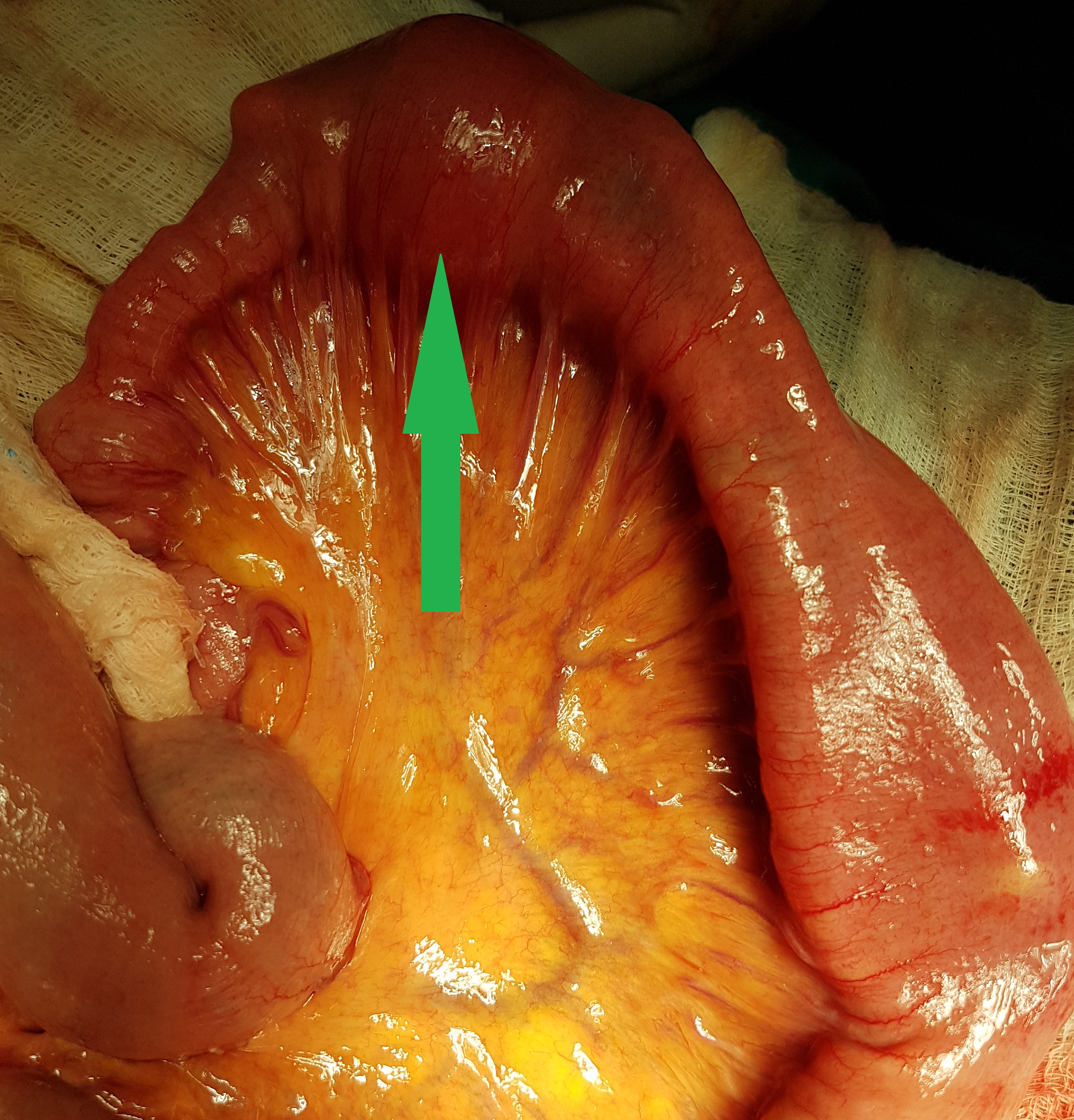
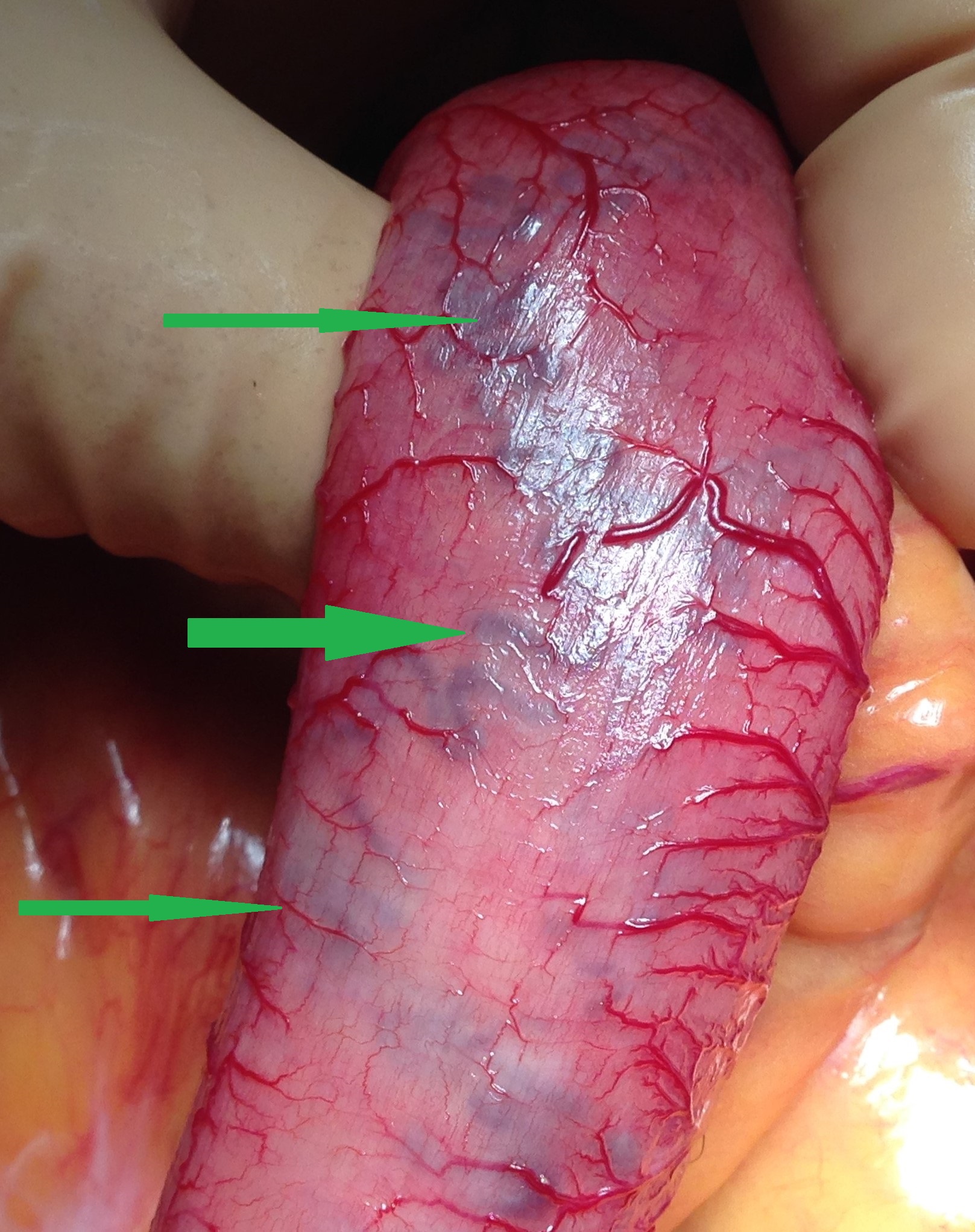
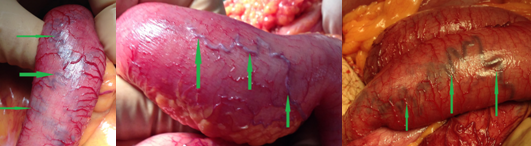
Operative view of pneumatosis intestinalis. Blue arrow - Pneumatosis. Green arrows - Diverticula
Figure 2 . Abdominal CT scan shows markedly dilated stomach with mass-like, thick-walled bowel loops (red arrow). ( Courtesy Dr . V . Penopoulos ) .

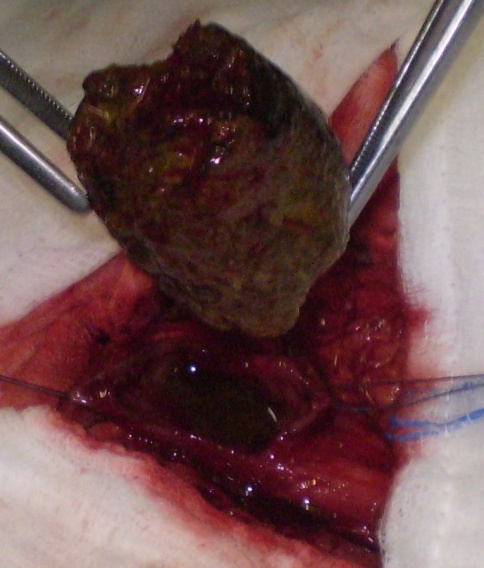
Figure 3 . A gross surgical specimen shows the necrotic changed intussusception (red arrow).